Abstract
Objective
Research is limited regarding biochemical markers of bone metabolism among children with cow’s milk protein allergy (CMPA). We aimed to determine differences in vitamin D and bone metabolism markers between infants with CMPA and healthy infants and explore relationships between these in a cross-sectional study.
Methods
In total, we included 41 children diagnosed with CMPA and under systematic medical and nutritional care at our center, and 50 healthy children as a control group. We reviewed demographic and clinical characteristics and measured serum biomarkers.
Results
We found that serum 25-hydroxyvitamin D (25(OH)D) levels among infants in the CMPA group were significantly lower than those in the control group, and levels of bone-specific alkaline phosphatase (BALP), serum phosphorus, and serum calcitonin were reduced. Pearson correlation analysis showed that serum 25(OH)D concentrations in the CMPA group were negatively correlated with parathyroid hormone but not significantly correlated with calcitonin and BALP. Logistic regression showed that CMPA was a risk factor for vitamin D deficiency.
Conclusions
Our study indicated that CMPA was associated with disturbances in bone metabolism. Levels of vitamin D in children with CMPA were lower than those in healthy children. CMPA was a risk factor for vitamin D deficiency.
Keywords
Introduction
Food protein allergy, which is an immune response triggered by food proteins, is common among children in many countries. Food allergy affects approximately 10% of infants and 5% of young children. The most common food allergens responsible for allergic diseases are cow's milk protein and egg protein. The incidence of cow’s milk protein allergy (CMPA) worldwide has reached 4.9%, and it is showing an increasing incidence. 1 CMPA not only affects the health of infants and young children but it also causes a heavy emotional and economic burden on families and society. The only treatment comprises elimination of cow’s milk protein from the diet and introduction of extensively hydrolyzed milk protein as a nutritional supplement. 2 The taste of this extensively hydrolyzed formula is very disagreeable to most children, which may increase their risk of malnutrition. Appropriate and adequate nutritional support is crucial for the growth and development of children with CMPA. 3 If children with CMPA do not receive adequate nutritional support, they are more likely to have reduced bone density and vitamin D deficiency, which can lead to rickets. 4 In the past, bone mineral density measurements were used to assess the level of bone metabolism in the clinical setting. However, this does not reflect dynamic changes in bone tissue in real-time. For the assessment of bone health-related indicators, dual-energy X-ray absorption is the gold standard for determining bone mineral density according to recommendations of the World Health Organization. 5 However, widespread controversy remains related to the accuracy and reference standards for using dual-energy X-ray absorption in children, where measurements only represent local changes in bone tissue. 6 Bone tissue in children is undergoing dynamic developmental processes, and misdiagnosis is common when measuring bone mineral density in the clinical setting. Investigation is needed into the characteristics and interactions among biochemical indicators of bone metabolism in children with CMPA to improve evaluation of bone metabolism status in children, reduce the incidence of metabolic bone disease, and more accurately monitor the effect of treatment. Many studies have shown that vitamin D is closely related to the occurrence and development of allergic diseases 7 ; however, the conclusions of these studies have not been consistent. Few studies have focused on the biochemical markers of bone metabolism in children with CMPA. 8 In this study, we aimed to determine the changes in bone metabolism indicators and examine correlations between vitamin D levels and bone metabolism clinical indicators among children with CMPA. Our study results can provide theoretical information on bone health status and dietary nutritional support for children with CMPA.
Methods
Study participants
This study included children who were treated and diagnosed at the Children’s Health Department of Guangdong Women and Children Hospital from January 2019 to December 2020. We collected clinical data of participants and measured serum vitamin D and bone metabolism-related levels. We enrolled children who received a definitive diagnosis of CMPA with an oral food challenge (OFC) in the study group.9,10
We recruited healthy children without CMPA as a control group during the same period. According to dietary supplement recommendations of the 2008 American Academy of Pediatrics, we assumed that all children had received 400 IU of vitamin D daily from day 14 after birth.
