Abstract
While there are many reports on partial aortic root remodelling, it is rarely performed for chronic aortic dissection of the coronary artery. This case report describes a 71-year-old male patient with chronic aortic dissection who was admitted to hospital due to repeated palpitations and chest distress. He had a long-term occlusion of the right coronary artery and an abnormal origin of the left vertebral artery. A carefully planned surgical strategy was arranged for this patient, and the surgical experience is described and discussed herein. Briefly, the patient was treated by aortic root repair plus ascending aorta replacement plus Sun's procedure plus left vertebral artery graft implantation plus coronary artery bypass graft (right coronary artery to saphenous vein to innominate artery). At approximately 6 months following surgery, the patient had returned to normal living conditions without any reports of discomfort.
Teaching points
For the treatment of aortic dissection combined with Neri type C coronary artery, coronary artery bypass grafting is recommended to completely cure the coronary ostium lesions. For patients with aortic dissection involving coronary arteries, preoperative decision-making needs to fully consider the poor perfusion effect of myocardial antegrade perfusion, and coronary retrograde perfusion is an effective alternative at this time. For patients with aortic dissection involving the coronary arteries, use of superior and inferior vena cava cannulation is an effective and safe strategy in the establishment of extracorporeal circulation to cope with coronary retrograde perfusion at any time.
Introduction
Coronary malperfusion is a deadly complication of aortic dissection, 1 with a reported rate of 7% on postmortem examination. 2 Moreover, coronary malperfusion secondary to aortic dissection is associated with a high postoperative mortality rate.3,4 However, reports of occurrence, classification, and surgical management are scarce. The optimal treatment modality remains unclear, and no specific guidelines have been outlined. Here, the case of an elderly male patient with aortic dissection complicated with Neri type C coronary occlusion is reported. We believe that combined immediate coronary artery bypass grafting (CABG) and aortic repair remains a safe, effective, and acceptable approach to this challenging patient group.
Case report
The study was reviewed and approved by the Ethics Committee of the First Affiliated Hospital of Wannan Medical College, and the patient provided written informed consent for publication of this case report and any accompanying images. The reporting of this study conforms to CARE guidelines. 5 A 71-year-old male patient was admitted to the Department of Cardiothoracic Surgery, First Affiliated Hospital of Wannan Medical College (Yijishan Hospital), Wuhu, China in June 2022, with repeated palpitations and chest distress lasting for more than 1 month. He reported an incidence of severe chest pain 1 month previously that resolved without formal examination or treatment, but recently felt that the chest tightness and palpitations had been worsening. The patient reported residing in the countryside as a farmer, with daily crop-planting activities. He reported having two sons and two daughters, and that only the youngest son lived with him. The main factor that led to him seeking a physical examination was an incidence of obvious severe pain in his chest and back, accompanied by suffocation, after giving a physical helping push to a villager struggling to ride a tricycle up a steep slope. The symptoms resolved without formal examination or treatment, and he returned to his usual busy farming activities. He reported worsening chest tightness and palpitations that were mainly concentrated on the front chest, as if there was a heavy stone pressing on him, and he was unable to walk without help, which led to him seek medical assistance at a local hospital. A chest computed tomography (CT) scan showed an ascending aortic aneurysm, and he was transferred to the First Affiliated Hospital of Wannan Medical College (Yijishan Hospital). He reported a history of hypertension for 5 years, and regular administration of antihypertensive drugs (10 mg nifedipine extended-release tablets, orally, once daily), which effectively controlled his blood pressure. He also had a 20-year history of smoking approximately 20 cigarettes per day. He reported no family history of chest tightness, palpitations, or chest pain.
On admission, his blood pressure was 130/78 mmHg (left upper limb), 120/80 mmHg (right upper limb), 104/67 mmHg (left lower limb) and 120/82 mmHg (right lower limb). An electrocardiogram (ECG) showed atrial premature beat and left ventricular hypertrophy. Computed tomography angiography (CTA) of the aorta and coronary artery (
Surgical procedure
The patient was diagnosed with chronic aortic dissection with right coronary artery occlusion, and prepared for surgery. The surgical treatment plan comprised aortic root repair plus ascending aorta replacement plus Sun's procedure plus left vertebral artery graft implantation plus CABG (right coronary artery to saphenous vein to innominate artery).
