Abstract
Objective
The association of chronic non-malignant pain (CNP) with dyslipidemia is unclear. This retrospective study was performed to evaluate the association between CNP and dyslipidemia in elderly patients with femoral neck fractures (FNFs) treated by primary unilateral total hip arthroplasty (THA).
Methods
We retrospectively identified 521 consecutive patients with FNFs (AO/OTA type 31B) who underwent primary unilateral THA from 2009 to 2021. The study population was divided into patients with and without CNP. Serum lipids were measured for each patient. The association between CNP and dyslipidemia was assessed using a multivariate binary logistic regression model.
Results
In total, 436 patients (220 with CNP, 216 without CNP) were eligible for analysis. In the quantile regression, the adverse effect of CNP was significantly attenuated by resilience in patients with a high high-density lipoprotein (HDL) concentration and low low-density lipoprotein (LDL) concentration. The multivariate binary logistic regression model showed that the HDL and LDL concentrations were the only variables significantly associated with the development of CNP.
Conclusion
Both a low HDL and high LDL concentration may result in the occurrence of CNP in elderly patients with FNFs treated by primary unilateral THA.
Keywords
Introduction
Chronic non-malignant pain (CNP), which has a high prevalence and refractory nature, is typically characterized by hyperalgesia and has been linked to restrictions in daily activities, emotions, and quality of life.1–3 Moreover, severe CNP can shorten patients’ life expectancy. 3 Population-based estimates of CNP among Chinese elderly individuals range from 10% to 39% with significant subgroup differences.4,5 The increasing prevalence of CNP is attributable to demographic and lifestyle changes and is predicted to lead to a pronounced increase in the prescription of opioid analgesics for CNP, which has initiated escalating concern regarding the potential harms of these drugs.4,6,7 However, no clear consensus on population-wide CNP prevention or interventions has been established. 8 Although the high prevalence of CNP has led to increased interest in underlying CNP-related risk factors, no clear risk factors for CNP appear to have been identified to date.9,10 Epidemiological studies have demonstrated that dyslipidemia may be a risk factor for the occurrence and development of CNP.11–13 Additionally, CNP might be highly comorbid with dyslipidemia. 14 The lipid–pain relationship may be bidirectional15–17: dyslipidemia may lead to gain (sensitization) or loss (desensitization) of function relative to the incoming CNP signals, whereas CNP may conversely have a feedback effect on serum lipid levels.
Whether CNP and dyslipidemia have a positive correlation has been debated.2,15 Increases in serum lipids may be paralleled by an increase in the duration of CNP.4,16 Furthermore, the focus on normal serum lipid levels may underestimate the harms of CNP. 15 Notably, dyslipidemia may instigate or exacerbate CNP, potentially increasing the risk of CNP-related events.5,18 No lipid-related assessment of the risk of CNP in elderly patients with femoral neck fractures (FNFs) treated by primary unilateral total hip arthroplasty (THA) has been performed to date. We therefore performed a retrospective study to evaluate the association between CNP and dyslipidemia in such patients.
Materials and methods
Study population
This study was approved by the Investigational Ethics Review Board of Pu’ai Hospital, Tongji Medical College, Huazhong University of Science and Technology (IRB-07214), and the board granted an exemption from the requirement for informed consent because of the retrospective nature of the study. The reporting of this study conforms to the STROBE guidelines, 19 and all patient details have been de-identified.
Data for 521 consecutive patients with FNFs (AO/OTA type 31B) who had been treated by primary unilateral THA (cemented femoral component and standard-device acetabular component; Stryker Orthopaedics, Mahwah, NJ, USA) from March 2009 to January 2021 were retrospectively identified from the East China Hip Arthroplasty Database. CNP was defined as chronic pain that had developed or increased in intensity after the surgical procedure and persisted for 3 months after the surgery in accordance with the International Association for the Study of Pain guidelines. 1 THA was performed using a direct anterior approach. The key exclusion criteria were deficient baseline data, hypoesthesia (decreased response to a stimulus that is normally painful), 2 hyperalgesia, allodynia, cancer pain, nerve trauma, joint damage, gastric ulcers, endometriosis, diseases related to cholesterol metabolism, thyroid dysfunction, polytrauma, Paget’s disease, rheumatoid arthritis, and consumption of lipid-lowering medications.