The inclusion criteria of this study were as follows: children younger than 24 months of age; family members involved in the study were fully informed and voluntarily agreed with their child’s participation; met the diagnostic criteria of CMPA guidelines; all children in the observation group were confirmed to have CMPA using an OFC.
The exclusion criteria were: children with major organ dysfunction (including congenital heart disease, acute or chronic lung disease, acute or chronic liver disease, acute or chronic kidney disease, congenital genetic metabolic disease, immune dysfunction, and delayed development of the nervous system); children with systemic infectious diseases and abnormal bone metabolism diseases such as calcium, phosphorus, and vitamin D deficiency; children suspected of having CMPA and undergoing dietary elimination; and children diagnosed with CMPA or food allergy.
This study and its protocols were approved by the Ethics Committee of Maternal and Child Hospital of Guangdong Province (approval no. 202001010) and carried out in accordance with the principles of the Declaration of Helsinki. We obtained written informed consent from each participant’s parent/legal guardian. The hospital approved this research. This study followed the relevant EQUATOR Network guidelines. 11
Diagnosis of CMPA
The diagnosis of CMPA was confirmed using an OFC as follows: infants suspected of CMPA were fed formula milk or mixed formula, supplied as an amino acid formula powder, for 4 weeks. CMPA was ruled out if there was no improvement in symptoms. If symptoms improved, we changed to regular formula for 1 week and observed the infant for any clinical manifestations. If allergic symptoms returned, the infant was diagnosed as having CMPA. In breastfed infants, mothers were encouraged to continue breastfeeding while avoiding milk and dairy products in their diet for 4 weeks. If allergic symptoms showed no improvement, CMPA was ruled out. If allergic symptoms disappeared, milk and dairy products were reintroduced to the mother's diet. If allergic symptoms recurred, CMPA was diagnosed.
Data collection
We collected general characteristics of infants in the observation and control groups, including age, sex, delivery mode, premature/full-term infant, and feeding patterns. Family history of allergic diseases (including allergic rhinitis, asthma, atopic dermatitis, or specific food allergies), smoking among family members; allergic symptoms and signs, and the child’s growth and development status. Venous blood specimens were collected during outpatient visits. Samples were collected in heparin for subsequent centrifugation and stored at −80°C, then subsequently thawed immediately before serum biomarker and hormonal analyses. Serum 25-hydroxyvitamin D (25(OH)D) levels were determined with enzyme-linked immunosorbent assay (Abbott Laboratories, Chicago, IL, USA) with the original reagents. Levels of bone-specific alkaline phosphatase (BALP), serum calcium, and serum phosphorus were determined using alkaline phosphatase chemiluminescence detected with a Beckman Coulter AU5800 (Brea, CA, USA), according to the manufacturer’s instructions. Levels of parathyroid hormone (PTH) and calcitonin (CT) were detected using an alkaline phosphatase chemiluminescence kit (Siemens AG, Munich, Germany) with the original reagent kit.
Vitamin D was considered deficient with serum 25(OH)D levels below 50 nmol/L (20 ng/mL), vitamin D insufficiency was defined as 25(OH)D of 52.5 to 72.5 nmol/L (21–29 ng/mL), and vitamin D sufficiency was defined as 25(OH)D levels above 75 nmol/L (30 ng/mL). 12
Statistical analysis
Clinical data were collected and managed using Microsoft Excel 2010. IBM SPSS version 23.0 (IBM Corp., Armonk, NY, USA) was used for data analysis. The measurement data are described as median (min–max) and mean ± standard deviation (SD) or number and percentage according to the type of variable. Variables with a normal distribution (P > 0.05) and the two-sample t-test for two independent trials were used to compare quantitative variables between children with CMPA and healthy controls. Count data are presented as number and percentage, and the χ2 test was used for analysis. The independent samples t-test was used to compare measurement data between the two groups, and multiple linear regression was used to evaluate the correlation between parameters. P < 0.05 indicated statistical significance.
