Abstract
Osteosarcoma is the most common bone tumor in dogs. However, current literature focuses primarily on appendicular osteosarcoma. This study examined the prognostic value of histological and clinical factors in flat and irregular bone osteosarcomas and hypothesized that clinical factors would have a significant association with survival time while histological factors would not. All osteosarcoma biopsy samples of the vertebra, rib, sternum, scapula, or pelvis were reviewed while survival information and clinical data were obtained from medical records, veterinarians, and owners. Forty-six dogs were included in the analysis of histopathological variables and 27 dogs with complete clinical data were included in the analysis of clinical variables. In the histopathologic cox regression model, there was no significant association between any histologic feature of osteosarcoma, including grade, and survival time. In the clinical cox regression model, there was a significant association between the location of the tumor and survival time as well as between the percent elevation of alkaline phosphatase (ALP) above normal and survival time. Controlling for ALP elevation, dogs with osteosarcoma located in the scapula had a significantly greater hazard for death (2.8) compared to dogs with tumors in other locations. Controlling for tumor location, every 100% increase in ALP from normal increased the hazard for death by 1.7. For canine osteosarcomas of the flat and irregular bones, histopathological features, including grade do not appear to be rigorous predictors of survival. Clinical variables such as increased ALP levels and tumor location in the scapula were associated with decreased survival times.
Osteosarcoma is the most common bone tumor in the dog and behaves aggressively exhibiting both local invasiveness and distant metastases. 22 However, the majority of canine osteosarcomas arise from the appendicular skeleton and it has been suggested that current data are biased towards appendicular tumors and that osteosarcoma of the flat and irregular bones has a different biological behavior and prognosis. 4,10,20 Dogs with mandibular osteosarcoma showed a higher one year survival rate and dogs with rib osteosarcoma showed a higher metastatic rate than dogs with appendicular osteosarcoma. 9,20
Several clinical and histologic criteria have been reported as potential prognostic indicators for osteosarcoma of the flat and irregular bones including anatomic site, 9 weight, 9 completeness of surgical excision, 9 breed, 4 definitive versus palliative radiation therapy, 4 and histologic grade. 20 However, these papers included only small numbers of cases from locations other than the rib and mandible. Tumor grade, while prognostic in human osteosarcoma, 8 has historically not been consistently prognostic in studies of canine osteosarcoma with several studies showing no prognostic signifigance. 9,20 However, a recent study by Kirpensteijn et al showed a histologic grade of III to be an independent predictor of clinical outcome when cases of canine osteosarcomas from all locations in the body were evaluated. 11 The existence of a grading system that is significantly associated with survival for osteosarcomas, especially for this subset of osteosarcomas for which survival may be longer, would be invaluable for the clinical decision making process. However, due to the variable production of osteoid, grading of osteosarcomas is difficult and potentially inconsistent.
The purpose of the present study was to evaluate potential histologic and clinical prognostic factors and survival times in a specific subset of dogs with flat and irregular bone osteosarcoma—dogs with osteosarcoma of the vertebra, rib, sternum, scapula, and pelvis. Our hypothesis was that histopathologic variables including tumor grade and classification as well as the degree of pleomorphism, the mitotic index, the amount of matrix present, and the presence or absence of vascular invasion in the tumor itself would have no significant association with survival time in dogs with osteosarcoma of the vertebra, rib, sternum, scapula, or pelvis. In contrast, clinical variables including the site of the osteosarcoma and the weight of the dog would have a significant association with survival time.
Materials and Methods
All dogs with biopsies consistent with osteosarcoma of the flat and irregular bones of the skeleton submitted to the Laboratory of Pathology at the Matthew J. Ryan Veterinary Hospital of the University of Pennsylvania between January 2004 and December 2009 were identified. Animals were eligible for inclusion if the tumor arose from the vertebra, rib, sternum, scapula, or pelvis; if histopathologic slides were available from the time of diagnosis; and if date of the dog’s death could be verified.
Clinical Data
Information regarding breed, age, sex, tumor location, type of surgery, serum ALP level, and date of death was obtained from telephone interviews with clients or referring veterinarians, written questionnaires completed by referring veterinarians, and hospital records. Whenever possible, additional information was obtained including initial physical exam findings; results of staging tests including thoracic radiographs, abdominal ultrasound, lymph node aspirates; use of adjunctive treatments including chemotherapy and radiation therapy; date of tumor recurrence; and cause of death.
