Abstract
Behçet’s disease (BD) is a rare systemic vasculitis that is characterized by recurrent oral and genital ulcers, uveitis, and skin lesions. Although neurological involvement is a known complication, ischemic stroke remains uncommon. Herein, we report a 37-year-old Kuwaiti woman who experienced recurrent ischemic stroke with no traditional risk factors. Imaging studies, including magnetic resonance imaging and angiography, confirmed the diagnosis of recurrent ischemic stroke and identified the underlying vasculitic changes. A detailed examination revealed a history of recurrent orogenital ulcers, leading to a diagnosis of BD. High-dose corticosteroids, azathioprine, and antiplatelet treatment were effectively used to manage her acute strokes and underlying vasculitis, thus preventing further thrombotic events. Our case report underscores the difficulties of diagnosing BD with ischemic stroke as the initial manifestation and emphasizes the importance of a multidisciplinary approach that involves rheumatologists, neurologists, and radiologists to create an effective treatment plan. Our findings also underscore the need for medical practitioners to be more knowledgeable about ischemic stroke in young patients without risk factors from endemic areas of BD, and to develop effective therapy plans. Our review of the English literature indicates that this is only the fifth report of stroke as the first presentation of BD.
Keywords
Introduction
Behçet’s disease (BD) is a variable vessel vasculitis of unknown etiology. It can affect veins and arteries in small, medium, and large vessels. Patients with BD present with recurrent oral and genital ulcers accompanied by skin and ocular manifestations. 1 Globally, the prevalence of BD is between 0.1 in 1000 and 1 in 10,000, with Asia having the highest prevalence. 2 The greatest incidence, ranging from 80 to 420 in 100,000, has been found in Turkey. 2 The disease onset often occurs during the third decade of life. 3
Approximately 5% to 10% of all BD cases exhibit neurological manifestations; such cases are known as neuro-BD.4–7 Neuro-BD is subdivided into parenchymal and nonparenchymal diseases. Nonparenchymal types include central venous thrombosis, intracranial hypertension syndrome, acute meningeal syndrome, and stroke.3–7 A higher risk of stroke has been observed in BD than in the general population with the same risk factors. 8 It was hypothesized that this finding may be related to the systemic inflammation, vascular damage, and hypercoagulability observed in BD, in addition to the stenosis, occlusion, dissection, and aneurysm of medium- to large-sized cerebral arteries.9,10 Nevertheless, limited publications have assessed stroke as the initial manifestation of BD. Herein, we describe a case in which recurrent symptomatic ischemic stroke was the first presentation of BD.
Case description
A 37-year-old Kuwaiti woman, who was married and had two offspring, first experienced a lacunar ischemic stroke in January 2021. However, no neurological deficit was present, and she was discharged against medical advice on oral aspirin (81 mg daily) and oral clopidogrel (75 mg daily). She arrived at Al Sabah Hospital in Kuwait in March 2021 after experiencing an occipital headache and left arm paresthesia for 3 days. She reported a history of recurrent orogenital ulcers for the last 5 years as well as intermittent left knee pain and swelling for 2 years.
She was taking oral contraceptives as a form of birth control. The patient did not smoke and had no other risk factors for cerebrovascular diseases. She had no eye symptoms, family history of autoimmune diseases, or parental consanguinity.
Upon physical examination, she was found to be afebrile, had an equal and normal pulse and blood pressure in both limbs, and had other normal vital signs; however, she appeared sick. Neurological examinations demonstrated left-sided hypoesthesia with intact motor power. Musculoskeletal examination revealed bilateral ankle tenderness and swelling, with a normal active and passive range of motion. Furthermore, she had active oral ulcerations. A pathergy test was negative, and no abnormalities were detected on chest or abdominal examinations.
Brain magnetic resonance angiography revealed a small area of restricted diffusion at the anterior aspect of the right thalamus, suggesting a recent lacunar vascular insult. An abnormal T2 fluid-attenuated inversion recovery signal that was patchy and high was noted in the right thalamus, extending to the related cerebral peduncle, bilateral basal ganglia, and anterior aspect of the left putamen. This finding was compatible with vasculitis. There was no significant enhancement in post-contrast T1-weighted imaging and no restriction in diffusion-weighted imaging. A small, high T2 fluid-attenuated inversion recovery signal focus was noted in the right periventricular region and another was observed in the right subcortical frontal region; however, there was no restriction in diffusion-weighted imaging, suggesting an old lacunar insult. Magnetic resonance angiography showed no stenotic lesions of the cerebral arteries (Figure 1). Carotid Doppler ultrasound was unremarkable. The 24-hour dynamic electrocardiogram, contrasted transthoracic echocardiography, and transesophageal echocardiography were all normal.
