Abstract
Osteoporosis is a rising concern in the aging population and should be considered before performing spinal surgery for older patients. Nonfusion surgery using interlaminar or interspinous devices is gradually gaining acceptance because adjacent segment disease seldom occurs postoperatively; however, other complications may occur. This report discusses the surgical outcomes of two women with osteoporosis treated by laminectomy and interlaminar device (IntraSPINE®) placement. Both patients had experienced low back pain for several years and had developed vertebral compression fractures. Several conservative treatments, including rehabilitation and local injections, were ineffective. Their bone mineral density levels were −3.0 and −2.8, indicating severe osteoporosis according to the definition established by the World Health Organization. They chose to undergo nonfusion surgery with IntraSPINE® interlaminar device placement. Their pain significantly decreased postoperatively, and their visual analog scale scores decreased from 8 to 2 and 3. Their extremity numbness and back pain resolved within 3 months. Both patients were satisfied with the surgical outcomes. No complications had occurred by 1 year postoperatively. These cases indicate that osteoporosis may not be an absolute contraindication for nonfusion spinal surgery. This report suggests a possible alternative surgical treatment for patients with osteoporosis that is refractory to conservative treatments.
Introduction
The number of cases of osteoporosis, a common bone disease characterized by high bone fragility, has increased annually because of the growth of the aging population, indicating a potential public health problem. 1 Likewise, spinal stenosis has become a common and major problem among older people. This condition is attributed to osteophyte formation from zygapophyseal joint degeneration, ligamentum flavum hypertrophy, disc space narrowing, and circumferential bulging of the disc osteophyte complex. 2 However, given the increasing lifespan of the general population, the number of older patients who require spinal surgery is also rising.3,4
Degenerative lumbar diseases can be treated in several ways, including decompression alone, posterior lumbar interbody fusion, and nonfusion lumbar spinal surgery.5,6 Among these, posterior lumbar interbody fusion is commonly used because of its biomechanical stability and high rate of successful fusion. However, it has some associated complications, such as adjacent segment disease (ASD), pedicle screw backout, and the halo phenomenon.7–9 Meanwhile, decompression alone sometimes results in iatrogenic instability, leading to poor outcomes. 10 In recent years, nonfusion lumbar spinal surgery has been gradually gaining acceptance.
According to the theory established by Tachibana et al., 11 dynamic stabilization by nonfusion devices can prevent the occurrence of ASD. Currently available nonfusion devices include the Wallis, Coflex®, X-Stop, Dynesys, and IntraSPINE®.12–14 Among these, the IntraSPINE® is placed only within the interlaminar spaces rather than the interspinous spaces. The IntraSPINE® was historically indicated for young patients with conditions such as disc degeneration, lumbar instability, and zygapophyseal joint syndromes. 15 Although the indications for IntraSPINE® placement were proposed by the designer, the application of this device in patients with osteoporosis has remained unreported. Hence, this study was performed to report the clinical outcomes of two patients with osteoporosis and spinal stenosis treated by posterior decompression and IntraSPINE® placement surgery.
The two patients described in this report were 87- and 81-year-old women with bone mineral density (BMD) levels of −3.0 and −2.8, respectively. Both patients had also previously sustained a vertebral compression fracture. As defined by the World Health Organization (WHO), the criteria for severe osteoporosis is a BMD level below −2.5 and one or more documented fragility fractures.1,16 Both patients satisfied the criteria for severe osteoporosis. Conservative treatments did not prove useful, and after discussions with the patients, they decided to undergo nonfusion spine surgery. After the surgery was performed, the patients’ back pain and lower extremity numbness disappeared within 3 months. Thus, the clinical outcomes were successful.
Case report
Case 1
An 87-year-old woman who had experienced low back pain and right thigh numbness for several years was brought to our outpatient department. Radiography and magnetic resonance imaging revealed T12, L1, and L2 compression fractures with prior cement augmentation, spondylolisthesis, and ligamentum flavum hypertrophy at the L4–5 level (Figure 1). Her BMD level was −3.0, and she was diagnosed with severe osteoporosis according to the WHO criteria. Thus, she was scheduled for decompression and laminectomy for lumbar spondylolisthesis and stenosis treatment.
