Abstract
Objective
Total hip arthroplasty (THA) involves postoperative risks, such as thigh pain, periprosthetic fractures, and stress yielding. Short, anatomical, metaphyseal-fitting, cementless femoral stems were developed to reduce these postoperative risks. This study aimed to examine the “MiniMAX” prosthesis, which is a new generation, short, anatomical femoral stem made by Medacta.
Methods
Patients underwent a low-dose computed tomography scan. Femoral anteversion was measured. We assessed the position and anteversion of the femoral component and compared them with the unoperated side. We also assessed the patients’ satisfaction and functional levels at 6 months postsurgery using the Harris Hip Score (HHS) and the Oxford Hip Score (OHS).
Results
Nineteen individuals were recruited in this study. We found no significant difference in femoral anteversion between the operated hip and the native hip. Using the HHS and OHS questionnaires, we found clinical improvement in the 6-month postoperative scores compared with the preoperative scores.
Discussion
The new-generation, short, anatomical femoral stem made by Medacta is successful in reproducing natural femoral anteversion, while also improving patients’ functioning and lifestyle. Future large-scale, prospective comparison trials are required to further investigate this topic.
Keywords
Introduction
Cemented and cementless total hip arthroplasty (THA) achieves good results.1–8 Nevertheless, thigh pain, periprosthetic fractures, and stress yielding are still potential postoperative risks.5–8 To reduce these risks, short, anatomical, metaphyseal-fitting, cementless femoral stems were developed. The absence of diaphyseal anchorage aims to achieve more proximal load transfer, reduce stress shielding and thigh pain, and preserve more diaphyseal bone for future revisions.9–18 When comparing short with conventional-length, cementless, anatomical femoral stems, the results are promising in achieving these goals.11,13,19
Current surgical recommendations regarding the positioning of the femoral component in THA are to restore the offset and the natural anteversion of the femur in normal femoral anatomy. 20 Dorr et al. 21 noted that the femoral stem position is predetermined by the femoral canal shape. However, little is known about the relationship between native anteversion of the unoperated femur compared with anteversion achieved in surgery.
There have been limited and contradicting data on successful reconstruction of natural femoral anteversion in THA surgery.22–24 Therefore, this study aimed to examine the “MiniMAX” prosthesis (Medacta International, Castel San Pietro, Switzerland), which is a new-generation, short, anatomical femoral stem. 25 We also investigated patients’ satisfaction 6 months postsurgery using the Harris Hip Score (HHS) and the Oxford Hip Score (OHS) to assess function, quality of life, and pain.
Patients and methods
The reporting of this study conforms to the STROBE guidelines. 26 The inclusion criteria were patients aged from 18 to 90 years who underwent elective THA from 2018 to 2020 with the MiniMAX short, anatomical femoral stem. All patients were operated on by the same joint replacement specialist using the antero-lateral approach. Exclusion criteria were patients who underwent THA in the past on the contralateral side, revision surgeries, disruption of the posteromedial cortex or lateral cortex of the femur, and patients who were not able to or capable of providing consent. Ethical approval was obtained from the Institutional Review Board of Emek Medical Center, Afula, Israel (25.6.2019; approval number: 0100-19-EMC; NIH No. NCT04243980). Written informed consent was obtained from the patient for their anonymized information to be published in this article.
The MiniMAX stem is anatomically designed, cementless, collarless, and made of titanium-niobium alloy (Ti-6Al-7Nb). This stem is coated with hydroxyapatite (Ra 80 μm) all along the shaft and there is titanium coating (Ra 300 μm) in the proximal two thirds of the shaft. The neck has a 127° neck–shaft angle with an anteversion of 9° (Figures 1, 2). MiniMAX stems can be classified as type 6 according to Khanuja et al. 27

Photograph of the MiniMAX stem.

(a, b) Postoperative X-ray of the prosthesis.
