Abstract
Objective
To implement a psychological intervention programme and explore its effects on anxiety and depression in patients with severe urinary incontinence following radical prostatectomy.
Methods
This pilot randomized controlled trial recruited patients that underwent laparoscopic radical prostatectomy. Patients were randomized to conventional nursing and psychoeducation groups. The primary outcome was the levels of anxiety and depression evaluated by the self-rating anxiety scale (SAS) and self-rating depression scale (SDS) at 3 months after urinary catheter removal. The quality of life (secondary outcome) was evaluated using the incontinence-specific quality of life scale (I-QOL).
Results
The study analysed 35 patients: 16 received conventional nursing and 19 received a psychoeducational intervention. There were no significant differences in the sociodemographic data and SAS, SDS and I-QOL scores between the two groups at baseline. At 3 months after catheter removal, the SAS and SDS scores in the psychoeducation group were significantly lower compared with the conventional nursing group; and the I-QOL score in the psychoeducation group was significantly higher compared with the conventional nursing group.
Conclusion
This pilot study suggests that the psychological nursing intervention improved the symptoms of anxiety and depression, and improved quality of life, in patients with severe urinary incontinence following radical prostatectomy.
Introduction
Prostate cancer (PC) is the most common malignancy of the male reproductive system. 1 The incidence of PC ranks second among the malignant tumours in males worldwide and it ranks sixth regarding the causes of death. 2 China has a low incidence of prostate cancer, but in recent years, with the aging of the population and changes in life style, the incidence rate has shown a rapid growth trend. 3
Radical prostatectomy is the gold standard treatment for localized prostate cancer, but it is associated with complications such as urinary incontinence, which has non-negligible impacts on the survivor’s quality of life.4,5 The prevalence of urinary incontinence after radical prostatectomy is 4–31%, 6 and the occurrence is related to the clinical features of PC, intraoperative injuries, surgical methods and experience of the surgeons.7,8 Currently, there are no absolute preventive measures and treatments.7,8Urinary incontinence is not only associated with urinary tract infection, skin eczema, ulceration and other physiological problems, but it also causes psychological distress such as feelings of loss, uncertainty in illness, stigma, detrimental effects on quality of life, reduced patient confidence in their treatment, and changes to their self-attitude, which can lead to pessimism, irritability and self-imposed isolation. 9 Urinary incontinence may also hinder physical and mental rehabilitation after prostatectomy. 10
The active prevention of postoperative urinary incontinence, accelerating the postoperative recovery of urinary control, helping pain relief and improving the quality of life of patients are crucial features of patient management after prostatectomy. 11 Nevertheless, most of the current studies focus on the physiological level (such as pelvic floor muscle training and bladder function training),12–14 with few studies examining psychological nursing interventions; 13 and those interventions that have been evaluated were relatively limited and lacked a systematic approach, diversity and continuity.15–17 Most studies on psychological interventions for urinary incontinence have been for women with stress or postpartum incontinence,18,19 and they have little pertinence and applicability for men with urinary incontinence after prostatectomy.
Therefore, designing new interventions for the management of urinary incontinence after prostatectomy is important to improve the quality of life and mental health of survivors after PC. The purpose of this pilot study was to design and implement a psychological intervention programme and explore its effects on anxiety and depression in patients with severe urinary incontinence after prostatectomy.
Patients and methods
Patients
This randomized controlled trial enrolled patients that underwent laparoscopic radical prostatectomy between June 2015 and December 2017 in the Department of Urinary Surgery, First Affiliated Hospital of Anhui Medical University, Hefei, Anhui Province, China. The inclusion criteria were as follows: (i) diagnosis of PC based on the histology results from a biopsy performed using the transrectal ultrasound-guided prostate 13-00 system; (ii) basic communication and literacy skills in Chinese; (iii) voluntarily participated in the study and signed the informed consent form; (iv) prostatectomies performed by the same three experienced surgeons at The First Affiliated Hospital of Anhui Medical University; (v) severe urinary incontinence after removing the urinary catheter; 9 (vi) did not receive any drug treatment for urinary incontinence after surgery. The exclusion criteria were as follows: (i) past history of prostate surgery; (ii) past history of urinary incontinence; (iii) neoadjuvant endocrine therapy or radiotherapy; (iv) uncontrolled diabetes mellitus, coronary heart disease or hypertension; (v) distant metastasis; (vi) urinary incontinence caused by reasons other than prostatectomy.