Before the operation, the anaesthesiologist routinely administered intravenous sufentanil combined with propofol to induce general anaesthesia. Anaesthesia was maintained with intravenous propofol, and muscle relaxants were intermittently administered. During the operation, one group of surgeons (HW and HZ) routinely dissociated the great saphenous vein of the right lower limb, and the other group (DZ, TT, and JW) routinely opened the chest through a median sternal incision to dissociate the innominate vein and artery, left common carotid artery, left vertebral artery and left subclavian artery. The veins were then heparinized. After cutting the pericardium, the ascending aorta was observed to be obviously dilated, with a diameter of 7 cm, displaying chronic changes. A single origin of the left vertebral artery could be seen at the aortic arch, and a 7-0 prolene suture was used to anastomose end to side with the distal end of the left common carotid artery after disconnecting the proximal end. An artificial blood vessel with a diameter of 10 mm was selected to anastomose with the innominate artery end to side and insert a 24 F arterial tube into the aorta. The ascending aorta and right upper pulmonary vein were sutured by the purse-string technique, and the perfusion tube and left heart drainage tube, respectively, were inserted into them. The superior and inferior vena cava were also sutured by the purse-string technique, and then intubated, respectively, to establish cardiopulmonary bypass. After cooling and ascending aorta occlusion, the ascending aorta was cut open, revealing the aorta double lumen alteration, with a huge and thickened false lumen (Figure 1). The left coronary was then exposed, and the perfusion tube was filled with blood hyperkalemic depolarizing cardioplegia solution. As the right coronary artery was occluded, the perfusion strategy was to open the right atrium and supplement the reverse perfusion through the coronary sinus. The above approaches provided a satisfactory setting for arresting the heart. The aorta was then incised longitudinally. The ascending aorta was completely severed and the proximal end was reinforced with artificial vascular strips.
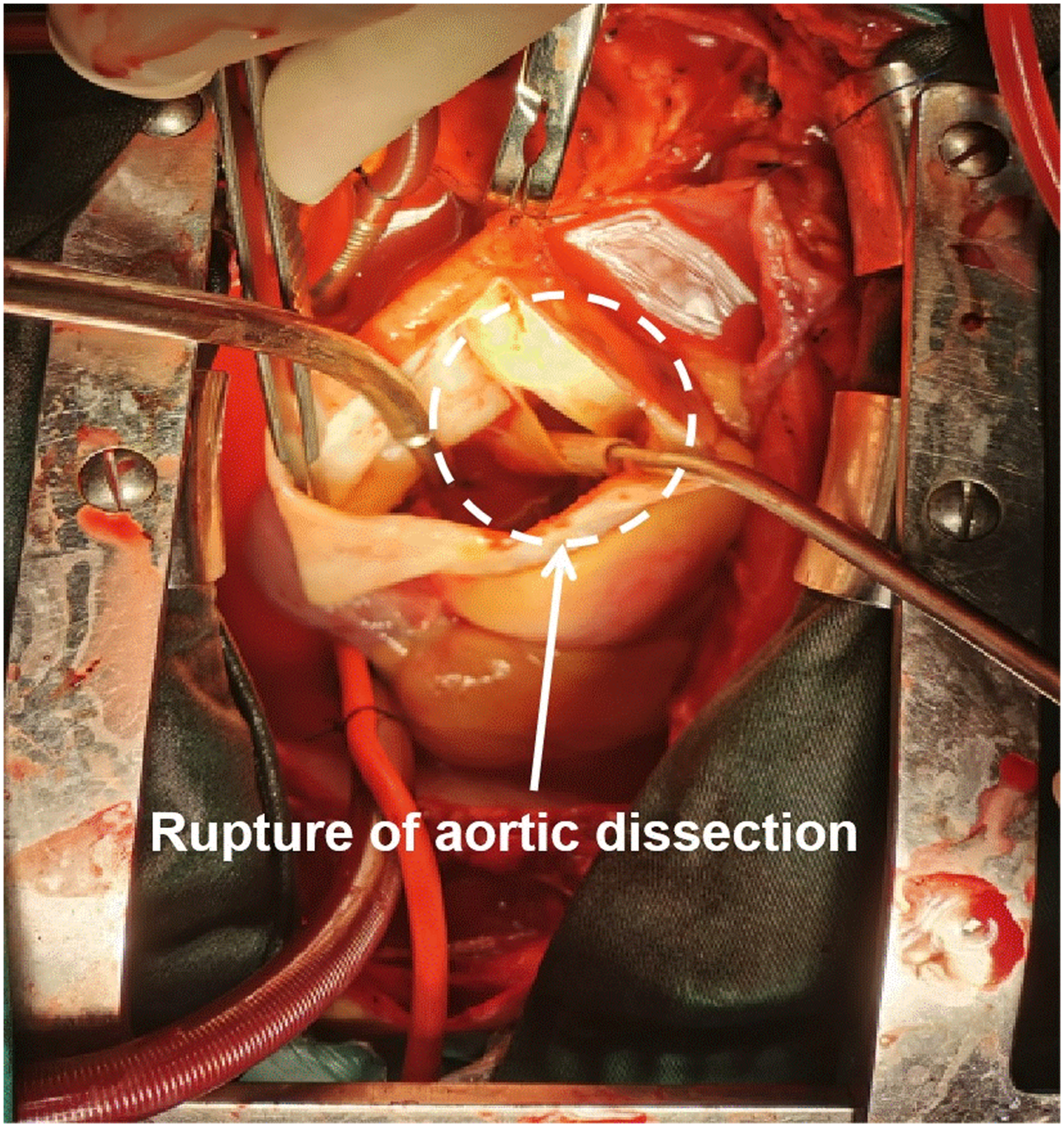
Intraoperative image from a 71-year-old male patient with chronic aortic dissection and right coronary artery occlusion, showing rupture of the aortic dissection (white dotted circle).
