Abstract
Purpose
Accidental tumor incision (ATI) can occur during nephron-sparing surgery (NSS) and correlates with recurrence and metastasis. This study investigated risk factors of intraoperative ATI in renal cell carcinoma (RCC) patients after NSS and the efficacy of povidone-iodine for ATI.
Methods
A retrospective analysis was performed on 150 consecutive stage I (pT1N0M0) RCC
patients who underwent NSS at The Second Hospital of Tianjin Medical University between
May 2010 and October 2015 for the causes of ATI. Furthermore,
Results
Among the 150 cases, 15 showed ATI, of which three suffered local recurrence during a
median follow-up of 56 months. Pseudocapsules, satellite nodules, and renal cystic
tumors were observed in ATI cases.
Conclusions
The probability of ATI is high in patients with complex-type RCC during NSS. ATI potentially increases the chance of metastasis and local recurrence, and 0.5% povidone-iodine kills tumor cells more effectively than distilled water.
Keywords
Introduction
The clinical application of nephron-sparing surgery (NSS) for treating stage I (pT1N0M0)
renal cell carcinoma (RCC) has gradually increased owing to improvements in surgical
concepts and the development of diagnostic imaging techniques.
1
NSS with renal preservation has become the
gold standard for treating pT1N0M0 RCC because of feasible surgical techniques and improved
prognosis.2–4 Complete tumor resection is a significant
surgical principle for any tumor type.
5
A prior study found that the rate of tumor
seeding and metastasis can be effectively reduced by avoiding tumor incisions.
6
However, accidental tumor
incision (ATI) occasionally occurs in patients treated with NSS and is associated with tumor
recurrence and metastasis.
7
To investigate the risk factors for tumor recurrence and metastases
associated with ATI, we collected data from pT1N0M0 RCC patients who underwent NSS between
2010 and 2015. Then, causes of ATI and consequences of tumor excision were analyzed in
patients who underwent tumor resection. Through
Materials and methods
Patients
This retrospective study enrolled 150 consecutive pT1N0M0 RCC patients who were treated with laparoscopic NSS at The Second Hospital of Tianjin Medical University (Tianjin, China) between May 2010 and October 2015.
Cell culture
786-O cells, which are a cell line derived from a primary clear cell RCC lesion, were provided by Dr. Wang Yong (Institute of Urology, the Second Hospital of Tianjin Medical University, Tianjin, China). Cells were cultured in RPMI-1640 medium containing 10% fetal bovine serum in a 5% CO2 incubator (HERAcell150, Thermo Fisher Scientific, Rockford, IL, USA) at 37°C with constant humidity.
In vitro experiments
Fresh human RCC samples were incised with laparoscope scissors
786-O cells were plated in 24-well plates at a density of 4000 cells/well. The control group was treated with normal saline. The experimental group was divided into the distilled water group and the 0.5% povidone-iodine solution group; both were soaked for either 5 or 10 minutes, and then washed with PBS for 3 minutes. Then RCC cells were stained with 10 µg/mL Hoechst 33258 (C0020, Solarbio) for 20 minutes. Cells were washed with PBS, covered with coverslips, and then observed under a FV1000 confocal microscope (Olympus Optical Co.).
Results
Among the 150 cases, the median age was 62.5 years and the average tumor diameter was 3.4 cm (range: 1–7 cm). Fifteen patients showed ATI during surgery, and these cases were followed up for a median duration of 56 months. Among these 15 patients, two had pseudocapsule invasion (Figure 1a), four presented irregular growth tumor (Figure 1b), one exhibited satellite nodules (Figure 1c), two showed renal cystic tumor (Figure 1d), and two showed intraoperative hemorrhage (Table 1).