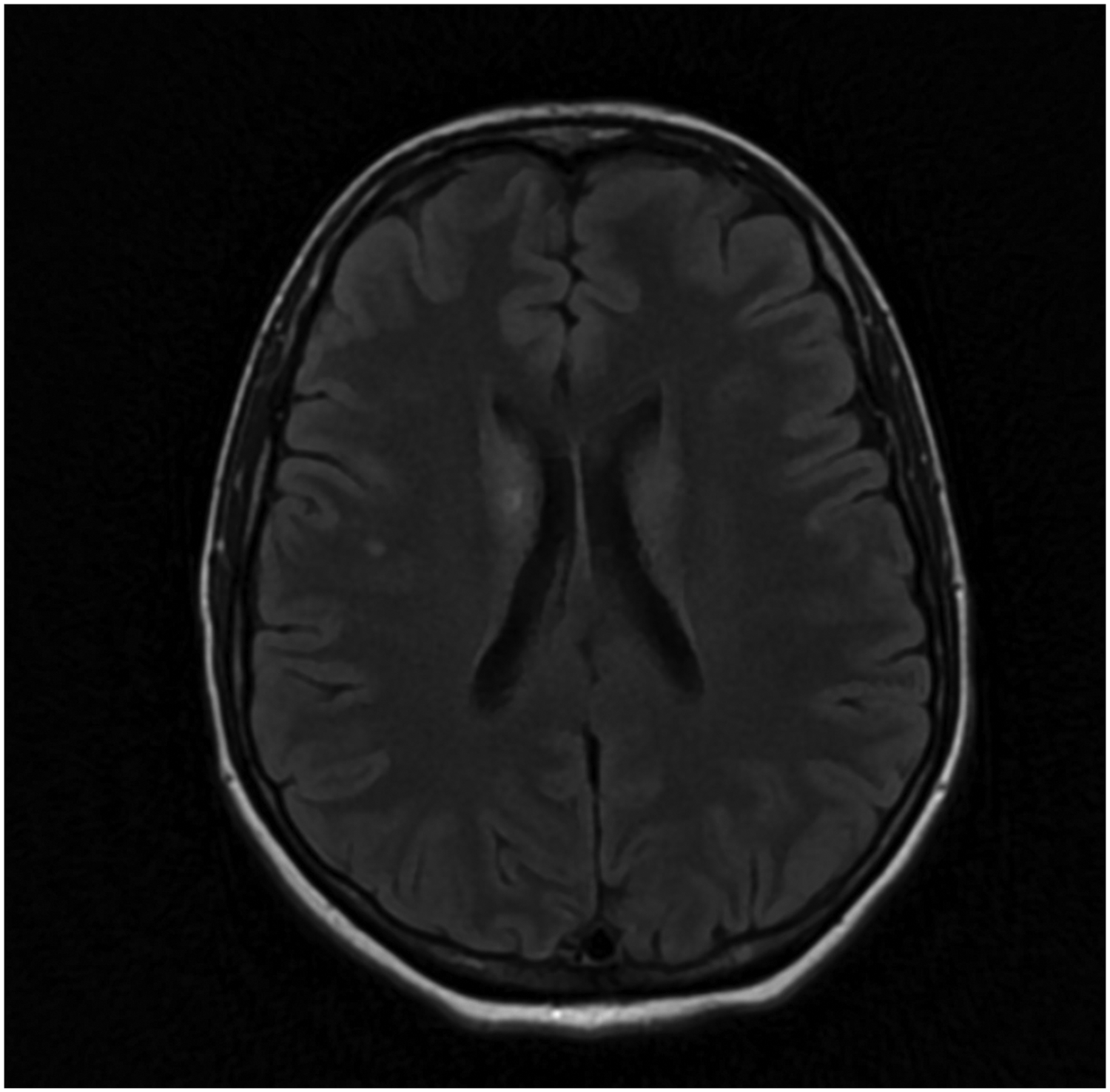
Brain magnetic resonance angiography. The anterior aspect of the brain displays a small area of restricted diffusion. The right thalamus indicates a recent insult to the lacunar vascular system. Abnormal patchy high T2 fluid-attenuated inversion recovery signal is noted in the right thalamus, extending to involve the related cerebral peduncle, bilateral basal ganglia, and anterior aspect of the left putamen, compatible with vasculitis. There were no stenotic lesions in the cerebral arteries or aneurysm formation.