After signing consent forms, the patients underwent a low-dose computed tomography (CT) scan from the level of the acetabular roof until the level of the lesser trochanter, with a total of 10 cm in length. A low-dose CT scan was also performed at the level of the femoral condyles. The CT scans were conducted during one of the routine follow-up visits.
Femoral anteversion was measured by one fellowship-trained musculoskeletal radiologist specialist. The neck horizontal angle and the condyle horizontal angle were measured to calculate the femoral anteversion (Figures 3–5). In cases where the femoral neck and condyle were rotated in opposite directions, the femoral anteversion was the sum of both angles. When both angles were rotated in the same direction, the femoral anteversion was the difference between both angles.
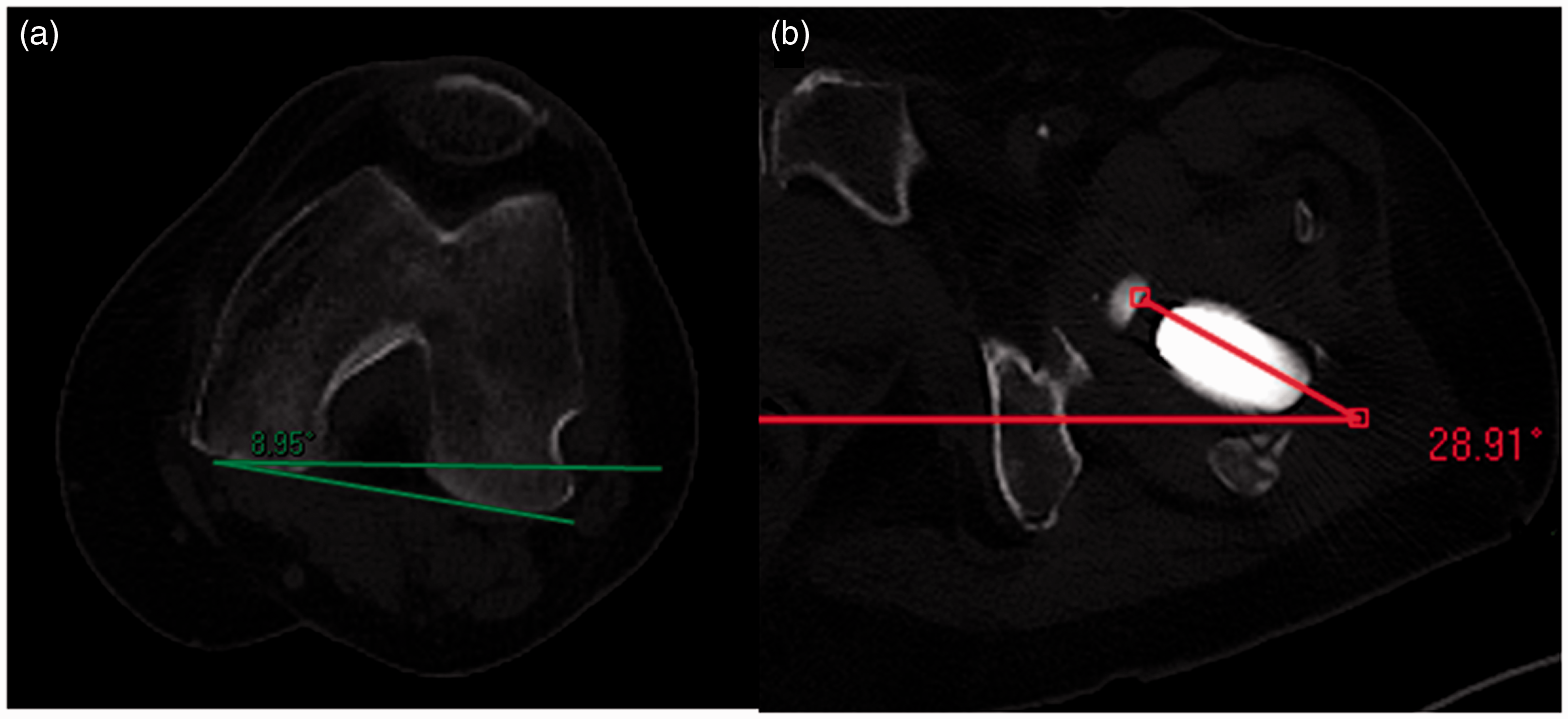
Measurement of the left neck–condyle angle. (a) Condyle horizontal angle. The condyle is rotated laterally. (b) Neck horizontal angle. The neck is rotated medially. Because the neck and condyle are rotated in the opposite directions, the neck–condyle angle (femoral anteversion) is the sum of both angles (9 + 29 = 380).
