Abstract
Biliary anomalies are a high risk for biliary injury during surgery, and although a biliary anomaly is occasionally encountered, variations in cystic ducts are rare. A preoperative diagnosis is highly valuable in facilitating surgical procedures and avoiding surgical complications. Herein, the case of a 67-year-old female patient with acute cholecystitis, in which preoperative fluoroscopic cholangiography clearly demonstrated a single gallbladder with double cystic ducts, is presented. The accessory duct was found to be dominant, draining into the otherwise normal right intrahepatic bile duct, and laparoscopic cholecystectomy was performed smoothly and successfully. Fluoroscopic cholangiography is a powerful tool that may clearly depict the anomaly of a single gallbladder with double cystic ducts. Through appropriate preoperative knowledge and demonstration of this biliary anomaly in the present case, laparoscopic cholecystectomy was safely performed, and the patient was symptom-free at the 3-year follow-up assessment.
Introduction
Variations in the biliary tree are occasionally encountered, however, a double cystic duct is relatively rare, and is often associated with a double gallbladder.1,2 The present report describes the case of a single gallbladder with double cystic ducts that were delineated during a preoperative fluoroscopic cholangiogram. Such an anomaly may pose a high risk for intraoperative biliary injury, particularly during laparoscopic cholecystectomy. 3 Preoperative fluoroscopic cholangiography is a powerful tool that may clearly depict this type of biliary anomaly and, thus, may facilitate safe laparoscopic surgery. 4
Case report
All procedures performed in the present case study involving a human participant were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Written informed consent for percutaneous gallbladder drainage was obtained from the patient and verbal informed consent was additionally obtained. Chang Gung Medical Foundation Institutional Review Board, IRB No. 202001054B0, provided approval to publish the case, and the need for informed consent was waived. The reporting of this study conforms to CARE guidelines. 5
A 67-year-old female patient, with a history of type 2 diabetes mellitus and essential hypertension, presented at the emergency room of Chang Gung Memorial Hospital in April 2016 with intermittent fever and progressive epigastralgia for the previous 5 days. Physical examination revealed Murphy’s sign, and a blood test showed leukocytosis (white blood cell count, 17.7 × 1000 cells/µl). Liver enzymes were found to be within normal limits ( glutamic-pyruvic transaminase [alanine aminotransferase], 16 U/l; total bilirubin, 0.7 mg/dl; and alkaline phosphatase, 82 U/l). A clinical diagnosis of acute cholecystitis was supported by computed tomography findings of gallbladder lumen distention, with gall stones and wall thickening (Figure 1). Subsequent percutaneous cholecystostomy was performed for decompression, resulting in drainage of dark brownish bile. At 14 days following percutaneous cholecystostomy, a fluoroscopic cholangiography was arranged for biliary assessment. The percutaneous cholecystostomy catheter was used to perform fluoroscopic cholangiography, during which a single gallbladder with double cystic ducts was discovered. The accessory duct was found to be dominant and drained into the otherwise normal right intrahepatic bile ductal system (Figure 2 and 3). As a result, an elective laparoscopic cholecystectomy was performed smoothly and successfully 3 months later. Over 3-years of clinical follow-up, the patient was well-recovered and reported no further symptoms.
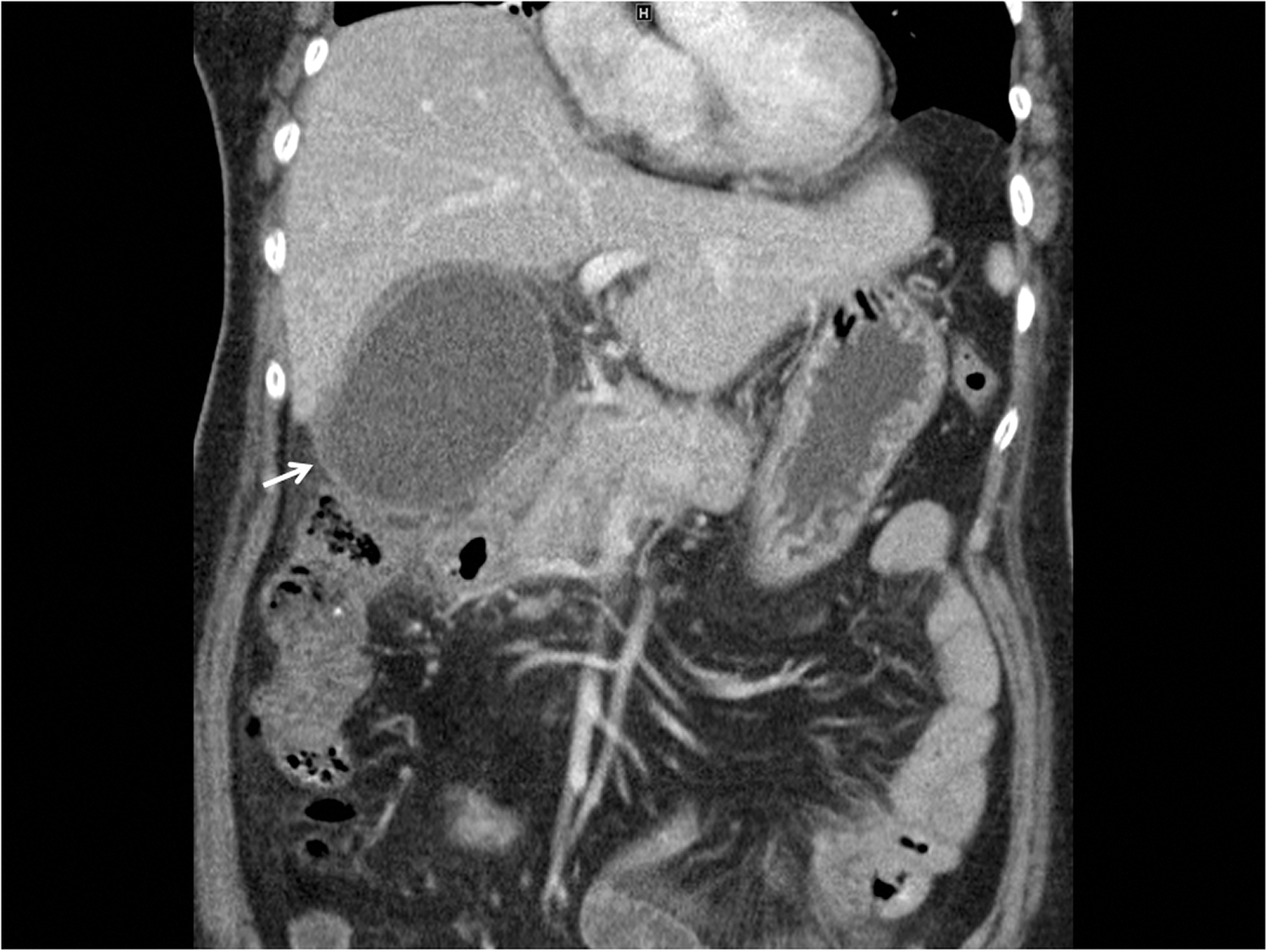
Representative coronal plane enhanced computed tomography image from a 67-year-old female patient with intermittent fever and progressive epigastralgia for the previous 5 days, showing a typical-looking inflamed gallbladder (arrow) with marked distention and wall thickening.

