Abstract
Treatment of lower limb ischemia in patients with diabetes is challenging because of the location of the ulcers and the complexity of their pathogenesis. Carbon dioxide fractional laser (CO2FL) therapy in conjunction with tibial periosteum distraction could become a substitute for conventional methods. We herein describe a patient diagnosed with ischemic diabetic foot with a complex ulcer in the upper third of the tibia. Laser irradiation (Deep FX mode with 30 mJ of energy and 10% density) was applied to the entire region of skin below the knee after surface anesthesia, and this treatment was performed twice a week until the ulcer healed. Computed tomography angiography showed successful establishment of a blood supply to the back of the right foot after treatment. Skin grafting was successfully performed, with only a few wounds remaining on the foot 8 months after treatment. The pain score was significantly decreased at the last follow-up. No complications occurred. This case report provides guidance for the performance of CO2FL, a fast, easy, accurate treatment in patients with diabetes. CO2FL can target lower limb arterial occlusive disease accompanied by refractory ulcers, addressing the underlying vascular occlusion and dysfunction as well as promoting microcirculation and wound healing.
Keywords
Introduction
Diabetic foot ulcer, a common complication of diabetes, is characterized by a high incidence and high disability and mortality rates. Such ulcers greatly affect the physical and mental health of patients as well as their overall quality of life.1,2 The lifetime risk of foot ulcers ranges from approximately 19% to 34%, and this risk has been increasing with the longer life expectancy and clinical complexity of people with diabetes. Persistent hyperglycemia leads to occlusion of major blood vessels and impaired microcirculation in the lower extremities, giving rise to ischemic diabetic foot. 3 This condition is predominantly characterized by foot pain, intermittent claudication, muscle atrophy, skin ulceration, and even gangrene.
Treatment for ischemic diabetic foot mainly involves revascularization techniques, microcirculation enhancement, and wound management. 4 Improved microcirculation and direct revascularization should be priorities in the management of lower limb ischemia in patients with diabetes. 5 Revascularization is a basic therapy that includes arterial bypass surgery and endovascular interventional techniques (e.g., balloon dilation, stent implantation) to maintain a sufficient blood supply to the limbs and promote adequate microcirculation.6,7 However, vascular intervention alone cannot fully heal wounds caused by lower limb ischemia in patients with diabetes. Transverse tibial bone transport and periosteal distraction have become popular methods of improving ischemic diabetic foot ulcer,8,9 but the need for multiple surgeries poses a challenge in gaining patient acceptance. Carbon dioxide fractional laser (CO2FL) therapy is a recently developed treatment that is now widely used for scars. The primary mechanism of CO2FL therapy is based on the theory of fractional photothermal interaction. 10 During application of the CO2FL to scar tissue, collagen fibers are directly absorbed by water. This leads to the generation of heat and vaporization of the scar tissue, 11 ultimately promoting tissue remodeling. The application of CO2FL therapy can promote tissue regeneration and stimulate angiogenesis, giving it the potential to greatly improve microcirculation in the lower limbs and facilitate regeneration of the microcirculatory system in patients with diabetic foot.
Case presentation
Patient information
A woman in her early 80s was admitted to the hospital 3 months previously with refractory skin ulceration and pain in the lower pretibial region. In July 2022, the patient developed erythema of unknown cause in the right anterior tibial region (Figure 1(a)). The patient repeatedly scratched the rash, resulting in rupture. When the patient arrived at our hospital, she reported having undergone dressing changes, balloon dilation, debridement, and skin grafting procedures at another hospital. Unexpectedly, however, the ulcer persisted and continued to grow despite balloon dilation, which had been performed to facilitate vascular patency.

(a) The patient developed erythema of unknown cause prior to admission, and subsequent scratching led to skin damage. (b) Exposed state of the pretibial tissue and tendons after admission. (c, d) Digital subtraction angiography images of pretibial arteries and peroneal arteries after admission and (e) Ultrasound images of pretibial arteries after admission. (Yellow arrow in computed tomography angiography image indicates reperfusion of the distal tibial artery and blood supply to the right foot after 2-mm micro-balloon dilation).
After interviewing the patient, we found that noncompliance with anticoagulant medication and poor glycemic control had led to recurrent vascular occlusion after hospital discharge.
