Abstract
Schistosomiasis is a parasitic disease that is widely considered a neglected tropical disease. It is ranked first after malaria among all parasitic diseases. The major forms of schistosomiasis are intestinal and urogenital; however, gallbladder involvement is rare and usually accompanied by imaging findings similar to those of acute cholecystitis, such as wall thickening or pericholecystic inflammation. We encountered a patient who did not show these typical imaging findings. A man in his late 40s presented to the emergency department with a 2-month history of abdominal distention. His initial laboratory examination showed iron deficiency anemia. Computed tomography revealed a mildly distended gallbladder with septations and a small calcified gallstone. Magnetic resonance imaging was performed for better characterization, and it showed gallbladder stones with multiseptated, cystic gallbladder mural lesions and no wall thickening or pericholecystic fluid. On his second visit, the patient complained of mild epigastric pain. A provisional diagnosis of cholecystitis was considered, and laparoscopic cholecystectomy was performed. Histopathological evaluation revealed a gallbladder wall with multiple foci of chronic granulomatous inflammation. Schistosoma-like ova were observed in the mucosa and submucosa and were consistent with schistosomiasis. Periodic acid–Schiff staining of the ova was positive. The patient’s postoperative course was uneventful.
Introduction
Schistosomiasis is a parasitic disease that is widely considered a neglected tropical disease. It is ranked first after malaria among all parasitic diseases. As of 2019, more than 236 million people have required prophylaxis for schistosomiasis, among whom 105.4 million have required treatment. Cases are common in tropical and subtropical areas in the Middle East, Sub-Saharan Africa, South America, and Southeast Asia where poor living conditions exist, such as areas with unsafe drinking or sanitation conditions.1,2
The major forms of schistosomiasis are intestinal and urogenital. Several species are found in the Middle East, including Schistosoma mansoni and S. haematobium, which are major causes of intestinal and urogenital schistosomiasis, respectively. 2 Humans become infected by coming into contact with contaminated water during recreational swimming or agricultural activities. Schistosomiasis is transmitted to humans by snails living in freshwater sources, such as lakes and rivers. 2
Saudi Arabia witnessed a reduction in the prevalence of schistosomiasis after implementing elimination programs; however, cases are still reported throughout the country. 3 Transmission can occur in endemic areas or in association with increasing travel frequency for economic purposes or leisure, and certain types of schistosomiasis have become more prevalent, which has led to more cases that present with unusual symptoms and severity. 2 We herein describe a Saudi man with gallbladder schistosomiasis.
Case report
A man in his late 40s with no prior medical history presented to the emergency department complaining of abdominal distension that had started 2 months prior to presentation. He reported no abdominal pain, nausea, vomiting, change in bowel habits, gastrointestinal bleeding, or weight change. On examination, his abdomen was soft with no tenderness on palpation. He was stable and showed no other signs or symptoms. He had no fever, but his systolic blood pressure was slightly elevated (Table 1).
Patient’s vital signs during first visit to emergency department.

BP, blood pressure.
Laboratory analysis showed signs of iron deficiency anemia (hemoglobin: 10.6 g/dL, iron: 8.6 µmol/L, ferritin: 15 µg/L); other laboratory tests were unremarkable. The patient was discharged, and an initial workup including computed tomography (CT) of the abdomen and pelvis was requested on an outpatient basis.
Enhanced CT of the abdomen and pelvis showed a mildly distended gallbladder with septations and small calcified gallstones (Figure 1). Magnetic resonance imaging (MRI) was performed for better characterization, and it revealed a gallbladder stone, multiseptated cystic gallbladder mural lesions, and no soft tissue component (Figure 2). The differential diagnoses included gallbladder lymphangioma, diffuse cystic adenomyoma, and xanthogranulomatous cholecystitis. No concerning features such as a soft tissue component, local invasion, or lymphadenopathy were noted.

Abdominal computed tomography in the portal venous phase showing (a, b) axial and (c, d) coronal views. The gallbladder is mildly distended with septation, and a small stone is noted. No adjacent fat stranding, gross soft tissue component, or biliary duct dilatation are noted.
