Abstract
Objective
Mammography and ultrasound are commonly used for early detection of breast cancer; however, they have several limitations and are outperformed by magnetic resonance imaging for screening and diagnosis because of its higher sensitivity. This study aimed to evaluate female awareness of magnetic resonance imaging as a tool for early breast cancer detection and to enhance early-stage diagnosis.
Methods
A cross-sectional study was conducted using an online questionnaire. Data were analysed using Statistical Package for the Social Sciences software. Awareness was categorised as poor or good.
Results
A total of 498 women participated in this study. Although 98% of the participants recognised the importance of early breast cancer detection, only 42.6% were aware of the role of breast magnetic resonance imaging. Awareness of the ability of magnetic resonance imaging to detect intraductal carcinoma and small invasive tumours, particularly in dense breast tissue, was moderate, with a mean awareness score of 2.5 ± 1.1 out of 4. Awareness was significantly higher among older women, those with family history of breast cancer and those who practised self-examinations or had prior magnetic resonance experience (p ≤ 0.002).
Conclusions
This study highlights a deficiency in awareness regarding the value of magnetic resonance imaging in breast cancer screening, particularly among young women with dense breast tissue and those without prior exposure to magnetic resonance imaging.
Keywords
Introduction
Breast cancer remains a major health concern, ranking as the second most common cancer and the second leading cause of cancer-related mortality among women. Screening plays a pivotal role in reducing breast cancer mortality. According to the 2023 statistics of the American Cancer Society (ACS), 1 one in eight American women will be diagnosed with breast cancer during their lifetime. In Saudi Arabia, 3777 breast cancer cases were reported among women in 2022.2,3 To address the high incidence of breast cancer, established guidelines recommend annual screening mammography starting at 40 years of age. 4 However, as breast cancer risk varies, personalised approaches are advocated, including the incorporation of magnetic resonance imaging (MRI) for women with a 20%–25% lifetime risk and those with increased breast density.4,5
Breast MRI is a nonionising imaging technique that uses radio waves and powerful magnets to create detailed three-dimensional images. 6 MRI is particularly sensitive and effective for individuals with a genetic or familial predisposition to breast cancer as well as for women with increased breast density. 6 Despite its advantages, MRI poses challenges, particularly regarding the economic feasibility of widespread population-based screening. Awareness campaigns and educational initiatives are essential to bridge the knowledge gap and inform women about the benefits and limitations of various screening methods. Female awareness directly influences their decision-making regarding breast cancer screening options. 7
Understanding the level of awareness can help guide improvements in educational programmes and promote the use of MRI as a valuable tool for early detection among women at risk. MRI screening for women at high risk improves the detection of early breast cancer by more than 50% compared with mammography and ultrasound combined. 8 Furthermore, MRI has been shown to be more sensitive than mammography and ultrasound in detecting intraductal carcinoma and small invasive tumours, particularly in high-risk groups. 9 Quality-assured MRI equipment can even identify the smallest lesions, making it an important tool for early detection in this population.10,11
Despite significant advances in breast cancer screening, the role of MRI in early tumour detection remains under-recognised among women in Saudi Arabia. Although mammography is widely promoted as a standard screening tool, MRI offers higher sensitivity in detecting early-stage tumours, particularly among high-risk women. However, little is known about the level of awareness among Saudi women regarding the potential of MRI as an effective complementary tool for early detection. This lack of evidence highlights a critical gap that may limit timely diagnosis and the adoption of advanced screening approaches. Therefore, this study aimed to assess female awareness of early breast cancer detection using MRI, enhance diagnosis at early stages and contribute to the development of targeted educational interventions. By correlating the results with existing international literature, the study also aimed to determine whether awareness patterns in Saudi Arabia align with or differ from global trends. Ultimately, the study seeks to improve early breast cancer detection strategies and promote informed decision-making among women at risk.
Methods
Ethical approval for this cross-sectional survey was obtained from the Institutional Review Board of King Saud University Medical City (Approval Project No. E-24-8732) in April 2024. The study aimed to assess awareness among Saudi women regarding the early detection of breast cancer using MRI, with the primary objective of evaluating their knowledge and awareness levels. The study was conducted in accordance with the principles of the Declaration of Helsinki (1975), as revised in 2024. The reporting of this study conforms to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. 12
Study design
This study was designed as a prospective observational cross-sectional study.
