Abstract
Objective
Sepsis is a complex clinical condition caused by a dysregulated immune response to an infection resulting in a fatal outcome. This study aimed to investigate the value of urine soluble triggering receptor expressed on myeloid cells (sTREM-1) for diagnosing culture-proven sepsis in preterm infants.
Methods
Preterm neonates were evaluated for late-onset sepsis (LOS). Laboratory investigations were performed. Urine sTREM-1 samples and blood cultures were synchronously collected. Using blood culture results, preterm neonates were divided into the culture-proven group and suspected sepsis group.
Results
A total of preterm 62 infants were included in the study; 31 had culture-proven sepsis and 31 were suspected as having sepsis. There were no significant differences in gestational age, sex, birth weight, and delivery mode between the groups. Neonates in the culture-proven group had significantly higher urine sTREM-1 levels than did those in the suspected sepsis group. Using a cut-off point for a urine sTREM-1 level of 78.5 pg/mL, the sensitivity was 0.90, specificity was 0.78, positive predictive value was 0.68, and negative predictive value was 0.94.
Conclusions
The present study highlights the role of urine sTREM-1 levels in LOS. Urine sTREM-1 may be a reliable and sensitive marker in detecting sepsis in preterm infants.
Introduction
Neonatal sepsis is an important cause of illness and death in developed and developing countries. 1 According to the World Health Organization, approximately 4 million infants die each year from sepsis, and a major proportion of these deaths is in developing countries and infections are high in the list of disease causes.1,2 The gold standard for sepsis is to isolate the agent in blood culture. However, even in the best centres, producing a pathogen is not possible for many reasons. Therefore, studies have searched for blood culture, as well as clinical and laboratory-assisted diagnostic methods, for diagnosing neonatal sepsis.3,4
Ideally, assistive diagnostic methods should be able to identify sepsis at a high rate to exclude sepsis if it is not present. However, because none of the screen tests are sensitive enough to identify infection, clinical evaluation is important for diagnosing sepsis and for initiating empirical treatment. Biomarkers are frequently used in the diagnosis and monitoring of sepsis. 5 Many markers, such as acute phase reactants, pro- and anti-inflammatory mediators, and cell surface antigens, have been used in studies. 6
Triggering receptor expressed on myeloid cells (TREM-1) is a glycoprotein and a member of the immunoglobulin family. TREM-1 is an important receptor for the inflammatory response upregulated by neutrophils and monocytes in the presence of inflammation and for diagnosing sepsis. 7 This glycoprotein is regulated by neutrophils following contact of monocytes and macrophages with lipopolysaccharides, and by Gram-positive bacteria, Gram-negative bacteria, or fungi. During inflammation, there is an increase in the neutrophil count, and this causes an increase in TREM-1 levels in case of sepsis. Furthermore, the fact that there is no increase in TREM-1 levels in noninfectious situations, as shown in recent studies conducted on adults, suggests that TREM-1 may be particularly sensitive for making the diagnosis of sepsis.7,8
The soluble form of TREM-1 (sTREM-1) is released by activated phagocytes and is present in all body fluids. 8 This soluble form is closely related to infection. There have been many studies of sTREM-1 in adults, including showing increased serum levels of sTREM-1 in body fluid samples for various diseases and conditions.9–11 This finding suggests that sTREM-1 may be a marker for diagnosing sepsis in preterm infants. There have also been studies in newborns on serum sTREM-1 levels to detect sepsis. 12
However, while studies on adults have suggested that sTREM-1 levels in urine can predict sepsis, whether sTREM-1 levels in urine can predict sepsis in preterm infants is unknown. Diagnosing sepsis in preterm infants is difficult, which is an important problem, especially in developing countries. Therefore, this study aimed to investigate the predictive effect of urinary sTREM-1, a noninvasive marker, in late-onset sepsis (LOS).
Patients and methods
Study design and interventions
This prospective, observational study was conducted in a level III neonatal intensive care unit (NICU) at Tepecik Training and Research Hospital, between January 2013 and January 2014. The NICU unit at Tepecik Training and Research Hospital is an international destination for treating rare and complex medical conditions in neonates. The recognized team of the unit comprises physicians, fellows, surgeons, and nurses who offer state-of-the art care. Each year, > 10,000 births occur and nearly 1500 neonates are admitted to the NICU. The exclusion criteria for the study were major congenital anomalies, congenital infections, infants born to mothers with clinical chorioamnionitis or those who had early-onset neonatal sepsis, perinatal asphyxia, sedation, symptomatic patent ductus arteriosus, nephrological problems at admission, and patients in a terminal state.
The study was approved by the local ethics committee of Tepecik Training and Research Hospital, and informed consent was obtained from the parents before enrolment (2013-40/1). The postnatal ages of all included neonates were older than 5 days with clinical and laboratory signs of sepsis. Only preterm infants whose serum renal function tests and urine output were within normal limits were included in the study. Cases of oliguria or polyuria were excluded.
Diagnosis of sepsis
The greatest problem in managing neonatal sepsis is obtaining a correct diagnosis. Newborns, especially preterm infants, have subtle clinical findings and multiple situations may mimic neonatal sepsis. 13
The diagnosis of sepsis was based on at least two clinical and two laboratory criteria. 14 The clinical criteria were as follows: hyperthermia (core body temperature ≥ 38°C), hypothermia < 36°C, or temperature instability; tachycardia (heart rate > 160 beats/min), bradycardia (heart rate < 100 beats/min), or rhythm instability; tachypnoea (respiratory rate > 60 breaths/min) or recurrent apnoea > 20 s; increased oxygen requirements or requirement for ventilator support; feeding intolerance suspected by the presence of gastric residuals, abdominal distension, gross or occult blood in the stool, and the onset of crises of apnoea/bradycardia; abdominal distension, lethargy and hypotonia; hypotension < 5th percentile for age or systolic blood pressure < 2 SD below normal for age; and skin and subcutaneous lesions, such as mottling and sclerema.
The laboratory criteria were as follows: metabolic acidosis, thrombocytopenia, leukopenia/leukocytosis, immature/total neutrophil ratio > 0.2, and C-reactive protein (CRP) levels > 10 mg/L.15,16 Because there is no consensus for preterm infants, we included both leukopenia and leukocytosis. A positive blood culture in the presence of clinical signs and symptoms of infection was defined as culture-proven sepsis. We defined coagulase-negative staphylococcus as the presence of two positive blood cultures or one positive blood culture plus a positive CRP. The presence of clinical signs and symptoms of infection and at least two abnormal laboratory results when blood culture was negative was verified as suspected sepsis. 16 To exclude false positive results, we considered contamination/colonization if there was no evidence of sepsis in the laboratory and clinically in neonates. The diagnosis was verified by a positive blood culture. 17
Group classification
The preterm infants were classified in the groups according to the same study protocol. According to the results of automatized blood cultures, the studied septic neonates were classified into two groups: culture-proven sepsis and suspected sepsis. All patients who were consecutively admitted to the NICU for suspicion of sepsis were included in the study. The initial laboratory investigations included the white blood cell (WBC) count, platelets (PLT), CRP levels, blood urea nitrogen (BUN) levels, and serum creatinine (SCr) levels, as well as blood cultures. We included neonates with proven (positive blood cultures for microbes or fungi) and suspected sepsis, but with negative blood cultures. Urine sTREM-1 samples and blood cultures were synchronously collected.
Blood sampling and assays
Blood samples and cultures were collected from peripheral veins. Peripheral blood samples were collected in ethylene diamine tetra-acetic acid (1.2 mg/mL) for a complete blood count (CBC) and analysed by flow cytometry (Beckman LH 780; Beckman Coulter, Brea, CA, USA). For blood culture, 1 mL of blood was obtained and placed into two culture bottles containing broth to grow aerobic and anaerobic microorganisms.
CRP levels were measured by scattering immunoturbidimetry (Beckman Coulter AU5800). BUN levels were measured by a kinetic UV test (Beckman Coulter AU5800) and SCr levels by a colorimetric-kinetic technique (Beckman Coulter AU5800). All assays were performed in strict accordance with the manufacturers’ instructions.
