Abstract
Objective
Evidence indicates that people with a high body mass index (BMI) tend to develop more severe forms of coronavirus disease 2019 (COVID-19). In this study, we aimed to determine the association between the duration of COVID-19 symptoms and variables such as BMI, age, presence of comorbidities, and smoking in non-hospitalized patients.
Methods
In this observational cross-sectional analytical study, we analyzed the data of patients with COVID-19 but without severe manifestations. We conducted descriptive statistics, non-parametric tests, and multivariate quasi-Poisson regression in the analysis. The quasi-Poisson regression model was configured with the duration of COVID-19 symptoms as the response variable, and BMI and the presence of comorbidities as the explanatory variables.
Results
Among 302 non-hospitalized patients, we found a significant difference in COVID-19 symptom duration between the overweight group and the group with normal weight. Multivariate quasi-Poisson regression analysis showed that BMI and the presence of comorbidities were associated with the duration of COVID-19 symptoms. On the contrary, sex, age, and smoking status were not related to COVID-19 symptom duration.
Conclusions
BMI and comorbidities were associated with the duration of COVID-19 symptoms in non-hospitalized patients.
Introduction
More than 2 years have passed since the start of the coronavirus disease 2019 (COVID-19) pandemic. COVID-19 is associated with considerable morbidity and mortality, mostly among patients with advanced age, male sex, and previous medical conditions. In most studies, the focus has been on severely ill patients. For instance, in a retrospective case series involving 1591 critically ill patients in the Lombardy region of Italy, mortality in the intensive care unit (ICU) was 26%. 1 A study using available body mass index (BMI) data of 329 hospitalized patients with confirmed COVID-19 in Amiens University Hospital in France found that obesity as well as overweight was associated with ICU admission, but overweight was not associated with death. 2
Among patients with COVID-19, the reported prevalence of obesity is 33% 3 and the prevalence of comorbidities is 40.80%. 4 Systematic reviews and meta-analyses3,5,6 have confirmed the association of increased BMI and obesity with the risks of hospitalization, ICU admission, and the need for invasive mechanical ventilation in patients with COVID-19. A higher prevalence of hypertension is indicated in severe cases of COVID-19 whereas hypertension, diabetes, and respiratory disease are more common in fatal cases. 4
Most past studies have been conducted among hospitalized patients with severe COVID-19, and studies among non-hospitalized patients with mild-to-moderate COVID-19 have mainly investigated patients’ clinical features.7,8 In the present study, we analyzed the data of non-hospitalized patients with COVID-19 who did not have severe manifestations to determine whether overweight and obesity, age, comorbidities, and smoking are associated with the duration of COVID-19 symptoms.
Methods
This was an observational cross-sectional analytical study. The participants were non-hospitalized patients with COVID-19. No patients had received any dose of COVID-19 vaccine. All participants had tested positive using both COVID-19 rapid antigen and reverse transcription polymerase chain reaction (RT-PCR) tests, as follows. Patients with COVID-19 symptoms were initially tested with a rapid antigen test, and those who tested negative were subsequently tested using RT-PCR. Patients were examined for pulmonary complications if they had positive results on either test. After a detailed examination at the health care center, patients were released to self-isolate at home if they did not satisfy the conditions for hospitalization. The prescribed therapy included vitamins (alfacalcidol and vitamin C for patients without kidney problems), antiviral therapy for patients with symptoms (Favipiravir tablet, 1600 mg every 12 hours on day 1 and then 600 mg every 12 hours for the next four days), and symptomatic therapy. Most patients had symptoms of cough, fever or chills, fatigue, muscle or body aches, and headache. Patients were instructed to measure their body temperature at home. After a minimum of 14 days from the day of diagnosis, if they were feeling well for at least 3 days and did not have an elevated body temperature, the patient presented to the health care center for a check-up. The number of days with a temperature of 37°C or above was recorded, as well as each patient’s age, weight, and height. Participants self-reported whether they smoked. Comorbidities were checked in the medical database and recorded. Patients with missing medical data were excluded from the study.
