Abstract
An alpaca was presented with a history of respiratory difficulty and death. Histology of the phrenic nerves and diaphragm revealed degenerative changes consistent with denervation atrophy, and a diagnosis of diaphragmatic paralysis was established. No gross or histological abnormalities were observed in the spinal cord or other organs. The etiology of the phrenic nerve neuropathy could not be determined. The need to examine phrenic nerves and diaphragm in camelids with respiratory distress is emphasized, as failure to examine these samples will preclude a diagnosis of diaphragmatic paralysis.
A 6-month-old, 12-kg female alpaca cria was presented for postmortem examination to the San Bernardino Branch of the California Animal Health and Food Safety laboratory, University of California, Davis. The animal had a 24-hour history of respiratory distress with paradoxical abdominal respiration and reduced air flow from the nostrils, followed by 4-limb symmetric ataxia and death. The animal had been thoroughly examined clinically by an experienced camelid clinician, including but not limited to evaluation of sensation, muscle tone, and weakness in the 4 limbs. These parameters were found to be reduced. No clinical signs consistent with pain were observed. No hematology or clinical chemistry was performed. This cria had no history of previous illness, and all other animals in the herd were healthy at the time of its death. The ranch had a history of 4 crias with similar clinical signs in the previous 3 years; of those, 3 animals recovered, and 1 died (no postmortem examination was performed on the latter). To the best of the owner’s and submitting veterinarian’s knowledge, these 4 animals were not related to each other or to the animal with diaphragmatic paralysis described in this report. Given the clinical signs of the current and previous cases, the submitting veterinarian made a clinical diagnosis of diaphragmatic paralysis due to possible myelopathy.
A full postmortem examination was performed approximately 6 hours after death. In particular, right and left external, middle, and inner ears; several peripheral nerves, including both phrenic, sciatic, vagus, and intercostal nerves; and several muscles, including the diaphragm and intercostal muscles, were carefully examined. Sampling of phrenic nerves included all segments (from origin to end) of both nerves. Choanal atresia was specifically looked for. The whole brain and spinal cord were examined in situ, and half of the brain and the whole of the spinal cord were sliced at 0.5-cm intervals and examined after formalin fixation. At postmortem examination, the carcass was in good nutritional condition and was well fleshed, with adequate amount of fat reserves and in mild state of postmortem decomposition. The lungs were diffusely and mildly congested; samples from all lobes of both lungs collected for histopathological examination floated in formalin. No other gross abnormalities were observed in any of the organs examined. The cerebellum-to-whole-brain ratio was found to be within normal range.
Differential Diagnosis
Respiratory distress followed by death can occur in alpacas and other animals due to bacterial (eg, Pasteurella spp., Escherichia coli) and parasitic (eg, Dictyocaulus viviparous) pneumonia, airway obstruction, neoplasia of lung, airways or mediastinum, pneumothorax, acute pulmonary edema, severe anemia, acute cardiac dysfunction due to toxicosis (eg, oleander, ionophors, gossypol), myocarditis due to bacterial (eg, E. coli) and parasitic (eg, Sarcocystis spp.) agents, diaphragmatic paralysis, diffuse muscular disease (eg, vitamin E and selenium deficiency), and several toxicosis (eg, heavy metals and several organic compounds). Diaphragmatic paralysis is a relatively uncommon medical condition in animals that has only recently been described, for the first time, in alpacas. 4 Bronchopneumonia, airway obstruction, neoplasia, pneumothorax, and acute pulmonary edema were ruled out due to the absence of any gross abnormalities. Grossly, the differentials for the clinical respiratory distress syndrome and death of this alpaca included diaphragmatic paralysis and acute interstitial pneumonia.
