Abstract
Lumbar disc herniation is a common disorder in adults that is accompanied by lower back and radicular pain. A 32-year-old man visited our clinic with 1-week history of persistent lower back pain and weakness in his right big toe. Magnetic resonance imaging (MRI) of his lumbar spine revealed herniated discs at L3/L4, L5/S1 and L4/L5, where a right-sided intraspinal mass lesion deep to the L4 vertebral body was causing compression of the nerve root. The patient underwent conservative treatment and reported no symptoms referrable to his back or leg 4 months later. Follow-up MRI showed no herniation of the nucleus pulposus at the L4/L5 level or lesion deep to the vertebral body of L4, whereas no changes had occurred to the status of the herniated L3/L4 and L5/S1 discs. The present case and a literature review show that a sequestered lumbar disc herniation can regress within a relatively short timeframe without surgery. The authors emphasise the utility of conservative therapy for patients who do not have a definitive surgical indication.
Keywords
Introduction
Lumbar disc herniation is a common disease, with an estimated incidence of 5% in adults. 1 Dandy 2 first described the clinical symptoms of radiculopathy resulting from disc herniation in 1929. Later, in 1934, Mixter and Barr 3 successfully performed surgery on patients with evidence of intervertebral disc rupture. Subsequent studies4,5 have shown that patients who undergo surgery early display faster pain relief and sensory recovery. In contrast, several clinical studies6,7 have shown no differences in outcomes between surgical and conservative care after 2 years, except that early surgery is associated with faster pain relief and recovery than non-surgical treatment. Furthermore, 8 surgery has been shown to be associated with significantly better outcomes than conservative management after 1 year, but no differences after 4 or 10 years. Finally, other studies9–31 have documented cases of excellent spontaneous lumbar disc regression following non-surgical treatment.
The exact mechanisms of the spontaneous regression of lumbar disc herniation remain to be determined.27,32,33 However, three principal hypotheses have been posited:1,34,35 dehydration and shrinkage, retraction, and inflammation and neovascularisation. Moreover, some previous studies36,37 have shown a relationship between the resolution of lumbar disc herniation and other factors. In the present article, we report a case of the spontaneous regression of lumbar disc herniation and review the related literature. The patient provided his informed consent for publication of the case details.
Case
The reporting of this study conformed to the CARE guidelines. 38 A 32-year-old man visited our clinic with a 1-week history of persistent lower back pain and weakness in his right big toe. Physical examination showed muscle weakness (grade 3/5) of his right extensor hallucis longus, with reductions in sensation over the L4 dermatome and the ability to raise his lower right leg by 40° while straight, but no incontinence. Magnetic resonance imaging (MRI) of his lumbar spine revealed herniated discs at L3/L4, L5/S1 and L4/L5, where there was a right-sided intraspinal mass-like lesion that extended deep to the L4 vertebral body, which was causing compression of the nerve root (Figure 1). The differential diagnosis of the intraspinal mass-like lesion included sequestered disc herniation and tumour, such as schwannoma or neurofibroma. Rim-enhanced MRI was conducted 4 days later, and showed a large nucleus pulposus herniation (Figure 2). The patient declined surgery in favour of conservative treatment, and agreed to undergo physical therapy, to sleep on a hard/firm mattress and to perform exercises, without taking medication. His lower back pain and leg numbness were gradually relieved and the patient reported no symptoms relating to his back or leg after 4 months. At follow-up examination, both physical examination and the straight-leg raising test yielded normal results, and MRI showed no herniation of the nucleus pulposus at the L4/L5 level, whereas the herniation status of the L3/L4 and L5/S1 discs was unchanged (Figure 3). Subsequent physical therapy, consisting of acupuncture and massage, helped to relieve the patient’s pain and numbness, and ongoing exercise maintained his quality of life.