Histopathology Data
Biopsy slides from diagnostic biopsies or excisional biopsies at the time of diagnosis were reviewed by 2 of the authors (MHG, JAB) and final grade was assigned by a single pathologist (MHG). The degree of pleomorphism, the mitotic index, the amount of matrix present, the amount of necrosis present, the presence or absence of vascular invasion, and the tumor type were evaluated and recorded for all samples. The degree of pleomorphism was graded on a scale from 0 to 3 with 0 = no nuclear variation, 1 = mild variation, 2 = moderate variation, and 3 = marked variation. The mitotic index was defined as the number of mitotic figures per 10 high power (400×) fields. The amount of matrix was graded on a scale from 1 to 3: 1, > 50% matrix; 2, 25%–50% matrix; 3, < 25% matrix. The amount of necrosis was graded on a scale from 0 to 3: 0, no necrosis; 1, < 15% necrosis; 2, 15%–50% necrosis; 3, > 50% necrosis. Vascular invasion was identified as present = 1 or absent = 0. Tumor type was identified as osteoblastic (OB), fibroblastic (FB), chondroblastic (CB), telangiectatic (TC), osteofibroblastic (OF), giant cell variant (GC), or osteochondrofibroblastic (OCFB) as described by Slayter et al. 17 All samples were assigned a histologic grade of I, II, or III based on the histologic scoring and grading system defined by Straw et al 20 and summarized in Tables 1 and 2.
Tumor Scoring System Modified From Straw et al 20
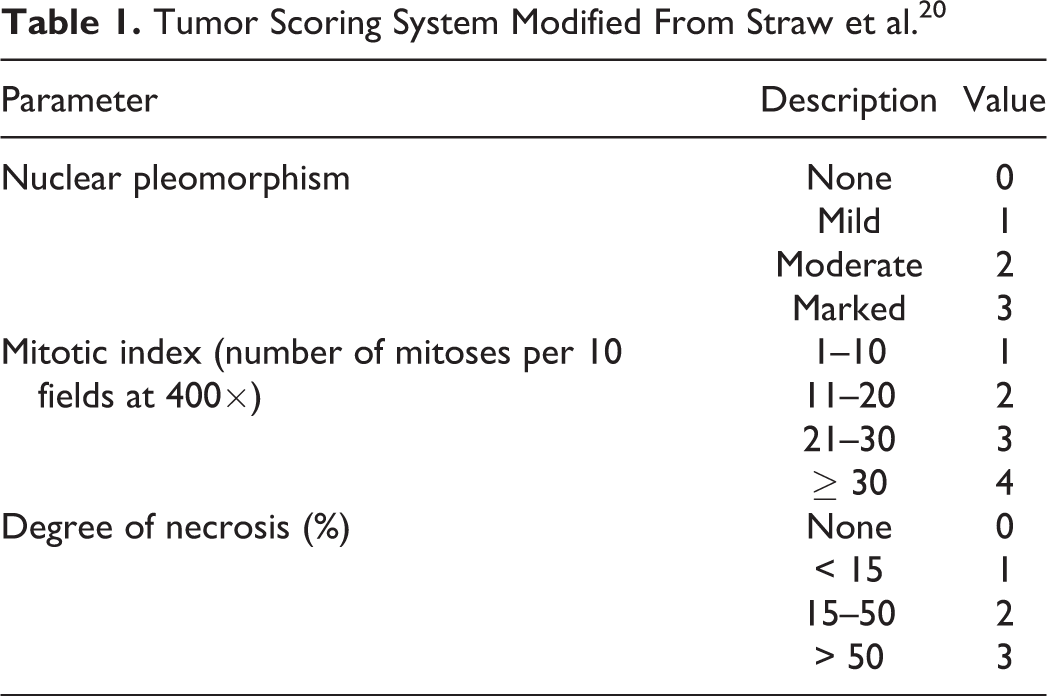
Tumor Grading System Modified From Straw et al 20 : Combined Scores From Nuclear Pleomorphism, Mitotic Index, and Degree of Necrosis

Statistical Analysis
Categorical variables were described as frequencies and percentages. Normally distributed continuous variables were described with means and standard deviations. Nonnormally distributed continuous variables were described with medians and ranges. Two Cox multivariable models were developed. The first model evaluated whether histopathologic factors were associated with survival time from diagnosis. The second model included only the subset of dogs for which clinical information was available and evaluated whether clinical factors, in addition to the histopathologic factors, were associated with survival time from diagnosis. Factors investigated in both models included pleomorphism, tumor type, amount of matrix, necrosis, grade, mitotic index, and vascular invasion. Other factors evaluated for association, interaction, or confounding in both models were age, breed, sex, and tumor location. For the second model, dogs that had the additional information on the clinical variables of type of surgery (none, marginal, wide margins, debulking) and alkaline phosphatase were included. For both models, standard stepwise development of models was followed: Two-way interactions among the main effects were investigated. An interaction term was retained based on a P value < .05. If not effect modifiers, univariate analysis was performed initially and factors with a P value < .20 were tested in each model. Factors were retained in the model based on a P value < .05 or if found to be a confounder (changing model coefficients by > 15%). All analyses were performed in Stata 11 (StataCorp, College Station, TX).