Examination and diagnosis
The patient presented with an approximately 15- × 5-cm wound on the anterior side of the lower segment of the right tibia (Figure 1(b)). Tendon and muscle tissues were exposed on the wound surface, and yellowish-white necrotic tissue was observed surrounding the wound. The back of the right foot showed redness and swelling. The dorsal foot artery was not palpable, and hypothermia was observed at the distal ends of the lower limbs. Digital subtraction angiography of both lower limbs revealed arteriosclerosis with multiple severe lumen stenoses, including the anterior tibial, peroneal, and distal posterior tibial arteries (Figure 1(c), (d)). In addition, the bilateral femoral arteries were nearly locally occluded. Ultrasound results of the right lower limb showed build-up of plaques in the pretibial arteries (Figure 1(f)). In cases such as this, careful examination can help to evaluate the entire arterial circulation of the lower extremity, diagnose the condition, predict the prognosis, and develop treatment strategies. Based on the patient’s symptoms and ancillary examination findings, the preliminary diagnoses in this case were type 2 diabetic foot ulcers and arterial occlusion of the lower extremities.
Therapeutic intervention
After pharmacological interventions to control the patient’s glycemic level and endovascular balloon angioplasty for the vascular stenosis, we explored strategies aimed at promoting microcirculation after vessel reperfusion. Given the elevated location of the wound and the risk of infection, periosteal stretching and bone transport were ruled out. We adopted CO2FL therapy as an innovative approach to facilitate wound healing, prompted by the therapeutic principles of periosteal distraction. The wound base was treated at 30 mJ and 10% density. 12
Follow-up and outcomes
We first performed debridement to prevent the wound from further expanding (Figure 3(a)). We then administered CO2FL treatment for 1 week and found that the skin graft had survived (Figure 3(b)). As expected, after almost 3 months of CO2FL treatment, we observed a notable improvement in the blood supply to the patient’s right foot. The digital subtraction angiography results showed that a significant blood supply had become established, and the blood vessels in the sole began to sprout into the dorsum of the foot (Figure 2(a)). On the basis of this establishment of a blood supply to the wound, we performed multiple debridement and skin grafting procedures to accelerate wound healing (Figure 3(c)). An additional 4 months of treatment resulted in restoration of the blood supply to the right foot and revascularization of the dorsal aspect of the foot (Figure 2(a)). The blood supply returned to normal after 7 months (Figure 2(b)). During the final follow-up, computed tomography angiography and three-dimensional computed tomography angiography revealed the establishment of a robust vascular network in the foot after 8 months of treatment (Figure 2(c), (d)). The patient’s pain score correspondingly exhibited a gradual but substantial decrease from admission to 3 months of treatment. The patient then reported complete absence of pain in the right lower limb, and the wound healed well (Figure 3(d)).

Patient’s condition after carbon dioxide fractional laser treatment of the wound. (a) Digital subtraction angiography image of the vascular supply to the foot 3 months after treatment. (b) Digital subtraction angiography image showing angiogenesis in the dorsalis pedis region of the right foot 7 months after treatment. (c) Computed tomography angiography image of lower extremity arteries 8 months after treatment and (d) three-dimensional computed tomography angiography performed for evaluation of lower extremity arteries 8 months after treatment. (The yellow arrow indicates the presence of new vessels in the dorsalis pedis region).
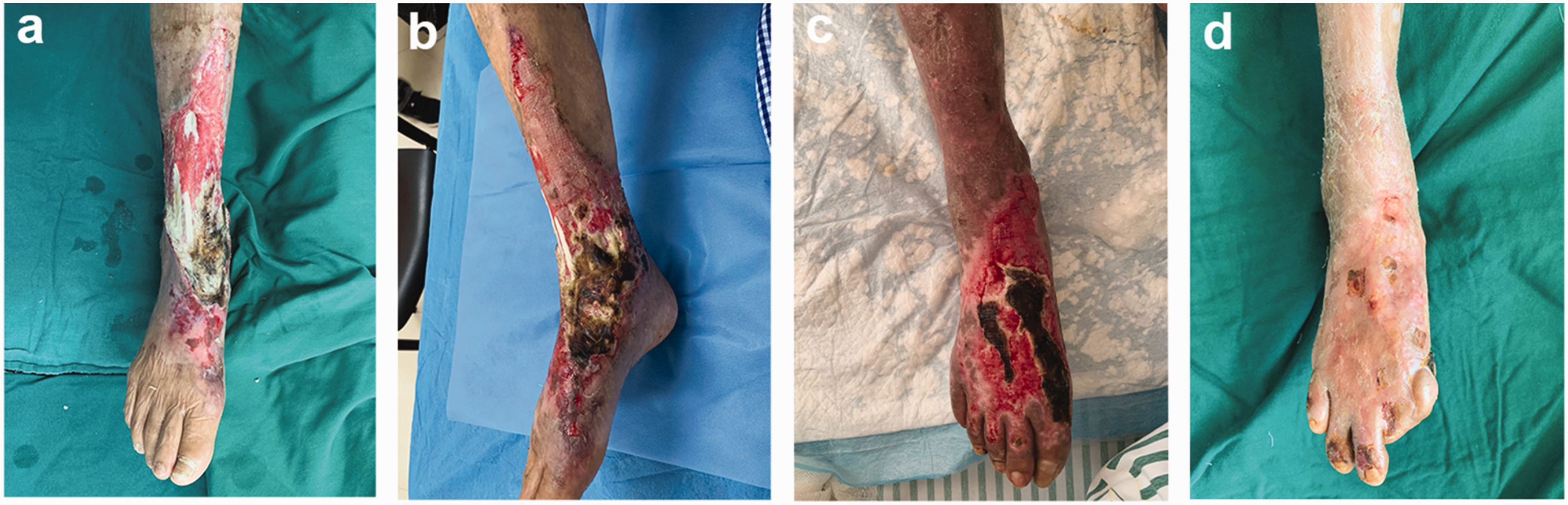
(a) View of the 20- × 6-cm shin wound after debridement. (b) View of the wound 7 days after carbon dioxide fractional laser (CO2FL) therapy and skin graft implantation. (c) View of the wound 3 months after CO2FL treatment and (d) view of the healed wound 8 months after CO2FL treatment.