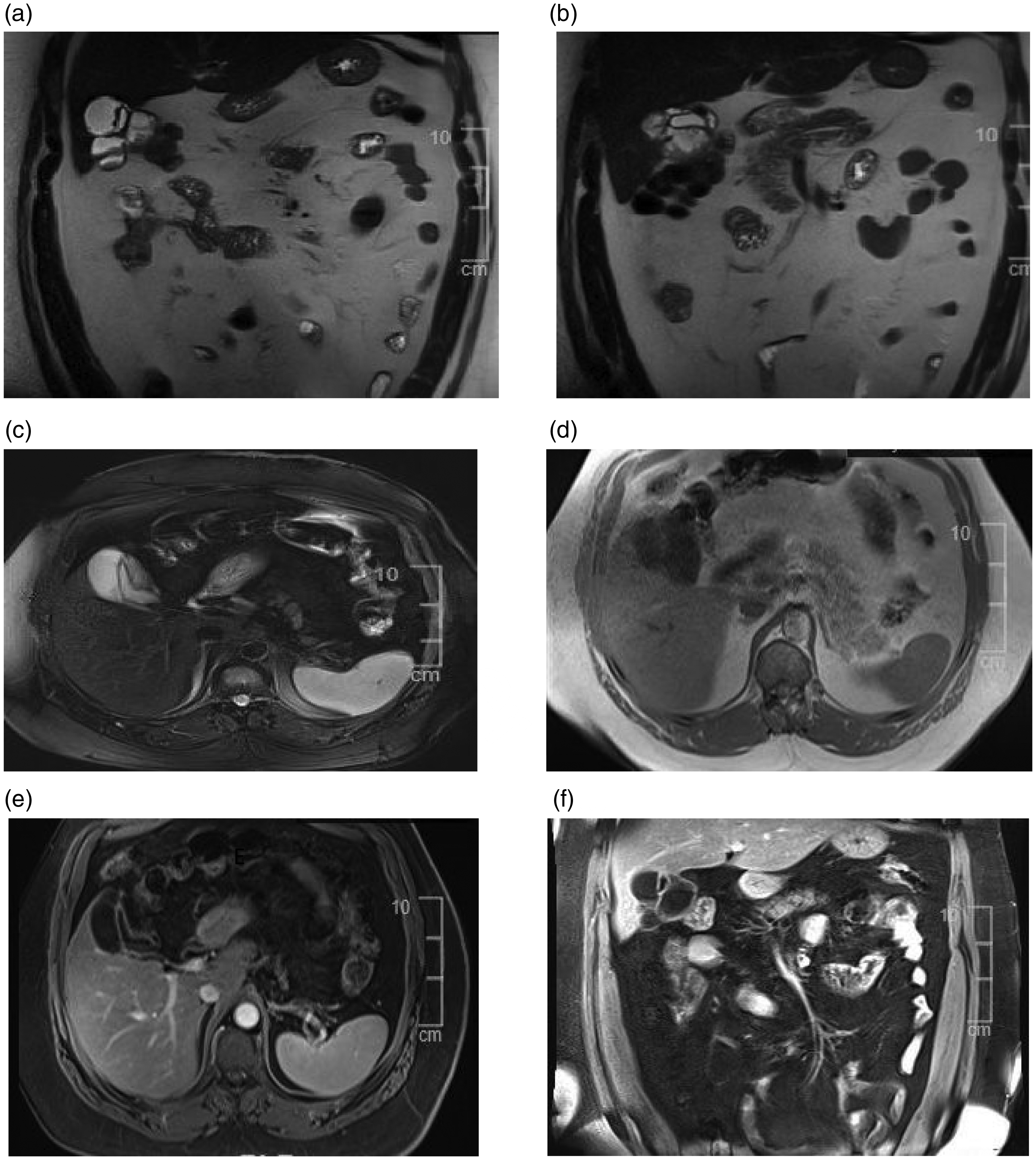
Magnetic resonance imaging of the gallbladder. (a, b) Coronal T2, (c) axial T2 fat-saturated, (d) axial T1, and (e, f) post-contrast views demonstrate a multi-septate cystic mural lesion with high T2 and low T1 signal intensity with enhancing septation on the post-contrast sequence. No nodular enhancement, soft tissue component, gallbladder wall thickening, or pericholecystic free fluid are noted.