Setting and study population
Inclusion criteria
This study included Saudi women aged 35 years or older, as this demographic represents the target age group for breast cancer screening and is associated with an increased risk of breast cancer. For a population of over 1,000,000 Saudi women, a minimum sample size of 385 participants (using a convenience sampling technique) was required to achieve a 95% confidence level with a 5% margin of error.
The study included both married and single women to ensure a diverse representation of marital and social statuses. Potential sources of bias were identified and addressed through careful study design, standardised data collection procedures and appropriate statistical adjustments.
Exclusion criteria
Women under the age of 35 years, those with metal implants and individuals with claustrophobia were excluded, as these factors could introduce confounding variables or affect participants’ suitability for MRI-based breast cancer screening.
Data collection method
Data were collected using a structured online questionnaire consisting of a comprehensive set of 13 questions assessing awareness levels among women regarding the early detection of breast cancer through MRI, along with demographic questions. The questionnaire was developed by the authors and underwent validity and reliability testing. To ensure inclusivity and accessibility, the questionnaire was made available in both Arabic and English, facilitating engagement among individuals with different language preferences. The questionnaire was disseminated through an extensive social media campaign that reached potential participants across various demographics. This multifaceted strategy aimed to enhance the reach and engagement of the survey. Participants were invited to complete the questionnaire between May and July 2024 via Google Forms, an online platform that provides flexibility and convenience for respondents with diverse schedules. Consent to participate was obtained from all participants, and all participant details were de-identified.
Questionnaire
The questionnaire comprised demographic items and 13 questions designed to assess participants’ awareness of breast cancer and the role of MRI in early detection.
Marital status:
Married
Single
Age:
35–40 years
>40–45 years
>45 years
Do you use contraceptive drugs?
Yes
No
Have you ever had breast cancer?
Yes
No
Does anyone in your family have breast cancer?
Yes
No
Do you self-examine your breasts?
Yes
No
Do you know about breast MRI?
Yes
No
Do you suffer from claustrophobia?
Yes
No
Do you have any metal implants?
Yes
No
Do you think that early diagnosis aids in the detection of breast cancer?
Yes
No
Have you ever used breast MRI for early diagnosis?
Yes
No
Do you know that MRI can detect tiny tumours that cannot be felt and may not appear on a mammogram?
Yes
No
Do you know that MRI can detect invasive breast cancer in some patients, especially in those with dense breasts, years before detection by mammography?
Yes
No
Testing the validity of the questionnaire
Pearson’s correlation coefficient was used to assess the validity of the survey. Responses to each item from each participant were summed to obtain a ‘Composite Score’, representing the overall response pattern. The relationships between each item and the ‘Composite Score’ were then examined to determine the validity of individual items.
Testing the reliability of the questionnaire
Cronbach’s alpha was used to assess the internal consistency of the questionnaire, which measures the reliability of a set of items. 13 The alpha coefficient ranges from 0 to 1, with higher values indicating greater agreement among the items and therefore higher internal consistency. 13
Statistical analysis
Data were collected, reviewed and analysed using IBM SPSS Statistics, version 21. 14 All statistical tests were two-tailed, with significance set at p ≤ 0.05. The overall awareness level regarding MRI was assessed by summing the discrete scores for the different correct awareness items. Awareness was categorised as poor if a participant scored below 60% of the overall score and good if the score was 60% or higher.15–17 Descriptive analysis was conducted using frequency distributions and percentages to summarise study variables, including participants’ demographic data and personal and family history of breast cancer. Participants’ awareness and practices regarding MRI were tabulated, and the overall awareness level was presented graphically. Cross-tabulation was performed to identify factors associated with awareness and practices regarding MRI, using the Pearson chi-squared test for significance. The exact probability test was applied in cases with small frequency distributions.
Results
A total of 498 eligible females completed the survey, with ages ranging from 35 to over 45 years (mean age: 42.6 ± 10.4 years). Of these, 150 (30.1%) were aged over 45 years. The majority of participants (398, 79.9%) were married, and 106 (21.3%) reported the use of contraceptive drugs. Only 11 women (2.2%) had a history of breast cancer, while 122 (24.5%) had a family history of the disease (Table 1, supplementary file).