Microscopic Findings
Samples from liver, kidney, spleen, small intestine, colon, lungs, adrenal glands, heart, skeletal muscles (including diaphragm and muscles from the back, neck, intercostal spaces, and 4 legs), peripheral nerves (including left and right phrenic, sciatic, and vagus nerves) were collected and fixed in 10% buffered (pH 7) formalin overnight. Half of the brain and the whole of the spinal cord were also collected and fixed whole in the same fixative for 7 days. Blocks of brain were obtained from cerebral cortex, corpus striatum, thalamus, midbrain at the level of cerebral colliculi, pons, anterior cerebellar peduncles, cerebellum, and obex. Blocks were also obtained from all cervical, thoracic, lumbar, and sciatic spinal cord segments. All the tissues were processed routinely for the production of 5-μm-thick hematoxylin and eosin sections. Selected sections of nerves were also stained with Luxol fast blue–Holmes. Histologically, the diaphragm revealed multifocal areas of angular atrophy of a small number of contiguous myofibers and fiber size variation, with central nuclei. Scattered necrotic fiber segments with loss of cytoplasm and striations, cytoplasmic vacuolation, and pyknotic or karyorrhectic nuclei were also seen (Fig. 1). Occasionally, repair attempts consisting of nuclear rowing were observed.
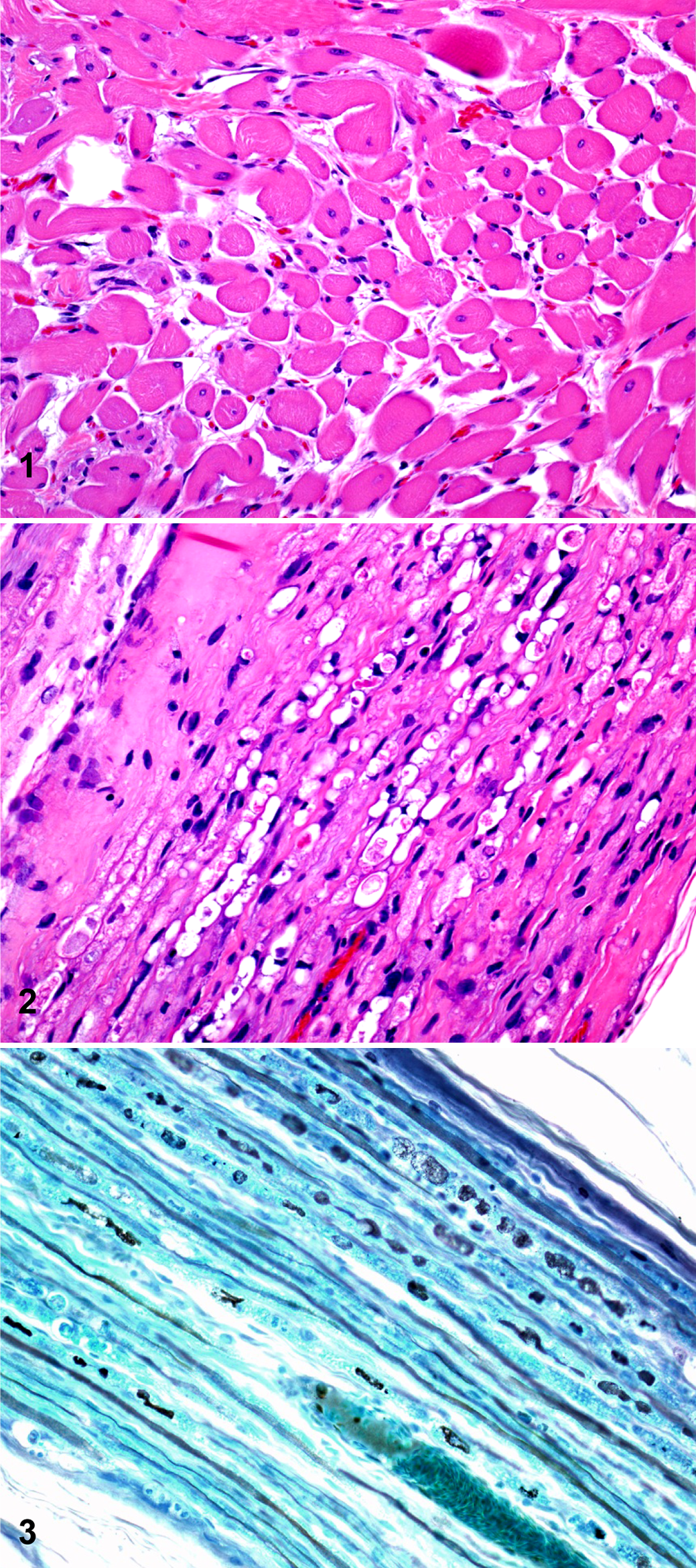
Alpaca. Diaphragm. Diaphragmatic paralysis. Angular atrophy, size variation of myofibers, and central nuclei are evident. HE.