Urine samples were drawn with urethral catheterization at the time of the initial laboratory evaluation for sepsis and centrifuged at 7462 ×g for 5 min. Urine sTREM-1 samples were simultaneously collected for laboratory tests and blood cultures when sepsis was suspected.
Supernatant was placed into Eppendorf tubes and stored at −80°C. All of the samples were renumbered before the experiment. Urine sTREM-1 levels were measured by using a double-antibody enzyme-linked immunosorbent assay (human urine sTREM-1 ELISA kit product number: 201-12-0311; Sunred Biological Technology Systems, Shangai, China). After stop solution was added, the optical density was determined by using a microplate reader (Biotech ELX-800 Microplate Reader; BioTek Instruments, Inc., Winooski, VT, USA) that was set at 450 nm with a 570-nm wavelength correction according to the manufacturer’s instructions. Levels of sTREM-1 were expressed as pg/mL. The analysts were not informed about the neonates’ culture results. All collected urine samples were measured at the same time and the total time to obtain result of all urine sTREM-1 samples was only 3 h.
Therapeutic strategy
In the hospital, when sepsis was suspected, empirical antibiotic therapy was initiated in neonates depending on the blood culture results. Coagulase-negative staphylococci were the predominant causative organisms for LOS, and Staphylococcus aureus and Gram-negative bacteria were common pathogens in preterm infants. According to the Turkish Neonatal Society, the most commonly isolated microorganisms in NICUs are coagulase-negative staphylococci and Klebsiella pneumoniae. An initial empirical antibiotic therapy for LOS was designed with vancomycin + cephalosporins/meropenem as the best combination to cover this spectrum until the culture results arrived. 18 Antibiotics were re-evaluated when the results of the cultures were available. 19
Statistical analysis
Analysis of the data was performed using the Statistical Program for Social Science version 18.0 software (SPSS Inc., Chicago, IL, USA). The Kolmogorov–Smirnov test was used to test the normal distribution of variables. Numerical data are described as mean ± standard deviation (SD). To compare quantitative variables between the two groups, the parametric Student’s t-test was applied. Qualitative variables are described as number and percentage and comparisons were performed using the chi-square test. Spearman’s rank correlation coefficient and multi-regression linear analysis were used to assess the relationships between sTREM-1 levels and the clinical and laboratory variables. Multi-regression analysis was performed to evaluate urine sTREM-1 levels for predicting the prognosis.
The receiver operating characteristic (ROC) curve was used to determine the optimal cut-off value and the area under the curve (AUC) was calculated for each plot. A p value < 0.05 was considered significant.
The sensitivity, specificity, and positive and negative predictive values of clinical findings related to urine sTREM-1 levels were calculated with the following formulas:
Sensitivity = true positives/(true positives + false negatives) × 100
Specificity = true negatives/(true negatives + false positives) × 100
Positive predictive value = true positives/(true positives + false positives) × 100
Negative predictive value = true negatives/(false negatives + true negatives) × 100
Results
Patients’ characteristics
During the study period, 150 preterm infants with a birth weight ≤ 1500 g were admitted to the NICU of which 103 were deemed suitable for the study. Forty-one preterm infants were excluded because of the absence of parental consent (n = 10), the presence of congenital heart disease (n = 3), diagnosis of early-onset sepsis/pneumonia (n = 3), a symptomatic patent ductus arteriosus that required treatment (n = 6), and inadequate sampling (n = 19; 14 patients in the suspected sepsis group and five in the culture-proven group). Sixty-two preterm infants were studied, with 31 in the culture-proven group and 31 in the suspected sepsis group.
Table 1 shows a general summary of the patients’ demographic and clinical characteristics in the trial. There were no significant differences between the groups regarding gestational age, sex, birth weight, and delivery mode.
Characteristics of the preterm infants

Values are mean ± SD or n (%). NVD: non-vaginal delivery, CS: caesarean section.
The most common microorganisms that were isolated from blood cultures were Gram-positive microbes (n = 25), followed by Gram-negative microbes (n = 6). As shown in Table 1, preterm infants in the culture-proven group had a significantly lower birth weight compared with those in the suspected sepsis group (p = 0.02).