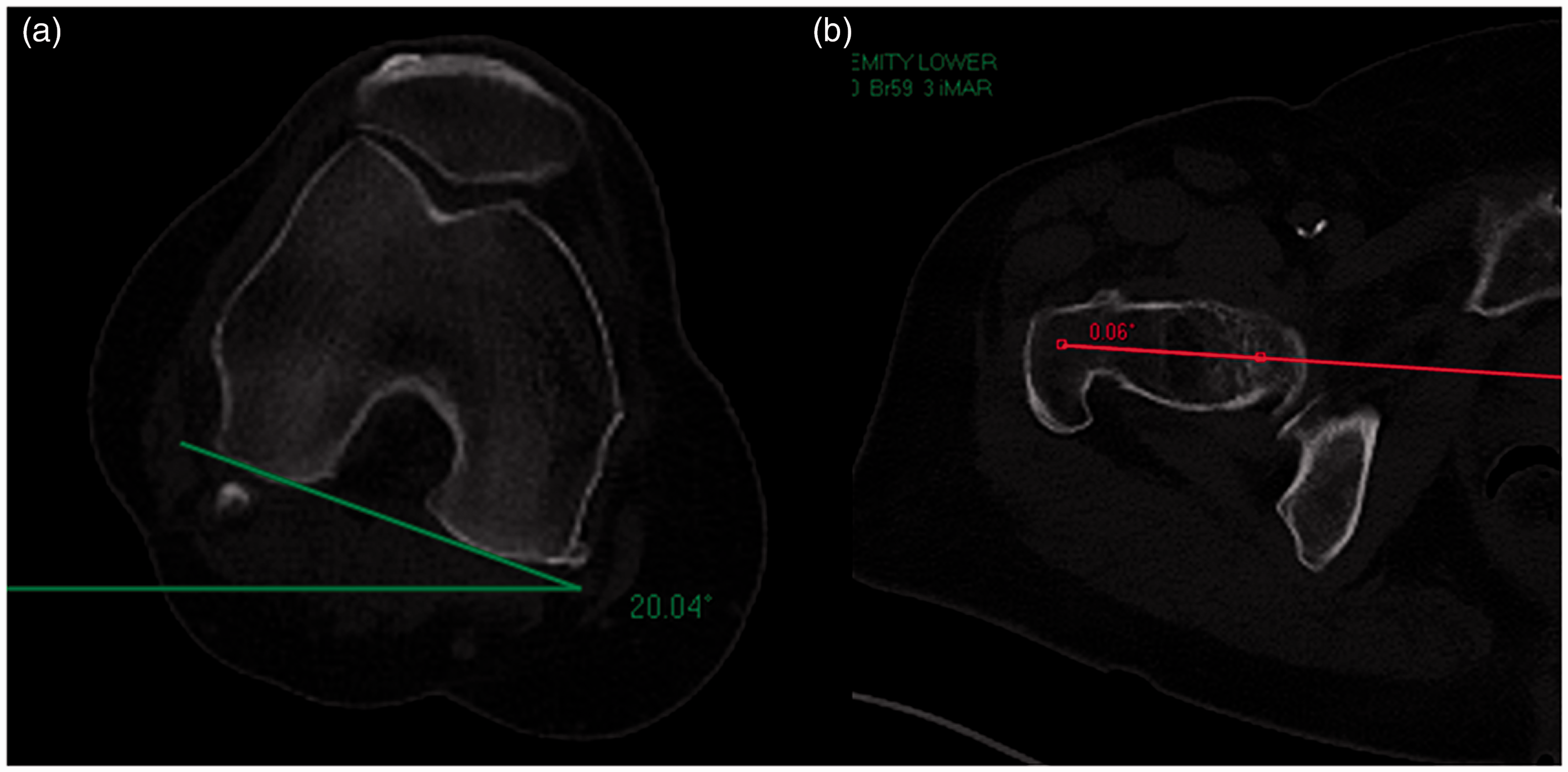
Measurement of the right neck–condyle angle. (a) Condyle horizontal angle and (B) neck horizontal angle. Because the neck horizontal angle is “0”, the neck–condyle angle (femoral anteversion) is 200.