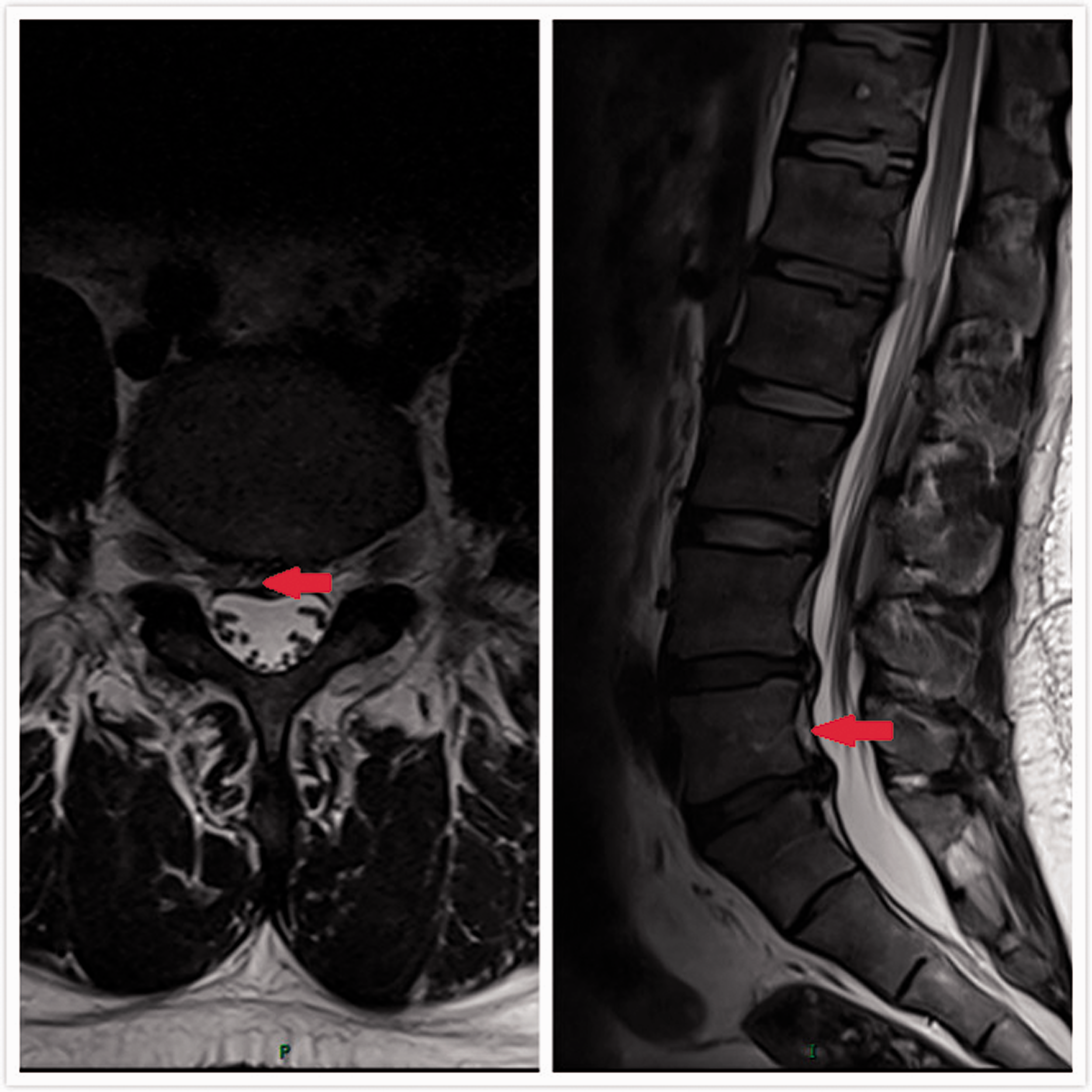
T2-weighted sagittal (left) and axial (right) magnetic resonance images showing an intraspinal mass-like lesion at the L4/L5 level and deep to the vertebral body of L4 (arrows), which was causing compression of the nerve root.

Post-gadolinium T1-weighted sagittal (left) and axial (right) rim enhancement magnetic resonance image obtained 4 days after the initial images shown in Figure 1, showing a large nucleus pulposus herniation at the L4/L5 level (arrows).
T2-weighted sagittal (left) and axial (right) magnetic resonance images showing the absence of the nucleus pulposus herniation (arrows) 4 months after the initial visit.
Discussion
The incidence of lumbar disc herniation in adults is approximately 5% and rising. 1 Following the development and rapid expansion of the use of a surgical intervertebral disc approach, a survey of 817 surgeons from 89 countries indicated that as many as 76 disc procedures were being performed per surgeon per year in 2015. 39 Since the first clinical report of the spontaneous regression of disc herniation was published by Guinto et al. 40 in 1984, increasing numbers of such instances have been reported, alongside the development of the widespread use of computed tomography and MRI. Recently, a study of 64 patients found that most showed complete resolution of their lumbar disc herniation after a mean of 17 months, and that their symptoms and function improved with conservative treatment. 41 The present case illustrates the possibility of achieving spontaneous disc regression without surgical management. However, we stress the importance of decompressive surgery when there is a significant motor deficit or cauda equina syndrome to avoid serious neurological sequelae and/or incontinence. Here, we will discuss the present case alongside the details of other published cases, to analyse the factors associated with the spontaneous regression of a herniated lumbar disc.