Results
Clinical parameters
We enrolled 41 children who had received a definitive diagnosis of CMPA in the study group. There were 24 male and 17 female children in the CMPA group. Among them, 13 children (31.7%) were under the age of 6 months, 10 (24.4%) were 7 to 12 months old, 9 (22%) were 13 to 18 months old, and 9 (22%) children were 19 to 24 months of age. No significant differences were identified for sex, age, gestational age, father’s history of allergies, family history of smoking, or vitamin D supplementation during pregnancy between the CMPA group and control group. There were significant differences in delivery mode and mother’s history of allergies between the two groups (P < 0.05), as shown in Table 1.
General comparison of infants between the CMPA group and control group.

Comparison of bone metabolism-related levels
The overall range of serum 25(OH)D levels in the CMPA group was 24.4 to 133.2 nmol/L (mean ± SD: 83.25 ± 26.65 nmol/L). In the CMPA group, BALP levels were 42.13 to 95.18 μg/L (63.94 ± 16.25 μg/L), serum calcium levels were 2.39 to 2.71 nmol/L (2.56 ± 0.08 nmol/L), serum phosphorus levels were 1.32 to 1.98 nmol/L (1.73 ± 0.17 nmol/L), PTH levels were 0.37 to 5.64 pmol/L (2.01 ± 1.13 pmol/L), and levels of CT were 2.0 to 10.8 pg/mL (4.05 ± 2.32 pg/mL). Levels of 25(OH)D in the CMPA group were significantly lower than those in the control group. Compared with the control group, levels of BALP, serum phosphorus, and CT were decreased to different degrees, with significant differences. PTH levels were significantly higher in the CMPA group than in the healthy control group (P = 0.001). No significant difference was found in serum calcium levels between the two groups (Table 2).
Vitamin D and bone markers in children with CMPA and healthy controls.

Data presented as mean ± standard deviation.
CMPA, cow’s milk protein allergy; PTH, parathyroid hormone; CT, calcitonin; BALP, bone-specific alkaline phosphatase; 25(OH)D, serum 25-hydroxyvitamin D.
The average level of 25(OH)D in children with CMPA was 83.25 ± 26.65 nmol/L whereas that in healthy children was 110.14 ± 22.04 nmol/L (P < 0.001). The frequencies of vitamin D deficiency in the two groups are shown in Figure 1. This result showed that the incidence of vitamin D deficiency and insufficiency in children with CMPA was much higher than that in healthy children with the same amount of vitamin D supplementation.

Percentage of vitamin D deficiency among infants in the CMPA group versus healthy controls
Correlation of vitamin D status and bone metabolism indicators in the CMPA group
Pearson correlation analysis was used to evaluate the correlation between serum 25(OH)D and PTH, CT, and BALP in the CMPA group. The results showed a negative correlation between 25(OH)D and PTH (r = −0.462, P = 0.002). However, no significant correlation was found between serum 25(OH)D levels and CT or BALP (r = 0.20 6, r = 0.032, respectively) (Table 3).
Correlation between vitamin D deficiency and bone metabolic markers in the CMPA group.
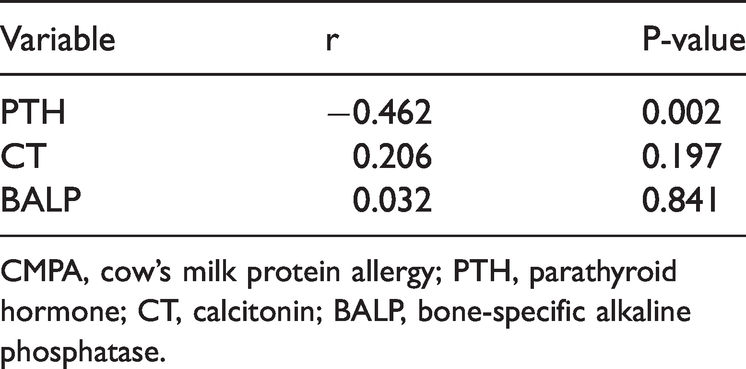
CMPA, cow’s milk protein allergy; PTH, parathyroid hormone; CT, calcitonin; BALP, bone-specific alkaline phosphatase.
