Abstract
Abdominal pregnancies are a rare form of ectopic pregnancy with omentum pregnancies being even rarer. Ectopic pregnancy should be diagnosed and terminated early to prevent the risk of harm to the mother. This case report describes a rare case of omentum pregnancy with severe hemoperitoneum. The patient had not visited a doctor until she failed to menstruate for 3 months, by which point she had developed severe hypogastralgia. The patient was diagnosed with a ruptured ectopic pregnancy after ultrasonography. The omentum pregnancy was complicated by severe hemoperitoneum, which was confirmed by emergency laparotomy. The patient was treated successfully with fetal extraction and partial omentectomy. Ultrasound examination in early pregnancy is essential to detect and treat ectopic pregnancies as early as possible, as surgery is usually required for abdominal pregnancies. Prompt treatment of ectopic pregnancies is critical, as an omentum pregnancy is dangerous and may result in severe intraperitoneal bleeding.
Introduction
Abdominal pregnancy is a rare type of ectopic pregnancy in which the embryo is implanted in the abdominal cavity instead of the uterus endometrium. Abdominal pregnancy is rare and embryo implantation in the omentum is even rarer. A few cases of omentum pregnancy have been reported in the literature.1–25 It is known that abdominal pregnancy often results in severe hemoperitoneum.2,3,7,10,13,15,18 This current case report describes a female patient with a second-trimester pregnancy in which the embryo was implanted in the omentum and the patient presented with severe hemoperitoneum.
Case report
A female in her mid-30s presented to the Department of Gynaecology and Obstetrics, The Central Hospital of Bengbu, Bengbu City, Anhui Province, China with sudden onset of hypogastralgia, nausea and vomiting lasting for 3 h. The patient’s menstrual cycle was irregular, ranging from 23 to 37 days. On 10 February 2021 (56 days previously), the patient had experienced a small amount of vaginal bleeding and abdominal discomfort, but these symptoms had resolved 3 days later. The patient did not pay attention to these symptoms; she thought it was a menstruation. We believed that the vaginal bleeding at this point indicated an ectopic pregnancy and the patient's actual last menstrual period was in January 2021. In fact, she had been menstruating for 3 months, but she did not visit the clinic. As such, she missed the early pregnancy ultrasound examination window. Three hours prior to presenting, the patient had experienced a sudden onset of hypogastralgia, which continued without relief, resulting in her vomiting once. The patient was healthy with no relevant medical history. She was unmarried, had no history of delivery, but had an abortion several years previously. She usually used condoms for contraception.
The patient’s vital signs at the time of admission were as follows: temperature, 36.0 °C; heart rate, 102 beats/min; blood pressure, 96/60 mmHg; and respiration, 20 breaths/min. Her body mass index was 27 kg/m2 (68 kg/1.58 m2). Although the patient was awake and mobile, we believe that the patient was in the compensatory phase of haemorrhagic shock caused by intraperitoneal bleeding. The patient’s abdomen was soft. Tenderness with no rebound pain was observed in the patient’s lower abdomen. We did not touch the mass on the patient’s lower abdomen. The patient’s vulva, vagina, cervix and uterus showed no abnormalities during the gynaecological examination. We observed an irregularly shaped mass on the left side of the uterus, but not on the right side. The patient complained of lower abdomen pain during the pelvic bimanual examination. On routine blood tests at admission, the patient’s haemoglobin level was 96 g/l and the white blood cell count was 22.65 × 109/l. Coagulation function, liver function and kidney function showed no significant abnormalities.
The patient underwent an urgent ultrasound examination, which indicated a rupture of an ectopic pregnancy and an intraperitoneal haematocele. The uterine echo was normal and there was no pregnancy sac in the uterine cavity (Figure 1). However, fetal echoes were observed on the left side of the uterus. The fetus had a biparietal diameter of 23 mm, crown-rump length of 53 mm and a fetal heart rate of 164 beats/min. Some dark fluid areas with small light spots were observed in the patient’s abdominal cavity. While performing the ultrasound examination, an abdominal puncture using ultrasound guidance was undertaken, which withdrew 5 ml of blood from the patient’s lower abdominal cavity. As a result, the patient was diagnosed with an ectopic pregnancy with abdominal bleeding. An emergency exploratory laparotomy was subsequently performed.