Deep hypothermia circulatory arrest was started when the nasopharyngeal temperature dropped to 25°C. The left subclavian artery was clamped with double Hem-o-lock clips and severed after three branches above the arch were blocked. The distal end was cut to the edge from the aortic arch to the root of the left common carotid artery. Exploration revealed that the breach of the intima of the aortic arch was at the greater curvature side, and a 26 × 100 mm intraoperative elephant trunk stent was implanted. First, one end of the 28-mm four-branch artificial vessel trunk was sutured continuously using 4-0 prolene to anastomose with the elephant trunk stent and the aortic arch. After the distal anastomosis was completed, the second artery cannula was connected with the fourth branch perfusion tube of the four-branch vessels to restore lower body perfusion. Careful examination of the distal anastomotic stoma showed satisfactory results. Using 5-0 prolene continuous suture, the left common carotid artery was successively anastomosed. Puncture was performed for exhausting, the patient was gradually rewarmed, and the left subclavian artery was anastomosed. The other end of the main trunk of the four-branch artificial blood vessel was continuously anastomosed to the reinforced ascending aorta with 4-0 prolene suture. The main trunk of the right coronary artery was then dissociated, the anterior wall was cut, the incision was enlarged to 5 mm, the great saphenous vein was trimmed, and the great saphenous vein was anastomosed to the right coronary artery continuously with 7-0 prolene suture (Figure 2). The first branch of the four-branch blood vessel was used to eliminate air. Then, the ascending aortic occlusion was released and the heart automatically rebounded. Finally, the innominate artery was anastomosed with the first branch of the four-branch blood vessel, and every anastomosis was checked. After blocking the proximal and distal end of the artificial vessel and the innominate artery, the anterior wall was perforated with an electrosurgical pen. The great saphenous vein was then continuously anastomosed to the artificial vessel using 7-0 prolene suture. The total operation lasted 6 h 30 min. The durations of cardiopulmonary bypass, aortic occlusion, and deep hypothermia circulatory arrest were 232 min, 163 min, and 26 min, respectively. The patient was returned to the general ward on day 3 following surgery, and was discharged successfully on day 13 following surgery. After the surgery, the aorta was rechecked by CTA, as shown in Supplementary Video 2 and Supplementary Video 3, and no obvious internal leakage at the aortic arch or the thoracic segment of the descending aorta was observed. The innominate artery–right coronary bridge was visible on the CTA images (Figure 3). After 6 months following surgical treatment, the patient was reported to have returned to his normal living conditions, often planting crops with no reported discomfort, despite his children wanting him to follow a more relaxed daily lifestyle.