We reviewed all the published case reports regarding patients diagnosed with spontaneous lumbar disc regression who underwent follow-up MRI. Cases that involved infectious, neoplastic, metabolic and/or congenital causes of lumbar disc herniation were excluded. The 31 cases discussed in the manuscript met all the inclusion and exclusion criteria. The comprehensive information collected included age, sex, location, classification of disc herniation, symptoms, defects on the neurological examination performed, and the time to resolution on MRI (Table 1). In 32 cases (including the present case) there was spontaneous regression of a herniated lumbar disc (Table 1). The mean age of the patients was 46.4 years and 71.0% were male. The locations of the disc herniations were L1/L2 (two cases, 6.3%), L2/L3 (one case, 3.1%), L3/L4 (eight cases, 25.0%), L4/L5 (13 cases, 43.8%), and L5/S1 (seven cases, 21.9%). Most of the cases (56.3%) of herniation involved sequestration and the rest (43.7%) were of the extrusion subtype. The case reports showed that 65.6% of the cases had lower back pain, 87.5% had radicular pain and 59.4% had both types. They also showed that 40.6% of the patients had a positive straight-leg raising test, 43.8% had sensory disturbances and 34.4% had motor weakness. The mean time to spontaneous lumbar disc regression was 10.1 months, the mean time to sequestration was 6.8 months and the mean time to extrusion was 14.4 months. The present case manifested the sequestration subtype and there was therefore a good chance that spontaneous regression would occur. In contrast to some of the other cases, the present patient only underwent physical therapy (acupuncture and massage) and performed exercises, but did not take medication. Our experience with the present case and the literature review suggest that rim enhancement MRI should be used to predict the spontaneous regression of lumbar disc herniation.
Summary of cases involving spontaneous regression of lumbar disc herniation.

LBP: lower back pain, RP: radicular pain, SLRT: straight-leg raising test. SD: sensory disturbance.
Previous studies have suggested various hypotheses for the mechanism of spontaneous disc regression. For example, the dehydration theory states that the nucleus pulposus herniation might shrink back into the annulus fibrosus as a result of gradual dehydration.32,42 A second hypothesis states that a herniated disc might retract back into the intervertebral space if it protrudes through the annulus fibrosus without separating from it. 9 A third hypothesis concerns inflammation and neovascularisation: lumbar disc herniation into the epidural space causes inflammation and neovascularisation, with gradual resorption of the cartilage through enzymatic degradation and phagocytosis.1,34 However, in our opinion, both dehydration and inflammation and neovascularisation may be involved in the process of disc herniation, and especially in nucleus pulposus herniation.
Although the exact mechanisms of the resolution of a herniated disc without surgery remain unclear, some previous studies have shown a relationship between the spontaneous resolution of lumbar disc herniation and other factors. Bozzao et al. 33 demonstrated a positive correlation between the size of a herniated disc and the amount of reduction, but no relationship between the reduction of disc herniation and the location of the herniation. Similarly, Splendiani et al. 43 found that the evolution of disc herniation showed no relationships with location, size, or level. The classification of disc herniation might be important for disc regression. For example, Virri et al. 44 found that sequestrated disc material contained more macrophages and involved a more intense inflammatory reaction than an extruded disc. Autio et al. 36 found a higher incidence of disc regression in patients of 41 to 50 years. Komori et al. 1 concluded that the migration of a herniated disc facilitated the resorption of a herniated nucleus pulposus because of greater vascular supply. Autio et al. 36 suggested that the thickness of the region of enhancement on the baseline MRI is the best predictor of the regression of disc herniation, with greater thickness being positively associated with absorption of the herniated nucleus pulposus.
The relationships between clinical outcomes and spontaneous disc regression require further study. Oktay et al. 27 showed that a decrease in the herniation ratio of over 20% is associated with clinical improvement, but Hong et al. 45 found that patients whose disc herniation does not improve radiologically can also show amelioration of symptoms. However, other studies25,34 have shown that lumbar disc herniation can disappear after treatment using pain relief alone, or that symptoms may reappear.
Conclusions
The details of the present case and literature review imply that patients with the sequestration subtype of disc herniation are significantly more likely to show spontaneous regression than those with bulging or protruding discs. Rim enhancement MRI should be used to predict the regression of lumbar disc herniation. For patients with a large herniated lumbar disc, especially if it is of the extrusion or sequestration subtypes, conservative treatment is preferable in the absence of definitive surgical indications.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211058987 - Supplemental material for Spontaneous regression of a large sequestered lumbar disc herniation: a case report and literature review
Supplemental material, sj-pdf-1-imr-10.1177_03000605211058987 for Spontaneous regression of a large sequestered lumbar disc herniation: a case report and literature review by Chengxiang Hu, Baocheng Lin, Zhixing Li, Xiaozhuan Chen and Kun Gao in Journal of International Medical Research
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This case was approved for publication by the Ethics Committee of Shenzhen Traditional Chinese Medicine Hospital (K2019-001-01). Written informed consent was obtained from the patient to publish this case report.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: This study was funded by the Sanming Project of Medicine in Shenzhen (No. SZSM201812066).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