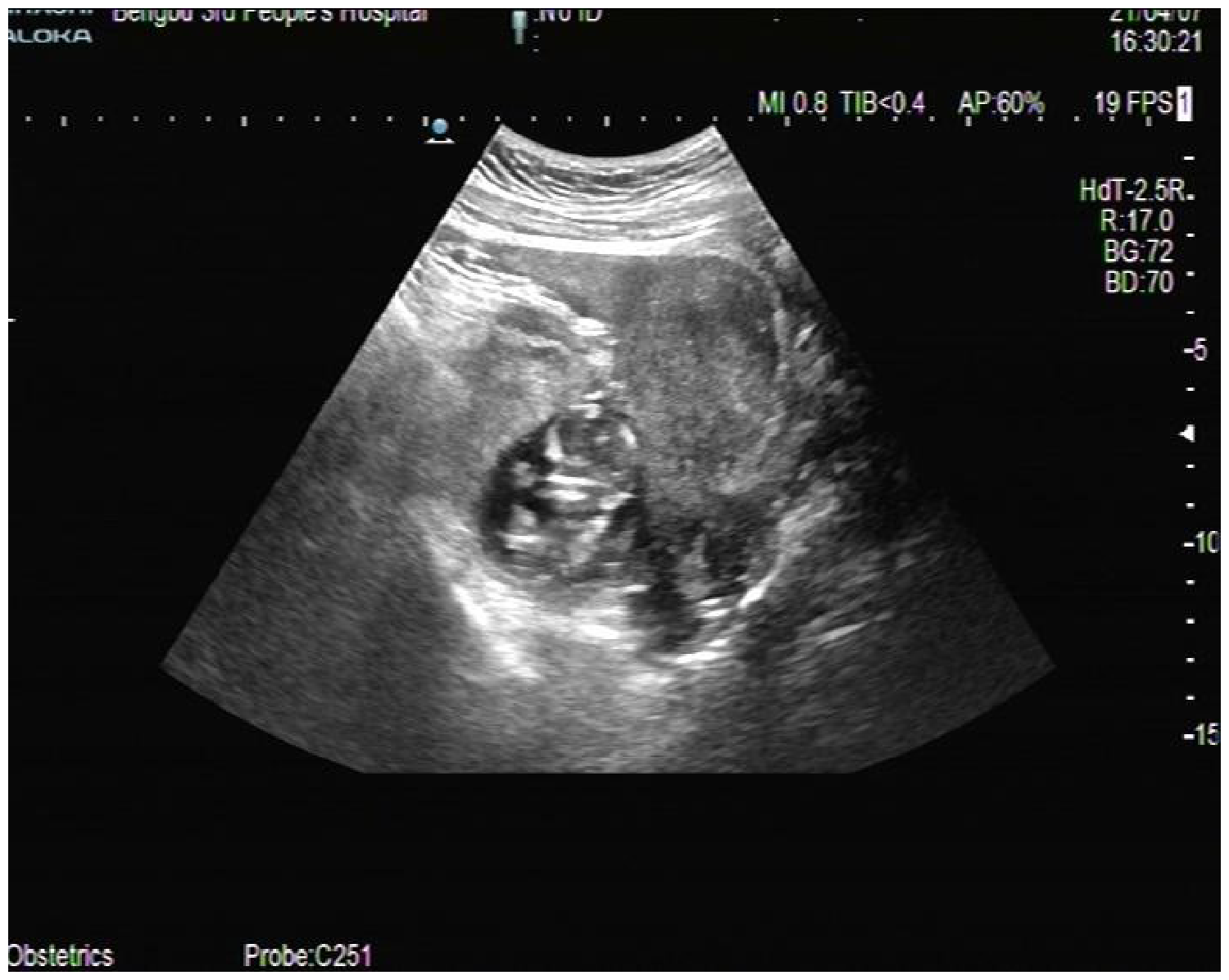
Ultrasound image of the ectopic fetus in a female in her mid-30s who presented with sudden onset of hypogastralgia, nausea and vomiting lasting for 3 h. The uterus showed no obvious abnormalities. A gestational sac was observed in the left pelvic cavity adjacent to the uterus.
While treating the shock with infusion and blood transfusions, an emergency exploratory laparotomy was performed. The total blood accumulation and clots in the abdominal cavity was approximately 2000 ml. After clearing the blood buildup, the pregnancy-sac mass, located on the left side of the pelvic cavity and approximately 10 cm in diameter, was lifted out of the pelvic cavity. Part of the gestational sac was enclosed by the omentum, wrapped and formed a pregnancy-sac mass, which was adhered to the left fallopian tube (Figure 2). After separating the left fallopian tube, the placenta was observed to be fully implanted in the omentum and was actively bleeding. The part of the omentum where the placental implantation had taken place was excised to remove the fetus and placenta. The ectopic fetus was approximately the size of a 12-week pregnancy. In addition, the left fallopian tube was severely enlarged, hyperaemic and oedematous (Figure 3). We believe that the omentum pregnancy occurred secondary to the left tubal abortion. As such, the diseased left fallopian tube was excised. The patient was finally diagnosed with secondary abdominal pregnancy, omentum pregnancy, abdominal haemorrhage and compensatory phase of haemorrhagic shock.

An emergency exploratory laparotomy identified an omentum pregnancy in a female in her mid-30s who presented with sudden onset of hypogastralgia, nausea and vomiting lasting for 3 h. The pregnancy sac had been broken. The placenta had implanted in the omentum, adhering to the left fallopian tube, with active bleeding. The colour version of this figure is available at: http://imr.sagepub.com.

An emergency exploratory laparotomy identified an omentum pregnancy in a female in her mid-30s who presented with sudden onset of hypogastralgia, nausea and vomiting lasting for 3 h. The image shows the oedematous left fallopian tube, which was auxetic and hyperaemic. It was hypothesized that the omentum pregnancy may have developed as a secondary abdominal pregnancy from an aborted tubal pregnancy in the left fallopian tube. The colour version of this figure is available at: http://imr.sagepub.com.
The patient recovered successfully after treatment. On day 3 after surgery, the serum beta human chorionic gonadotropin (beta-hCG) concentration declined from 15000 IU/l to 3789.2 IU/l. The patient was discharged on day 7 after surgery. After 1 month, the patient’s serum beta-hCG concentration had decreased to normal levels. This case report was approved by the ethics review board of The Central Hospital of Bengbu, Bengbu City, Anhui Province, China (no. 2021IT0007).
The patient provided informed consent to undergo examination and treatment. Informed written consent was obtained from the patient for publication of this report and any accompanying images. The reporting of this case report conforms to CARE guidelines. 26
Discussion
Ectopic pregnancies can be classified as fallopian tube pregnancy, ovarian pregnancy, cervical pregnancy or abdominal pregnancy, depending on the exact location of implantation. Omentum pregnancy is a rare type of abdominal pregnancy, which is itself a rare presentation. Pregnancy of the omentum is a rare subset of abdominal pregnancy that can only be diagnosed during surgery,1–25 as the location of the ectopic embryo can only be determined at this time. Ectopic pregnancies can be dangerous and may cause a large amount of abdominal bleeding.2,3,7,10,13,15,18 As such, ectopic pregnancies represent a serious threat to life and safety and should be diagnosed as early as possible and dealt with expediently. Women of childbearing age should seek medical attention immediately after experiencing paramenia because this might be caused by an ectopic pregnancy.