The patient returned to the emergency department 1 week later because of a 3-day history of acute-onset, continuous fever associated with chills. This was relieved by paracetamol and was not exacerbated by anything. He reported fatigue, diarrhea, and generalized abdominal pain. He had also experienced intermittent shortness of breath for 3 days that was not relieved or exacerbated.
On his second visit to the hospital, the patient’s vitals indicated low-grade fever and elevated blood pressure (Table 2). On physical examination, he was alert, conscious, and oriented. His abdomen was soft with mild epigastric tenderness. A provisional diagnosis of acute cholecystitis was made, and the patient was scheduled for laparoscopic cholecystectomy.
Patient’s vital signs during second visit to emergency department.

BP, blood pressure; SpO2, oxygen saturation.
Intraoperatively, a laparoscope was inserted into the abdomen under direct vision. The peritoneal cavity was inspected, and severe omental attachments to the gallbladder were observed and gently swept away until an atraumatic grasper could be used to superiorly retract the fundus of the gallbladder. The gallbladder was inadvertently opened, and pus poured out (empyema), which was suctioned. Filmy adhesions between the gallbladder and the omentum and duodenum were lysed, and the gallbladder was shaved off the liver bed. The infundibulum was hard and contained an impacted stone. Following complete removal of the gallbladder, we identified and suctioned a pus collection beneath the posterior wall of the gallbladder.
The gallbladder was sent for gross and microscopic pathological assessment. Grossly, the specimen consisted of a previously opened gallbladder measuring 5.0 × 3.5 cm, and its wall thickness ranged from 1.0 to 0.4 cm. The serosal surface was firm, heterogeneous, brown, hemorrhagic, and irregular. The mucosal surface was heterogenous, pale, brown, and thickened. Representative samples were submitted in two cassettes. Microscopically, the specimen showed a gallbladder wall with multiple foci of chronic granulomatous inflammatory. Schistosoma-like ova were seen in the mucosa and submucosa, consistent with schistosomiasis. Periodic acid–Schiff staining of the ova was positive. The patient had an uneventful postoperative course and was discharged home.
The reporting of this study conforms to the CARE guidelines. 4
Discussion
Schistosomiasis is one of the most prevalent neglected tropical diseases worldwide, accounting for 240 million cases per year. 5 Although efforts to control the parasite in Saudi Arabia have shown some success, elimination remains a challenge. 3 Most cases in Saudi Arabia are seasonal, occurring after the rainfall season, when people tend to use seasonal lakes for recreational purposes or agricultural uses. Although schistosomiasis is endemic in Saudi Arabia and is expected to be encountered in clinical practice, the presentation of gallbladder schistosomiasis is rare on a global scale. Few cases of gallbladder schistosomiasis have been reported worldwide; one recent case was reported in Saudi Arabia by Majrashi and Al Amoodi. 6
The clinical presentation is highly dependent on the affected organ. Intestinal schistosomiasis will result in pain in the abdominal area and loose and bloody stool; the late stage is associated with hepatosplenomegaly, portal hypertension, and ascites. By contrast, urinary schistosomiasis can result in granulomatous inflammation and subsequent ulceration of the ureters and urinary bladder. Urinary schistosomiasis is associated with obstructive symptoms, frequent and painful urination, and hematuria. 7 Chronic renal disease and urinary bladder cancer have also been reported. Moreover, schistosomiasis is associated with anemia and unwanted outcomes in pregnant women and their fetuses as well as poor growth and hampered milestone developments in children.5,8 Symptoms of gallbladder schistosomiasis are not specific to Schistosoma infection; nevertheless, it includes features of the typical presentation of other gallbladder pathologies, such as right upper quadrant pain that might radiate to the right shoulder and general symptoms such as nausea, vomiting, or diarrhea.9,10 On physical examination, abdominal tenderness is the most commonly reported symptom,6,10,11 and a positive Murphy’s sign has also been reported. 6 In our case, the initial presentation was abdominal distension; during the second visit, the patient reported abdominal pain, low-grade fever, difficulty breathing, fatigue, and diarrhea. Complications were reported in a case in Qatar, and the literature review associated with that case report revealed complications of cholangitis, liver abscess, and even fibrosis. 9
The radiological presentation of gallbladder schistosomiasis consists of typical wall thickening and external perturbance. Other presentations include a smooth luminal surface, and chronic cases may result in a negative Murphy’s sign, which can be an alarming sign of malignancy. Other manifestations reported in the literature include impaired contractility and the presence of calculi and sludge.12–14 However, no wall thickening or pericholecystic inflammation was present in our case. We instead observed a multiseptated cystic mural lesion with enhancing septation on post-contrast CT and MRI, which is rarely reported in the literature. To the best of our knowledge, most of the reported cases in the literature do not include MRI; this adds to the novelty of the present case.