Laboratory tests revealed mild normocytic normochromic anemia, an increased erythrocyte sedimentation rate (81 mm/hour) and C-reactive protein level (40.8 mg/dL), and HLA-B51 genetic marker positivity. By contrast, the serologic etiology tests (including syphilis and human immunodeficiency virus), lipid profile, plasma glucose, plasma and urine homocysteine levels, activated protein C resistance, deficiency of proteins C and S, antithrombin III deficiency, antiphospholipid antibodies, antinuclear antibody, antineutrophilic cytoplasmic antibodies, and factor V Leiden were all within normal limits.
A diagnosis of BD with presumed cerebral vasculitis and a subsequent ischemic stroke was made under the guidance of the International Criteria for BD 11 (Table 1). Following counseling and acceptance, the patient was initially treated with intravenous pulse methylprednisolone (500 mg daily for 3 days) followed by oral prednisolone (40 mg daily). She was then started on oral colchicine (0.5 mg daily), oral azathioprine (100 mg daily), oral aspirin (81 mg daily), and oral clopidogrel (75 mg daily).
International Criteria for Behçet’s Disease – point score system: scores >4 indicate a diagnosis of Behçet’s disease.

Pathergy testing is optional, and the primary scoring system does not include pathergy testing; however, if pathergy testing is conducted, one extra point may be assigned for a positive result.
The patient’s symptoms gradually alleviated and her inflammatory markers and anemia returned to normal. With a tapered prednisolone dosage, the patient was discharged from the hospital. Because oral contraceptives have diverse effects on BD course in different patients, 3 she was advised to stop oral contraceptives and consider an intrauterine device. The patient’s nervous system manifestations and oral ulcer symptoms did not return after 3 years of maintenance therapy with oral colchicine and oral aspirin. This study’s reporting complies with CARE criteria (for CAse REports). 12
Discussion
The relationship between BD and ischemic stroke has garnered increasing attention in the past several years, particularly because of the unique pathophysiological mechanisms involved in this uncommon but devastating manifestation of the disease. BD is characterized by systemic vasculitis, which predominantly affects venous structures; however, it can also involve arterial systems, leading to various neurological complications, including ischemic strokes. 8
The mechanisms underlying ischemic strokes in BD are multifaceted. One important factor is the chronic inflammation associated with the disease, which can lead to vasculitis affecting the cerebral vessels. This inflammation can result in endothelial dysfunction, increased vascular permeability, and ultimately thrombosis, which may precipitate ischemic events.13,14 For example, one study directly linked cerebral vasculitis to ischemic strokes in BD patients, highlighting the role of vascular inflammation in the pathogenesis of these strokes. 14 Furthermore, antiphospholipid antibodies in some patients with BD have been linked to an increased risk of thrombotic events, including strokes. 15
The incidence of stroke in patients with BD is approximately 4.2%; 16 this is relatively low compared with Takayasu’s arteritis, in which strokes occur in 10% of all patients. 17 Old age and hypertension are considered independent risk factors for ischemic strokes in BD 1 and 16% of ischemic strokes in the younger population have BD as the cause. 2
Clinical presentations of ischemic stroke in BD can vary substantially. Some studies have documented cases of stroke in younger populations, which are often linked to specific triggers such as pregnancy or other inflammatory conditions. 15 For example, pregnancy-related strokes have been observed in patients with cortical vein thrombosis, underscoring the importance of considering specific risk factors in this population. 15 Additionally, the locations of ischemic lesions may provide clues about the underlying pathophysiology. For example, BD cases often have lesions in the brainstem, which may reflect the specific vascular areas that are affected by this disease. 18 Moreover, the clinical management of ischemic stroke in patients with BD poses unique challenges; the standard treatment protocols for ischemic stroke may not be entirely applicable because of underlying vasculitis and the potential for recurrent thrombotic events. A tailored approach that considers the inflammatory nature of BD is therefore essential. 14 Although some case reports have suggested the effectiveness of anticoagulants and immunosuppressive therapies, research into the most effective management strategies remains ongoing.