Study endpoints
The primary endpoint was the association between CNP and dyslipidemia in elderly patients with FNFs treated by primary unilateral THA. Pain measurement was performed using a visual analog scale on the first day after surgery. Assessment of serum lipids was performed for each patient in both groups. Serum lipids included total cholesterol (TC), triglycerides (TGs), low-density lipoprotein (LDL), high-density lipoprotein (HDL), apolipoprotein A1 (apoA1), apolipoprotein B (apoB), apolipoprotein E4 (apoE4), leptin, and adiponectin. The blood samples were processed in accordance with the method described in previous reports.20,21 Dyslipidemia was defined as a TG concentration of ≥8.3 mmol/L, HDL concentration of ≤2.2 mmol/L, and LDL concentration of ≥8.9 mmol/L. 22
Statistical analysis
The serum lipid variables are expressed as mean ± standard deviation. Categorical variables were compared using the chi-square test or Fisher’s exact test, and continuous variables were compared using Student’s t-test for normally distributed data and the Mann–Whitney U test for non-normally distributed data. The primary analysis of the association between CNP and dyslipidemia was performed using a multivariate binary logistic regression model. All analyses were performed using IBM SPSS Statistics for Windows, Version 26.0 (IBM Corp., Armonk, NY, USA). The level of significance was set at p < 0.05 for all statistical analyses.
Results
