Abstract
Arterial catheter blood sampling is widely used among critically ill patients to minimize repeated punctures; however, improper techniques may lead to misleading laboratory results. This case report presents a clinically significant hemoglobin discrepancy observed between blood gas analyzer and automated hematology analyzer during arterial catheter sampling in a patient with cerebral infarction. After catheter placement, the interplatform hemoglobin discrepancy reached 13 g/L despite prior concordance. The discordance was attributed to pre-analytical errors, including inadequate discard volume (4–5 mL) of heparinized saline–contaminated blood, which causes sample dilution. This case underscores that catheter sampling protocols must rigorously focus on dead space clearance to prevent artifactual hemoglobin variations. Such vigilance is particularly critical in hemodynamically unstable patients, in whom erroneous values may directly impact transfusion decisions. Adherence to evidence-based discard volume guidelines, with protocol tailoring based on individual patient factors, constitutes an essential safeguard for test accuracy in critical care settings.
Introduction
As an important laboratory test for emergency patients, hemoglobin (HB) test serves as a critical parameter for anemia assessment and transfusion guidance. 1 In the management of critically ill patients, serial blood sampling for laboratory analysis is required for dynamic monitoring of hematological and biochemical parameters. Conventional repeated punctures using disposable blood collection needles cause pain and anxiety, with skin and vascular damage observed in severe cases. In contrast, arterial indwelling catheters not only enable continuous blood pressure monitoring but also provide convenient vascular access for blood sampling. This eliminates the need for repeated vascular punctures, improves specimen collection efficiency, saves time for other critical interventions, and is thus widely adopted in emergency critical care settings. 2 Herein, we present a case of HB measurement discrepancy between blood gas analyzer (BGA) and automated hematology analyzer (AHA) resulting from arterial catheter sampling errors, and our findings emphasize the key role of standardized sampling protocols in minimizing pre-analytical errors.
Case report
A man in his late 60s was sent to the emergency department of Qingdao Central Hospital for cerebral infarction in June 2024. Following admission, laboratory blood tests were performed. Arterial blood samples (3 mL) were obtained via radial artery puncture using a BD Preset™ arterial blood sampler and analyzed using GEM Premier 5000 BGA (Werfen, USA). Venous blood samples (2 mL) were collected from the antecubital vein using a disposable venous blood collection needle into vacuum tubes, and complete blood count (CBC) was performed using XN-550 AHA (Sysmex, Japan). Blood collection devices and analytical parameters are shown in Table 1.
Blood collection devices and analytical parameters of hemoglobin measurements.

SLS: sodium lauryl sulfate; HB: hemoglobin.
The patient underwent two major surgical procedures on hospital days 2 and 3, including decompressive craniectomy and inferior vena cava filter placement. Subsequently, on day 5, he developed acute upper gastrointestinal bleeding (UGIB). Clinicians suspected that this hemorrhage was triggered by severe brain injury in combination with significant surgical stress. These events culminated in a sharp decline in HB concentrations on day 5. Given the patient’s critical condition, an arterial catheter was placed on day 5 to facilitate continuous hemodynamic monitoring and safe, efficient blood sampling, thereby optimizing resuscitation efficacy (Figure 1). Subsequent blood samples for both laboratory tests were drawn through this catheter. However, over the next 3 consecutive days, discrepancies in HB measurements emerged between the two analytical platforms—AHA and BGA (Table 2). The clinicians began to pay attention to this issue on day 8.