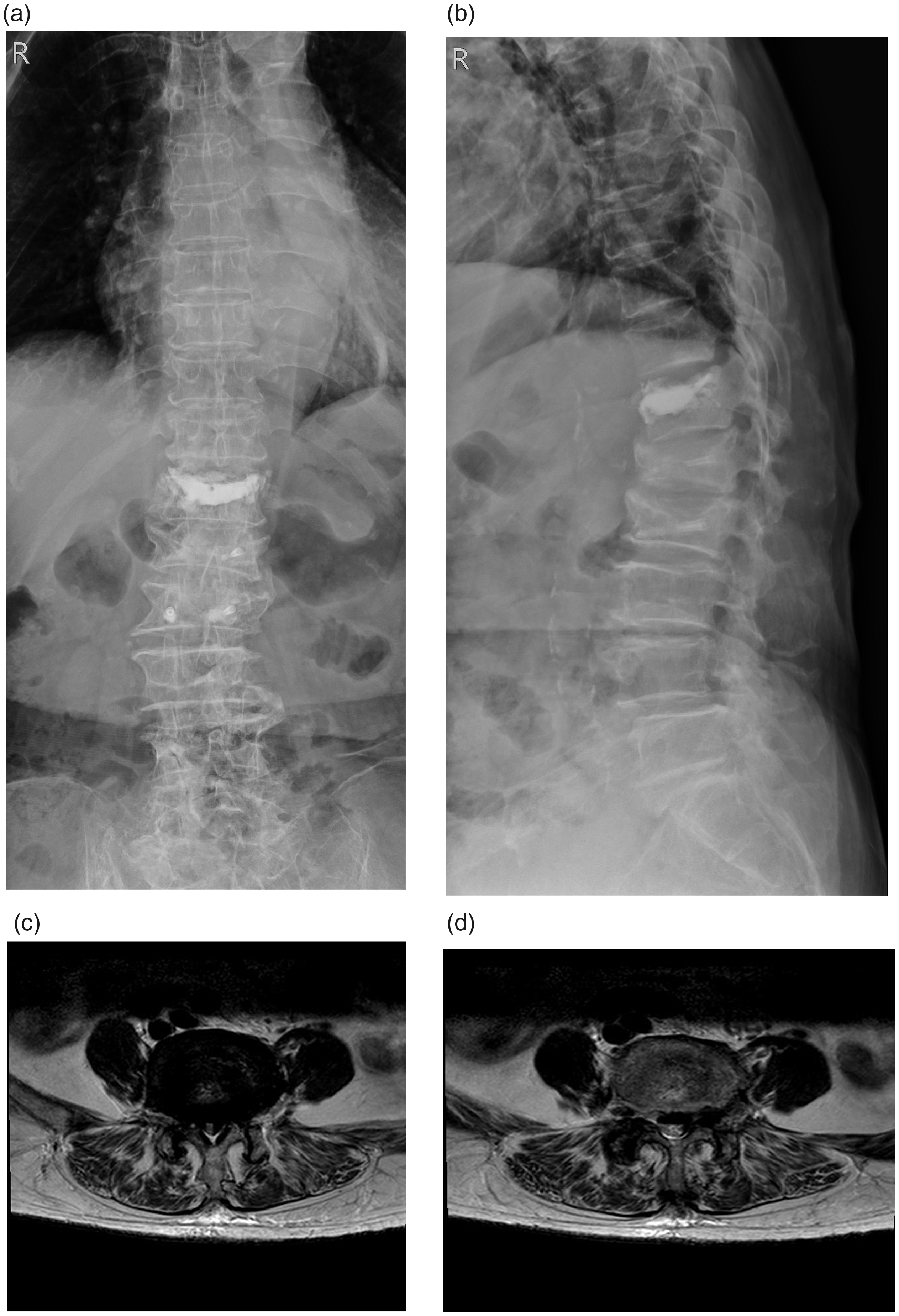
Case 1. Preoperative (a, b) radiographs and (c, d) magnetic resonance images. The images revealed L4–5 spondylolisthesis (grade I) with spinal stenosis. T12, L1, and L2 compression fractures with prior cement augmentation were observed.