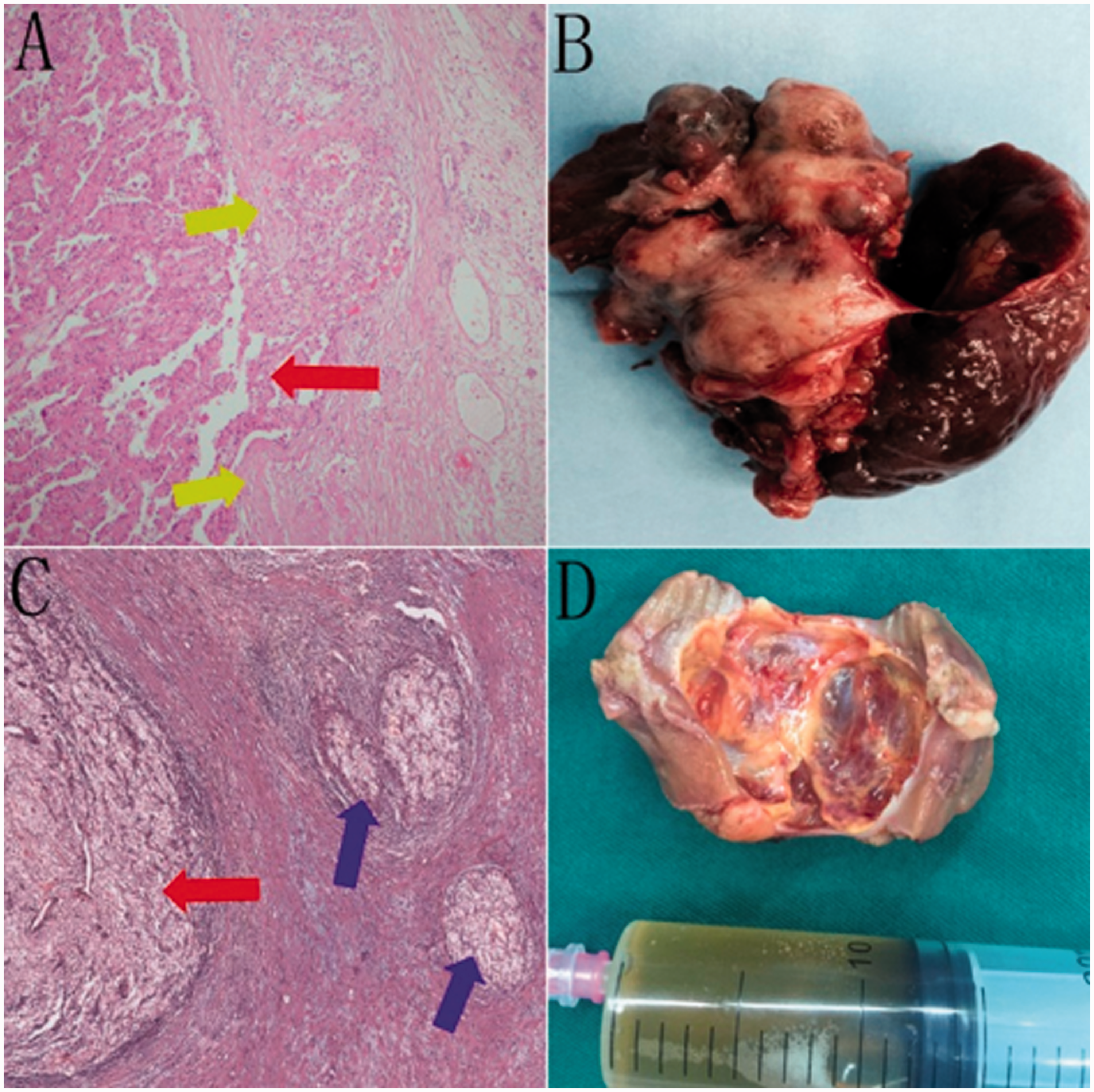
Analysis of risk factor for ATI in 15 pT1N0M0 RCC patients with ATI.
Type of accidental tumor incision during nephron-sparing surgery.

Tumor samples were also incised using laparoscope scissors

Tumor cells remaining on the surface of scissors after ATI. ATI, accidental tumor incision
768-O cells were treated with distilled water and 0.5% povidone-iodine for 30 minutes, followed by staining with Hoechst 33258. Hoechst is a nuclear membrane-permeable fluorescent dye. Hoechst staining of normal cell nuclei is round and blue, while the nuclei of dead cells are lobulated and fragmented. As the results showed, 768-O cells were killed in 30 minutes by distilled water, and the morphology of the cells treated with distilled water changed. However, 0.5% povidone-iodine killed 768-O cells more effectively than distilled water treatment (Figure 3).

The effect of distilled water and povidone-iodine on 786-O cells.
During follow-up, local recurrence occurred between 3 months and 4 years in three cases. One case underwent seeding metastasectomy, one received radical nephrectomy, and the other was accompanied by multiple lung and liver metastases, and died 4 months after surgery (Table 2). Among the three cases of local recurrence, tumors of one case migrated onto the surface of the kidney (Figure 4a), and tumors of the other two cases metastasized to peripheral and adipose tissues (Figure 4b–d). The four recurrences were found among 135 cases without ATI during follow up, yielding a recurrence rate of 2.96% (Table 3).
Analysis of metastasis and local recurrence in patients with ATI.