In the neonatal period, the Tollner score and the Score for Neonatal Acute Physiology Perinatal Extension are used to assess sepsis at first admission. The Tollner score in the culture proven group was > 10 and that in the suspected sepsis group was 5–10.
Comparison of laboratory findings
The WBC count in the culture-proven group was significantly higher than that in the suspected sepsis group (p = 0.03). The PLT count, BUN levels, and SCr levels were similar in both groups (Table 2). Urine sTREM-1 levels were significantly higher in the culture-proven group compared with the suspected sepsis group (p < 0.001) (Table 2). No correlation was found between baseline sTREM-1 and CRP levels (r = 0.14, p = 0.25).
Comparison of laboratory findings between the groups

Values are mean ± SD. WBC: white blood cell, PLT: platelets, BUN: blood urea nitrogen, SCr: serum creatinine, sTREM-1: soluble triggering receptor expressed on myeloid cell levels.
Multi-regression analysis was performed to evaluate urine sTREM-1 levels for predicting the prognosis for neonates with sepsis. We found that urine sTREM-1 levels were an independent factor for predicting culture-positive sepsis (p < 0.001).
ROC curve analysis for the cut-off of urine sTREM-1 levels
ROC curve analysis was performed for urine sTREM-1 levels. The AUC was 0.87 for urine sTREM-1 levels (Figure 1). Using a cut-off point for a urine sTREM-1 level of 78.5 pg/mL, the sensitivity was 0.90, the specificity was 0.78, the positive predictive value was 0.68, and the negative predictive value was 0.94 (Table 3).
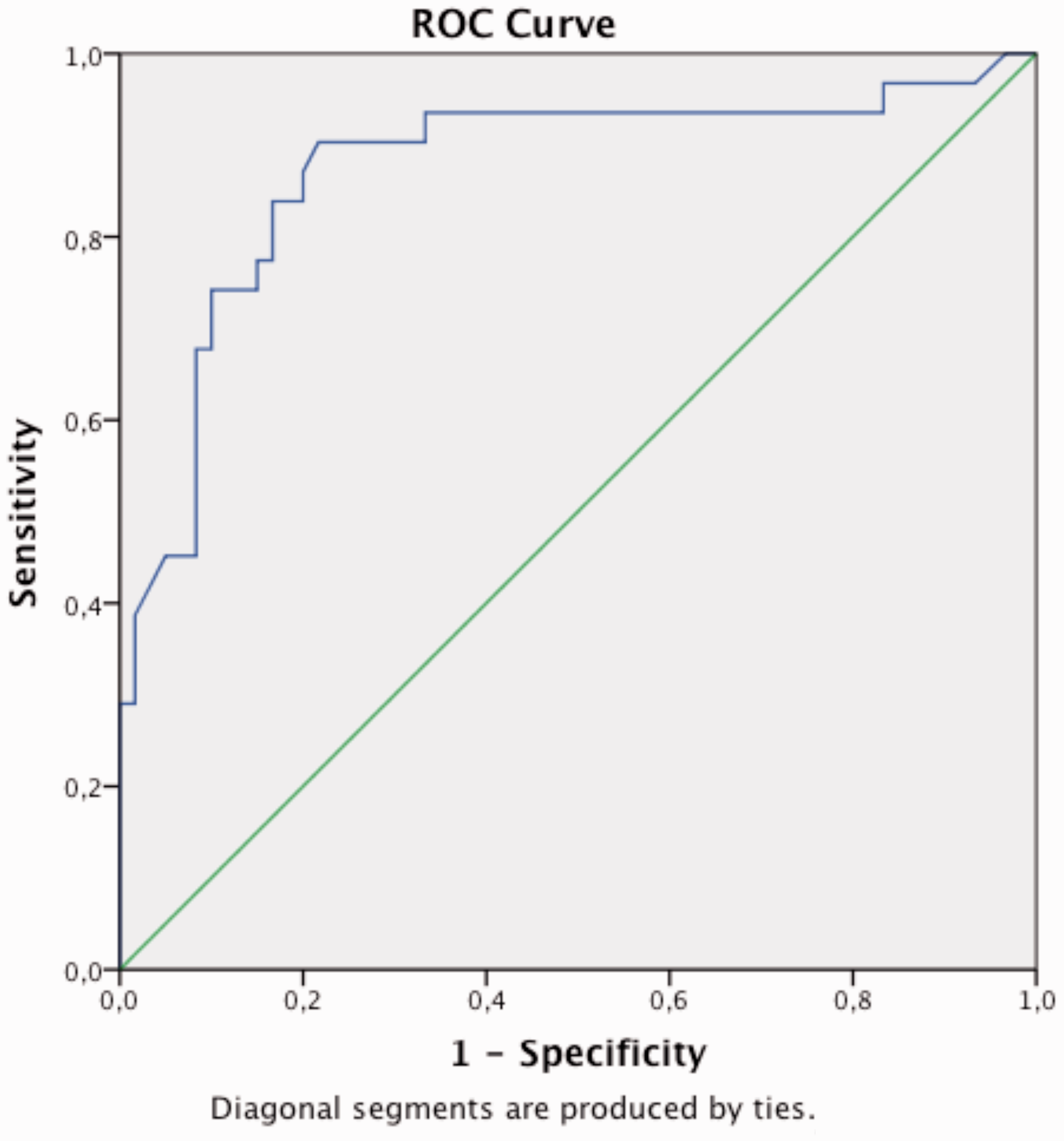
Receiver operating characteristic curves of the sensitivity and specificity of urine soluble triggering receptor expressed on myeloid cell levels in the study group
Diagnostic accuracy of urine sTREM-1 levels

The 95% confidence interval is shown in parentheses.
sTREM-1: soluble triggering receptor expressed on myeloid cell levels, PPV: positive predictive value, NPV: negative predictive value.
Discussion