In total, 521 elderly individuals with FNFs who had been treated by primary unilateral THA and had available baseline data were included in the study. Eighty-five patients did not meet the study criteria, and the remaining 436 patients were analyzed as shown in Figure 1. The study population was divided into patients with CNP (Group CP, n = 220) and patients without CNP (Group NC, n = 216). The median age was 67.74 years (range, 61–73 years) in the CP group and 67.65 years (range, 61–74 years) in the NC group with no significant difference. In the baseline data on serum lipids, we found significant differences in leptin, adiponectin, TC, HDL, LDL, TGs, apoE4, and apoE genotype (p < 0.001). The mean leptin, adiponectin, LDL, TG, and apoE4 carrier values were considerably higher in the CP group than in the NC group (p < 0.001), and the mean TC and HDL values were significantly lower in the CP group than in the NC group (p < 0.001). A significant difference was also detected in the apoE genotype (p < 0.001). No significant differences were detected in the remaining baseline data, as shown in Table 1.
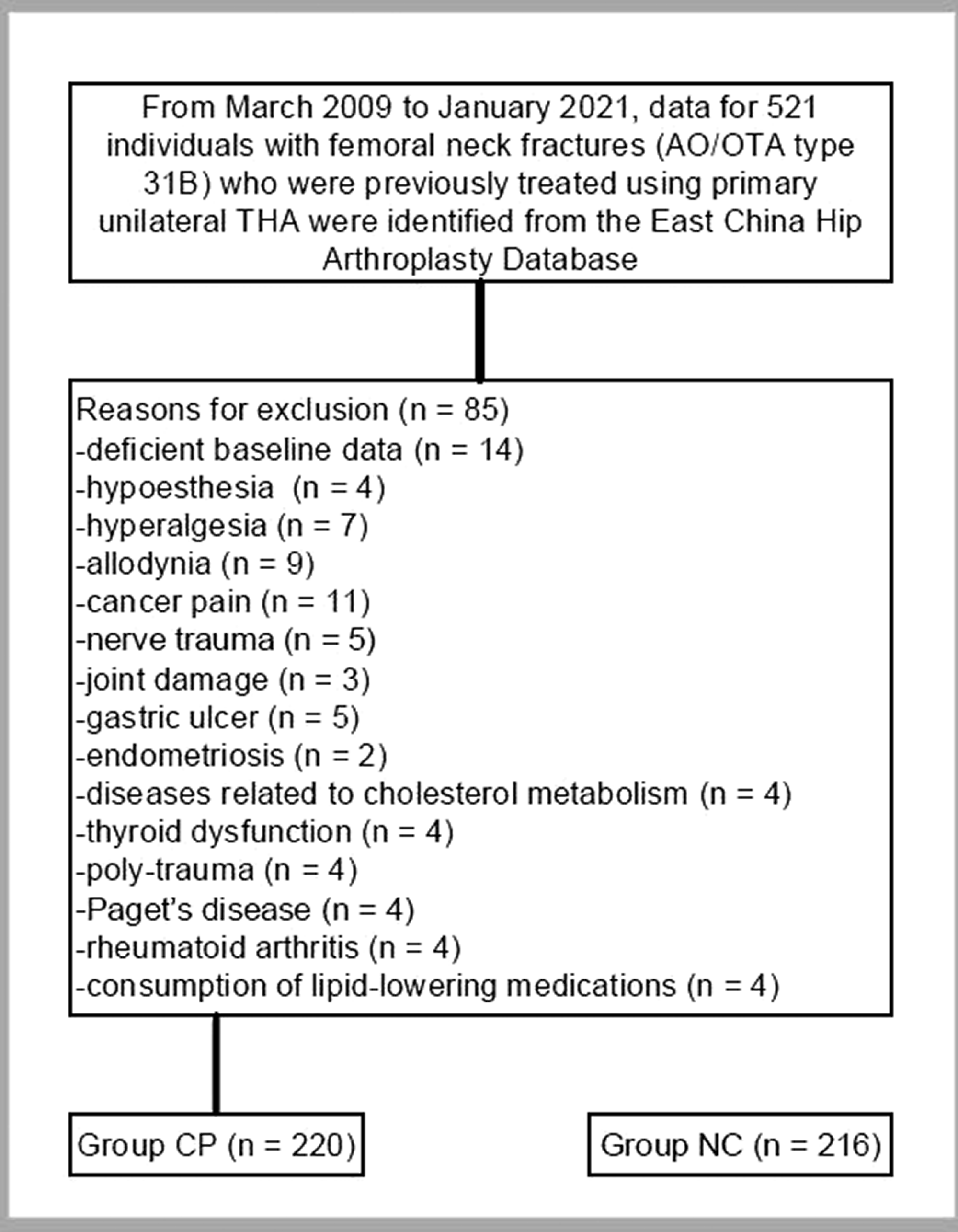
Flow diagram demonstrating selection of patients for evaluation of the association between chronic non-malignant pain and dyslipidemia in a cohort of elderly individuals with femoral neck fractures treated by primary unilateral total hip arthroplasty, and reasons for exclusion
Patient demographics
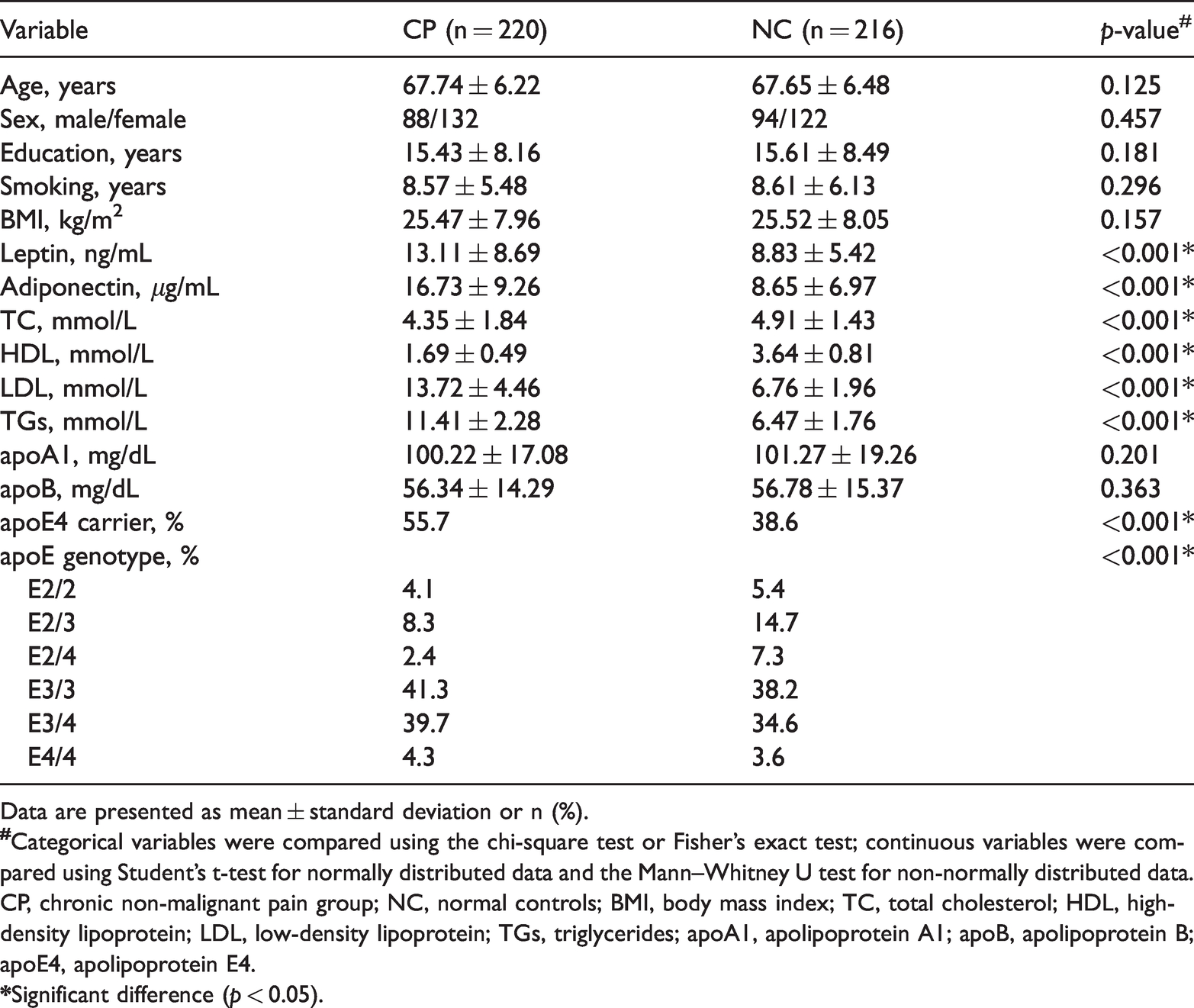
Data are presented as mean ± standard deviation or n (%).