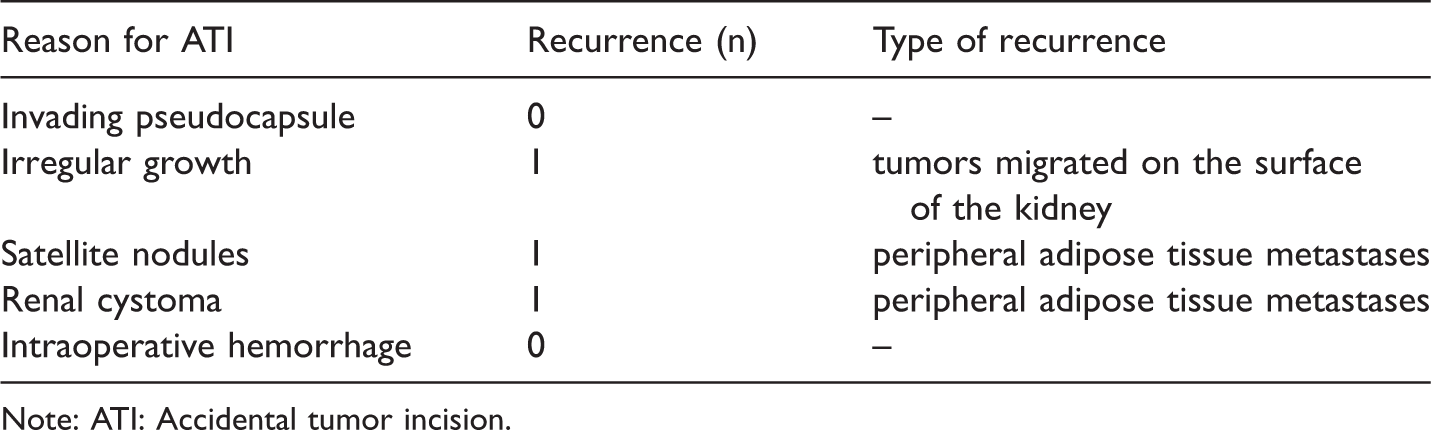
Note: ATI: Accidental tumor incision.

Analysis of metastasis in three pT1N0M0 RCC patients with local recurrence after ATI.
Pathological classifications and relapse characteristics.
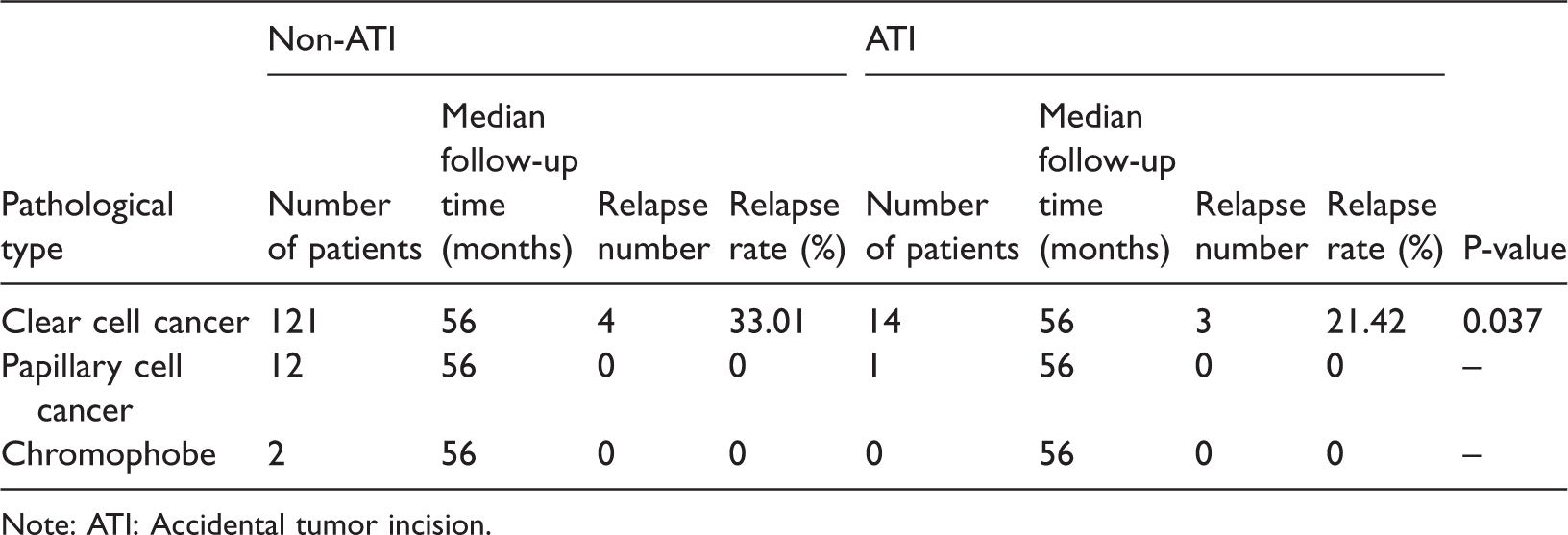

Note: ATI: Accidental tumor incision.