In the present report, we have described an unusual case of a woman with recurrent ischemic stroke as the first presentation of BD. Our patient met the International Criteria for BD diagnostic requirements, with recurrent oral aphthosis (2 points), genital aphthosis (2 points), neurological manifestations (1 point), and vascular manifestations (1 point). She also had the genetic marker HLA-B51, which is associated with BD.
Literature review
An extensive literature search of PubMed was performed using the keywords “Behçet’s,” “ischemic,” and “stroke” from January 2004 to January 2024. Thirty-one articles were retrieved and independently reviewed by two authors (Anwar Albasri and Wesam Gouda). Five articles in languages other than English and 18 articles with low relevance were excluded. We included English-language articles that specifically targeted adults. Following the screening process, we ultimately included eight reports in our review. The clinical data of the included patients are illustrated in Table 2.14,16,19–23 The two authors performed a comprehensive manual data extraction for each included study, focusing on key aspects such as the neurological presentation, HLA-B51 status, diagnostic methods, treatment strategies, and management outcomes. All eight cases showed signs of ischemic stroke. Only two of the eight cases were women. The age range was 22 to 59 years. Four of the eight cases had BD prior to developing ischemic stroke, whereas four cases were similar to our reported case with stroke as the first presentation of BD. The recurrence of ischemic stroke was documented in only three cases. Similar to our patient, the majority of cases had no documented risk factors for ischemic stroke. HLA-B51 status was positive in two cases (as in our case), negative in two cases, and not reported in the remaining four cases. Almost all of the patients received glucocorticoids at the time of diagnosis, followed by immunosuppressive therapy. However, the choice of immunosuppressive therapy varied from case to case. Almost all cases had a good or stable outcome.
Summary of the cases reviewed in terms of demographic data, clinical presentation, and treatment mode.

BD, Behçet’s disease; CPAP, continuous positive airway pressure; CRP, C-reactive protein; CT, computed tomography; CVST, cerebral venous sinus thrombosis; DWI, diffusion-weighted imaging; ECG, electrocardiogram; ECHO, echocardiogram; ESR, erythrocyte sedimentation rate; F, female; FLAIR, fluid-attenuated inversion recovery; HLA, human leukocyte antigen; ICA, internal carotid artery; ICH, intracerebral hemorrhage; IV, intravenous; M, male; MR, magnetic resonance; MRA, magnetic resonance angiography; MRI, magnetic resonance imaging; NBD, neuro-Behçet’s disease; PAH, pulmonary arterial hypertension; T2WI, T2-weighted image; TR, tricuspid regurgitation.
Our report contributes to the growing body of literature on the atypical presentations of BD and sheds light on the intricate interplay between vasculitis and ischemic stroke in this unique clinical context. Further research is warranted to explore the underlying pathophysiological mechanisms linking BD to cerebrovascular events, thus facilitating the development of targeted therapeutic approaches for this rare but severe complication.
Conclusions
The present case highlights the challenges of diagnosing patients with ischemic stroke as a first presentation of BD and emphasizes the importance of a multidisciplinary strategy involving rheumatologists, neurologists, and radiology specialists. It also underscores the need for medical practitioners to be more knowledgeable about ischemic stroke in young patients from endemic areas of BD because this might be an early BD symptom. BD should be considered in individuals who have no risk factors for ischemic stroke so that effective therapy plans can be rapidly developed.
Footnotes
Author contributions
WG conceived the article. AA wrote the draft. AA and WG reviewed the literature and handled the screening process and data extraction. FA provided supervision or mentorship. WG, MMM, AAM, and NEG contributed to the clinical management of the patient, manuscript editing, and data collection. All authors have read and approved the final manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics statement
The patient gave written consent for the publication of her de-identified data, and the case report did not need approval from the ethics committee because our institutions do not require ethical approval for the publication of case reports.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