Representative cholangiography image from a 67-year-old female patient who had presented with intermittent fever and progressive epigastralgia for the previous 5 days. Iodine contrast medium was injected via the percutaneous cholecystostomy catheter used to treat the patient, and was shown to flow into the right hepatic duct (arrowheads) and further into the common hepatic duct.

Representative cholangiogram at the right posterior oblique position from a 67-year-old female patient who had presented with intermittent fever and progressive epigastralgia for the previous 5 days, showing: (a) an accessory cystic duct (arrow) draining into the right hepatic bile ductal system; and (b) a following supine film revealing the smaller ordinary cystic duct (arrow).
Discussion
A cholecystohepatic duct is an anomalous hepatic duct that connects directly to the cystic duct or gallbladder, 1 observed with a frequency of 0.7–1.2%. 6 The incidence of cholecystohepatic duct anomaly is much lower than that of other aberrant hepatic ducts and is thought to arise as a result of abnormal biliary tract embryology. 7 Among the hepatic duct anomalies, a single gallbladder with double cystic ducts is extremely rare, with only a few cases reported in the English language literature.3,4
A comprehensive surgical approach during cholecystectomy is mandatory for patients with a cholecystohepatic duct anomaly. 7 Injury to the bile duct may result in bile leakage, bile duct stricture, cholangitis, or liver abscess, and surgical injury related to this biliary anomaly have been reported with morbidities in 0.2–2% of cases after laparoscopic cholecystectomy. 8 Such an injury was highly likely to occur in the present case, as the right hepatic duct being mistaken for the cystic duct may have been erroneously ligated and divided during surgery.
Preoperative identification of cholecystohepatic duct anomalies is pivotal to avoid surgical complications, however, preoperative diagnosis of the biliary anomaly is deemed difficult without a tailored imaging investigation. 4 Although magnetic resonance cholangiopancreatography is reported to have a 66% sensitivity in identifying accessory bile ducts, 9 it is not routinely used for preoperative evaluation.
If emergency surgery is not advised in a patient with acute cholecystitis, delayed or elective laparoscopic cholecystectomy after percutaneous cholecystostomy is often considered. In addition, a fluoroscopic cholangiography for bile duct evaluation before definitive laparoscopic cholecystectomy is often recommended. 10 The present report clearly demonstrates this rare anomaly of a single gallbladder with double cystic ducts, in which the accessory duct is dominant and drains into the normal right intra-hepatic ductal system. Laparoscopic cholecystectomy is widely applied for acute cholecystitis, and is feasible for this rare anomaly of a single gallbladder with double cystic ducts. 3 In the present case, fluoroscopic cholangiography allowed the dynamic bile flow to be observed, providing a clear map for facilitating the surgical procedure.
Surgeons and radiologists should be aware of this rare anomaly of a single gallbladder with double cystic ducts, and should note that this uncommon condition may be clearly detected by fluoroscopic cholangiography. Preoperative use of this powerful tool in the present case provided appropriate preoperative knowledge and demonstration of this biliary anomaly, allowing laparoscopic cholecystectomy to be safely performed without biliary complication.
Footnotes
Acknowledgements
The authors give their thanks for the work of their radiological colleagues and all staff at Chang Gung Memorial Hospital involved in managing the case.
Author contributions
C-HW and PWW drafted the manuscript. S-CK performed the surgery. C-HW, Y-CW, and S-CK collected and analysed the clinical and imaging data. C-HW critically revised the article for important intellectual content, and C-HW and PWW edited the manuscript. C-HW and PWW reviewed the draft. All authors read and approved the final manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors