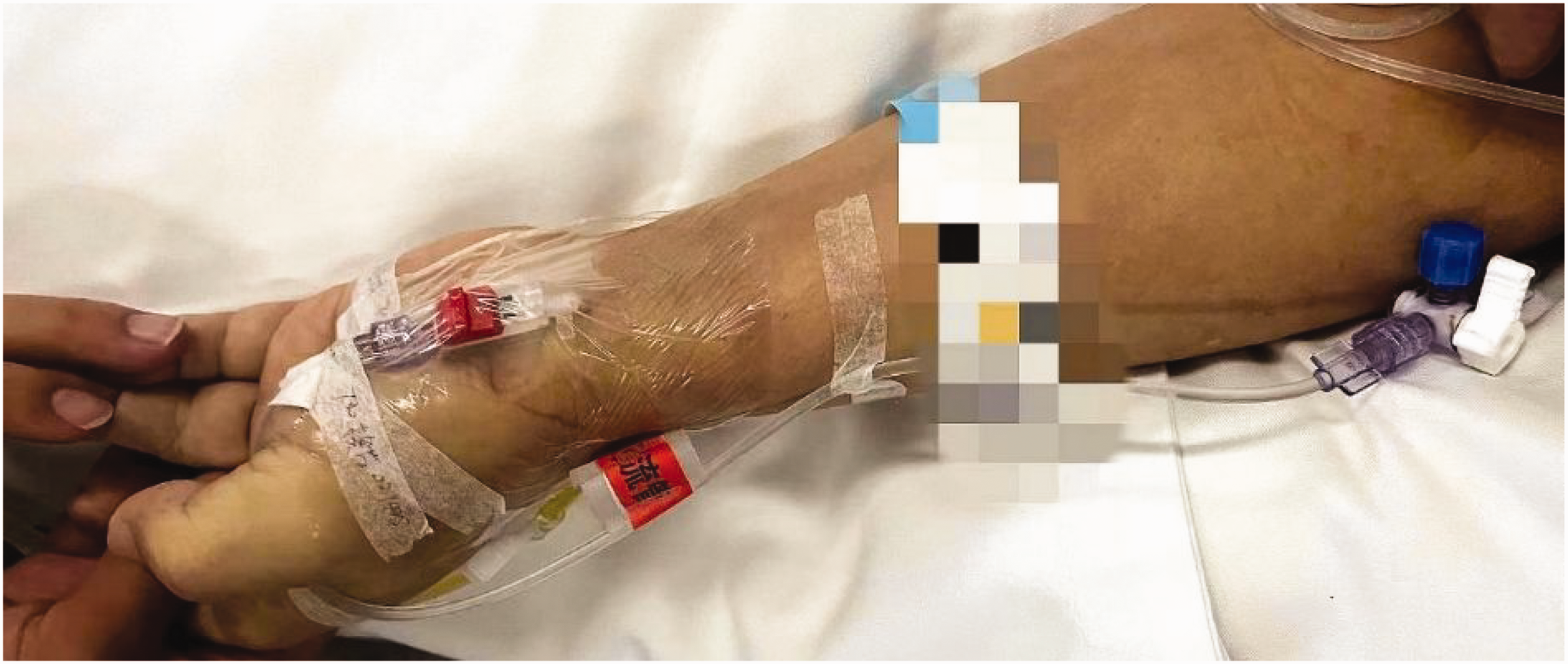
A patient fitted with an indwelling catheter in the radial artery.
Comparison of hemoglobin levels at different time points.

After identifying this issue, the clinical laboratory staff rechecked the blood samples, evaluated the performance of analytical instruments and reagents, and reviewed any human errors in the operational process. We used manufacturer-provided reagents and conducted all tests in strict adherence to the department’s standard operating procedures for the respective instruments and reagents. Daily in-house quality control measures were performed for the instruments, and regular participation in external quality assessment programs was maintained to ensure the accuracy and reliability of the test results. Subsequently, to assess potential methodological discrepancies, repeat measurements were performed immediately after initial analysis using two distinct analyzers for the original aliquots of both blood samples collected on day 8. The results showed that the HB concentrations measured by the two analyzers for each blood sample were consistent with the initial results (Table 3). A difference in HB concentrations between the two blood samples was still observed. This finding led us to suspect that the discrepancy was not attributed to different detection methods, but to inherent issues within the two blood samples.
Verification of repeat hemoglobin measurements.

After consulting with the clinical team, we determined that the blood samples collected from the hospital on day 6 onward were obtained via an indwelling arterial catheter. Notably, the catheter lumen was locked with heparinized saline, and before each collection, approximately 4–5 mL of mixed blood (equivalent to 3 times the catheter dead space volume) was discarded. 3 We postulated that incomplete evacuation of heparin-diluted blood from the catheter lumen caused sample dilution, adversely affecting test results, particularly reducing HB concentration in the first-drawn sample. 4 This hypothesis was corroborated by nursing records. On days 6 and 7, the first blood sample was collected for CBC, while on day 8, the initial sample was drawn for blood gas analysis. To address this, nurses subsequently increased the discard volume to 6 mL and standardized the collection sequence. This intervention restored concordance in HB measurements across analytical platforms (Table 2). The reporting of this study conforms to the Case Report (CARE) guidelines. 5
Discussion
For emergency patients, the arterial indwelling catheter blood collection method is convenient and fast, which can not only alleviate pain but also reduce the waste of medical resources. Blood HB concentration is one of the most frequently measured parameter in clinical medicine, particularly for patients with active hemorrhage. 1 The cyanmethemoglobin (HiCN) detection method is the reference method recommended by the International Council for Standardization in Hematology. 6 However, this method presents potential toxic hazards due to disposal concerns regarding large volumes of cyanide-containing reagents. In contrast, the sodium lauryl sulfate (SLS) method utilizes nontoxic substances while demonstrating comparable reliability and reproducibility to the HiCN method for HB measurement, making it suitable for automated measurement systems. 7 The XN-550 AHA system employs the SLS-HB method for testing HB concentrations. With the exception of sulfhemoglobin, various HB species in the blood form complexes with low concentrations of SLS, and these complexes exhibit characteristic absorption spectra. HB concentration is then rapidly and accurately determined using colorimetry. Conversely, the HB concentration measured using the GEM Premier5000 BGA system was calculated using the formula HB (g/dL) = HCT (%) × 0.34, where hematocrit (HCT) level was determined by measuring the conductivity of red blood cells.