Results
Between January 2004 and December 2009, 108 biopsies in 108 dogs were consistent with osteosarcoma of the vertebra, rib, sternum, scapula, or pelvis. Of these 108 dogs, 62 (57%) dogs were lost to follow up and a definitive date of death was obtained for 46 (43%) dogs.
Of the 46 osteosarcomas, 22 (48%) arose from the rib, 11 (24%) arose from the scapula, 7 (15%) arose from the pelvis, 5 (11%) arose from the vertebrae, and 1 (2%) arose from the sternum. The most common single breed was Labrador retriever with 11 (24%) dogs. Ten (23%) dogs were mixed breeds and 12 (26%) dogs were other purebred dogs. In addition, there were 6 (13%) Golden Retrievers, 4 (9%) Greyhounds, and 3 (7%) Rottweilers. The mean age at the time of diagnosis was 8.6 ± 3.7 years (1.5–14.3 years). Twenty-three dogs (50%) were spayed females, 14 (30%) were castrated males, 6 (13%) were intact males, and 3 (7%) were intact females. Weight at the time of diagnosis was available for 33 dogs and the mean weight for these dogs was 31.7 ± 11.2 kg (5.4–56.8 kg). ALP level at the time of diagnosis was available for 30 dogs. No dog had a low ALP level, 15 (50%) dogs had a normal ALP level, and 15 (50%) of dogs had an ALP level above the reference range. The median percent increase of the ALP level above normal was 0% (0%–1607%). Information on the extent of surgery performed in each case was available in 36 cases. Of these cases, 24 (67%) had no surgery performed, 7 (19%) had a radical excision with wide surgical margins performed, 4 (11%) had a marginal excision performed, and 1 (3%) case had a debulking procedure only.
Histopathologic evaluation of the 46 osteosarcomas classified the majority of tumors, 34 cases (74%), as osteoblastic. Seven (15%) cases were classified as fibroblastic; 2 (4%) cases each were classified as chondroblastic and osteofibroblastic; and 1 (2%) case was classified as osteochondrofibroblastic. No case was classified as telangiectatic or giant cell variant. The histologic features were combined as previously described to create the histologic grade. Thirty-five (76%) osteosarcomas were grade I, 7 (15%) were grade II, and 4 (9%) were grade III. The amount of matrix was evaluated separately and 5 (11%) cases of cases showed > 50% matrix, 8 (17%) showed 25% to 50% matrix, and 33 (72%) of cases showed < 25% matrix. No cases showed evidence of vascular invasion.
All 46 cases of osteosarcoma were included in the histopathologic cohort and model. Of these 46 dogs, 27 dogs had complete clinical data regarding alkaline phosphatase level and type of surgery performed and these dogs were included in the clinical cohort and model. For the 46 cases included in the histopathologic model, there was no significant association between grade—or the other histopathologic features of the tumors—and survival time from diagnosis. For the 27 cases included in the clinical model, there was a significant association between the location of the tumor as well as the percent elevation of ALP above normal and survival time. Controlling for ALP elevation, dogs with the tumor located in the scapula had a significantly greater hazard for death (hazard ratio = 2.8, 95% confidence interval = 1.0–7.4, P = .04) compared to dogs with tumors in other locations. Controlling for tumor location, for every 100% increase in ALP from normal, the hazard for death increased by 1.7 (95% confidence interval: 1.2–2.3, P = .001). Kaplan Meier survival estimates are presented in Figure 1. No significant association was found between dog weight or dog size and survival.