The study was approved by the Ethics Committee of The First Affiliated Hospital of Anhui Medical University (no. 81630019). Each patient provided written informed consent.
Randomization and intervention
During the screening process, the degree of urinary incontinence (mild, moderate or severe) was determined according to the International Continence Society definition, 9 based on routine examination. Patients with severe incontinence were randomly divided into the psychoeducation and conventional nursing groups by an independent statistician using a random number table.
The patients in the conventional nursing group received a routine nursing intervention, which included communication, health education during the perioperative period, guidance about functional exercise before and after removing the urinary catheter, health education after discharge, arranging regular re-examinations and telephone follow-up (including nursing for daily life, psychological counselling [focus on assets and strengths, person–environment interactions, educational and career development, brief interactions, and a focus on intact personalities], pelvic floor muscle training methods, and bladder function training methods).
In addition to the basic routine nursing care, as provided in the conventional nursing group, the patients in the psychoeducation group were given an intervention by a team consisting of an attending physician and a head nurse, a postgraduate nursing student, a senior nurse from the Department of Urinary Surgery (nurse-in-charge, >10 years of experience) and two nurses with an intermediate professional qualification. The physicians were responsible for the surgery and postoperative ward rounds, and for the management of any medical condition arising from the surgery. The patients in the psychoeducation group received the same routine nursing and health guidance as in the conventional nursing group. In addition, the senior nurse was responsible for the patients’ postoperative rehabilitation, active care and surveillance, communication with the patients and their family members, listening to their complaints, and to actively manage the problems and issues. The assessment of the patients’ acceptance of health guidance and functional exercise was performed in real-time and appropriate corrections were performed using oral, written, picture and video instructions. The patients and their families were instructed to learn relaxation therapy in advance. The patients’ family members were encouraged to participate in supervision and help training, thus establishing a relationship of trust with the patients and their family members to ensure the smooth progress of the psychological nursing intervention.
In addition to the basic routine nursing care provided after removing the urinary catheter, a variety of ways was adopted to conduct bedside guidance to strengthen the understanding of the patients and their families on the nursing of urinary incontinence and recovery of urinary control. At the moment of removing the urinary catheter, the patients were guided to perform relaxation exercises, which were learned in advance, prior to surgery, at each patient's convenience (individually or in a group). After the removal of the catheter, the patients were followed over the telephone once a week (5–15 min/call), which could be extended or shortened according to the patient's wishes. The purpose of follow-up was to listen to the patients, understand their existing problems and needs, inform them of coping methods, comfort them, and point out the adverse effects of anxiety, depression, and other negative emotions on incontinence and health in general. All members of the nursing team participated in the group psychological nursing intervention, which was conducted every month (2 h/session, for 3 months) to follow the patients’ rehabilitation status, to strengthen health education and to promote peer support. The specific meeting plan is presented in Table 1. Finally, family members were encouraged to participate in the psychological nursing intervention of patients. Family members were informed about the psychological problems that the patients might have. Family members were encouraged to communicate, discuss, consult, interact (role playing) and support.
Plan for the group intervention in the psychoeducation group.

The head nurse was responsible for organization and leadership. The attending physician was responsible for teaching and answering questions. The senior nurse was responsible for controlling the atmosphere and maintaining discipline. The postgraduate nursing student served as a secretary, was responsible for meeting minutes and arrangement, and reminded the patients to attend 1 day before the meeting, over the telephone.