Discussion
In the genitourinary system, renal cancer is the third most common malignancy, accounting
for 4% to 5% of all male malignancies and 2% to 3% of all female malignancies in the United
States.8,9 Approximately 63,990 cases
of renal masses are expected to be diagnosed
Although
To reduce the risk of tumor recurrence and metastasis, we analyzed the reason for ATI in patients undergoing NSS and impact of tumor incision. Among 150 cases receiving NSS, ATI occurred in 15 cases. Our analysis found that the risk factors for ATI included pseudocapsule invasion, irregular tumor growth, satellite nodules, and renal cystic tumors. Meanwhile, intraoperative hemorrhage may interfere with the operator's judgment.
A previous study concluded that 82% of RCC cases will develop pseudocapsules. 8 Pseudocapsules are an easily identifiable marker of tumor-substantial demarcation, 20 and can benefit surgeons in their efforts to efficiently remove complete tumors, especially in blunt tumor enucleation. 21 According to our research, some tumors might grow invasively and invade the pseudocapsule. There are two possible situations for this: on the one hand, the pseudocapsule is incomplete and tumor is incised; on the other hand, the pseudocapsule is incomplete, but the tumor is completely contained within the pseudocapsule when it is removed. The former can be considered ATI and have the possibility of metastasis and recurrence, while the latter is almost impossible. Satellite nodules were another reason for ATI. Because pT1N0M0 RCC is <7 cm, most satellite nodules are only found by pathological examination after surgery. Meanwhile, renal cystic tumor was also a risk factor of ATI because the morphology of cystic tumors is similar to renal cysts. The main pathology types of renal cystic tumors are low malignant potential clear cell carcinoma. Clinicians should distinguish between tumors and cysts by careful preoperative diagnosis to avoid the occurrence of ATI.
Based on our cases, local recurrence appeared in three cases among those with ATI. Tumors of one of these cases migrated onto the surface of the kidney, and tumors of the other two cases had metastases to peripheral and adipose tissues.
To decrease the risk of tumor seeding and metastasis after ATI, we should treat or replace equipment. A prior study suggested that tumor cells can be killed after ATI by treatment with electricity. 22 Currently, tissues around solid tumors are often sealed with electrocoagulation after ATI. However, distilled water is always used during ATI treatment in renal cystic tumors. Our study showed that 0.5% povidone-iodine had a more lethal effect on RCC cells than distilled water over a short time period.
This study was a retrospective single-center empirical study with some deficiencies. The
cases enrolled were performed by different surgeons. Hence, there were differences in the
surgical skills among these surgeons. The induction of risk factors for ATI is very
informative and instructive; however, because of the limited number of cases and no
statistical analysis, multi-center peer reviews are needed to test the results obtained from
our study for the representativeness and reliability of the conclusions. Additionally, we
simply verified the possibility of recurrence after ATI by
Conclusions
Our data elucidated the impact of ATI on tumor metastasis and local recurrence in RCC patients undergoing NSS as well as the risk factors for ATI, including pseudocapsules, satellite nodules, irregular tumor growth, and renal cystic tumors. The probability of ATI is high in partial nephrectomy for these types of RCC. In accordance with previous experiments in the literature, our study suggested that tumor cells could remain on the surface of scissors and have the ability to seed or recur after ATI. Additionally, 0.5% povidone-iodine killed more RCC cells than distilled water in 30 minutes. Povidone-iodine treatment may decrease potential implant metastasis or recurrence of non-solid tumors after ATI. In summary, it is particularly critical that ATI be avoided by preoperative diagnosis and assessments of tumor shape.
Abbreviations
Accidental tumor incision (ATI); renal cell carcinoma (RCC); nephron-sparing surgery (NSS)
Footnotes
Ethics approval and informed consent
This study was approved by The Second Hospital of Tianjin Medical University Ethics Committee and was performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. All persons gave their informed consent prior to their inclusion in the study. Details that might disclose the identity of subjects under study have been omitted.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by Tianjin Municipal Natural Science Foundation (Grant 17JCYBJC26000), and Science and technology innovation fund projects of Tianjin Institute of Urology (number MNYB201503).