Both phrenic nerves exhibited multifocal and marked degenerative changes consisting of dilated myelin sheaths, swollen axons and occasionally foamy macrophages within dilated myelin sheaths (digestion chambers) (Figs. 2, 3). The changes in the phrenic nerves were similar in nature and severity throughout the whole length and width of both nerves. No histological changes were observed in the nerve interstitium, including connective tissue and blood vessels. No other significant histological abnormalities were observed in any of the tissues examined.
Ultrastructural Findings
Samples of formalin-fixed, paraffin-embedded diaphragm and nerves (both phrenic, vagus, and sciatic) were deparaffinized in xylene, placed in half strength Karnovsky’s fixative, and processed routinely for transmission electron microscopy (TEM). TEM of diaphragmatic muscle revealed disruption of Z lines, central nuclei, and severe dilation of the rough and smooth endoplasmic reticulum. TEM of phrenic nerves revealed dissociation of the myelin sheaths that left large spaces occasionally occupied by electron-dense membrane fragments or large macrophages with multiple lysosomes containing mostly membrane debris.
Ancillary Tests
Small intestinal contents were processed by a capture ELISA for alpha, beta, and epsilon toxins of Clostridium perfringens and for toxins A and B of Clostridium difficile using commercial kits (BioX, Belgium, and Techlab, Virginia, respectively) and according to the manufacturers’ instructions. No C. perfringens or C. difficile toxins were detected.
The following tests were performed according to the California Animal Health and Food Safety’s standard operating procedures. Samples of liver and lung were aseptically collected and processed for aerobic and anaerobic bacteriology on blood agar plates at 37°C for 48 hours. Small intestinal contents were cultured aerobically and anaerobically on blood agar and anaerobically on cycloserine-cefoxitin-fructose. No significant aerobic or anaerobic bacterial pathogens were isolated. The liver was analyzed for heavy metals (lead, manganese, cadmium, copper, iron, tin, zinc, molybdenum, arsenic, and mercury), selenium, and vitamin E. Whole blood was analyzed for selenium, and serum was processed for vitamin E and trace elements (including calcium, copper, iron, magnesium, phosphorus, potassium, sodium, and zinc). Heavy metals and vitamin E concentrations were within expected ranges in the liver, blood, and serum. Selenium in liver was within a reported adequate range, 9 but the concentration of this metal in blood was slightly below an adequate range for camelids (this animal: 0.078 ppm; reference range: 0.08–0.50 ppm). 9 The trace element screen of serum revealed that the zinc concentration was slightly below a reference range for camelids (this animal: 0.23 ppm; reference range: 0.30–1.50 ppm) as well. 9 One half of the brain was collected and stored frozen until analyzed for cholinesterase activity, which was found to be within expected range for this species. The liver was tested for 42 organophosphorus insecticides. None of the organophosphorus insecticides included in our routine diagnostic screen were detected in the liver. In addition, a toxicant screen by gas chromatography-mass spectrometry was performed on a liver sample, but no unusual compounds were detected in the liver by this test.
Diagnosis
Based on the degenerative lesions observed in the diaphragm and both phrenic nerves and the absence of lesions in the spinal cord and other tissues of this animal, a diagnosis of denervation atrophy of the diaphragm due to primary degeneration of both phrenic nerves was established. The cause of the phrenic nerves degeneration could not be determined.
Discussion
Diaphragmatic paralysis results in the limited ability to generate negative intrathoracic pressures during inspiration, which in turn results in respiratory dysfunction. The pulmonary gas exchange and alveolar ventilation in cases of diaphragmatic paralysis can be maintained only through activation of inspiratory intercostal muscles, active expiratory muscle contraction, and passive elastic recoil properties of the lung and chest wall. 8 However, this mechanism is usually not enough to keep an acceptable level of oxygenation of the blood and tissues, which seems to have been the case with this alpaca.