CP, chronic non-malignant pain group; NC, normal controls; BMI, body mass index; TC, total cholesterol; HDL, high-density lipoprotein; LDL, low-density lipoprotein; TGs, triglycerides; apoA1, apolipoprotein A1; apoB, apolipoprotein B; apoE4, apolipoprotein E4.
Table 2 shows the results of the multivariate binary logistic analysis of factors associated with CNP in this cohort of elderly patients with FNFs treated by primary unilateral THA. Age, education, smoking, and body mass index were not involved in this analysis. In the quantile regression, the adverse effect of CNP was significantly attenuated by resilience in patients with a high HDL concentration (p = 0.003) and low LDL concentration (p = 0.001). This effect appeared to be mainly driven by the high HDL and low LDL. The multivariate binary logistic regression model showed that the HDL and LDL concentrations were the only variables associated with the development of CNP (odds ratio, 7.08; 95% confidence interval, 4.30–8.72; p < 0.001 and odds ratio, 6.51; 95% confidence interval, 3.93–7.48; p < 0.001, respectively). Other variables (leptin, adiponectin, TC, apoA1, apoB, TGs, apoE4, and apoE genotype) were not associated with CNP in the present analysis.
Multivariate binary logistic regression analysis of factors associated with chronic non-malignant in the present cohort of elderly patients with femoral neck fractures treated by primary unilateral total hip arthroplasty

CI, confidence interval; TC, total cholesterol; TGs, triglycerides; LDL, low-density lipoprotein; HDL, high-density lipoprotein; apoA1, apolipoprotein A1; apoB, apolipoprotein B; apoE, apolipoprotein E
Discussion
This retrospective study may provide evidence that both a high LDL and low HDL concentration are strongly associated with the occurrence of CNP in elderly patients with FNFs treated by primary unilateral THA. Both a high LDL and low HDL concentration may be the primary risk factors for CNP in most patients. Measurement of serum lipids may be particularly important for elderly patients with CNP. Both a low LDL and high HDL concentration may have a favorable benefit–risk profile for the prevention of CNP, but the consumption of lipid-lowering drugs may be increased in patients with both a high LDL and low HDL concentration.
