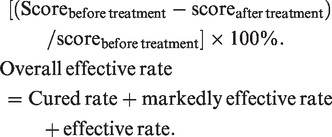Abstract
Objective
The aim of this study was to evaluate the therapeutic effects of transcutaneous electrical nerve stimulation (TENS) on opioid-induced constipation (OIC) and patient quality of life.
Methods
A total of 251 patients were randomly allocated to a treatment group, who received TENS and oral lactulose solution (n = 124), and a control group, who received only oral lactulose solution (n = 127). Constipation and quality of life after treatment were measured by comparing semiquantitative scores based on subjective symptoms.
Results
The defecation difficulty, incomplete defecation feeling, and overall defecation satisfaction scores of the treatment group were significantly different from those of the control group (P = 0.018). Bowel Function Index and quality of life scores of the treatment group were significantly greater than those of the control group. The effective rates of control and treatment groups were 85.8% and 91.9%, respectively.
Conclusion
TENS of relevant acupuncture points significantly relieved the clinical symptoms of constipation of patients with OIC and improved their quality of life.
Keywords
Introduction
In 1986, the World Health Organization (WHO) proposed a three-step analgesic ladder that incorporated the use of opioids for moderate-to-severe cancer pain; 1 26 years later, the European Association for Palliative Care still recommended opioids as the primary therapy for moderate-to-severe cancer pain based on medical evidence. 2 The WHO three-step analgesic ladder has been extensively recognized and used worldwide.3,4 However, the incidence rate of opioid-induced constipation (OIC) is 90%, and long-term administration can lead to side effects that substantially affect quality of life 5 and lead to poor compliance.
Opioids exert their pharmacological and physiological effects by binding to their endogenous receptors to modulate nerve conduction. 6 The opioid system also exerts analgesic effects by affecting central nervous system sites. 7 However, the combination of opioids and µ-opioid receptors in the gastrointestinal tract hinders gastrointestinal motility, prevents gastric emptying, inhibits the secretion of bile and gastric juices, suppresses faecal excretion and leads to constipation.8–10
The National Comprehensive Cancer Network guidelines recommend that prescription opioids be administered in combination with prescription laxatives to prevent and treat constipation. 11 Regardless, OIC remains troublesome during cancer pain treatment. OIC is characterized by continuous constipation throughout administration, which, if not promptly controlled, severely affects the mood, quality of life and treatment of patients. In extreme cases, patients may die of paralytic ileus. Accordingly, constipation should be prevented and treated. Therefore, we assessed the therapeutic effects of transcutaneous electrical nerve stimulation (TENS) for patients with OIC to determine if this treatment could improve their quality of life.
Material and methods
Study population
Participants were constipated patients with moderate-to-severe cancer pain, who were hospitalized and receiving oral administration of opioids (controlled-release oxycodone hydrochloride tablets and morphine tablets) in Zhejiang Cancer Hospital, China, from January 2013 to June 2016. Two experienced pathologists separately diagnosed pathological sections and the degree of differentiation for adult cancer patients aged ≥18 years admitted to our hospital. Patients’ cases were reviewed if both pathologists diagnosed advanced malignant tumours, and patients with moderate-to-severe cancer pain (treated with oxycodone hydrochloride sustained-release tablets and morphine tablets for pain relief and constipation) and their families were interviewed. Patients and interviewed family members provided written informed consent.
Patients were randomized into two treatment groups using a random number table.
The study protocol was approved by the Medical Ethics Committee of Zhejiang Cancer Hospital, Hangzhou, Zhejiang Province, China (No. 2014-09-86). The study was conducted in accordance with the principles of the Declaration of Helsinki.
Diagnostic criteria
Patients were diagnosed according to the constipation diagnostic criteria of Wang’s (2007) text ‘Internal Medicine of Traditional Chinese Medicine’ 12 and the OIC diagnostic criteria of the American Multidisciplinary Panel. 13
Wang’s (2007) constipation diagnostic criteria are as follows: prolonged defecation time (defecation interval of 48 hours, or defecation frequency less than three within 1 week); dry and hard rod-like or granular faeces; defecation difficulty complicated with acute lower abdominal distension; fatigue, weakness and appetite reduction.
The OIC diagnostic criteria of the American Multidisciplinary Panel are as follows: use of opioids for more than 1 week; independent defecation frequency of less than three per week; and difficult, incomplete and dry defecation.