Measurement of the left neck–condyle angle. (a) Condyle horizontal angle. The condyle is rotated medially. (b) Neck horizontal angle. The neck is rotated medially. Because the neck and condyle are rotated in the same direction, the neck–condyle angle (femoral anteversion) is the difference between both angles (21 − 3 = 180).
In addition to the low-dose CT scans, patients were asked to fill out two questionnaires, which were the Oxford Hip Score (OHS) and the Harris Hip Score (HHS). The OHS is a joint-specific, patient-reported measurement tool designed to assess disability in patients undergoing THA. 28 The OHS was originally developed in 1996 29 and updated in 2007 30 The most current scoring system is based on 12 questions regarding pain and function over the past 4 weeks. Forty-eight is the maximum score on the questionnaire, and it represents the highest level of functioning along with the least amount of pain, while zero represents the worst possible score. 30 The HHS is a questionnaire filled out by the surgeon and patient together. The HSS uses a scoring system where 100 represents the highest functioning hip joint, and zero indicates the lowest functioning hip joint. We used these questionnaires to measure the patients’ satisfaction regarding their function, pain, and quality of life. We compared preoperative scores with the 6-month postoperative scores.
Categorical variables are shown as percentages, and continuous variables are represented by the standard distribution indices. Differences in continuous variables were tested using the paired t test or the Wilcoxon signed rank test. McNemar's test was performed to analyze categorical variables. All data were analyzed using SAS 9.4 software (SAS, Cary, NC, USA). Statistical significance was accepted to be P < 0.05.
Results
Between 2018 and 2020, 19 individuals were recruited into our prospective study. There were 9 men and 10 women aged from 27 to 83 years, with a mean (standard deviation) age of 59.2 ± 17.5 years. All patients except for five suffered from primary osteoarthritis. The remaining five suffered from avascular necrosis of the femoral head.
With regard to radiological parameters, we found that the acetabular inclination angle was significantly lower (P = 0.003) and the neck horizontal angle was significantly higher (P = 0.004) in the operated side than in the non-operated side. These differences were caused with intent by the surgeon based on his preference when placing the acetabular component. We found no significant difference in femoral anteversion, which represents successful reconstruction of femoral anatomy after THA using a short anatomical femoral stem, between the operated and non-operated sides (Table 1, Figure 6).
Comparison of radiographic parameters between the non-operated side and the operated side.

Data are mean ± standard deviation [median].

Mean femoral anteversion on the non-operated side compared with the operated side. There was a difference of 1.3°.
When we compared the mean femoral anteversion between the operated and unoperated sides, we found a 1.3° difference. As stated above, this difference was not significant. The mean neck–shaft angle on the unoperated side was 128.79° ± 4.79° compared with 130.99° ± 5.9° on the operated side, with no significant difference between the sides.
When we analyzed the HHS and OHS questionnaires (Table 2), we found significant clinical improvement in the 6-month postoperative scores compared with the preoperative scores (both P < 0.001). At the 6-month follow-up, we did not find any complications.
Comparison of OHS and HHS scores between preoperatively and 6 months postoperatively.

Data are mean ± standard deviation [median].
OHS, Oxford Hip Score; HHS, Harris Hip Score.
Discussion
Short versus conventional-length, cementless, anatomical femoral stems show promising results.11,13,19 With regard to the preservation of bone mass density, short femoral stems appear to be superior to conventional-length stems.31,32
One important aspect involved in successful THA surgery is component positioning. Malposition is recognized as a major determinant of instability in an artificial hip, and it may lead to bony and prosthetic impingement, which precedes the majority of dislocations after THA. 20 Anisha et al. performed computer simulations in a wide range of activities in cadavers after THA. 20 They concluded that in the absence of overt femoral or acetabular deformity, prosthetic impingement is minimized by the restoration of femoral offset and natural anteversion.
There are limited and contradicting data regarding successful restoration of natural femoral anteversion. A study by Emerson et al. reported that a canal-filling, press-fit, long femoral component showed a wide variation of postoperative component anteversion with most stems placed in increased anteversion compared with the anatomical head. 22 They offered a possible explanation for their findings as follows. Because the shape of the femoral canal determines the anteversion of the stem in the setting of a canal-filling stem, and the canal is more anteverted at the level of the lower neck and intertrochanteric region compared with the area of the head, postoperative femoral anteversion is increased. The authors concluded that the surgical technique may need to be adjusted for this femoral anteversion if it causes intraoperative impingement or instability. Similar discrepancies were found in a study by Reikeras et al. who used a straight, press-fit, long femoral stem, where the intraoperative estimation of femoral and acetabular anteversion in many cases was inadequate in relation to the intended range of 10° to 30° of anteversion. 23 However, Sue et al. observed the positioning of the femoral stem and its correlation with true anteversion of the contralateral side using postoperative CT scanning. 24 They showed that anteversion was compatible with true femoral anteversion.
In our study, we investigated postoperative femoral anteversion using a new-generation, short, anatomical femoral stem. To the best of our knowledge, this is the first study to examine this topic using a short, anatomical femoral stem. Previous studies used standard-length femoral stems.21–24 When we compared the operated hip with the native hip, we found an approximately 1° difference between the sides. Therefore, we succeeded in reproducing natural femoral anteversion.
Similar to many other studies on THA surgery,1–8 we assessed the patients’ satisfaction using OHS and HHS scores. We found a significant improvement in both scores postoperatively. The association between successful restoration of natural femoral anteversion as an isolated parameter and its effect on patients’ satisfaction has yet to be studied. Combined anteversion and optimal positioning of the acetabular and femoral components has been studied by many authors, and the stem and cup should provide a mean combined anteversion of approximately 37.5° (range: 25°–50°) to avoid impingement and/or dislocation.21,33,34
As mentioned above, the surgical technique may need to be adjusted when natural femoral anteversion is not restored owing to intraoperative impingement or instability. 22 Our study suggests that there is no need for intraoperative adjustments in the surgical technique when inserting the MiniMAX short femoral stem.
This study has certain limitations. First, our study population was relatively small. Second, although all the data were collected prospectively, the study was not randomized, and there was no control group in which a different component or different surgical technique was used to compare outcomes.
In conclusion, this is the first study to determine the restoration of natural femoral anteversion using a short anatomical femoral stem. The new-generation, short, anatomical MiniMAX femoral stem was able to reproduce natural femoral anteversion and succeed in improving the patients’ functional levels and lifestyle. Future large-scale, prospective, comparison trials are required to further investigate this topic.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605221091500 - Supplemental material for Successful reconstruction of natural femoral anteversion using a short femoral stem in total hip arthroplasty surgery
Supplemental material, sj-pdf-1-imr-10.1177_03000605221091500 for Successful reconstruction of natural femoral anteversion using a short femoral stem in total hip arthroplasty surgery by Raja Hakim, Aryeh Weinstein, Dan Dabby, Nimrod Rozen, Nogah Shabshin and Guy Rubin in Journal of International Medical Research
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