After obtaining an accurate diagnosis of the spinal lesion, proper decompression and laminectomy at the L4−5 segment was performed. The IntraSPINE® interlaminar device was then placed within the L4−5 level. Postoperatively, the patient’s visual analog scale score for the right lower limb decreased from 8 to 3. She underwent low back muscle exercises for rehabilitation. For protection, she wore a lumbar brace attachment for 6 months. Three months after the decompression surgery, her discomfort and back pain were completely resolved. She could walk using crutches and was satisfied with the surgical outcome.
The patient was followed up regularly as an outpatient. One year postoperatively, plain radiography revealed no progression to spondylolisthesis or laminar breakdown-related implant failure (Figure 2). Her symptoms ultimately subsided with no occurrence of ASD.

Case 1. One-year postoperative radiographs. No implant loosening or spinal structure fracture was noted in the images.
Case 2
An 81-year-old woman presented to our outpatient department because of low back pain and left thigh numbness and pain. She had a history of cement augmentation for a T12 compression fracture and open reduction and internal fixation surgery for a left proximal humerus fracture. She was unable to walk independently using crutches for more than 10 m. Previous angiography findings had ruled out the possibility of vascular claudication. Additionally, radiography revealed no spondylolisthesis over the lumbar area. However, magnetic resonance imaging showed L3–5 segment ligamentum hypertrophy with central stenosis and L4–5 lateral recess with spinal stenosis (Figure 3). Her BMD level was −2.8, which met the criteria for severe osteoporosis as defined by the WHO.
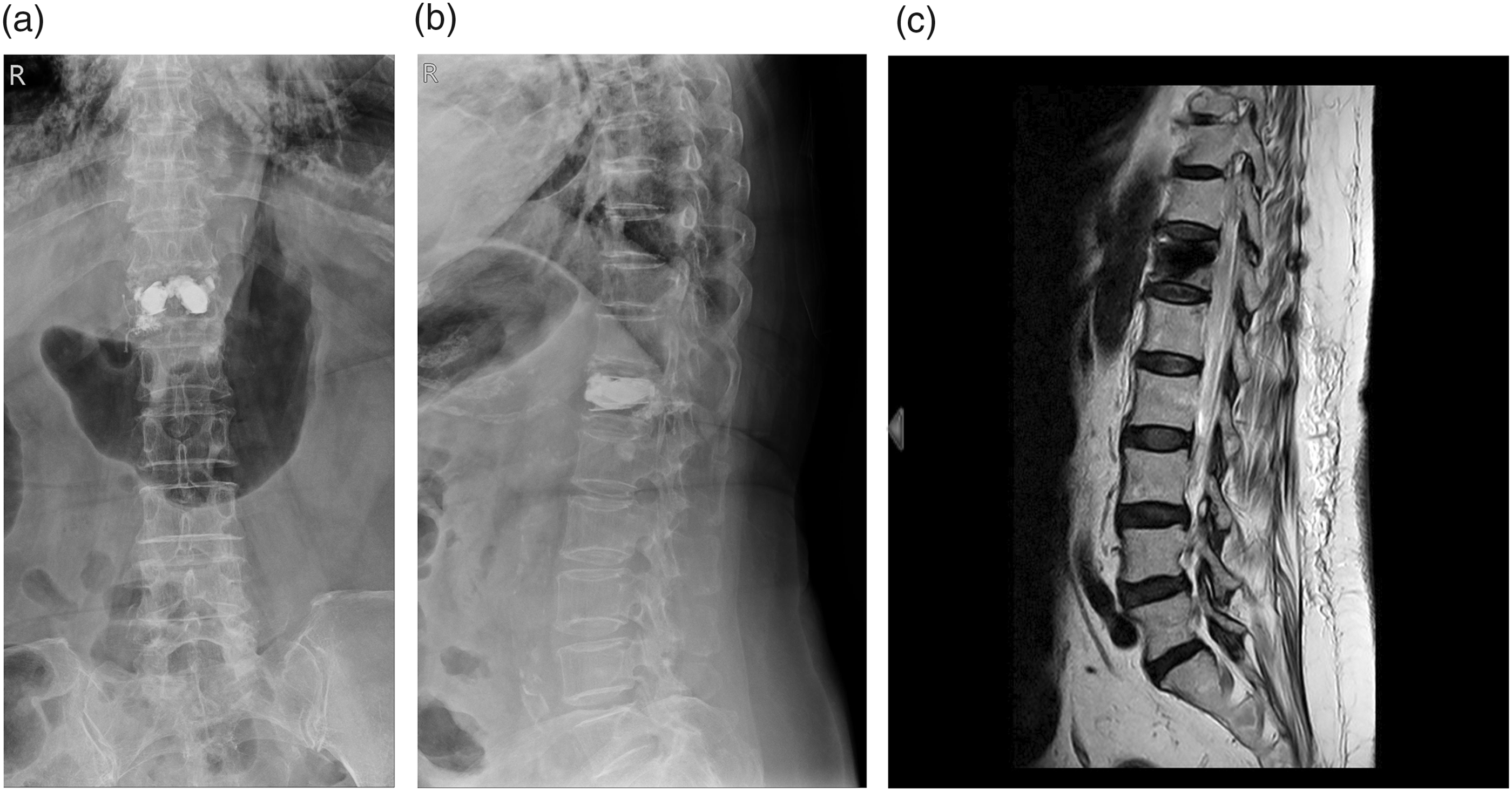
Case 2. Preoperative (a, b) radiographs and (c) magnetic resonance images. The images revealed an L3–5 bulging disc. T12 compression fracture with cement augmentation was observed.
Medial facetectomy and ligamentum flavectomy were performed at the L4–5 and L3–5 levels, respectively. After proper decompression, the IntraSPINE® device was inserted within the L3–4 and L4–5 levels to restore the disc height. Postoperatively, the patient gradually recovered and became able to perform her usual activities, and she was further encouraged to participate in a low back muscle exercise rehabilitation program. Moreover, the patient’s visual analog scale score for her back pain and left thigh pain decreased from 8 to 2. One year after the surgery, no restenosis, ASD, or implant migration or failure had occurred (Figure 4).
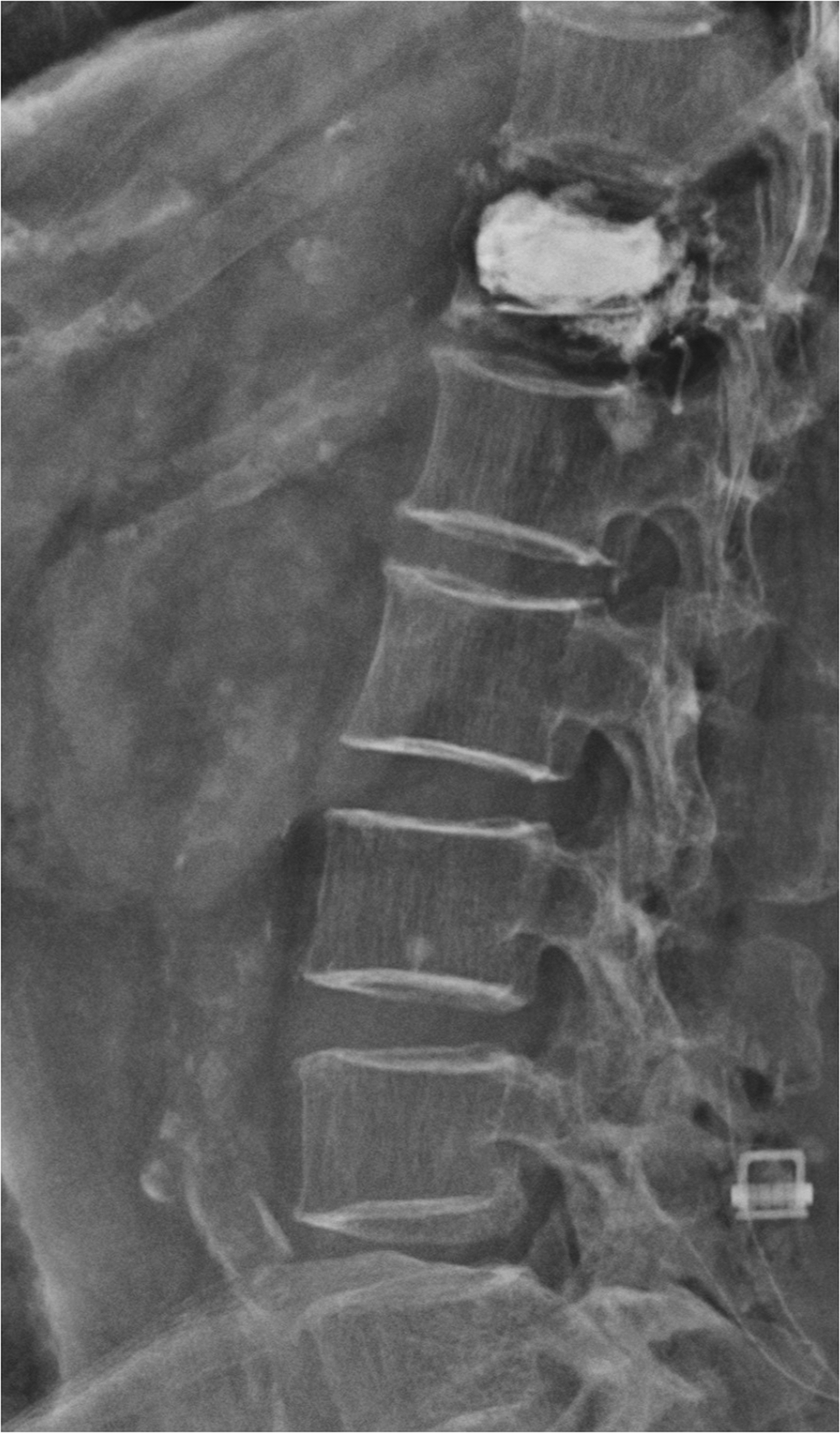
Case 2. One-year postoperative radiographs. No implant loosening or spinal structure fracture was noted in the images.
Discussion