Criteria for pain intensity scoring
Pain intensity was scored using a numerical rating scale (NRS): 14 0 points: painlessness; 1 to 3 points: mild pain that does not affect normal work or sleep; 4 to 6 points: moderate, hardly bearable pain that disturbs sleep, requiring administration of analgesics; 7 to 10 points: severe pain that may be complicated with autonomic nerve function disorder and seriously disturbs sleep, and for which analgesics must be used. Patients chose the score that best represented their pain intensity.
Inclusion and exclusion criteria
The inclusion criteria were as follows: patients 1) with malignant tumours and an expected survival time of over 3 months based on pathological diagnosis, in accordance with the Rome III diagnostic criteria for functional constipation; 15 2) with moderate-to-severe pain (average NRS score of >4 points 24 hours before enrolment); 3) who had received oral administration of opioids to relieve pain; 4) who were aged ≥18 and ≤75 years; 5) with an Eastern Cooperative Oncology Group score of ≤2 points; 6) who understood the study aims and procedure and had provided written informed consent.
The exclusion criteria were as follows: patients with 1) anoxic respiratory depression, cardiocerebral dysfunction or severe hepatic and renal insufficiency; 2) history of drug abuse or antidepressant administration; 3) patients with acute abdominal pain and intestinal obstruction as disclosed by abdominal plain film.
Treatment methods
All patients received oral administration of controlled-release oxycodone hydrochloride tablets in combination with immediate-release morphine (injection or tablets) for alleviating breakthrough pain. The dose of controlled-release oxycodone hydrochloride tablets was gradually adjusted until a stable analgesic dose was found. Patients were observed for 14 days in total. All patients also received oral administration of laxatives (15 mL of lactulose solution, twice per day), and given sufficient fluid and dietary fibre daily.
The treatment group received TENS. TENS combines traditional Chinese acupuncture with electrical stimulation, using a specific time-varying pulse current. This method can stimulate acupoints, regulate the body's qi and blood meridians and relieve symptoms to some extent. Briefly, the skin at the acupuncture point was routinely sterilized and the patient lay in a supine position. An electrode plate was placed over the acupuncture point and connected to a HANS-100A transcutaneous electrical nerve stimulator (Nanjing Jisheng Medical Technology Co., Ltd., Nanjing, Jiangsu, China). The therapy was conducted once daily for 14 consecutive days, 30 minutes each time.
The same electrode plate was attached to patients in the control group, but TENS was not performed.
Acupuncture points were selected according to the China GB Standard ‘Nomenclature and Location of Acupuncture Points' (GB/T 12346-2006). 16 The ‘Guanyuan' point, ‘Qihai' point, bilateral ‘Tianshu' points, bilateral ‘Zusanli' points and bilateral ‘Shangjuxu' points were selected. Traditional Chinese Medicine syndrome differentiation was carried out according to the ‘Diagnosis and Treatment Criteria of Common Diseases in Chinese Medicine' stipulated by the State Administration of Traditional Chinese Medicine of the People’s Republic of China. 17 Clinical symptoms include faecal dryness, defecation difficulty, stomach rumble, exhaustion of qi, appetite reduction, tongue redness, yellow or white greasy tongue coating, and slippery or wiry pulse; for these symptoms, bilateral ‘Ganshu' points should be acupunctured. Asthenic symptoms include defecation difficulty despite faecal dryness, sweating, shortness of breath, pale skin, fatigue, upset, hyposomnia, and thready, deep or slow pulse; for these symptoms, bilateral ‘Shenshu' and ‘Sanyinjiao' points should be acupunctured. For the TENS parameters, a dilatational wave (frequency 2/100 Hz) and bearable current intensity were used.
Patients who did not defecate for 3 consecutive days and thus required an examination to exclude acute ileus were requested to quit this study and to switch to other laxative therapies. Throughout the study, chemotherapy, interventional therapy, nerve block therapy and other therapies that can interfere with constipation observation were not carried out.
Observation indices
Bowel Function Index (BFI)
BFI scores over the past week were evaluated by medical staff: 1) defecation difficulty; 2) feeling of incomplete defecation; 3) overall defecation satisfaction. The above three items were scored by patients on a scale of 0 to 100 points; 0 and 100 points represent no feelings and the strongest feelings, respectively. A total score is obtained by averaging these three items; higher scores indicate more severe constipation. 18 BFI scores before and after treatment were recorded to calculate the total scores.