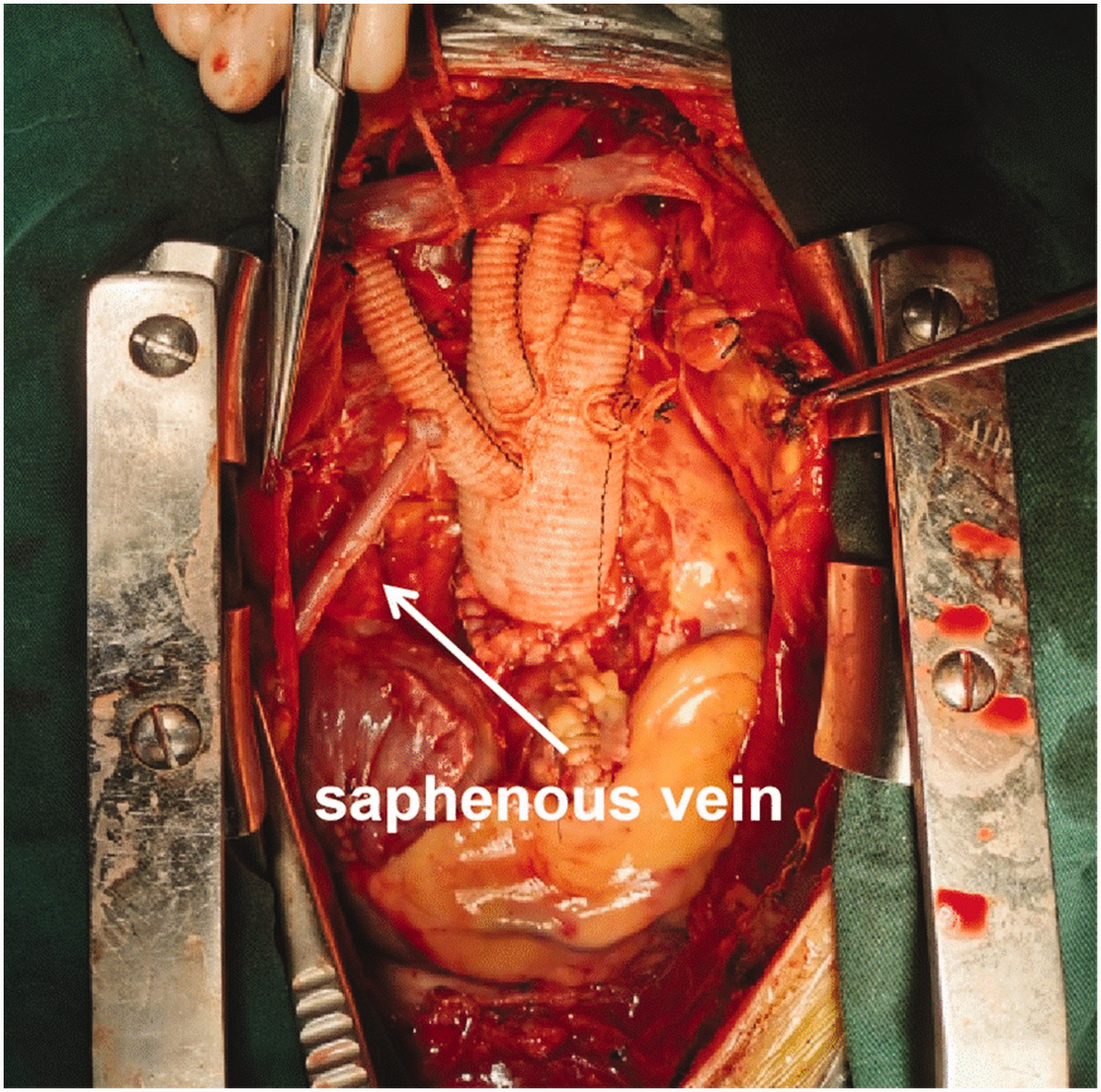
Intraoperative image from a 71-year-old male patient with chronic aortic dissection and right coronary artery occlusion, showing the great saphenous vein as the bypass vessel (white arrow).

Computed tomography angiography (CTA) in a 71-year-old male patient with chronic aortic dissection and right coronary artery occlusion, showing: (a) preoperative CTA image suggesting aortic dissection and aneurysmal bulging; and (b) postoperative CTA image suggesting satisfactory aortic repair.