Female awareness about early detection of breast cancer using MRI.
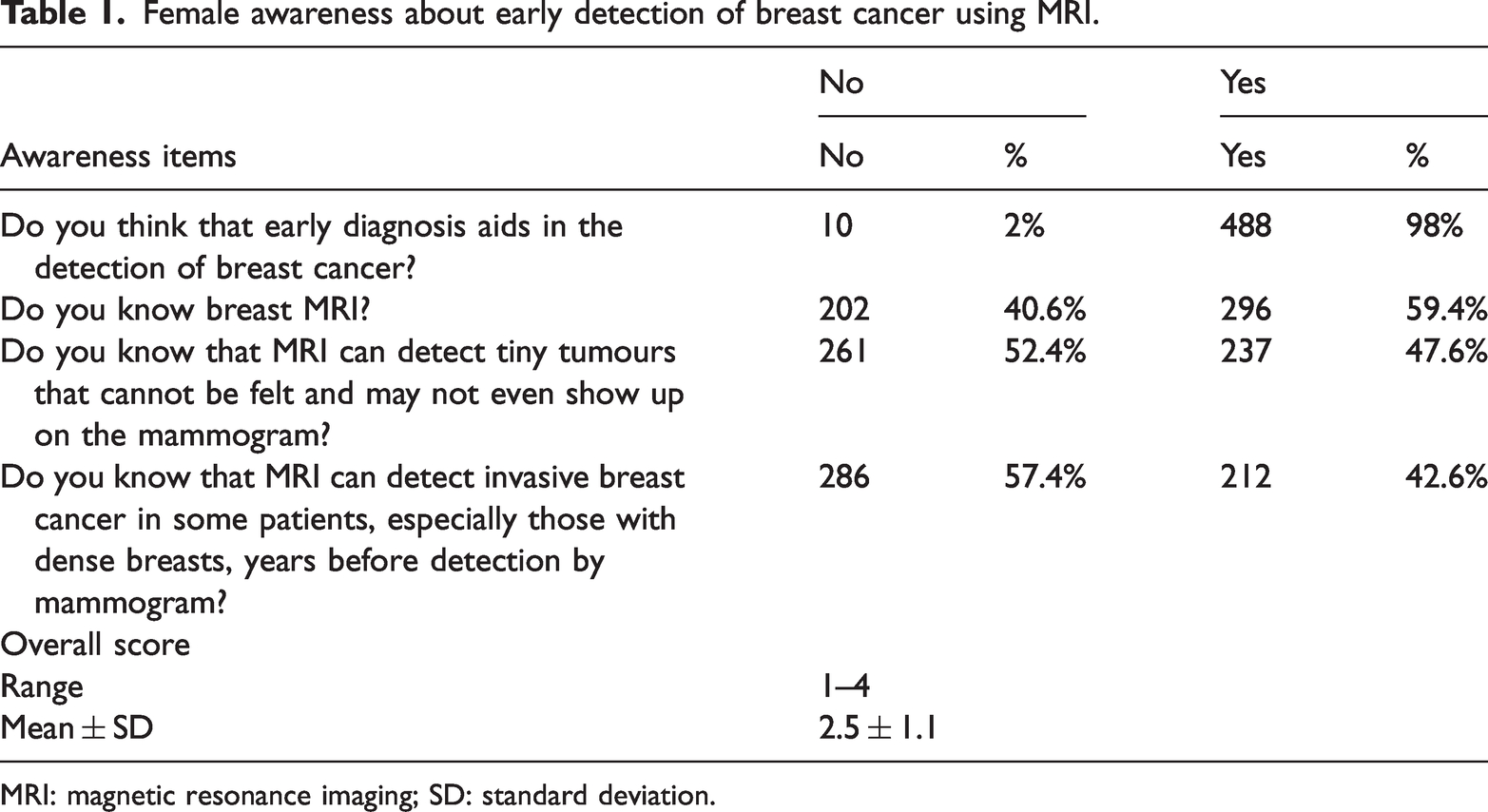
MRI: magnetic resonance imaging; SD: standard deviation.
Validity of the questionnaire
As shown in Table 2 (supplementary file), the questionnaire’s validity test revealed significant positive correlations between each item and the overall Composite Score.