Evaluation of quality of life
The Patient Assessment of Constipation Quality of Life (PAC-QOL) questionnaire was used to assess treatment outcomes and quality of life in constipated patients. 19 The questionnaire comprises 28 self-report items on four dimensions: physical discomfort (items 1–4), psychosocial discomfort (items 5–12), worries and concerns (items 13–23) and satisfaction (items 24–28). The following 5-point Likert-type scale was used for responses to each item: 1) degree: not at all, a little bit, moderately, quite a bit and extremely; 2) frequency: none of the time, a little of the time, some of the time, most of the time and all of the time. Responses were scored from 0 to 4 points. The total score for each dimension is the average of all items on that dimension; the total score is the average of all dimension scores. Higher scores indicate poorer quality of life. Scores on the above four dimensions before and after treatment were recorded to calculate the total scores.
Criteria for scoring constipation symptoms and therapeutic effect evaluation
Constipation symptoms were scored according to the relevant criteria in ‘Applied Research on Traditional Chinese Medicine Spleen and Stomach Theory'
20
(Table 1). Scores on the four items were summed to obtain the total score, and scores before and after treatment were recorded. The criteria for therapeutic effect evaluation after 2 weeks of treatment were as follows: cured: disappearance of symptoms and scores of 0 for more than 2 weeks; markedly effective: significant mitigation of symptoms and score decrease by over 2/3 for more than 2 weeks; effective: mitigation of symptoms and score decrease by over 1/2; ineffective: mitigation of symptoms but score decrease lower than 1/2, or aggravation of symptoms. Calculations were performed using the equation
Constipation symptom score criteria.

Total score = sum of four item scores. Symptom scores of all patients before and after treatment were compared. Constipation treatment efficacy evaluation criteria: efficacy evaluation after 2 weeks of treatment: cured: disappearance of symptoms, score of 0 for more than 2 weeks; markedly effective: significant mitigation of symptoms, score decrease by over 2/3 for more than 2 weeks; effective: mitigation of symptoms, score decrease by more than 1/2; ineffective: mitigation of symptoms but score decrease by no more than 1/2 or aggravation of symptoms. Calculation formula: [score before treatment − score after treatment] ÷ [score before treatment] × 100%. Overall effective rate = cured rate + markedly effective rate + effective rate.
Statistical analysis
All data were analysed using SPSS 18.0 software (SPSS Inc., Chicago, IL, USA). Categorical data are expressed as mean and standard deviation. Numerical data were subjected to the χ2 test. Intergroup comparisons were performed using the independent sample t-test, and intragroup comparisons were conducted using the paired sample t-test. A value of P < 0.05 was considered statistically significant.
Results
Baseline clinical data
A total of 268 patients were included in this study. Patients were randomly assigned to a treatment group who received TENS and an oral lactulose solution (n = 130), and a control group who received only oral lactulose solution (n = 138). The treatment group comprised 48 cases of primary lung cancer, 9 cases of pancreatic cancer, 8 cases of gastric cancer, 24 cases of breast cancer, 3 cases of cervical cancer, 2 cases of ovarian cancer, 9 cases of colon cancer, 6 cases of hepatic cancer, 8 cases of prostate cancer, 4 cases of malignant melanoma and 4 cases of metastatic cancer with unknown primary foci. There were 74 males and 56 females aged 25 to 77 years (average: 55.3 ± 3.1 years). The control group comprised 41 cases of primary lung cancer, 6 cases of pancreatic cancer, 10 cases of gastric cancer, 30 cases of breast cancer, 7 cases of ovarian cancer, 2 cases of cervical cancer, 15 cases of colon cancer, 4 cases of hepatic cancer, 6 cases of prostate cancer, 6 cases of malignant melanoma, 4 cases of malignant lymphoma, 1 case of malignant mesothelioma, 2 cases of soft tissue sarcoma and 4 cases of metastatic cancer with unknown primary foci. There were 72 males and 66 females aged 31 to 80 years (average: 51.2 ± 3.4 years). The two groups had similar baseline clinical data (Figure 1).

Flowchart of the clinical study.
Overall effective rates for treatment and control groups
Of the 130 patients in the treatment group, 6 switched to other therapies (after 14 days) owing to severe constipation. Of the remaining 124 cases, 34 had clinical symptoms of constipation (27.4%) and 90 had asthenic symptoms (72.6%). The overall effective rate was 91.9% (114/124). Of the 138 patients in the control group, 11 switched to other therapies because of severe constipation. Of the remaining 127 patients, 32 had clinical symptoms (25.2%) and 95 had asthenic symptoms (74.8%). The overall effective rate was 85.8% (109/127). The treatment group showed a significantly higher overall effective rate than the control group (P = 0.018).