The variables considered were age (years), BMI (kg/m2), presence of comorbidities, and whether the patient smoked. The number of days with a body temperature above 37°C was used to measure the duration and severity of COVID-19 symptoms. This variable is a valid indicator because the most common symptom in mild-to-moderate cases of COVID-19 infection is fever, with 98% of people diagnosed with COVID-19 having a fever. 9
The study setting was Novi Sad Health Care Center. The duration of data collection was from 1 December 2020 to 31 January 2021. All participants provided informed oral consent to participate in this study. We deidentified all patient details, and the clinical data were kept confidential.
Statistical analysis
In the statistical analysis, we used the t-test, Mann–Whitney U-test, Kruskal–Wallis test, and multivariate quasi-Poisson regression. We analyzed the data using TIBCO Workbench, version 14 (TIBCO Data Science, Palo Alto, CA, USA), MedCalc version 18.2.1 (MedCalc Software, Ostend, Belgium), and R version 4.0.3 (The R Project for Statistical Computing, Vienna, Austria).
Results
A total of 302 participants were included in this study, 146 women and 156 men, with age range 18 to 76 years and average age (± standard deviation [SD]) 41.09 ± 11.95 years. The average (± SD) BMI for the total participants was 26.39 ± 4.42 kg/m2, with 24.9 ± 4.43 kg/m2 in the female group and 27.8 ± 3.94 kg/m2 in the male group. The number of days with fever ranged from 0 to 16, with an average (± SD) of 4.37 ± 3.19 days. Table 1 shows the characteristics of participants in the whole group and among men and women.
Participant characteristics.
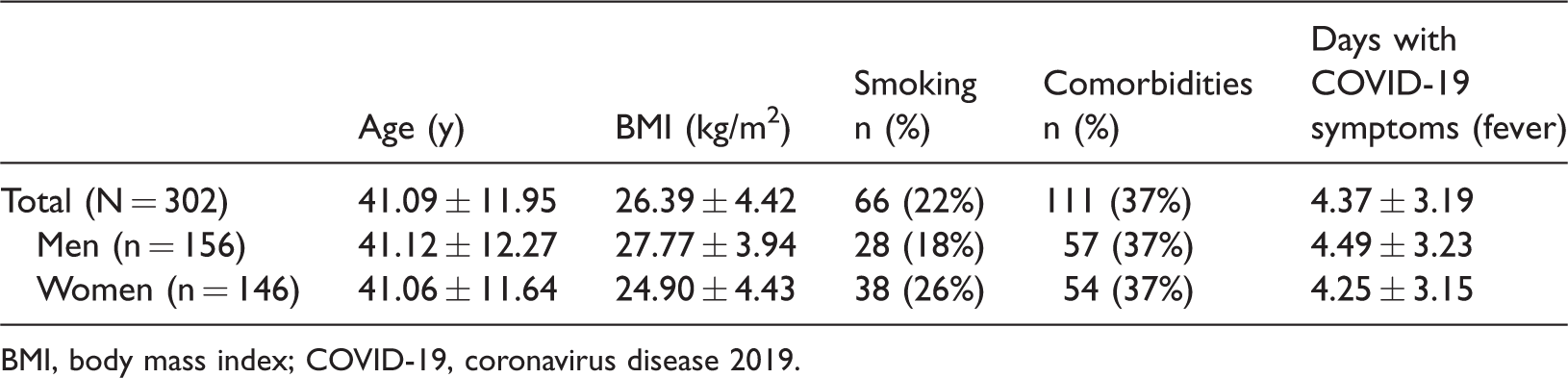
BMI, body mass index; COVID-19, coronavirus disease 2019.