In this study, urine sTREM-1 levels were significantly elevated in the culture-proven group compared with the suspected sepsis group. Preterm infants with culture-positive sepsis had significantly higher urine sTREM-1 levels than did those who had culture-negative sepsis. Although comparing urine sTREM-1 and CRP levels was not the purpose of the study, we found that urine sTREM-1 levels were better than CRP levels as a diagnostic marker for culture-proven, late-onset, neonatal sepsis. The signs and symptoms of sepsis can be subtle and nonspecific. Therefore, laboratory evaluation is performed in any infant with identifiable risk factors, with physical findings consistent with sepsis, or those who deviate in any way from the usual pattern of activity or feeding. Suspected sepsis is one of the most common diagnoses made in the NICU. Isolation of a microorganism from blood culture is the gold standard to confirm the diagnosis of neonatal sepsis. However, there is a considerable delay before blood culture results are available. Although automated blood culture systems are more advanced, fastidious organisms and inadequate specimen volumes decrease the sensitivity of neonatal blood cultures. Therefore, an empirical antibiotic therapy is usually started.20,21,22
Preterm infants are 20 times more likely to develop infection than term infants. Additionally, many invasive interventions increase the risk of LOS in preterm infants. Therefore, being vigilant and treating sepsis as early as possible are important, especially in very low birth weight infants. 23 Promising biomarkers are interleukin-6, interleukin-8, and tumour necrosis factor-α for the early phase of sepsis, whereas procalcitonin is promising for the mid phase and CRP is promising for the late phase. The ideal marker for sepsis should have high sensitivity in recognizing infection at the early stage, be inexpensive, and most importantly, be noninvasive. We paid approximately $3 (USD) for each sample. The budget was paid from Katip Çelebi University Department of Scientific Research ($300 was paid).