Although the detection principles of the two analyzers are different, previous studies have evaluated the agreement of HB measurements via BGA and AHA in adult patients. Most studies have indicated that BGA-derived HB and HCT values are correlated with those obtained from AHA. Based on routine clinical observations, HB results obtained from simultaneously drawn blood samples for CBC and blood gas analysis demonstrate broad alignment when analyzed using their respective analyzers.8–11 In our case, internal validation (Table 3) confirmed that both analyzers achieved excellent correlation when identical blood samples were tested. Variations in the order of drawing blood sample accounted for the observed directional discordance in the results. On days 6 and 7, the first tube drawn for CBC contained more residual heparinized saline that equally affected both platforms. On day 8, the first tube was drawn for blood gas analysis, and heparinized saline dilution disproportionately increased the conductivity of red blood cells, resulting in an underestimation of HCT and the calculated HB. Although both platforms passed the routine quality control, our case revealed that dilution tolerance is not routinely verified during analyzer validation. Pre-analytical errors (e.g. inadequate discard volume) can amplify platform-specific vulnerabilities, particularly for calculated parameters.
Importantly, the HB discrepancy between the two analyzers during days 6–8 reflects two concurrent factors: (a) a true physiological decline in HB concentration (to ∼80–90 g/L) driven by postoperative stress from dual major surgeries and acute UGIB and (b) pre-analytical errors in arterial catheter sampling. In particular, pre-analytical errors such as suboptimal discard volume and deviations in collection sequence artificially amplified the analytical discrepancy (up to 13 g/L). Although the patient’s critical condition justified the lower HB concentrations, the magnitude of inter-analyzer discrepancy was clinically relevant. Discrepancies of this magnitude could potentially misguide transfusion decisions or bleeding assessments. Crucially, standardization of the sampling protocol resolved the inconsistency, confirming that the observed variance was an artifact rather than a true clinical change.
Although HB served as our primary indicator due to its clinical significance in bleeding or transfusion decisions, improper discard volume likely impacted multiple parameters. Calculated parameters, such as HCT detected by BGA, may exhibit amplification errors due to conductivity artifacts. 12 In addition, several studies have shown that blood samples mixed with heparinized saline affect electrolyte results, as they increase the total sample volume and dilute the specimen. Additionally, heparin itself binds to positively charged ions, which may cause pre-analytical biases in electrolyte concentrations.13–15 The dilution of blood samples results in linear decreases in electrolyte concentrations as well as partial pressure of carbon dioxide (pCO2), glucose, and HB concentrations. Conversely, pH, partial pressure of oxygen (pO2), and bicarbonate concentration remained relatively stable owing to blood buffering capacity. As partial pressure of oxygen in arterial blood (PaO2) represents only 2% of physically dissolved oxygen in the plasma, oximetry parameters expressed as percentages remain unchanged. 16 In our case, we observed minimal impact of the dilution effect on other parameters. In fact, inadequate discard volume during arterial catheter blood sampling may compromise multiple aspects of patient monitoring in addition to HB measurements.
Conclusion
This case underscores a critical pre-analytical factor in arterial catheter sampling, i.e. the impact of inadequate discard volume on HB concentration measurements. Our findings demonstrate that pre-analytical vigilance is crucial when HB concentration trends guide life-saving interventions, particularly in actively hemorrhaging, monitoring-dependent patients admitted to the intensive care unit. Furthermore, interpatient variability necessitates tailored clinical assessment strategies. Addressing these procedural gaps will enhance diagnostic accuracy and improve outcomes in hemodynamically vulnerable populations.
Footnotes
Acknowledgements
The authors sincerely thank the editors and reviewers for their feedback and comments.
Author contributions
Jinle Wang, Huihui Jiang: Writing–original draft, visualization, and investigation
Qingqing Bi, Kegang Tian: Investigation and conception
Lei Zhang, Xiaofeng Mu: Writing–review & editing, resources, and supervision
Consent for publication
Not applicable.
Data availability statement
The datasets provided within the current study are available from the corresponding author on reasonable request.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was financially supported by grants from the Industry-Academia Collaborative Education Program of the Ministry of Education, China (2411142809).