The number (percentage) of participants with comorbidities was as follows: obesity (BMI ≥ 30 kg/m2), 61 (20%); hypertension, 54 (18%); endocrine and metabolic diseases, 35 (12%); cardiovascular diseases, 8 (3%); autoimmune diseases, 8 (3%); pulmonary diseases, 6 (2%); oncological diseases, 4 (1%); gastrointestinal diseases, 4 (1%); hematological diseases, 2 (<1%); kidney diseases, 2 (<1%); and neurological diseases, 2 (<1%). Some participants had more than one comorbidity. Most participants with comorbidities had been receiving appropriate, long-term therapy for their condition (data not shown).
Figure 1 depicts the distribution of COVID-19 symptom duration in the study group, and Table 2 presents the number of days with fever according to sex, age, BMI, comorbidities, and smoking, using the Mann–Whitney U and Kruskal–Wallis tests. The number (± SD) of days with COVID-19 (fever) was 4.25 ± 3.15 days among women and 4.49 ± 3.23 days among men. There was no significant difference in the number of days with COVID-19 symptoms between the male and female groups (Z = 0.616).

Number of days with COVID-19 symptoms and number of cases.
Number of days with COVID-19 symptoms stratified by risk factors.

*p < 0.05 , **p < 0.01.
BMI, body mass index; COVID-19, coronavirus disease 2019; SD, standard deviation; IQR, interquartile range.
Regarding comorbidities, the average number of days (± SD) with COVID-19 symptoms in the group without comorbidities was 4.06 ± 2.97 days; in the group with comorbidities, this was 4.91 ± 3.49 days. There was a significant difference in the number of days with COVID-19 symptoms between patients with comorbidities and those without comorbidities (Z = 1.979, p = 0.048).
There was no significant difference in the number of days with COVID-19 symptoms between the smoking and non-smoking groups (Z = 0.155). Regarding age, three groups were considered: 18 to 35 years, 36 to 50 years, and 51 to 76 years. The Kruskal–Wallis test showed no significant difference in the duration of COVID-19 symptoms among these groups (H = 3.70).
A total of 117 participants had BMI values <25 kg/m2 and 185 participants had BMI ≥ 25 kg/m2. There was a significant difference in the number of days with COVID-19 symptoms between these two groups (Z = −2.379, p = 0.02). In total, 241 participants had BMI values <30 kg/m2 and 61 had BMI ≥ 30 kg/m2. There was a significant difference in the number of days with COVID-19 symptoms between the groups with BMI ≥ 30 and BMI < 30 (Z = 2.849, p = 0.004).
Multivariate quasi-Poisson regression analysis showed that BMI and the presence of comorbidities were associated with the duration of COVID-19 symptoms (Table 3). On the contrary, sex, age, and smoking status were not related to the duration of COVID-19 symptoms. Using this model, we created graphs of the duration of COVID-19 symptoms in patients with comorbidities and without comorbidities, shown in Figure 2.
Results of quasi-Poisson regression estimating the risk of longer COVID-19 symptom duration with higher BMI and comorbidities.
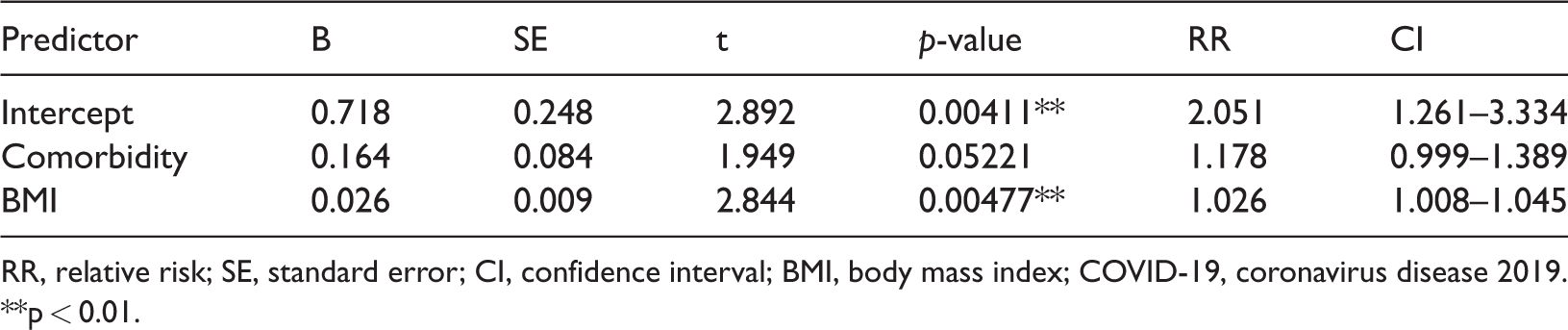
RR, relative risk; SE, standard error; CI, confidence interval; BMI, body mass index; COVID-19, coronavirus disease 2019.