TREM-1 is an important receptor involved in the innate inflammatory response and sepsis.24,25 In the present study, sTREM-1 samples were collected early in suspecting sepsis in all neonates. Because mortality may be increased in LOS in preterm infants, starting early antibiotic treatment is important while awaiting blood culture results. Our findings support the role of urine sTREM-1 levels as a potentially easy and reliable marker in neonatal sepsis while awaiting culture results. Moreover, we found that sTREM-1 levels had a significant negative predictive value and its sensitivity reached 0.90. Adly et al. 26 assessed serum sTREM-1 levels in 112 septic neonates (63 culture-positive and 49 culture-negative) and 40 healthy controls as a potential early diagnostic and prognostic marker for neonatal sepsis, and compared them with CRP levels. 26 They found that sTREM-1 levels were superior for detecting sepsis compared with CRP. They also found that serum sTREM-1 levels were negatively correlated with gestational age and birth weight. Similarly, in another trial, serum sTREM-1 levels were negatively correlated with birth weight, while there was no significant correlation with gestational age. 27 In this study, preterm infants with culture-proven sepsis had higher urine sTREM-1 levels than did those with suspected sepsis. This finding may be related to weight at diagnosis. However, there are no data on urine sTREM-1 levels according to weight and gestational weeks. Nevertheless, urine sTREM-1 levels were easy to assess and cost-effective, and the AUC for urine sTREM-1 was 0.87.
In our study, there was no correlation between CRP and urine sTREM-1 levels. Similar to our findings, Sarafis et al. 28 investigated serum sTREM-1 and interleukin-6 levels in 31 neonates, nine with suspected LOS and 22 with culture-positive LOS. They found that blood sTREM-1 levels resulted in early identification of infected neonates. A study performed on adults investigated the diagnostic value of urine sTREM-1 levels for identification of early sepsis, severity and prognosis assessment, and secondary acute kidney injury. 29 This previous study showed that the urine sTREM-1 test is more sensitive than the WBC count, CRP levels, and procalcitonin levels for early diagnosis of sepsis, as well as for dynamic assessment of severity and prognosis. Additionally, the cut-off level for urine sTREM-1 was 69.04 pg/mL with 0.94 sensitivity and 0.76 specificity. The present study provided evidence that urine sTREM-1 levels may be more sensitive than CRP levels for assessing neonatal nosocomial infections, which have not been previously studied in preterm infants.
Palmiere et al. 30 evaluated urine sTREM-1 levels in postmortem septic cases and found that they ranged from 11.2 pg/mL to 380.9 pg/mL, with a mean value of 102.9 pg/mL. The urine sTREM-1 cut-off value was calculated as 90 pg/mL in their study. Oku et al. 31 measured sTREM-1 levels and found that septic adult patients had significantly high sTREM-1 levels and these were correlated with the severity score. This finding is in line with a recent meta-analysis involving 13 studies in adults, where serum sTREM-1 levels were reliable in bacterial infection, with a sensitivity of 0.82 and specificity of 0.86. 32 We defined that a cut-off value of sTREM-1 ≥ 78.5 pg/mL could be diagnostic of LOS in culture-proven septic neonates with a sensitivity of 0.90 and specificity of 0.78. There are scarce data regarding sTREM-1 levels in preterm infants with LOS.
A recent study in children investigated whether sTREM-1 is present in urine samples from children with a urinary tract infection and in samples from healthy children. 33 All of the patients (healthy and diseased) in this recent study showed TREM-1 expression, but diseased children had TREM-1 percentages of > 10%, while in the non-infected group, only 35% presented with similar levels. These findings suggest the usefulness of determining TREM-1 levels in childhood infections as a potential diagnostic test.
Our study has several implications. This is the first study to show that urine sTREM-1 levels may predict LOS in preterm infants. This research combined urine sTREM-1 levels with the results of blood culture to evaluate their value. We showed that urine sTREM-1 levels were significantly higher in culture-proven sepsis than in culture-negative sepsis in preterm infants. This potential marker is inexpensive and it could be useful in developing countries.
Limitations of the present study are the small sample size and absence of changes in the dynamics of sTREM-1 and CRP levels during the course of sepsis. This study also did not investigate the association between morbidities and urine sTREM-1 levels.
In conclusion, the present study highlights the role of urine sTREM-1 levels in LOS. We conclude that this may be a reliable and sensitive marker in detecting sepsis in preterm infants. Besides being noninvasive, urine sTREM-1 levels are easy to assess and can also provide an early warning of culture-positive sepsis in preterm infants. However, further large, prospective studies are required to confirm our conclusions.
Comments
This study was presented at the European Academy of Pediatrics Young Investigator Awards section in the European Academy of Pediatrics 2016, Geneva.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
Financial support was provided by Izmir Katip Celebi University for the sTREM-1 ELISA kit.