Lumbar spinal stenosis is one of the most common degenerative changes in the aging population. 18 However, surgery should remain elective for older patients whose condition has not improved after conservative treatment. 19 Although fusion spinal surgeries are generally accepted for lumbar spinal stenosis, several complications have been reported, including ASD, massive trauma, excessive bleeding, extensive posterior column destruction of the spine, acquired spinal instability, and pseudarthrosis resulting in implant failure. The complication rate is as high as 33%.12,20 Thus, nonfusion spinal surgery has been developed to resolve these limitations.
Dynamic stabilization devices carry and balance the load between vertebrae while retaining the motor function of the fixed segments and reducing the influences of stress and movement of the adjacent segments. 12 Thus, ASD can be avoided or delayed. These devices are divided into two categories: interlaminar devices and interspinous devices. However, osteoporosis is another important issue among the aging population.
Dynamic stabilization using interspinous devices was historically unsuitable for patients with osteopenia or osteoporosis because of the theoretically increased risk of spinous process fractures. 21 In one cohort study, the rate of spinous process fractures was as high as 18% in patients who underwent Coflex® interspinous device placement. 21 Another study even suggested that Coflex® interspinous dynamic stabilization system implantation should be contraindicated in patients with osteoporosis. 22 However, whether the application of interlaminar devices, such as the IntraSPINE®, is suitable for patients with osteoporosis has seldom been investigated.