**p < 0.01.

Model showing number of days with COVID-19 symptoms among participants with comorbidities (yellow) and without comorbidities (blue).
Discussion
Many studies have reported the association between BMI, comorbidities, and critical COVID-19 illness.1–3,10–14 Obesity has also been associated with disease severity, hospitalization, ICU admission, and death.12,13 In most studies, the whole cohort of patients with COVID-19 was considered, and obesity was found to be a risk factor of more severe COVID-19.12–14 Some studies investigating symptoms and the course of disease have involved patients with mild-to moderate COVID-19.7,8 The novelty of our study is that we investigated the association of the duration of COVID-19 symptoms with BMI and comorbidities among non-hospitalized patients.
The study population included 20% of patients who were obese. This differs from the data of a systematic review and meta-analysis, 6 which indicated that the prevalence of obesity among patients with COVID-19 was 33%. However, the patients in our study were not hospitalized whereas that previous study also considered hospitalized patients. 6
The reported duration of COVID-19 symptoms in patients with mild-to-moderate illness is 11.5 ± 5.7 days. 15 In our study, the duration of fever among patients with COVID-19 was 4.37 ± 3.19. The difference in findings might be because the indicator of the disease in our study was elevated body temperature; other symptoms of mild illness but that persist longer were not taken into account, such as loss of taste or smell.
More than 30 risk factors (comorbidities) are associated with a higher risk of severe COVID-19. 16 In our study, we found an association of higher BMI and the presence of comorbidities with the duration of COVID-19, similar to the findings of another study. 16
We analyzed the data of 302 non-hospitalized patients with COVID-19 who did not have severe manifestations and concluded that obesity and the presence of comorbidities are associated with the duration of COVID-19 symptoms. The clinical relevance of our study is that a person's weight alone can increase their risk for a longer duration of COVID-19 symptoms, even in mild to moderate cases.
Limitations of the study
A limitation of this study is that patients admitted to the hospital (the most complex cases) were not considered. The second limitation was that the duration of COVID-19 was determined according to the duration of elevated body temperature, which is the most common symptom in mild-to-moderate cases. 9 We chose to use the duration of fever as a measure of COVID-19 symptoms because it is a well-defined symptom that can be objectively measured. Another limitation is that patients self-measured their body temperature and self-reported these data. Finally, we did not conduct follow-up among the included patients.
Conclusion
In the present study, BMI and comorbidities were associated with the duration of COVID-19 symptoms in non-hospitalized patients. Further investigation is needed among vaccinated patients with mild symptoms.
Footnotes
Acknowledgements
We are very grateful to two anonymous reviewers whose comments helped us to considerably improve this article.
Author contributions
ZS and AT jointly conceived and designed the research, ZS conducted practical research, and AT analyzed the data. Both authors contributed to the drafting of the manuscript and reviewed and approved the final version.
Data availability statement
The corresponding authors will provide the anonymized data on reasonable request.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethical approval
This research study was conducted retrospectively using data obtained for clinical purposes. The study was approved by the Ethical Committee of Novi Sad Health Care Center (approval no. 21/1-1 of 21.1.2021).
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