Logistic regression analysis of infant vitamin D deficiency
Multivariate logistic regression analysis was conducted using 25(OH)D deficiency as the dependent variable and gestational age, months of age, delivery mode, feeding mode, CMPA allergy, and maternal vitamin D supplementation in late pregnancy as independent variables. The results showed that age (odds ratio [OR] = 2.276, 95% confidence interval [CI]: 1.119–4.627, P = 0.023) and milk protein allergy (OR = 14.065, 95% CI: 2.399–82.444, P = 0.003) were risk factors for 25(OH)D deficiency in infants.
Discussion
In recent decades, many studies have concluded that the physical growth parameters of food protein allergy in children are usually lower than the mean level, especially in children with CMPA. 11 Flammarion et al. found that when intakes of each nutrient component in allergic children were compared with the recommended nutrient intakes, the intakes of nutritional components such as dairy products, meat, fruits, vegetables, and grains in most children with food allergies were much lower than the recommended standard. In particular, calcium, vitamin D, vitamin E, and zinc intakes were only 67% of the recommended values. 13 Cow’s milk protein is an important source of nutrients for the growth and development of young infants. Long-term elimination and replacement therapy with an extensively hydrolyzed formula may affect the growth and development of young children. 14 Decreased peak bone mass is an important risk factor for osteoporosis and infants and toddlers with food protein allergies are more likely to have bone metabolic disorders and an impaired process of bone growth and development.15,16
Bone metabolism indicators are usually derived from hormones, enzymes, and metabolites secreted by osteoblasts and osteoclasts, including calcium and phosphorus metabolism regulators, bone conversion markers, hormones, and cytokines. The regulation and maintenance of calcium and phosphorus metabolism mainly involves the comprehensive regulation of PTH, vitamin D3, and CT. BALP is a marker of bone formation and is often used in clinical settings. The detection of BALP is specific, but there is still cross-reaction between 20% of bone BALP and liver enzymes, which requires comprehensive judgment in clinical practice. The mechanism of these bone metabolism indexes warrants further exploration and cannot be explained by a single factor; however, a combination of factors may be present. A French multicenter cross-sectional study among 1674 infants who were suspected of CMPA concluded that there was a higher incidence of atopic diseases among first-grade relatives of infants with CMPA. There was a stronger positive association with having two or more allergic family members, with their offspring being more likely to have food allergic diseases, 17 particularly a maternal history of allergic disease. 18 In addition to genetic susceptibility, lifestyle factors are closely linked with food allergy. Certain factors affect microflora colonization on the skin and mucous membranes, including cesarean delivery and use of antibiotics. It is reported that babies born via cesarean delivery have an increased risk of food allergies compared with those delivered naturally.19,20 The results of our study were consistent with these findings.
Vitamin D is an important nutrient for bone growth and development, which can increase the absorption of calcium and phosphorus in the mucosa of the small intestine and kidney and can downregulate the level of PTH, increase bone mineral density, and improve bone strength and function. 21 However, there is little evidence regarding whether high doses of vitamin D can adversely affect bone formation. 22 Further research is needed to confirm this. In recent decades, understanding of the role of vitamin D in regulating the immune system has improved dramatically. Components of the adaptive immune system, such as T cells, B cells, macrophages, and dendritic cells, all express vitamin D receptors and all respond to vitamin D. 23 Many studies have shown that vitamin D deficiency is closely related to the occurrence of infectious, autoimmune, and allergic diseases.24,25 The results of our study confirmed that under the premise of the same amount of vitamin D supplementation after birth, the vitamin D level of infants in the CMPA group was significantly lower than that of healthy children whereas the deficiency rate of vitamin D was significantly increased, and CMPA is a risk factor for vitamin D deficiency. Recent studies have shown that vitamin D appears to maintain the integrity of the mucosal barrier and reduce permeability of the intestinal mucosal, protecting the intestinal immune system from exposure to food allergens. 26 We consider that vitamin D deficiency may lead to intestinal mucosa damage, allowing allergenic food protein to enter the immune system through the intestine, thereby increasing the Th2 allergic immune response. A number of factors can affect vitamin D levels, such as dietary supplements, outdoor activities, skin color, gastrointestinal diseases, and multiple metabolic processes. It can be difficult to diagnosis food allergy in the clinical setting. To date, few high-quality randomized controlled trials have been conducted on vitamin D and food allergy. Recent studies have shown that vitamin D levels are comparable among children with CMPA, those with other food allergy, and those with no food allergy. 27 Therefore, further randomized controlled trials are needed to confirm the relationship between allergic diseases and vitamin D levels.