Early pregnancy ultrasound testing is crucial.1–9,11–16,18,20,23 Women should undergo standardized prenatal checkups when their menstrual period fails to come on time. Ultrasonography should be performed to detect ectopic pregnancies as early as possible. In the present case, the patient did not seek medical attention and did not undergo early pregnancy ultrasonography until abdominal pain was presented. Many undiagnosed abdominal pregnancies occur due to a lack of ultrasound in early pregnancy.10,17,19,25 Accurate diagnosis of abdominal and omentum pregnancies is difficult, and the exact location of an ectopic embryo can usually only be determined at the time of surgery.
The clinical manifestations of omentum pregnancies are similar to those of other types of ectopic pregnancies. In its early stages, omentum pregnancy may be asymptomatic or non-physically signed and is detected only by auxiliary examination. As the disease progresses, ectopic pregnancies often result in abdominal pain and vaginal bleeding and present with symptoms of abdominal bleeding and haemorrhagic shock.2,10,14,18,21 During the gynaecological examination of patients with abdominal pregnancy, the examiner may detect lumps, tenderness and haphalgesia. In the present case, the patient developed nausea and vomiting. Moreover, other researchers have reported upper digestive tract symptoms in patients with omentum pregnancies,6,18 which may be related to omentum attachment to the stomach.
Abdominal pregnancies generally require surgical treatment and early omentum pregnancy can be treated laparoscopically.1,2,5,7,9,11–13,16 Often, ectopic embryo implantation sites can only be identified at the time of surgery. Because of the high risk of bleeding and accidental damage to adjacent organs, performing abdominal pregnancy surgery to resect the gestational sac is challenging.5,17 In ectopic pregnancy surgery, if an ectopic pregnancy sac cannot be found, a thorough examination of the abdominal cavity is warranted.1,2,4,7,8,11–14
In a previous case report, conservative treatment of an omentum pregnancy by injecting potassium chloride into the fetal heart was successful. 27 In other case reports, in which the diagnosis and treatment of the omentum pregnancies were delayed, the ectopic fetus survived to the third trimester of pregnancy and the mother gave birth to a live newborn via laparotomy.17,19 However, there have been only a few cases that have resulted in a live infant. Abdominal pregnancies in the second or third trimester are extremely dangerous with poor pregnancy outcomes and prompt exploratory laparotomy is required. In particular, dealing with an ectopic placenta can be particularly challenging. The placenta may become implanted during middle to late pregnancy. Depending on the surgical context, the placenta and attached organs (part of the omentum, intestinal canal, broad ligaments, ipsilateral adnexa and uterus) should be excised. If the fetus has been dead for a long time, only the placenta should be removed. If the fetus is alive or has only recently died, it may not be possible to remove the placenta safely. In such cases, the umbilical cord next to the placenta can be ligated, chemotherapy can be administered or an alternative time for surgery can be selected. Fortunately, in the present patient, the placenta was only implanted in the omentum, and the placenta and part of the omentum were excised together, resulting in favourable outcomes.
Abdominal pregnancies are classified as primary or secondary according to Studdiford’s criteria. 28 We believe that the present case of omentum pregnancy occurred secondary to an abdominal pregnancy resulting from a left tubal pregnancy abortion. The patient’s left fallopian tube was thickened and inflamed. Because the diseased left fallopian tube was prone to ectopic pregnancy, it was resected. From our perspective, the vast majority of abdominal pregnancies are secondary to tubal pregnancy abortions.22,25
Footnotes
Acknowledgements
We want to express our gratitude to Ling Tian for her cooperation during the laparotomy and to Jie Gao for her assistance in writing the manuscript.
Author contributions
S.Y. reviewed the patient’s medical records and drafted the article; and Y.W. approved the final version of the article to be published.
Data availability statement
The authors confirm that the data supporting the findings of this study are available within the article.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