Outcomes of treatment and control groups
The treatment group included 85 cases of moderate cancer pain (NRS score: 4–6 points; 65.3%) and 45 cases of severe cancer pain (NRS score: 7–10 points; 34.6%). The NRS scores ranged from 4 to 9 points (average: 5.6 ± 0.9). The control group consisted of 90 cases of moderate cancer pain (NRS score: 4–6 points; 65.2%) and 48 cases of severe cancer pain (NRS score: 7–10 points; 34.8%). The NRS scores ranged from 4 to 9 points (average: 5.6 ± 0.7). Throughout the study, neither group suffered from opioid-induced mental disorders, toxic responses of the central nervous system, drug overdose or opioid poisoning. Notably, the treatment group did not show any TENS-induced adverse reactions, such as fainting or allergies.
BFI scores before and after treatment
The BFI scores after treatment (Table 2) showed a significant difference between the overall defecation satisfaction scores of the treatment and control groups (P = 0.027).
Between-group comparison of Bowel Function Index scores before and after treatment.

▲Compared with the control group after treatment, P < 0.05.
*Compared with the same group before treatment, P < 0.05. TENS: transcutaneous electrical nerve stimulation.
Quality of life before and after treatment
After treatment, the physical discomfort, psychosocial discomfort and satisfaction scores of treatment and control groups showed a significant difference (P = 0.037) (Table 3).
Between-group comparison of the PAC-QOL score before and after treatment.
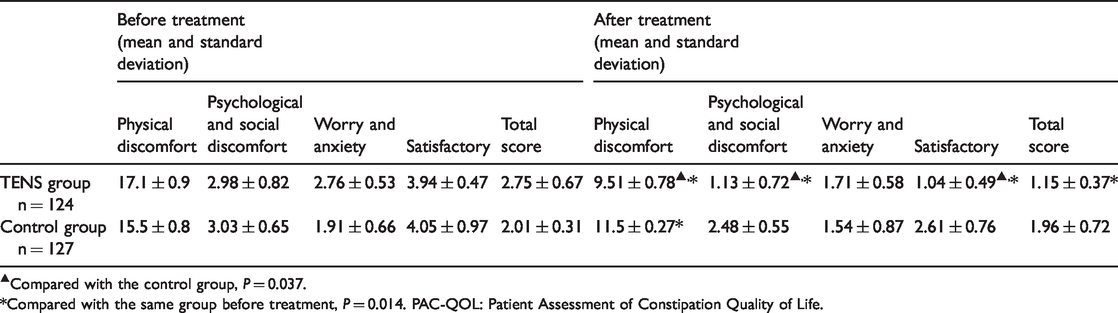
▲Compared with the control group, P = 0.037.
*Compared with the same group before treatment, P = 0.014. PAC-QOL: Patient Assessment of Constipation Quality of Life.
Scores of constipation symptoms before and after treatment
Compared with the control group, the treatment group showed a significant post-treatment reduction in constipation symptom scores (before treatment: 8.3 ± 1.4 vs. after treatment: 5.1 ± 0.6) (P < 0.05) (Table 4).
Between-group comparison of constipation symptom scores before and after treatment.
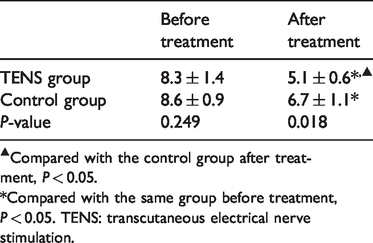
▲Compared with the control group after treatment, P < 0.05.
*Compared with the same group before treatment, P < 0.05. TENS: transcutaneous electrical nerve stimulation.
Therapeutic effects on constipation before and after treatment
After treatment, the overall effective rate of the treatment group reached 91.9% (Table 5).
Between-group comparison of constipation efficacy before and after treatment, cases (%).

▲Compared with the control group, P = 0.013. TENS: transcutaneous electrical nerve stimulation.
Discussion
As the most common adverse reaction of opioids, OIC seriously affects patient quality of life and cannot currently be effectively treated. There are many opioid receptors in the human gastrointestinal tract. After binding opioids, they become activated and delay gastric emptying owing to smooth muscle spasm. The intestinal tract simultaneously undergoes hypertonic rhythmic peristalsis and propulsive contraction that weaken bowel evacuation and delay anal sphincter spasm, finally decelerating faecal transport. Opioid receptors decrease the secretion of intestinal glands in the gastrointestinal tract, generating hard and dry faeces and eventually causing constipation. Traditional Chinese Medicine holds that opioids are warm, dry, spicy and migratory, qualities that disturb the yin and yang qi–blood circulation and, particularly, induce qi stagnation in the large and small intestines. 21 Cancer pain mostly occurs in patients with advanced malignant tumours, and their constipation generally manifests as asthenic symptoms (deficiency of both qi and yin, spleen and kidney deficiency) after surgery, radiotherapy and repeated chemotherapy that consume qi, impair body fluids, and induce spleen–kidney deficiency. Consistently, most patients in both groups in this study experienced asthenic symptoms.
