Abstract
Objective
This study was performed to compare the use of a video laryngoscope-guided lightwand versus a single lightwand for tracheal intubation performed by non-experts in cervical spine-immobilized patients.
Methods
In total, 318 patients under general anesthesia were assigned either to the single lightwand group (Group L) or the video laryngoscope-guided lightwand group (Group VL) at a 1:1 ratio. First- or second-grade residents performed tracheal intubation with the assigned device after applying semi-hard fitted cervical collars to the patients. Outcomes, including the success rate and airway complications, were compared between the two groups.
Results
There were no significant differences in demographics or airway-related characteristics between the two groups. The success rate of intubation on the first attempt was significantly higher in Group VL than in Group L (90% vs. 64%, respectively). Postoperative complications, including oral mucosal bleeding, hoarseness, and sore throat scores at 1 and 24 hours after surgery, were significantly lower in Group VL than in Group L.
Conclusions
The use of a video laryngoscope-guided lightwand for tracheal intubation can be useful for non-experts who encounter difficult airway situations.
Keywords
Introduction
In patients with suspected cervical instability, it is important to limit cervical spine movement during tracheal intubation to prevent secondary neurological damage. 1 Several methods with which to maintain a neutral head position have been studied, such as the use of cervical collars, sandbag, tapes, and manual in-line stabilization.2–5 These methods can limit cervical spine movement. However, they make tracheal intubation more challenging, even for experienced anesthesiologists, leading to increased mortality. 4
A direct laryngoscope is commonly used for tracheal intubation. Careful attention is needed for patients with cervical instability because of the need for head flexion and neck extension. 6 Various alternative intubation devices have been developed to reduce the difficulty of tracheal intubation using direct laryngoscopy. Of these, the lightwand, a lighted stylet, is a useful device in patients with cervical instability because this device does not require neck extension to directly visualize the vocal cord.7–9 However, use of the lightwand carries a risk of causing oral cavity injury because it is a blind technique. 8 In addition, the lightwand requires a jaw thrust maneuver for easier placement in the midline underneath the epiglottis. Such a maneuver also causes cervical spine movement.2,10
The video laryngoscope has recently been used in difficult intubations.11,12 The video laryngoscope allows for better glottis visualization than does a direct laryngoscope because the camera at the tip of the video laryngoscope blade can enable visualization of the vocal cord without the need to achieve alignment of the oral, laryngeal, and pharyngeal airway axes.11,13 However, despite the theoretical advantages of this device, previous studies have shown no difference in cervical spine movement between the video laryngoscope and direct laryngoscope.7,12 Based on these results, we used a lightwand and video laryngoscope together in the present study to amplify the advantages of each device. We hypothesized that video laryngoscope placement prior to insertion of the lightwand into the oral cavity would serve as a guide to facilitate tracheal intubation. The aim of this study was to compare the success rate of intubation performed by first- or second-grade residents and the incidence of airway complications between use of a single lightwand and combined use of both a video laryngoscope and lightwand for tracheal intubation in simulated cervical spine-immobilized patients.
Methods
Study population
This prospective, single-blind randomized study was approved by Institutional Review Board of Yonsei University College of Medicine (1-2016-0069), and the study protocol was registered at ClinicalTrials.gov (NCT03169556). Written informed consent was obtained from all participants. Patients aged 20 to 80 years with an American Society of Anesthesiologists physical status of 1 or 2 who were scheduled to undergo surgery with general anesthesia were included in the study. The exclusion criteria were a history of gastroesophageal reflux disease, airway surgery, or difficult intubation; an anatomical abnormality in the upper airway such as an abscess, tumor, stenosis, or vocal cord palsy; coagulopathy; a body mass index (BMI) of >35 kg/m2; hemodynamic instability; loose teeth; illiteracy, foreign residence (i.e., outside South Korea); refusal to participate in this study; and lack of decision-making capability.
Randomization
The participants were randomly assigned to one of the following two groups at a 1:1 ratio: the single lightwand group (Group L) or the video laryngoscope-guided lightwand group (Group VL). The randomization was generated in blocks of six using R 3.4.0 (Vienna, Austria; http://www.R-project.org/). Each group assignment was concealed in a sealed, opaque envelope. The envelope was opened by one of the authors (H.J.Y.) immediately before induction of anesthesia. The preoperative and postoperative outcome assessors and patients were blinded to the type of intervention (group assignment).