For patients developing severe urinary incontinence after removing the urinary catheter, the baseline mental state was first assessed by conducting a one-to-one interview with the patient to understand their families and social and cultural background, and to assess the psychological condition due to the occurrence of severe urinary incontinence.
Data collection and outcome measures
Demographic and socioeconomic data, including age, ethnicity, education level, marital status, primary caregiver, occupation, religious belief and income were collected using a uniform structured questionnaire by trained nurses.
The primary outcome was the levels of anxiety and depression in patients with severe urinary incontinence at 3 months after removal of the urinary catheter. The secondary outcome was quality of life in patients with severe urinary incontinence at 3 months after removal of the urinary catheter. The levels of anxiety were assessed using the Zung self-rating anxiety scale (SAS) and the levels of depression were assessed using the Zung self-rating depression scale (SDS). 20 The quality of life in patients with severe urinary incontinence was evaluated using the incontinence-specific quality of life scale (I-QOL). 12
The SAS includes 20 questions that are evaluated using a 4-point Likert scale (1 = never or rarely and 4 = most of the time). Reverse scoring was used in some entries. The total score was multiplied by 1.25 and the integer was taken as the standard score. A standard score of 50–60 indicated mild anxiety, 61–70 indicated moderate anxiety and >70 indicated severe anxiety.20,21
The SDS includes 20 questions that are evaluated using a 4-point Likert scale. Reverse scoring was used in some entries. The total score was multiplied by 1.25 and the integer was taken as the standard score. A standard score of 53–62 indicated mild depression, 63–72 indicated moderate depression and >72 indicated severe depression.20,21
The I-QOL includes 22 questions about restrictive behaviour, psychosocial impact, and social barriers, which are evaluated using a 5-point Likert scale. The higher the score, the better the patient's quality of life. The Cronbach’s α coefficient of the scale was 0.93 and the reliability was good. 22 The questionnaires have been validated in Chinese.23–25
Safety
Potential adverse events (e.g. pain, nausea and breathlessness) related to the surgery, to the nursing intervention, or to neither, were recorded using standardized logs. Adverse events reported spontaneously by the patient or observed by therapists were also recorded.
Statistical analyses
All statistical analyses were performed using IBM SPSS Statistics for Windows, Version 23.0 (IBM Corp., Armonk, NY, USA). Descriptive statistics included mean ±SD and
Results
This randomized controlled trial screened 188 patients. According to the diagnostic criteria for urinary incontinence, 9 103 patients had mild urinary incontinence, 45 had moderate urinary incontinence and 40 had severe urinary incontinence. The 40 patients with severe urinary incontinence were enrolled and randomized. There were 18 patients in the conventional nursing group with a mean ± SD age of 70.4 ± 5.2 years. There were 22 patients in the psychoeducation group with a mean ± SD age of 72.8 ± 5.2 years. There was no significant difference in age between the two groups.
In the psychoeducation group, one patient withdrew because of improvements in urinary symptoms and two patients were excluded because they were unable to regularly participate in the intervention, which resulted in 19 patients completing the psychoeducation intervention. In the conventional nursing group, one patient withdrew because of physical discomfort and another patient was excluded due to repeated failure to attend follow-up. Figure 1 presents the patient flowchart. Table 2 presents the demographic and socioeconomic characteristics of the patients in both groups at baseline.