There are currently no universal OIC diagnostic criteria and treatment outcomes are generally evaluated based on patient-reported symptoms. The Rome III diagnostic criteria are frequently used to assess chronic functional constipation, which is defined as symptoms that persist for at least 6 months before diagnosis or occur within the last 3 months. 22 Therefore, the criteria are not applicable to the diagnosis of all OIC cases (some patients became constipated after taking oral opioids just once). In combination with clinical practice, we selected the 2014 OIC diagnostic criteria of the American Multidisciplinary Panel, which requires that related symptoms appear following oral administration with opioids for more than 1 week. Traditional Chinese Medicine concepts of constipation were also considered.
The BFI was proposed by Mundipharma Research in 2002 to assess OIC symptoms.18,20,23 This scale was designed to evaluate the degree and symptoms of secondary constipation after oral administration of opioids for almost 1 week, and has well-proven clinical practicability, simplicity, reliability and focus on patient-reported symptoms. 24 In addition, the scale can correct the likely bias resulting from comprehensive symptom scoring, producing a composite outcome index, in the evaluation system for the therapeutic effects of Traditional Chinese Medicine on chronic constipation. 25 In this study, satisfactory treatment outcomes were obtained after simultaneous oral administration with opioids and lactulose solution, resulting in a significant difference in BFI scores before and after treatment (P = 0.027). Moreover, the overall defecation satisfaction score was further improved by combining the treatment with TENS (P = 0.001), indicating that constipation symptoms were relieved. Collectively, BFI scores improved consistently with Traditional Chinese Medicine constipation symptom scores and therapeutic effects.
The PAC-QOL questionnaire was developed to assess treatment outcomes and quality of life in constipated patients. 26 Compared with universal scales such as the Short Form Health Survey (SF36), 27 this questionnaire is a more intuitive measure of the detrimental effects on quality of life caused solely by constipation, so therapeutic effects can be evaluated more sensitively. After treatment, the physical discomfort, psychosocial discomfort and satisfaction scores of both groups, particularly those of the treatment group, were significantly better than before treatment (P = 0.037), but the total score did not drop significantly.
Acupuncture and moxibustion can treat OIC; all such treatments (including simple acupuncture, acupuncture and moxibustion, auricular acupuncture and acupoint injection) have some beneficial effect.28,29 TENS uses mild electrical stimulation through skin electrodes and is equivalent to needle-free electroacupuncture. The condensation-rarefaction wave used can stimulate the release of endogenous endorphins, dynorphins and other neurotransmitters, promoting normal gastrointestinal tract movement. 30 The therapeutic effect of TENS is based on its action on somatic (visceral) nerve reflexes. For instance, acupuncture on the stomach meridian of Foot-Yangming can facilitate intestinal peristalsis and treat constipation. The spinal cord projecting nerves of T10 to L5 correspond to the distribution of the segments of the large intestine. 31 Xu et al. 21 treated chronic slow transit constipation with transdermal electrical stimulation and achieved good results. However, further studies are needed to confirm the mechanism by which TENS ameliorates defecation difficulty in OIC patients. Yu et al. 32 have suggested that human motor nerves can convert the external current of 1 kHz (a low-frequency current) into biological electricity in the body, which then has biological effects on human tissues. Xu 14 has reported that low-frequency electrical stimulation can reduce the release of neurotransmitters that inhibit gastrointestinal motility, thereby regulating intestinal activity. In the present study, bilateral ‘Tianshu’ and ‘Zusanli’ (ST36) acupoints were stimulated using TENS, which promoted local blood circulation, ameliorated gastrointestinal function and mitigated constipation symptoms. Animal studies 33 have suggest that electroacupuncture can promote distal colon contractile function via cholinergic neuromediated stimulation. Therefore, the action mechanism of TENS on OIC constipation symptoms may also involve neuromodulation, but more research is needed to confirm this.
Conclusion
TENS is simpler, safer and more repeatable than traditional acupuncture therapies, and so is more suitable for the self-management of patients who must stay at home for lengthy periods or cannot take drugs orally. Therefore, TENS should be promoted for use in clinical practice for such patients.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The research was supported by the Zhejiang Provincial Traditional Chinese Medicine Fund (No. 2019ZB018), Zhejiang Provincial Medical and Health Scientific and Technical Fund (No. 2018KY312) and Zhejiang Provincial Natural and Science Fund (No. LY19H290001).