The IntraSPINE® device distracts the laminar space and restricts extension. 23 The IntraSPINE® is located close to the normal center of rotation, allowing more physiological movement without hindering extension compared with interspinous devices. 24 Thus, the IntraSPINE® can stop or reverse the progressive cascade associated with disc degeneration. 25 However, the efficacy and outcome of IntraSPINE® placement in patients with osteoporosis remain unknown.
In a controlled laboratory study, the lamina and inferior articular process contained the highest total BMD, thickest cortical shell, and largest percent volumes of cortical bone in a single vertebral unit. 5 With respect to complications, another study showed that spinal fracture only occurred in patients treated with interspinous devices and not in patients treated with interlaminar devices. 22 The precise position of the IntraSPINE® was within the two segments of lamina, which is the strongest bone structure in the vertebrae, giving the IntraSPINE® a higher success rate than other interspinous devices in patients with osteoporosis.
In this case report, we only investigated two patients with osteoporosis who underwent decompression and IntraSPINE® placement surgery. Further high-powered studies, such as case series that report more postoperative surgical outcomes, are necessary to obtain convincing evaluation findings. Additionally, the follow-up period (1 year) was relatively short. Thus, a longer observation period is required. Despite these limitations, this case report describes possible indications for nonfusion surgery with IntraSPINE® implantation in patients with osteoporosis. More standardized reporting of clinical, radiographic, and biomechanical outcomes would be clinically beneficial.
No spinal fracture occurred after the decompression and IntraSPINE® placement surgery in either patient described in this report. No ASD was observed 1 year postoperatively. With the alleviation of symptoms, the patients were satisfied with the surgical outcomes. Therefore, osteoporosis may not be an absolute contraindication for nonfusion surgery with IntraSPINE® placement. These successful cases should encourage surgeons to provide patients with more surgical treatment choices.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211049961 - Supplemental material for Application of the IntraSPINE® interlaminar device in patients with osteoporosis and spinal stenosis: two case reports
Supplemental material, sj-pdf-1-imr-10.1177_03000605211049961 for Application of the IntraSPINE® interlaminar device in patients with osteoporosis and spinal stenosis: two case reports by Kuei-Lin Yeh, Szu-Hsien Wu and Shing-Sheng Wu in Journal of International Medical Research
Supplemental Material
sj-pdf-2-imr-10.1177_03000605211049961 - Supplemental material for Application of the IntraSPINE® interlaminar device in patients with osteoporosis and spinal stenosis: two case reports
Supplemental material, sj-pdf-2-imr-10.1177_03000605211049961 for Application of the IntraSPINE® interlaminar device in patients with osteoporosis and spinal stenosis: two case reports by Kuei-Lin Yeh, Szu-Hsien Wu and Shing-Sheng Wu in Journal of International Medical Research
Footnotes
Author contributions
Conceptualization – Kuei-Lin Yeh, Shing-Sheng Wu
Data curation – Szu-Hsien Wu, Kuei-Lin Yeh
Formal analysis – Kuei-Lin Yeh, Szu-Hsien Wu
Funding acquisition – Szu-Hsien Wu, Shing-Sheng Wu
Investigation – Shing-Sheng Wu, Kuei-Lin Yeh
Methodology – Szu-Hsien Wu
Project administration – Szu-Hsien Wu
Resources – Shing-Sheng Wu
Software – Shing-Sheng Wu, Szu-Hsien Wu
Supervision – Shing-Sheng Wu, Kuei-Lin Yeh
Validation – Kuei-Lin Yeh
Visualization – Kuei-Lin Yeh
Writing – original draft – Kuei-Lin Yeh, Szu-Hsien Wu
Writing – review & editing - Kuei-Lin Yeh, Shing-Sheng Wu
Ethics approval
Both patients provided written informed consent for their surgical treatment and publication of their data. This study was approved by the institutional review board of Shin-Kong Wu Ho-Su Memorial Hospital, Taiwan (approval number: 20200708R) on 10 August 2020. The present study was conducted in accordance with the principles of the Declaration of Helsinki and reported in accordance with the CARE guidelines. 17
Data availability statement
The data used to support the findings of this study are available from the corresponding author upon request.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