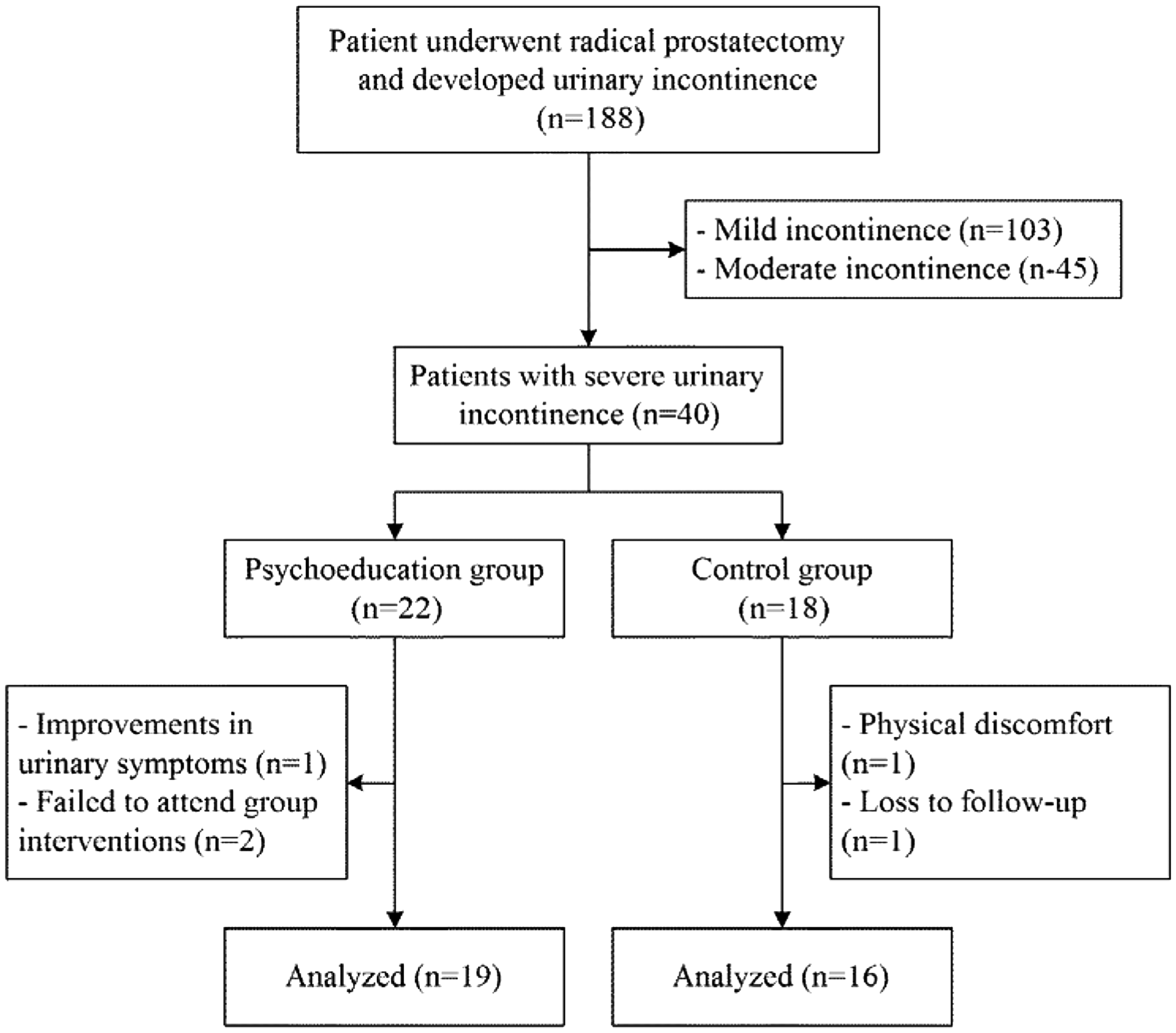
Patient flowchart showing the flow of patients through this randomized controlled trial to evaluate a psychoeducation intervention for severe urinary incontinence following prostatectomy.
Baseline demographic and socioeconomic characteristics of the patients (

Data presented as mean ± SD or
No significant between-group differences (
SAS, self-rating anxiety scale; SDS, self-rating depression scale; I-QOL, incontinence quality of life scale.