Study protocol
In-room anesthesiologists (first- or second-grade residents) measured the modified Mallampati score, thyromental distance, and interincisor distance of patients in the preanesthetic room without knowing the group assignment of the patient. After arrival in the operation room without premedication, the patients underwent basic monitoring including pulse oximetry, electrocardiography, and noninvasive blood pressure measurement. After preoxygenation via a facial mask, the patients began target-controlled infusion of anesthetic drugs [remifentanil (effect site concentration of 3.0 ng/mL) and propofol (effect site concentration of 5.0 mcg/mL) followed by rocuronium (0.6–1.0 mg/kg)]. Manual mask ventilation with 100% oxygen was then maintained for 5 minutes before intubation to ensure sufficient oxygenation and muscular relaxation. During manual mask ventilation, one of the authors (H.J.Y.) applied a semi-hard cervical collar (Philadelphia Tracheostomy Collar; OSSUR, Kunming, China) to the patient to simulate cervical immobilization and opened the envelope to confirm the group assignment of the patient. The lightwand (LightWand™; GE Healthcare, Chicago, IL, USA) with an endotracheal tube was prepared after bending it to a 90° angle at 6 cm from the distal end based on a previous study of the optimal bending length and angle14,15 (Figure 1). The video laryngoscope (UESCOPE®; Zhejiang UE Medical Corp., Zhejiang, China) was additionally prepared for patients in Group VL. Among many kinds of video laryngoscopes, we chose the UESCOPE® with a blade size of 3 because this device has a blade angle of 40°, which facilitates an anterior view of the respiratory tract without blind zones.

Lightwand (LightWand™; GE Healthcare, Chicago, IL, USA) with endotracheal tube and video laryngoscope (UESCOPE®; Zhejiang UE Medical Corp., Zhejiang, China). The lightwand was prepared by bending it 6 cm from the distal end.
At the time of tracheal intubation, a manual in-line stabilization maneuver was performed and a cervical collar was applied by one of the authors (H.J.Y.) to reduce unintended cervical spine movement for all patients. Tracheal intubation was attempted by first- or second-grade residents with >10 months of training in intubation. They had performed >100 procedures with the video laryngoscope and a ≥10 successful intubations with the lightwand intubation device. The jaw thrust maneuver, which is recommended in conventional lightwand intubations to create space for free movements of the lightwand in the oral cavity, was not used in Group L because an excessive jaw thrust maneuver itself could cause cervical movement.2,10 The inner diameter of the endotracheal tube was 7.5 mm in men and 6.5 mm in women. For Group L, after turning the lights off in the operating room and turning on the lightwand light source, the lightwand with the endotracheal tube was introduced toward the corner of the mouth laterally and rotated 90° toward the anesthesiologist to position the lightwand tip at the midline underneath the epiglottis. After confirming transillumination of the patient’s neck, the endotracheal tube was gently advanced. For Group VL, the video laryngoscope was first inserted into the oral cavity until the epiglottis tip was visible. After confirming the epiglottis tip without raising the handle or blade of the video laryngoscope, the lights in the operating room were turned off and the lightwand with the endotracheal tube was advanced; its position was confirmed in the same way as described for Group L. If the patient’s oxygen saturation as shown by pulse oximetry decreased to 95% or the intubation process was prolonged beyond 90 seconds, the attempt was stopped and mask ventilation was applied until the oxygen saturation had increased to 100% before another intubation attempt was made. A maximum of three intubation attempts were allowed. If intubation failed after three attempts, failure of tracheal intubation was declared. At that point, the cervical collar was removed from the patient and tracheal intubation was conducted using the standard technique. The patient’s heart rate and noninvasive blood pressure were recorded sequentially from immediately before insertion of the intubation device to 5 minutes after successful intubation.
Outcome measurement
The primary outcomes were the success rate on the first attempt and the intubation time. Success of intubation was confirmed when end-tidal carbon dioxide was detected after connecting a capnography device to the end of the endotracheal tube. The successful intubation time was defined as the duration between insertion of the lightwand or video laryngoscope into the oral cavity and removal of all intubation devices from the oral cavity after successful intubation. The total intubation time was defined as the sum of the duration of all attempts (within three attempts). The secondary outcomes were the number of intubation attempts; the incidence of hypertension, tachycardia, oral cavity injury, tooth injury, and postoperative hoarseness; and the postoperative sore throat score. Hypertension and tachycardia were defined as increases in the blood pressure and heart rate by >30% compared with the baseline values from insertion of the intubation device to 5 minutes after successful intubation.