Both CT and MRI revealed the presence of stones in our case. There are several hypotheses for the development of such stones. One explanation is a granulomatous reaction of the gallbladder wall, 15 another is the development of gallbladder stenosis that narrows the outflow of bile and results in stone formation, 10 and another is that schistosomiasis coexists with cholelithiasis and does not necessarily cause it. On CT, the gallbladder may show wall thickening and calcification, while ultrasound may reveal a hyperechogenic gallbladder bed due to either calcification or fatty involvement of the gallbladder fossa.12,16
In the literature, the gross presentation usually shows an irregular wall with fibrotic changes associated with liver infiltration and adhesions to the omentum or bowels. 9 Similar to the present case, the histological presentation usually includes the presence of a fibrotic granuloma containing a Schistosoma ova. However, granulomatous changes are not limited to schistosomiasis; the differential diagnoses include xanthogranulomatous cholecystitis, Crohn’s disease, X-linked chronic granulomatous disease, and cancer.9,11,16–19
Most cases of gallbladder schistosomiasis are managed by laparoscopic surgery. Surgeons should consider the possibility of schistosomiasis when managing patients with cholecystitis and should be prepared for worst-case scenarios.6,20 While not used in our case, medical management for schistosomiasis includes praziquantel, which might be prescribed postoperatively as a complementary treatment.9,20 Reinfection with Schistosoma remains a possibility in a portion of cases. Our patient’s postoperative course was unremarkable.
In patients with a history of travel to or residence in endemic areas, the possibility of schistosomiasis as a cause of cholecystitis should be considered. Prevention remains the best approach to avoid infection with schistosomiasis. Although no vaccine exists, another approach that has shown success is avoidance of swimming, bathing, and drinking fresh water in areas where local transmission of schistosomiasis occurs. If the situation warrants the use of fresh water, the water should be boiled or filtered before personal use for bathing or drinking. 21
Conclusion
When encountering a patient with suspected gallbladder disease, physicians should consider the possibility of gallbladder schistosomiasis, especially in endemic countries or in individuals who have recently traveled to endemic countries. Laparoscopic cholecystectomy with or without additional medical treatment is the most common approach for such patients. Avoiding contact with unfiltered or untreated fresh water in endemic areas remains the preferred method of prevention.
Footnotes
Acknowledgements
We would like to thank the patient and the hospital staff for their cooperation.
Author contributions
M. Aldamegh and YM: Acquisition of data, interpretation of radiological findings, and writing of case report. M. Aljohani: Writing of case report. All authors have reviewed the manuscript and approve its publication.
Data availability statement
The data are available upon reasonable request from the first author.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics statement
This study was conducted according to the World Medical Association Declaration of Helsinki. Consent was waived, and the patient’s information was de-identified. Ethical approval was obtained from King Fahad Medical City Institutional Review Board (IRB registration number: H-01-R-012, IRB log number: 23-171).
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
