Abstract
We report the first case of a woman with Behcet's disease (BD) with multiple hand ulcers secondary to coninfection by
Introduction
BD is a systemic vascular inflammatory disease associated with a high incidence of skin lesions. Patients with BD take prednisone and immunosuppressants for long durations and are thus more vulnerable to complex infections compared with the general population. Because of the complex anatomical structure of the hand, suppurative infections can easily spread and lead to complex severe soft tissue infection. The causative pathogens of such infections are diverse.
Case report
This study was approved by the Ethics Committee of Changzheng Hospital, Naval Medical University, China. Written informed consent was obtained from the patient for publication of this case report and any accompanying images. The reporting of this study conforms to CARE guidelines. 13
A 72-year-old woman was admitted to our hospital on 14 February 2017 complaining of oral cavities and multiple skin ulcers (6 months) as well as swelling and pain in both hands (1 week). The patient had previously experienced shoulder pain with no apparent cause in August 2016 and multiple ulcers in both hands with pain and exudation in October 2016. She was diagnosed with herpes zoster skin infection at a local hospital and received antibiotics (details unknown), but her condition did not improve. The areas of ulceration on both hands gradually expanded, and ulcerations appeared successively on the trunk and oral cavity mucosa. She visited the local hospital again in December 2016 and was diagnosed with BD. She was treated with prednisone 10 mg
The patient had a history of left eye vision loss resulting from retinal detachment in 2002. Five years prior to admission to our hospital, she underwent cholecystectomy. She had a history of hypertension and took amlodipine irregularly. She was allergic to penicillin and cephalosporin and had no self-reported history of diabetes, tuberculosis, or hepatitis.
On admission, the patient had a body temperature of 36.5°C, a blood pressure of 120/75 mmHg, a pulse of 72 beats per minute, and a respiratory rate of 16 breaths per minute. Physical examination revealed mild anemia. Scattered ulcers (approximately 1 × 1 cm) were observed on the trunk, hands, and feet and had a foul odor with wrapping (Figure 1). Both hands were significantly swollen and showed elevated skin temperature, positive needle puncture response, and limited finger movement.

On admission, both of the patient’s hands were swollen, her skin temperature was elevated, several ulcers approximately 1 × 1 cm in size and deep wounds were observed, and yellow pus exuded from the wounds.
Initial laboratory results showed low hemoglobin levels and elevated neutrophil count, C-reactive protein (CRP) level, erythrocyte sedimentation rate (ESR), and D-dimer level. In addition, alterations in hepatic and immunological function measures were observed: levels of pro-brain natriuretic peptide and ferritin were elevated, while CD3+CD4+ T-lymphocyte counts, CD3+CD8+ T-lymphocyte counts, total protein level, and albumin level were all decreased (Table 1). Additional laboratory test results were normal. Because the infection had caused severe tissue destruction and decreased hand function, we performed emergency surgery on the patient’s infected hands under brachial plexus anesthesia. The goal of surgery was to incise, drain, and debride the septic infection in both hands. During the operation, the encapsulated pus cavity was opened. The traumatic wound of the left hand and the ulnar side of the forearm wound were completely subcutaneously connected to the skin. After thorough cleaning of the wrapped pus moss and surrounding inflammatory granulation tissue, the tendons of each finger extensor muscle on the back of the hand were observed to be severely compressed, without any elasticity or toughness, and showed necrotizing fasciitis-like changes (Figure 2). The inflammatory fibers were completely removed. Specimens of ulcerated tissue and the necrotic vascular wall were taken for pathological and microbiological examinations. The wound was cleaned with normal saline, hydrogen peroxide and chlorhexidine, then dressed with sterile clean excipients.
Laboratory test results of the patient on admission.
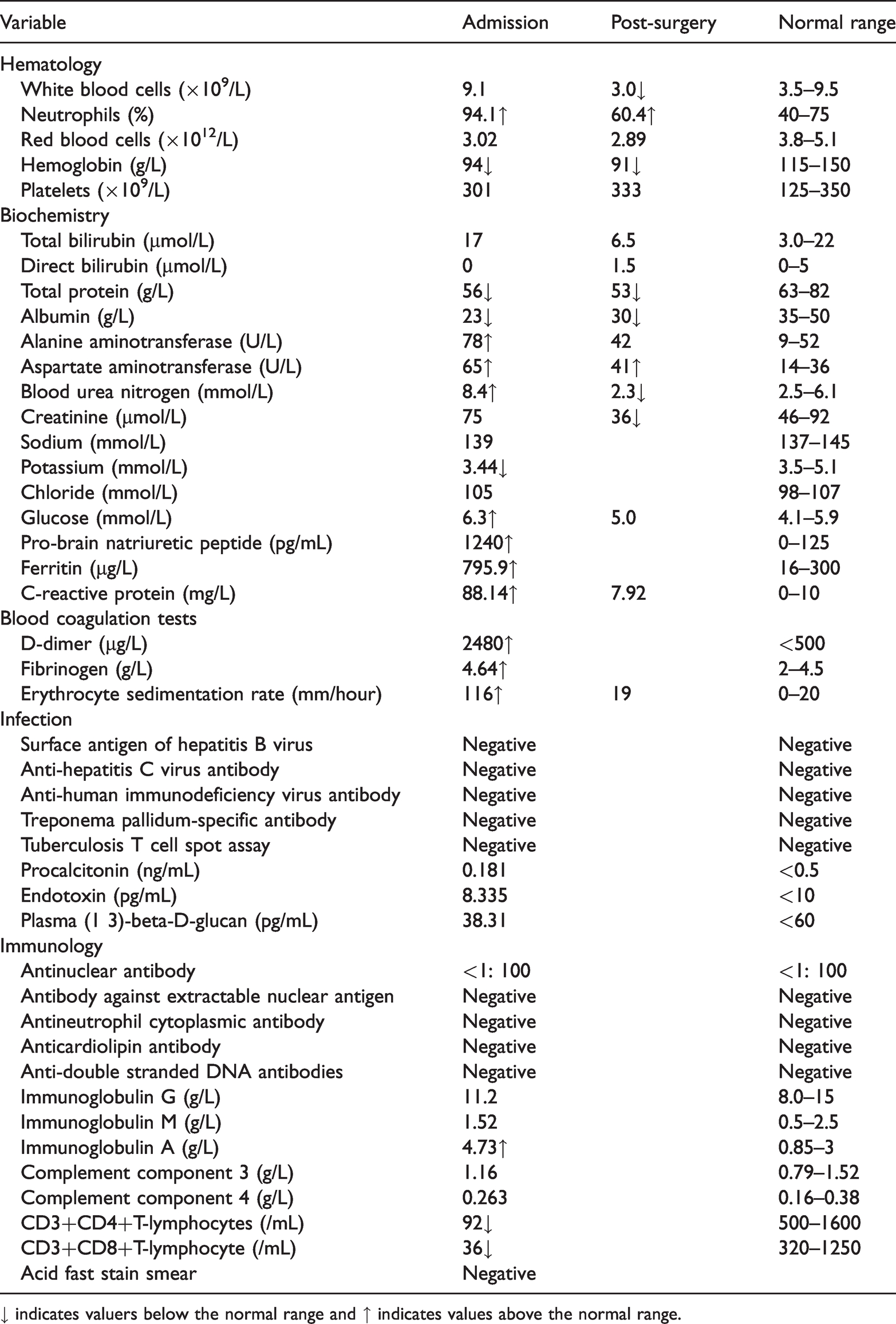
↓ indicates valuers below the normal range and ↑ indicates values above the normal range.

After surgical debridement, the tendons of the extensor digitorum of the dorsum of the hand were severely compressed without any elasticity and toughness and showed necrotic fasciitis-like changes.
Gram-stained smears of wound pus revealed the presence of Gram-positive cocci and Gram-negative bacilli. Within 24 hours, bacterial growth was observed in blood agar cultured at 35°C with 5% CO2. Blood agar cultures were positive for

Colony morphology of

Microscopic examination of bacterial colonies following Gram staining revealed long and slender Gram-negative bacilli (original magnification ×100).
Discussion
BD is a chronic systemic vascular inflammatory disease associated with a high incidence of skin lesions (up to 80%) and a variety of manifestations, including erythema nodosum, pyoderma, papules, and acne-like rash.
14
The inflammatory manifestations of BD can also mimic infection, making diagnosis and treatment challenging. In the case described here, pathological analysis revealed vasculitis and suppurative infection. Moreover, an increase in CRP indicated that the patient had an infection that could not be explained by BD activity. We speculate that our patient had taken glucocorticoids and immunosuppressive medications for a long duration, and after ulceration destroyed the skin’s immune barrier,
Mixed infection with
In summary, we report the case of a rare coinfection by
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211072783 - Supplemental material for Secondary hand infection with Eikenella corrodens and Staphylococcus aureus in a patient with Behcet's disease: a case report
Supplemental material, sj-pdf-1-imr-10.1177_03000605211072783 for Secondary hand infection with
Footnotes
Acknowledgements
We thank Dr. Xin Wu for advice on patient treatment and Dr. Hu Zhao for experimental guidance. We are grateful to Dr. Zhou Yi for help with language editing.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on request.
Authors’ contributions
YTL and JYZ collected the data and wrote the manuscript. HQH, QH, XFC, and ZJW performed the microbiological analysis. LZ critically reviewed the manuscript and supervised the research. All authors read and approved the submitted manuscript.
Ethics approval and consent to participate
This study was approved by the Ethics Committee of Changzheng Hospital, Naval Medical University, China.
Consent for publication
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent was available for review by the editor of this journal.
The reporting of this study conformed to CARE guidelines. 13
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for publication of this work was provided by the National Natural Science Foundation of China (82072371), the Leading Talent Project of Shanghai Huangpu District (2020-1-28), and the Special Foundation for National Science and Technology Basic Research Program of China (2019FY101200).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