Discussion
Stanford type A aortic dissection is an acute and dangerous aortic disease with rapid progression and high mortality rate. With continuous improvements in surgery and cardiopulmonary bypass technology, the prognosis of patients with Stanford type A aortic dissection treated by active surgery has been greatly improved. However, if the dissection involves the coronary artery, resulting in poor coronary perfusion, the prognosis is often poor, which is an important factor affecting early postoperative mortality. 6
Organ ischemia caused by major branch vascular involvement is an important pathophysiological change of aortic dissection. The incidence of aortic dissection involving the coronary artery has been previously reported as between 6% and 19%,7–9 and the probability of patients with poor coronary perfusion being misdiagnosed with acute coronary syndrome may be as high as 80%. 10 Misdiagnosed patients are prone to receive coronary angiography, antiplatelet drugs, thrombolysis and even coronary stent implantation, which has a negative impact on the next surgical procedure. 11 Poor coronary perfusion has been shown to significantly increase in-hospital mortality in patients with type A dissection versus those with adequate coronary perfusion (15% versus 9%). 12
In the present case, the patient had chronic aortic dissection with coronary artery disease. Preoperative aortic and coronary CTA found that the dissection involved occlusion of the right coronary artery, but the preoperative ECG did not indicate obvious myocardial infarction. At the same time, the myocardial enzyme index did not fluctuate abnormally. Neri et al. 4 classified coronary lesions due to proximal dissection into three main types: (1) type A, ostial dissection; (2) type B, dissection with a coronary false channel; and (3) type C, circumferential detachment with an inner cylinder intussusception. Uchida et al. 13 advocated coronary artery orthotopic transplantation for type A lesions; for type B and type C lesions, the torn coronary artery is repaired and reconstructed in situ by patch or autologous vein, to preserve the original artery branches and avoid competitive blood flow after CABG, which leads to re-tearing of the coronary intima and the formation of a new dissection. However, if the dissection involves the distal coronary artery, CABG is recommended. Some scholars believe that in situ reconstruction of the affected coronary artery is potentially dangerous, as it may be easy to damage the coronary artery and difficult to perform the operation, while CABG surgery is relatively simple and minimally invasive, with acceptable short-term and long-term prognoses. 14 At present, there is consensus in support of patients with type C lesions receiving CABG, but the treatment of patients with type B lesions remains controversial. Zhang et al. 15 recommend type B CABG directly, however, Kreibich et al. 3 suggest that selection should be according to intraoperative perfusion of the cardioplegic solution. For patients with a type B lesion with smooth antegrade perfusion, the opening should be shaped, and for those with poor perfusion, CABG should be performed. Some scholars have suggested that treatment should be selected according to the integrity of the coronary artery opening intima. 16 Coronary repair is the first choice for patients with complete coronary intima, and CABG is the first choice for patients with coronary intima rupture or disconnection. The present case belongs to type C coronary artery involvement. For patients with severe coronary artery ostium involvement; presence of crevasse; difficulty in forming, or high perfusion, pressure; long range of coronary artery tear; and foreseeable difficulty in eliminating the false lumen in the coronary artery, the current authors have used direct suture of the coronary artery ostium before treatment of aortic root lesions for preventive CABG. In the present case, in order to shorten the duration of the operation and myocardial ischemia, the great saphenous vein was selected as the graft.
Preoperative myocardial perfusion selection should be predicted in advance for such patients, with consideration to the combination of antegrade perfusion of the good coronary artery and retrograde perfusion or complete retrograde perfusion. For the vena cava intubation strategy, superior and inferior vena cava intubation is recommended, to avoid the unexpected situation of unsatisfactory conventional myocardial perfusion arrest. Careful and comprehensive identification of the origin of the branches of the arch blood vessels help to predict abnormal vascular shape in advance. In the present case, with the existence of a single left vertebral artery origin of the special circumstances of the arch, the choice of surgical approach was tailored to individual treatment, and the proximal end of the severed vertebral artery was anastomosed with the distal end of the left common carotid artery using a 7-0 prolene suture. Due to the long natural course of chronic aortic dissection, the preparation of the present case was comprehensive and the surgical plan was reasonable. The individualised treatment of the case was finally completed, and the patient's prognosis was good.
Conclusion
Aortic dissection involving the coronary artery is dangerous and complex, and misdiagnosis and mortality rates are high. Different surgical treatment strategies, according to different lesion types, are helpful to improve the prognosis of such patients. At present, there are still no authoritative standards for diagnosis, classification or treatment strategies, thus, further exploration and improvements are needed in practice.
Research Data
Research Data for Management of chronic Stanford type A aortic dissection combined with Neri type C coronary occlusion: a case report and literature review
Research Data for Management of chronic Stanford type A aortic dissection combined with Neri type C coronary occlusion: a case report and literature review by Tiansheng Tang, Ziao Wang, Wei Zhou, Hai Wang, Hanjun Zhang, Ayu Sun, Jun Wei, Weiyong Sheng and Dafa Zhang in Journal of International Medical Research
Footnotes
Author contributions
WS drafted the manuscript. DZ designed the study. TT revised the manuscript. ZW, JW, WZ, AS, HW, and HZ were responsible for the collection of data or analysis. All authors read and approved the final manuscript. TT and ZW contributed equally to this work.
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