Based on the clinical observation of concurrent respiratory distress and 4-leg ataxia, diaphragmatic paralysis due to a multifocal or cervical spinal lesion was initially suspected in this alpaca. Extensive gross and microscopic examination of the whole spinal cord, with special emphasis in the segments included between C4 and C7 (the area or origin of the phrenic nerves), however, did not reveal significant lesions in this organ. It is possible that the ataxia observed clinically in this animal was consequence of general hypoxia and/or weakness related to diaphragmatic paralysis and not to a medullary lesion. Also, several peripheral nerves were examined, but lesions were found in only the phrenic nerves. This suggests that this neuropathy affected specifically the phrenic nerves. We cannot completely rule out, however, that focal and/or subtle lesions were present in nerves or nerve segments not examined in this study.
The lesions observed in the diaphragm of this alpaca were characteristic of denervation atrophy, which, coupled with the absence of lesions in the spinal cord, suggests that the degenerative lesions in both phrenic nerves were the primary event that led to diaphragmatic degeneration and paralysis. Nevertheless, to further rule out primary diaphragmatic myopathy due to nutritional deficiency, we measured vitamin E and selenium (the deficiency of which can cause degenerative myopathy) in the liver, blood, and serum. Except for a slightly below-normal selenium level in blood, all other parameters were within normal ranges. Given the adequate concentration of selenium in the liver, the slightly low concentration in whole blood was considered to be an incidental finding in this case. Furthermore, degenerative lesions in muscles other than diaphragm were not observed. These results suggest that deficiency of selenium or vitamin E were not responsible for the diaphragmatic myopathy.
Diaphragmatic paralysis has been described in only a few animals, including a pony, 2 a dog, 6 a llama, 3 11 alpacas, 4 and 3 cats. 6 Both in animals and humans, diaphragmatic paralysis has been attributed to trauma or compression of the spinal cord, phrenic nerve neuropathy, or myopathy.1,3,4
Diaphragmatic paralysis associated with neuropathy of phrenic nerves was previously described in a llama 3 and in 2 alpacas. 4 The etiology of the lesions was not determined in any of these cases. The etiology of the neuropathy of the phrenic nerves in the present study also remains undetermined. However, in 2 of the alpacas with phrenic nerve neuropathy previously reported, 4 there were lesions in the spinal cord, and it was speculated that these cord lesions were the primary abnormalities leading to phrenic nerve neuropathy and diaphragmatic muscle degeneration.
A number of toxicants can cause peripheral neuropathies; these include metals (arsenic, lead, manganese, mercury and tin) and organic compounds (6-amino-nicotinamide, azides, carbon tetrachloride, doxorubicin, chloramphenicol, cyanide, ethanol, methanol, methyl bromide, organophosphorus insecticides, and 3-nitroproprionic acid). 7
Extensive toxicologic testing did not suggest a chemical cause for the phrenic nerve neuropathy in our alpaca. Although testing was not specific for some of the listed toxicants, lesions caused by these chemicals would not be expected to be limited to the phrenic nerve. In addition, the history did not suggest exposure to any of these toxicants.
Because 4 previous cases of apparent diaphragmatic paralysis had occurred in the same herd, it was initially thought that this may be an inherited condition. However, further investigation of these cases showed that none of these animals were related to each other or to the case presented here, which would suggest that a genetic cause is unlikely. However, a hereditary predisposition cannot completely be ruled out, and further work is required to investigate this possibility. An autosomal-dominant peripheral neuropathy called “hereditary neuropathy with liability to pressure palsies” has been described in humans. 5 To the best of our knowledge, this condition has never been diagnosed in animals. This condition is characterized by focal tomacular degeneration of the affected nerves, a change not observed in the phrenic nerve of this alpaca.
The postmortem diagnosis of diaphragmatic paralysis associated with phrenic nerve neuropathy can be challenging. It is critical to collect samples of phrenic nerves and diaphragm for histological examination. Because in this and in the previously reported cases of diaphragmatic paralysis in a llama 3 and 2 alpacas, 4 histological lesions were observed only in these 2 tissues, failure to examine them histologically will most likely result in a missing diagnosis.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