Many previous observational studies have focused on the dynamic changes between 25(OH)D and PTH in different populations under different environments. Consistent with previous studies,28,29 we confirmed the inverse relationship between 25(OH)D and PTH levels. Its regulatory mechanism is known because PTH is an important hormone in regulation of bone metabolism by binding with specific receptors and increasing intracellular cyclic adenosine levels. phosphate (cyclic adenosine monophosphate) levels, and promoting bone conversion. When levels of calcium or phosphorus are decreased, PTH can regulate bone metabolism by inducing the gene expression of 1α-hydroxylase and promoting the synthesis of 1,25(OH)2 D. When levels of 25(OH)D in the body increase, the conversion rate of 1,25(OH)2 D also increases, which increases levels of calcium and phosphorus in the blood and suppresses the secretion of PTH. The concentration of PTH in the circulatory system declines. This indicates that a low level of vitamin D in allergic children will induce increased PTH concentrations. Under a continuous high dose of PTH, osteoclast activity will exceed osteoblast activity and total bone mass will eventually decrease.
BALP is an extracellular enzyme secreted by osteoblast. BALP is involved in the process of bone formation and is also a marker of osteoblast maturity and activity. Conventionally, vitamin D insufficiency reduces the absorption rate of calcium. Bone-like tissues cannot be calcified, and osteoblasts cannot be transformed into osteoblasts. The proliferation of osteoblasts is activated, and greater amounts of BALP are released into the blood, leading to increased activity of BALP. However, we observed that the activity of BALP in children with CMPA was significantly lower than that in healthy children, and the levels of serum phosphorus and CT were also lower than those in healthy children; these conditions would reduce bone formation and mineralization. The status of bone formation in children with CMPA can be detected by monitoring these indicators. Serum vitamin D levels appear before BALP changes. 30 This suggests that a reduction in vitamin D levels is more sensitive than other markers in allergic children.
In this study, serum calcium levels tended to be stable and there was no significant correlation with 25(OH)D levels, which was consistent with most survey results. 31 Considering that human serum calcium levels play an important role in the body, such as in the activity of nerves and muscles, blood calcium should be maintained at a stable concentration. Although serum calcium is positively correlated with bone mineral density, it does not directly reflect calcium deficiency and bone abnormality. Therefore, a single serum calcium index is less sensitive in terms of reflecting bone metabolism level.
Compared with previous studies, we focused more on the correlation between bone metabolism markers, especially changes in bone metabolic markers, among children with CMPA. Monitoring changes in these indicators can help to identify the potential risk of allergies earlier. However, there are still some limitations in our study. First, the sample size in this study was insufficient. Including more cases can contribute to drawing more accurate conclusions. Second, we did not include information about daily sunlight exposure, season, and dietary calcium intake.
To conclude, vitamin D levels in children with CMPA were lower than those in healthy children, and PTH was increased at the same time, suggesting that osteoblastic dysfunction and osteoclast hyperactivity in children with CMPA are likely to result in a reduction in peak bone mass. These bone metabolism indicators, especially serum 25(OH)D and PTH, may be more sensitive in reflecting the status of bone metabolism among children with CMPA in real-time, which can be used to monitor the efficacy of vitamin D supplementation in clinical settings. Appropriate substitution of essential micronutrients in the diet of children with CMPA could result in complete resolution of the clinical symptoms of osteopenia and rickets.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: This work was supported in part by the Maternal and Child Health Care Center, Chinese Center for Disease Control and Prevention (number 2020FYH006).