Factors associated with female awareness of MRI and its role in early diagnosis of breast cancer.

p values were calculated using Pearson X2 test.
p < 0.05 (significant)
Exact probability test.
MRI: magnetic resonance imaging.
Reliability of the questionnaire
Cronbach’s alpha for internal consistency was 0.902, indicating a high degree of reliability (Table 3, supplementary file).
Factors associated with woman practice of MRI for early breast cancer diagnosis.

p values were calculated using Pearson X2 test.
p < 0.05 (significant)
Exact probability test.
MRI: magnetic resonance imaging.
Table 1 presents the awareness levels of participants regarding the early detection of breast cancer using MRI. Among the 498 women surveyed, 488 (98%) believed that early diagnosis aids in breast cancer detection. A total of 296 (59.4%) women were aware that MRI can detect tiny tumours that may not be palpable or visible on a mammogram, and 237 (47.6%) were aware that MRI can detect invasive breast cancer in some patients, particularly those with dense breasts, years before detection by mammogram. Additionally, 212 women (42.6%) were aware of breast MRI. The overall awareness score ranged from 1 to 4, with a mean score of 2.5 ± 1.1.
Figure 1 (supplementary file) illustrates the overall level of awareness. Among the participants, 265 (53.2%) demonstrated good awareness of MRI and its role in breast cancer diagnosis, whereas 233 (46.8%) had poor awareness.
Figure 2 (supplementary file) depicts participants’ practices regarding breast self-examination and MRI use. Among the participants, 35 (37.2%) reported performing breast self-examination, while 19 (20.2%) had utilised breast MRI for early diagnosis of breast conditions.
Table 2 shows the factors that considerably influence female awareness of MRI and its role in the early diagnosis of breast cancer. Among older participants (aged >45 years), 72.7% had good awareness, compared with 37.4% among younger women (aged 35–40 years) (p = 0.001). Notably, women with a history of breast cancer demonstrated good awareness of MRI’s role in early diagnosis, whereas only 52.2% of those without a history of the disease reported good awareness (p = 0.002). Similarly, 78.7% of women with a family history of breast cancer had good awareness, compared with 44.9% among those without such a history (p = 0.001). Breast self-examination habits also influenced awareness (p = 0.001), with 65.2% of women who regularly performed self-examinations demonstrating good awareness, compared with 46.0% among those who did not. Furthermore, among participants who had used MRI, 80% reported good awareness, compared with 46.5% among those who had never used the technology (p = 0.001) (Table 2).
Table 3 presents factors associated with the use of breast MRI for early breast cancer diagnosis among women. Among participants aged over 45 years of age, 36.0% reported using MRI, compared with 7.6% of women aged 35–40 years (p = 0.001). Contraceptive use also influenced MRI utilisation; 23.0% of nonusers underwent MRI, whereas only 9.4% of contraceptive users did so (p = 0.002). All women with a history of breast cancer reported MRI use, compared with 18.3% of those without a history of the disease (p = 0.001). Additionally, 44.3% of women with a family history of breast cancer had utilised MRI, whereas only 12.2% of those without a family history reported the same (p = 0.001). Finally, among women who performed regular breast self-examinations, 45.5% underwent breast MRI, compared with only 4.8% of those who did not practice self-examination (p = 0.001).
In the multivariable logistic regression analysis (Table 4), age above 45 years, family history of breast cancer, breast self-examination and prior breast MRI use were identified as significant independent factors associated with good awareness, with adjusted odds ratios remaining statistically significant. Although univariate analysis showed a significant association of awareness with the age of 40 years, this link disappeared when other factors were included in the model. Similarly, a weak but significant correlation between awareness and contraceptive use was observed in univariate analysis, but this effect was no longer significant in the multivariable model. Neither crude nor adjusted analysis demonstrated a significant relationship between awareness and marital status. Limited variation in awareness among women with a personal history of breast cancer prevented meaningful analysis within this group.
Logistic regression analysis showing COR and AOR for factors associated with good awareness of MRI.

MRI: magnetic resonance imaging; COR: crude odds ratio; AOR: adjusted odds ratio; CI: confidence interval.