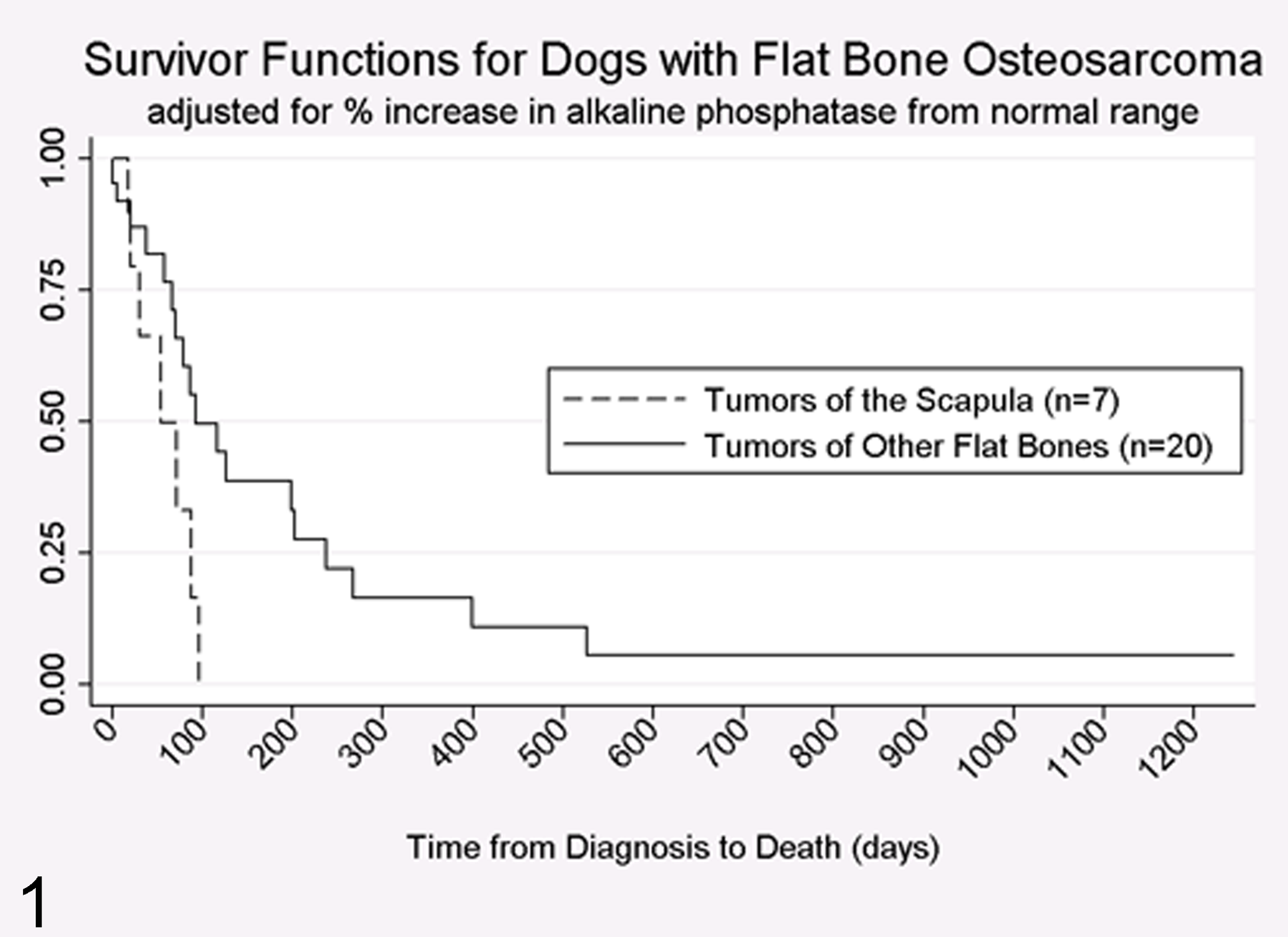
Survivor functions for dogs with flat bone osteosarcoma.
Discussion
The majority of dogs in this study were large breed dogs and this is consistent with previous reports. 3,7,10,13 No cases were identified in giant breeds and the lack of giant breed dogs may reflect a lack of popularity of giant breed dogs during this study period or, alternatively, may support a previous finding that giant breed dogs are more likely to develop appendicular osteosarcoma than axial osteosarcoma and are therefore underrepresented when only axial osteosarcomas are considered. 10,12
The mean age at diagnosis of 8.6 years in this report is consistent with the previously reported mean age of dogs with osteosarcoma of 7 to 8 years. 3,7,10 Females were slightly overrepresented in this study; however, the sex distribution found in this study was similar to the sex distribution for all biopsies submitted between January 2004 and December 2009. Most previous reports have shown males to be more frequently diagnosed with osteosarcoma, 3,7 but few recent veterinary reports have shown overrepresentation of females. 10,18
The median survival time in this study was 12 weeks with a 1-year survival rate of 17.0%. This is similar to previous reports of median survival times and 1-year survival rates for appendicular osteosarcomas 3,4,16,19 and contradicts the suggestion that axial osteosarcomas have a more favorable prognosis. 10 However, due to the retrospective nature of this report, the treatment protocols were not standardized and the reason for euthanasia was not always available from the medical records. It is possible, then, that the mean survival times in this report are underestimates of the actual mean survival times of canine osteosarcomas of the pelvis, scapula, vertebrae, rib, and sternum.