A series of clinical aggravations attributed to high-impact CNP have been frequently mentioned in published reports.3,23 These aggravations have indisputably become important factors restricting patients’ daily activities. 3 In the present study, both a high LDL and low HDL concentration tended to be robust predictors of CNP. However, we detected little evidence of a temporal relationship between the occurrence of CNP and the presence of dyslipidemia, and we found no evidence that the occurrence of CNP can further aggravate dyslipidemia. CNP is usually recognized to arise from altered neuronal activity that is associated with a heightened perception of pain (peripheral and/or central sensitization).4,15,24 An elevated cholesterol level or hyperlipemia (a high LDL level in particular) may be an important risk factor for the occurrence of CNP.10,15 Dyslipidemia is associated with an increased risk of the development of atherosclerosis. 25 Several studies have demonstrated that atherosclerosis promotes neuronal degeneration or neurotransmitter synthesis disorder,26,27 which leads to a disorderly increase in lipid metabolites (such as oxidized lipids). The accumulation of oxidized lipids in the microvasculature stimulates the local release of inflammatory mediators, 28 which can directly initiate and accelerate sensitization of pain-sensing nociceptors located at functional afferent neurons. 29
Previous studies of CNP tended to underrate serum lipids among elderly individuals, focusing instead on the management of high-impact CNP.14,24 Recent studies have shown that dyslipidemia may be one of the most important contributors to CNP,30,31 and even more recent studies have revealed that the plasma lipidomic profile is associated with CNP.32,33 However, the role of dyslipidemia in the occurrence and development of CNP remains controversial. 18 A few studies regarding the effect of dyslipidemia on CNP have shown that hydroxymethylglutaryl-coenzyme A (HMG-CoA) reductase inhibitors (such as atorvastatin) can competitively inhibit the conversion of HMG-CoA to mevalonic acid.34,35 Although HMG-CoA reductase inhibitors represent an encouraging opportunity to improve the management of CNP, 34 clinical application is limited and few products appear to be in use for CNP. 10 In 2013, Pathak et al. 36 assessed the antihyperalgesic and anti-inflammatory effects of atorvastatin in a chronic constriction injury model of neuropathic pain in rats. The results showed that atorvastatin tends to be a supplementary therapeutic option in treating neuropathic pain. In 2014, Pathak et al. 37 further evaluated the effect of atorvastatin on oxidative stress and hyperalgesia in a chronic constriction injury model of neuropathic pain in rats. The results demonstrated that atorvastatin attenuates neuropathic pain by down-regulating oxidative damage at peripheral levels. Analogously, Ala et al. 14 investigated the efficacy of atorvastatin in reducing postoperative pain in 66 patients who underwent open hemorrhoidectomy in a randomized, placebo-controlled trial. The results demonstrated that atorvastatin reduces postoperative pain and decreased opioid requirements compared with placebo. Based on comparable scenarios, several other studies have revealed that dyslipidemia is apt to instigate the occurrence of CNP and that the onset of dyslipidemia is significantly associated with the duration and extent of CNP.13,16,38
Dyslipidemia is involved in the evolution of CNP. 24 In this process, oxidized lipids frequently inhibit or interrupt the normal nerve signal transmission pathway, triggering the enhancement of neuronal feedback and promoting the excessive release of neurotransmitters; this eventually leads to the establishment of abnormal signal transmission pathways and the occurrence of CNP.28,29 However, CNP further induces the release of inflammatory mediators, which further aggravates or worsens dyslipidemia and finally leads to breakdown of the lipid metabolic balance.28,39 Dyslipidemia plays a key role in this vicious circle. This is primarily because dyslipidemia can not only directly trigger the release of neurotransmitters but also promote the explosive release of inflammatory factors through the immune response.15,16
The results of this retrospective study should be interpreted in light of several key limitations. First, the retrospective nature of the study and the exclusion criteria somewhat limit our ability to draw reliable conclusions. Second, the sample size was relatively small, restricting the estimation of consistent conclusions. Replication of the study with a larger sample size appears to be necessary. Furthermore, several subjective outcome measures (such as age, education, and smoking) were included in the study, and subjective self-assessment could result in potential reporting bias. Third, some comorbidities were not involved when evaluating the baseline data. Fourth, stratification of dyslipidemia was not performed in this study, which may have introduced a deviation. Fifth, the lack of generalizability is inevitable because our study population comprised elderly patients, the direct anterior approach was used for THA in all patients, and strict exclusion criteria were applied. Finally, although our study followed the general principles of research and the factors influencing CNP were multifaceted, involving both laboratory and non-laboratory parameters (i.e., duration of the operation, surgical approach), these factors are relatively fixed, and interventions for dyslipidemia may have a certain impact on the outcome of CNP.
In conclusion, the results of this retrospective study reveal that both a low HDL and high LDL concentration tend to be associated with the occurrence of CNP in elderly patients with FNFs treated by primary unilateral THA. This implies that dyslipidemia may be involved in the occurrence of CNP in these elderly patients. Given the retrospective nature of this study and the small sample size, future large-sample randomized controlled studies are needed to determine whether such a relationship exists.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211045224 - Supplemental material for Association of dyslipidemia with chronic non-malignant pain in elderly patients with femoral neck fractures treated by primary total hip arthroplasty: a retrospective study
Supplemental material, sj-pdf-1-imr-10.1177_03000605211045224 for Association of dyslipidemia with chronic non-malignant pain in elderly patients with femoral neck fractures treated by primary total hip arthroplasty: a retrospective study by Chen Wang, Bo Xu, Pengfei Wang, Weiguang Yu, Xianshang Zeng, Nana Xiong, Pingping Yin, Qilong Liu and Huanyi Lin in Journal of International Medical Research
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