The reporting of this study conforms to the CARE guidelines. 13
Discussion
Treatment of diabetic foot disease requires multidisciplinary techniques aiming to achieve revascularization and wound healing. Blood glucose regulation is a precondition for treatment. In the complex pathology of lower limb ischemia, interventional ultrasound can guide revascularization and help to develop a novel standardized approach to manage the arterial circulation of the lower limbs.14,15 Moreover, interventional radiology plays a vital role in the treatment of diabetic foot, whereas balloon expansion and stent implantation are fundamental measures for ensuring circulation patency. A new interventional approach for revascularization was reported by Cangiano et al. 16 The authors created an arteriovenous fistula with intravascular ultrasound-guided percutaneous deep vein arterialization to treat patients with chronic critical limb ischemia, and they achieved technical success and a notable limb salvage rate (78%). 16 Furthermore, periosteal distraction and bone transport showed good clinical effects in promoting microcirculation in the lower extremities. 16 Previous studies have verified that the stretch–stress mechanical stimulus can promote the regeneration of capillaries and tissues. The process of distraction histogenesis can recreate a vascular network, which enhances the wound repair process.17,18
Notably, the ulcer in the middle of the tibia was atypical in this patient. The precise execution of periosteal distraction and bone transport in this specific region poses a significant risk of postoperative subperiosteal or bone marrow infection. 19 In this case, we identified a commonly employed technique, CO2FL therapy, which has been demonstrated to be effective in accelerating the healing of persistent wounds.12,20 Angiogenesis is a crucial process for tissue repair and regeneration. Previous studies have confirmed that CO2FL therapy can stimulate angiogenesis in treated areas. 21 The photothermal effect of the laser induces collagen remodeling and triggers the release of growth factors, cytokines, and other signaling molecules that promote angiogenesis and tissue repair. Consequently, CO2FL therapy has the potential to not only expedite wound healing but also enhance microcirculation through the promotion of angiogenesis, which is valuable in managing diabetic foot ulcers affecting the middle tibial region.
Conclusions
In this study, we investigated the effectiveness of CO2FL treatment in managing patients with lower extremity arterial occlusion, diabetes mellitus, and lower extremity ulcers. Our findings confirm that CO2FL therapy is a straightforward, safe, and precise approach for enhancing the microcirculation in ischemic lesions of the lower extremities. In the present case, the combined approach of vascular interventional surgery and CO2FL therapy on the lower extremities contributed to transformation of the blood supply to the patient’s right foot from a state of virtual absence to one of abundance. Further research incorporating microcirculatory monitoring techniques is warranted to gain a comprehensive understanding of the effectiveness of CO2FL therapy in managing lower extremity arterial occlusion, diabetes mellitus, and lower extremity ulcers.
Research ethics and patient consent
All procedures were approved by the Ethics Committee of the First Affiliated Hospital of Anhui Medical University (PJ2023-11-46). The reporting of this study conforms to the CARE guidelines. Written informed consent was obtained from the patient for treatment and for publication of this case report and accompanying images. The patient’s details have been de-identified.
Footnotes
Authors’ contributions
DX proposed the study concept, devised the methods, and was a major contributor to writing the manuscript. YZ reviewed and edited the manuscript. WS and XF collected and analyzed the clinical data. ZZ contributed to visualizing the conception. LQ performed the procedure and collected the clinical data. XC administered and supervised the project and edited the final manuscript. All authors read and approved the final manuscript.
Data availability statement
Not applicable.
Declaration of conflicting interests
The authors have no conflicts of interest.
Funding
This work was supported by the National Natural Science Foundation of China (82372517) and the Postgraduate Innovation Research and Practice Program of Anhui Medical University (YJS20230013).