Several reports have examined the relationship between anatomic location of osteosarcoma and prognosis. Mandibular location was significantly and directly associated with increased survival time in univariate analysis with a median survival time of 165 days compared with a median survival time of 120 days for all osteosarcomas in the study. 9 There was a trend toward longer survival times with 3 cases of scapular osteosarcoma despite a 67% metastatic rate at diagnosis. In addition, Heyman et al 10 reported an increased metastatic rate with rib and cranial osteosarcomas and a lower metastatic rate with osteosarcomas arising from the mandible and maxilla. In the present study, data on metastasis was not consistently available so this aspect of the disease was not addressed; however, it was found that a scapular location of osteosarcoma was significantly and inversely associated with mean survival time with a 2.8 times increased hazard for death compared with osteosarcomas originating from the other locations.
Serum ALP level at diagnosis has previously been shown to correlate with survival in canine appendicular osteosarcoma, 5,6 although the biological explanation for the correlation remains unknown. In human patients, an increased serum ALP level at the time of diagnosis is inversely related to survival 15 and directly related to the likelihood of recurrence following treatment. 2,21 Furthermore, human patients with appreciable metastatic disease at the time of diagnosis are more likely to have increased ALP levels than patients without appreciable metastatic disease. 1 The present study confirmed a significant inverse relationship between serum ALP levels and survival time. Controlling for tumor location, every 100% increase in ALP level led to a 1.7 times increase in the hazard for death.
The clinical value of classification into histopathologic subtypes remains questionable. Loukopoulos and Robinson 14 found significant differences in tumor grade and score between different subtypes, but no association between histopathologic subtype and metastatic status or between subtype and survival time. Kirpensteijn et al 11 also found no associations between prognosis and subtype and they deemed division into subclasses to be unwarranted. The present study showed no significant association between subtype and survival for canine osteosarcomas of the sternum, rib, vertebrae, pelvis, and scapula. However, almost 75% of tumors in this study were classified as osteoblastic so this may have predisposed to a type II statistical error in which small sample size led to a finding of no significance where one actually existed.
The veterinary literature on grading of osteosarcomas remains divided. Some authors have shown no relation between prognosis and grade. 9,20 In contrast, Kirpensteijn et al showed significantly better prognosis for grade I and grade II OS when compared with grade III osteosarcoma using a new classification system. 11 However, there was insufficient description of the criteria used in the new grading system to allow its reproduction. 11 Loukopoulos and Robinson found that primary osteosarcoma that had metastasized had a higher grade on histologic examination than did primary osteosarcomas that had not metastasized. 14 In this study, neither tumor grade nor any of the individual histological parameters was associated with survival time. Time to metastasis and occurrence of metastasis were not able to be assessed in this study due to the retrospective nature so no conclusions could be drawn related to the association between grade and metastasis. However, our results suggest that in these specific types of osteosarcomas, histologic parameters and grade are not predictive of outcome.
Two major limitations to grading of tumors include the subjective nature leading to interobserver variation and tumor heterogeneity leading to inaccurate assessment from small samples. Tumor heterogeneity may present a real concern, however, especially in osteosarcoma samples where, in addition to normal variation between areas of the tumor, there is also variation between the amount and the location of osteoid production by the tumor. Further investigation into the variation and production of osteoid and its relationship and potential effect on histologic grading in osteosarcomas is warranted.
Additional limitations of this study include its largely retrospective nature leading to incomplete clinical data and follow-up, small sample size, and a wide variety of diagnostic and treatment protocols. In addition, all of the histologic samples were reviewed by a single reviewer to decrease interobserver variation; however, this can also introduce bias. Finally, a large number of cases reviewed were referral biopsy reports leading to a higher than normal number of animals that were lost to long-term follow-up.
Conclusion
For canine osteosarcoma of the vertebra, sternum, ribs, scapula, and pelvis, histopathological features, classification, and grade do not appear to be rigorous predictors of survival. The production of osteoid by these tumors may make grading and scoring of histologic features difficult by creating large variations between individual fields. In contrast, increased ALP levels and tumor location in the scapula were significantly associated with decreased survival times. Tumors of scapular origin may show decreased survival times as a result of delayed diagnosis. Tumors in this region may be relatively larger and present for longer periods of time before development of clinical signs or identification by owners and referring veterinarians.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