We examined the lips, oral mucosa, and teeth immediately after intubation to check for oral cavity injury and tooth injury. We examined the endotracheal tube cuff at the time of extubation. Postoperative hoarseness was measured by patient responses of “yes” or “no” and sore throat was measured by a visual analog scale (0 = none, 100 = worst) at 1 hour after arrival in the postanesthetic care unit and 24 hours after surgery. These measurements were conducted by the attending nurse.
Statistical analysis
Differences between the two groups were analyzed using the chi-squared test or Fisher’s exact test for categorical variables. Continuous variables were analyzed using Student’s t-test by the central limit theorem that normal distribution can be assumed when the sample size is appropriate. 16 Analysis using a generalized estimating equation was applied to repeated measurements of parameters. Correlations of variables were analyzed by Spearman’s rank order correlation. Predictors of failed intubation were tested by logistic regression analysis. After logistic regression analysis of each parameter, performances were evaluated using receiver operating characteristic curves and the area under the curve (AUC). A P value of <0.05 was considered statistically significant. All statistical analyses were performed using SAS version 9.4 (SAS Institute Inc., Cary, NC, USA).
Sample size calculation
The sample size was calculated using G power 3.1 (Franz Faul, Germany; http://www.gpower.hhu.de/). Of the two primary outcomes in this study (success rate on the first attempt and intubation time), we focused on the success rate on the first attempt to calculate the sample size. A previous study compared the lightwand with other devices in 24 patients with applied cervical collars 17 and found that the success rate of intubation on the first attempt was 63% in the group in which only the lightwand was used. Anticipating a 15% increase in the success rate in the video guided lightwand group, we determined that 144 patients were required in each group with a type I error of 0.05 (two-tailed) and a power of 0.8. Considering a dropout rate of 10%, we determined that 159 patients were required for each group.
Results
After excluding 23 patients who met the exclusion criteria, 318 patients were enrolled in this study from December 2016 to October 2017. They were randomly allocated to the two groups with 159 patients per group. Intraoperative variables, including data associated with intubation attempts, hemodynamic changes, and injury to the oral cavity and teeth, were analyzed for all patients. During postoperative follow-up, five patients were excluded (four were transferred to the intensive care unit and sedated unexpectedly, and one developed postoperative delirium). Therefore, 313 patients were finally analyzed for postoperative outcomes, such as hoarseness and sore throat. The CONSORT flow chart is shown in Figure 2. The demographics and airway-related characteristics of the patients were not significantly different between the two groups (Table 1).

CONSORT flow chart. Group L, single lightwand group; Group VL, video laryngoscope-guided lightwand group.
Demographics and airway-related characteristics.

Group L, single lightwand group; Group VL, video laryngoscope-guided lightwand group.
Continuous data are given as mean ± standard deviation. Nominal data are given as number (percentage).
The intubation characteristics and intraoperative hemodynamics are summarized in Table 2. The five patients with failed intubations were successfully intubated with the standard technique after removal of the neck collar. The success rate on the first attempt was significantly higher in Group VL than in Group L (P < 0.001). The cumulative number of successful intubations for each attempt is shown in Figure 3. The intubation time, measured only at the moment of successful intubation, was comparable between the two groups. Additional insertion of the video laryngoscope in Group VL did not prolong the time required for successful intubation. However, the total intubation time, calculated as the sum of each intubation time within three attempts, was shorter in Group VL than in Group L (P = 0.004). The incidence of hypertension did not significantly differ between the two groups, although there was significantly less tachycardia in Group VL than in Group L (P = 0.002) (Table 2).
Intubation characteristics and intraoperative hemodynamics.

Group L, single lightwand group; Group VL, video laryngoscope-guided lightwand group; CI, confidence interval.
Continuous data are given as mean ± standard deviation. Nominal data are given as number (percentage).
aSuccessful intubation time was defined as the duration between insertion of the lightwand or video laryngoscope into the oral cavity and removal of all intubation devices from the oral cavity when the intubation attempt was proved successful by detection of end-tidal carbon dioxide.
bTotal intubation time was defined as the sum of the durations of all attempts (within three attempts).