There were no significant differences in the baseline SAS, SDS and I-QOL scores between the two groups immediately after the removal of the urinary catheter (Table 2). At 3 months after removal of the urinary catheter, the SAS and SDS scores (primary outcome) in the psychoeducation group were significantly lower compared with the conventional nursing group (
The SAS, SDS and I-QOL scores at 3 months after removal of the urinary catheter in patients (

Data presented as mean ± SD.
aBetween-group comparison; independent sample
SAS, self-rating anxiety scale; SDS, self-rating depression scale; I-QOL, incontinence quality of life scale.
Discussion
Radical prostatectomy is the main treatment for PC, but surgical injury to the external sphincter muscle of the urethra and the urinary incontinence caused by the paraprostatic neurovascular bundle are the most common postoperative complications.4,5Although postoperative urinary incontinence does not endanger the life of patients, it profoundly affects their quality of life.4,5 Psychological interventions have been studied in women,18,19 but few data are available regarding psychological interventions for urinary incontinence after prostatectomy. 26 Therefore, this current randomized pilot study aimed to design and implement a psychological intervention programme and to explore its effects on anxiety and depression in patients with severe urinary incontinence after prostatectomy. The current results showed that the psychological nursing intervention improved the symptoms of anxiety and depression in patients with severe urinary incontinence after radical prostatectomy, which improved their quality of life. This current intervention could help increase patient satisfaction. Even if studies in male patients with urinary incontinence are lacking, similar psychoeducational approaches have been used in a variety of diseases with success.27–30
Patients with severe urinary incontinence generally suffer from anxiety and depression. 9 The possible causes include physiological, psychological and social aspects. Indeed, urinary incontinence changes the original physiological balance of the patients, leading to restriction of drinking water intake, poor sleep quality, sexual disorder, skin eczema and ulceration, which reduces the comfort and satisfaction with life of the patients, and further aggravates their anxiety and depression in a vicious cycle.22,31 In addition, urinary incontinence brings serious psychological distress and economic pressure to both the patients and their family, and the patient experiences a sense of loss and stigma. 26 Self-control of urination cannot be recovered quickly after surgery, leading to irritability, worry, and uncertainty in illness, and some patients even regret having undergone the surgical treatment. 32 All of these negative emotions can further aggravate the psychological distress, affecting daily life and resulting in a vicious cycle of negative feelings. 32 Furthermore, after the removal of the urinary catheter, urine overflow causes inconvenience and trouble, and the patients often feel that their body is unclean, even fearing that their body odour will lead them to be discriminated against. 12 Therefore, patients have a sense of shame and inferiority, often reducing their daily activities and social communication, leading to loneliness, lack self-confidence and self-efficacy, and their interest in the outside world is decreased, which further results in anxiety and depression. 33 At the same time, shame and embarrassment can prevent patients from seeking medical treatment, which affects their rehabilitation. 34 In the present study, the SAS and SDS were not assessed before prostatectomy because the patients were screened based on the presence of urinary incontinence after removing the urinary catheter. Even if some patients had anxiety and depression before prostatectomy, the present study still showed that the psychoeducation intervention resulted in better improvements in anxiety, depression and quality of life compared with conventional nursing.
Research has shown that negative emotions easily strengthen the patient's sensitivity to pain, touch, and temperature, and aggravate the symptoms of urinary incontinence. 35 On the other hand, maintaining a positive and optimistic attitude and seeking social support can be beneficial to patients, helping them to adopt a positive coping style, which could promote tolerability toward urinary incontinence. 36 The present study strongly suggests that a supportive psychological nursing intervention could mitigate some of the negative emotions involved in anxiety and depression and improve the quality of life of patients with severe urinary incontinence after radical prostatectomy. The psychoeducation intervention used a variety of psychological nursing interventions. Among them, the intervention helped the patients establish a correct understanding of urinary incontinence. Patients often feel self-abased, ashamed, disappointed, isolated, helpless and uncertain about the future because of urinary incontinence. Therefore, medical staff need to do a good job in health education, so that the patients can have a correct understanding of the operative principles, advantages and disadvantages, causes and outcomes of urinary incontinence. The nurses play a key role in the management of urinary incontinence because they are more available than physicians and develop a better trust relationship with the patients. During the nursing process, they will help the patients understand and manage urinary incontinence correctly; and tell them that urinary incontinence is a common phenomenon after prostatectomy and most of it is temporary, and that it can be gradually improved with time and human effort. The nurses will teach the patients the methods of managing urinary incontinence, such as wearing a condom catheter and using and replacing urine pads, which improve the patient and family's sense of control of the disease.37,38Another important aspect of the psychoeducation intervention provided by the nurses was to make the patients obtain psychological support and persuasion. The nurses helped patients develop positive attitudes through psychological counselling, including talking and listening to them, feeling their experience, and helping lighten their burden. Guiding the patients on how to divert attention away from the disease by relaxation, listening to light music, meditation and maintaining a happy mood was also important. The psychological intervention was also combined with training of pelvic floor muscles and bladder function. In the process of training the patient's consciousness during urination, the patients were encouraged, their self-confidence was praised, and the conditional reflex of urination was gradually established and strengthened. In addition, family support and peer support also effectively promoted the patient's return to family and society. In the era of personalized medicine, achieving targeted and individualized intervention is an important aspect. Providing individualized services to patients could ultimately help patients improve their quality of life and the patients feel less let down by the healthcare system, improving their positive feelings. 16 Because of the range of patient conditions, cultural backgrounds and character traits, patients' attitudes toward urinary incontinence, coping styles and psychological reactions are different from one patient to another. In this current study, the mental state of patients was assessed before surgery and personal files were established. According to the physiological status of the different patients after surgery, the patients were guided to carry out skin care and to select the appropriate nursing supplies. The nurses helped the patients plan daily activities, regularly carried out follow-up by telephone and group discussion, and encouraged each patient for self-disclosure. Taken together, this package of nursing interventions helped relieve the anxiety and depression of patients with severe urinary incontinence and improved their incontinence-related quality of life.
The present study had several limitations. First, the sample size was small because only patients with severe urinary incontinence after radical prostatectomy were included. The mean age of the patients in this study was about 71 years; they were elderly and their compliance was poor. When implementing the group psychological nursing intervention, two patients complained about the number of visits and even gave up the psychological guidance. The communication process over the telephone needed repeated communication to confirm information, which caused a certain burden to both the patients and the interviewer. The study did not aim to intervene on patients with diagnosed anxiety or depression, but to observe whether the intervention could decrease the levels of anxiety and depression symptoms. Therefore, the study examined the changes in the scores, but not changes in diagnoses. The clinical significance of this pilot study is limited, but improvements in SAS and SDS scores could have long-term impacts on the quality of life of patients and possibly on the development of anxiety and depression, but future studies will have to examine this issue. Finally, this study only included patients with severe urinary incontinence, hence limiting the generalizability of the results. Future research will consider cooperating with community care services in order to instruct and entrust community doctors and/or nurses to adopt one-to-one home visits.
In conclusion, this pilot study demonstrated the positive effects of a psychological nursing intervention on the symptoms of anxiety and depression of patients with severe urinary incontinence after radical prostatectomy. The psychological nursing intervention helped patients to overcome psychological barriers, alleviate anxiety and depression, and improve their quality of life. This type of intervention could have important clinical implications in the future.
Footnotes
Acknowledgement
The authors acknowledge the invaluable contribution of the study participants.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This study was funded by the National Key Clinical Specialty Construction Project (2012), General Programme of the National Natural Science Foundation Project of China (no. N81370856), the first batch of science and technology projects in Anhui China in 2017 (no. 1704a0802173) and the Fund for the humanities and social sciences of colleges and universities of the Anhui Provincial Department of Education (no. SK2017A0171).