Discussion
This study aimed to assess female awareness of breast MRI for early breast cancer detection and its potential to improve diagnosis at early stages. Early detection during the asymptomatic phase can improve survival by 27%–47% compared with detection at later symptomatic stages. 18 Studies have shown that women with a personal history of breast cancer benefit greatly from additional screening using breast MRI, which has a high diagnostic success rate and acceptable positive biopsy outcomes.18,19 MRI screening not only enhances the cancer detection rate but also facilitates the identification of biologically aggressive and early-stage breast tumours,19,20 particularly in females with mammographically dense breasts. 5
The findings of this study revealed a significant awareness gap among Saudi women regarding the role of MRI in the early detection of breast cancer. Although nearly all participants understood that early diagnosis is crucial, less than half were aware that breast MRI serves as a diagnostic tool. Awareness of its specific benefits was even lower: just over half of the participants recognised that MRI could detect small tumours not visible on mammograms, and approximately half of them were aware that it could identify invasive breast cancer, particularly in patients with dense breast tissue. These results are consistent with those of other studies in the region, where awareness of advanced diagnostic tools such as MRI is generally limited. For example, a study conducted in the United Arab Emirates found that although a high percentage of women understood the importance of early detection, only 30% were aware of the role of MRI in breast cancer diagnosis. 21 Although global awareness of early detection methods, including MRI, is improving, considerable gaps remain, particularly in countries with limited access to advanced diagnostic technologies. In developed nations, studies indicate higher awareness, with 60%–70% of women recognising the role of MRI in detecting breast cancer, especially among high-risk populations. 22 However, even in these countries, awareness is often influenced by factors such as age, education level and access to healthcare services, highlighting the need for targeted public health education campaigns to bridge knowledge gaps both locally and globally. Our findings are consistent with those of previous studies in Saudi Arabia, where awareness of advanced breast cancer detection methods remains low. One study 23 reported that although 90% of Saudi women were aware of mammography, only 25% had heard of breast MRI, aligning with the relatively low MRI awareness observed in our study. 23 Similarly, a study conducted in Jeddah in 2013 found that although 85% of women were aware about mammography, only 30% were familiar with MRI’s ability to detect breast cancer. 24
A study conducted in 2021 25 concluded that most women prefer screening with MRI. Females’ perceptions of MRI and mammography are influenced by the specific screening strategy they undergo. When comparing contrast-enhanced spectral mammography (CESM) with MRI, most high-risk women preferred CESM over MRI if both methods offered equivalent sensitivity. 26 Although CESM is often preferred by high-risk women due to its shorter duration and greater accessibility, it involves exposure to ionising radiation, which raises particular concern for BRCA-positive women who already carry an elevated lifetime cancer risk. In contrast, MRI avoids radiation, making it a safer option for repeated screening in this population and aligning more closely with international guidelines. Another study reported that CESM may be preferable to MRI in certain contexts. 27 Conversely, a previous study 28 found that women at higher risk of breast cancer who underwent MRI screening primarily preferred MRI over mammography as a screening test. In the American College of Radiology Imaging Network (ACRIN) 6666 study, 29 many women declined breast MRI mainly due to uncertain reimbursement, while claustrophobia was cited less frequently. In well-managed centres, the rate of dropout due to claustrophobia is typically 18.2%, indicating that financial and logistical barriers, rather than the procedure itself, are the main factors limiting MRI uptake in high-risk populations. Numerous studies have assessed female awareness of breast cancer screening and detection, with breast self-examination and mammography being the most widely recognised methods, whereas MRI and computed tomography (CT) are rarely mentioned.23,30,31
Regarding breast cancer screening practices, approximately one-third of females in this study reported performing breast self-examination, whereas only approximately one-fifth had used breast MRI for early diagnosis. MRI usage was highest among older women (aged >45 years), those with a family history of breast cancer and those who regularly performed breast self-examinations. Similar findings have been reported in other studies conducted in Saudi Arabia. In Riyadh, a 2018 study 23 found that although 52.4% of women practised breast self-examination, only 17.5% were aware of breast MRI as a diagnostic tool, and approximately 10% had ever utilised it. Another study in Jeddah reported that only 19.3% of women had ever undergone breast MRI. These findings suggest that although breast self-examination is relatively common, MRI usage remains low, primarily due to limited awareness and access to healthcare services. 24 This emphasises the urgent need to increase awareness and accessibility of advanced diagnostic methods such as MRI, which are essential for early detection, particularly among high-risk populations. Awareness of breast MRI can be improved through targeted education, integration into clinical consultations, social media outreach, community programmes and collaboration with advocacy groups, alongside providing information on insurance coverage and subsidised screening to enhance accessibility. Internationally, a 2011 study 32 reported that MRI utilisation among patients with breast cancer increased from 3.9% in 2003 to 10.1% in 2005, a rate lower than that observed in the current study. Similarly, a 2018 study 33 found that the reported lifetime MRI screening rate in community practices was less than 20%. Another study in 2014 34 showed that the overall utilisation rate of breast MRI nearly tripled between 2005 and 2009, increasing from 4.2 to 11.5 examinations per 1000 women, with the most rapid increase occurring from 2005 to 2007 (p = 0.02). The most common clinical indications for MRI were diagnostic evaluation (40.3%) and screening (31.7%). Additionally, a 2013 study 35 revealed that 41% of surgeons reported routine MRI use for newly diagnosed patients with breast cancer, a rate higher than that observed in our study.