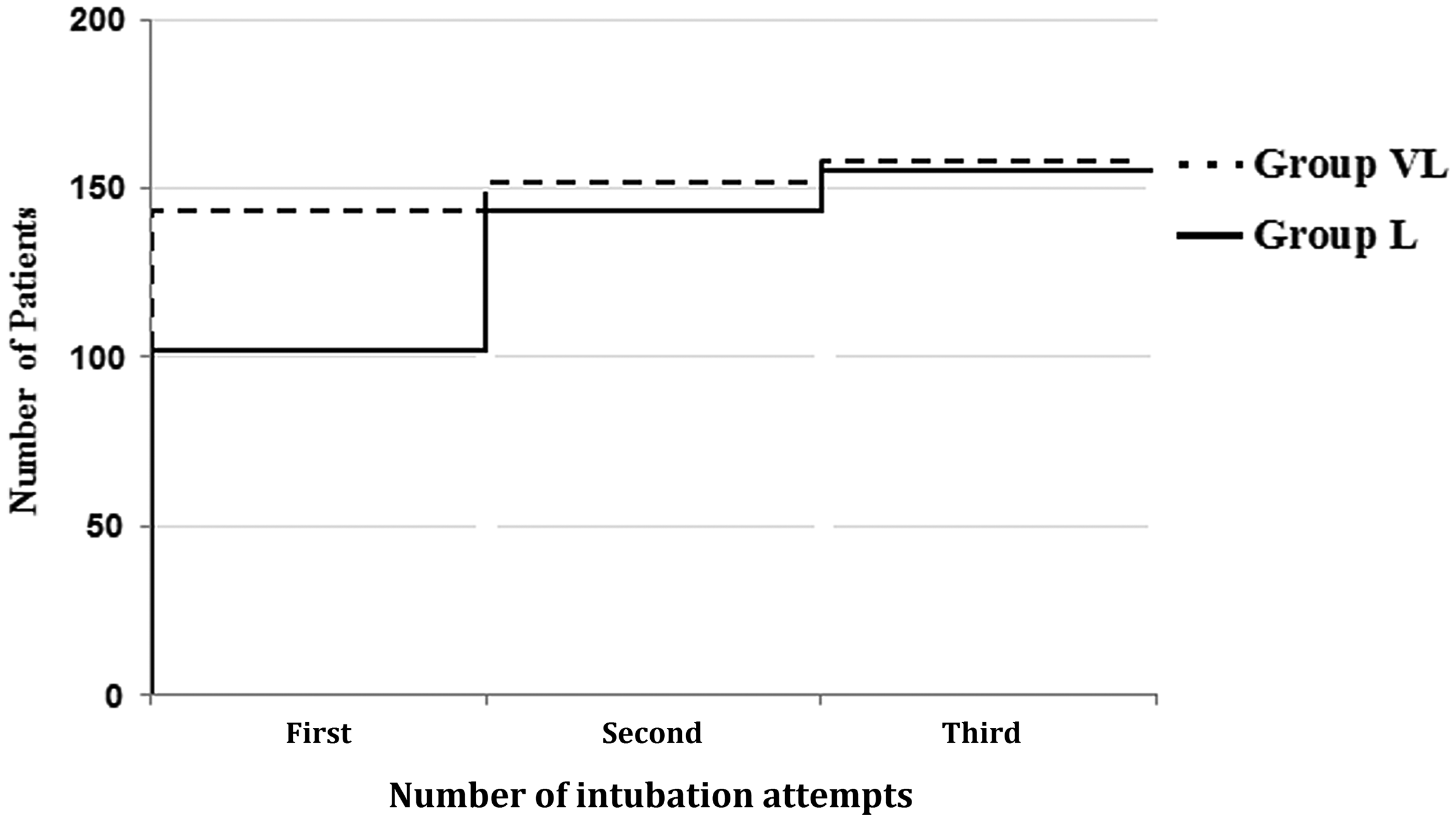
Cumulative number of successful intubations for each attempt. Group L: single lightwand group, Group VL: video-laryngoscope guided lightwand group.
The incidence of oral mucosal bleeding was significantly lower in Group VL than in Group L (P = 0.03). Dental injury did not occur in either group. The incidence of hoarseness and the visual analog scale scores for sore throat at 1 and 24 hours postoperatively were significantly lower in Group VL than in Group L (P = 0.049 for both) (Table 3).
Complications associated with intubation.