The findings of this study can guide public health initiatives by identifying awareness gaps and informing targeted educational campaigns to promote the use of MRI among high-risk women. Increased awareness may encourage earlier screening, support timely diagnosis and reduce breast cancer mortality. The results can also inform national screening guidelines, improve access to MRI services and help address cultural and systemic barriers, ultimately strengthening early detection strategies and potentially lowering healthcare costs.
This study has several limitations. First, it relied on self-reported data, which may be subject to recall bias or inaccuracies in participants’ responses regarding their awareness and practices related to breast cancer screening and MRI use. Additionally, the study was conducted using an online questionnaire, potentially excluding women without internet access or those less familiar with digital platforms. Moreover, the use of nonrandom convenience sampling and recruitment through social media may have introduced selection bias, potentially limiting the generalisability of the findings to the broader population.
Conclusions
This study highlights considerable deficiencies in awareness among Saudi Arabian women regarding the use of MRI for early breast cancer detection. Although some participants demonstrated awareness, considerable knowledge gaps remain, underscoring the need for targeted educational initiatives to enhance understanding and promote proactive screening practices. Improving awareness can lead to increased use of MRIs, ultimately facilitating earlier detection, improving outcomes and strengthening breast cancer prevention efforts. Further research and public health initiatives are essential to support the widespread adoption of MRI screening as a valuable tool for breast cancer detection and prevention. In addition, the cost of breast MRI should be carefully considered, and discussions are warranted on whether government funding or subsidised programmes should be implemented to ensure equitable access for high-risk women.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605251395573 - Supplemental material for Awareness of magnetic resonance imaging for early detection of breast cancer: A cross-sectional study
Supplemental material, sj-pdf-1-imr-10.1177_03000605251395573 for Awareness of magnetic resonance imaging for early detection of breast cancer: A cross-sectional study by Meaad M Almusined, Salman M Albeshan, Abdulaziz S Alshabibi, Alaa M Almutairy, Haya A Almujali and Areej S Aloufi in Journal of International Medical Research
Footnotes
Acknowledgements
The authors would like to thank Ongoing Research Funding Program, (ORFFT-2025-116-1), King Saud University, Riyadh, Saudi Arabia, for financial support. The authors also acknowledge the Investigator Support Unit (ISU), Prince Naif Health Research Center, for providing language editing support through Editage (![]() ).
).
Authors’ contributions
Meaad M Almusined contributed to the study concept and design, data analysis, manuscript writing, critical revision of the manuscript and paper submission. Salman M Albeshan, Abdulaziz S Alshabibi and Areej S Aloufi participated in methodology development, literature review and manuscript revision. Alaa M Almutairy and Haya A Almujali contributed primarily to data collection, data analysis, manuscript writing.
Data availability statement
All data generated or analysed during this study are included in this published article and its supplementary information file, including questionnaire links.
Declaration of conflicting interests
The authors declare no conflict of interest.
Consent to participate
All participants provided informed consent.
Consent for publication
The authors have agreed to publication.
Source of support
The authors would like to thank Ongoing Research Funding Program, (ORFFT-2025-116-1), King Saud University, Riyadh, Saudi Arabia, for financial support.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