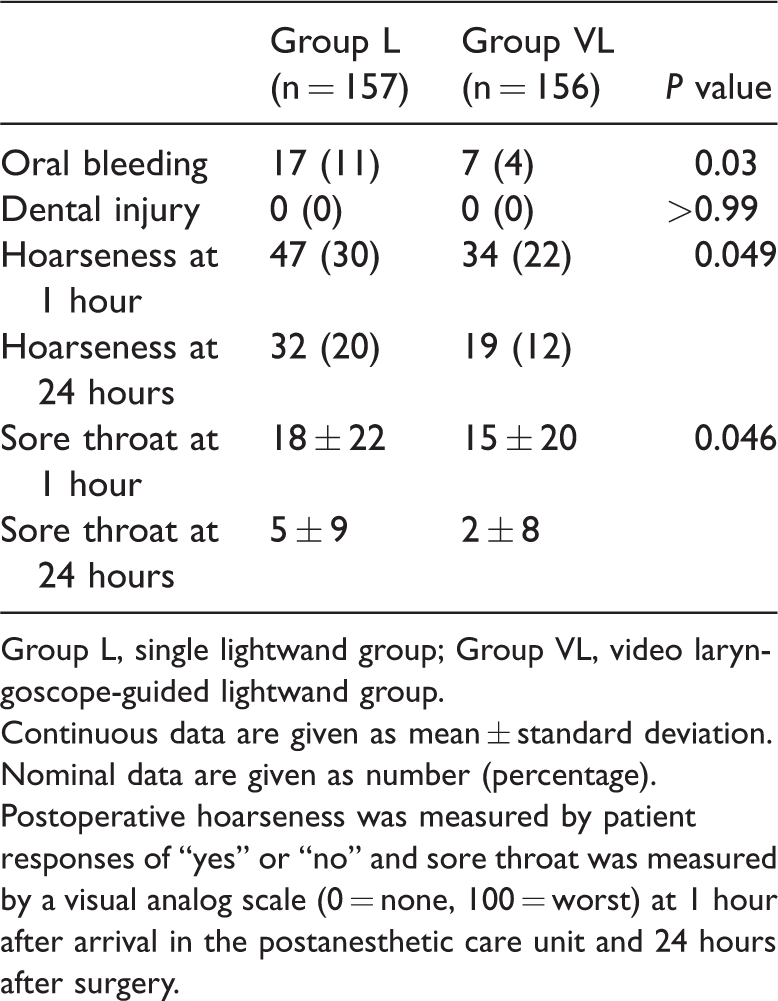
Group L, single lightwand group; Group VL, video laryngoscope-guided lightwand group.
Continuous data are given as mean ± standard deviation. Nominal data are given as number (percentage).
Postoperative hoarseness was measured by patient responses of “yes” or “no” and sore throat was measured by a visual analog scale (0 = none, 100 = worst) at 1 hour after arrival in the postanesthetic care unit and 24 hours after surgery.
Correlation analyses were performed between the number of intubation attempts and four parameters (BMI, thyromental distance, interincisor distance, and Mallampati grade) to predict difficult airways within each group. In Group L, there were no significant correlations between the number of intubation attempts and the four parameters. In contrast, in Group VL, the interincisor distance and thyromental distance showed significant negative correlations with the number of intubation attempts (r = −0.227, P = 0.004 and r = −0.286, P < 0.001, respectively). The BMI was a significant negative predictor of successful intubation within three attempts (odds ratio = 0.72, 95% confidence interval = 0.55–0.96, P = 0.02, AUC = 0.82) (Figure 4). In Group L, the BMI remained the only significant negative predictor of successful intubation (odds ratio = 0.64, 95% confidence interval = 0.44–0.95, P = 0.03, AUC = 0.85).

Receiver operating characteristic curves and area under the curve for four parameters predicting successful intubation. ROC, receiver operating characteristic; BMI, body mass index.
Discussion
Our study showed that video laryngoscope-guided lightwand intubation increased the success rate by up to 90% in patients with simulated difficult airways on the first attempt; this was 26% higher than the success rate of 64% on the first attempt using single lightwand intubation. The intubation time was comparable between the two intubation techniques at the moment of successful intubation. However, the total intubation time, calculated as the sum of all intubation attempts, was shorter in video laryngoscope-guided lightwand intubations than in single lightwand intubations. The incidence and severity of postoperative complications, including oral mucosal bleeding, hoarseness, and sore throat, were lower in video laryngoscope-guided lightwand intubations than in single lightwand intubations.
Compared with previous studies of cervical-immobilized patients showing initial intubation success rates of 63%, 75%, or 87% using the lightwand,17–19 our study showed a similar or slightly lower success rate on the first attempt (64%) in the single lightwand group. In our study, intubation was performed by first- or second-grade residents under intense conditions of limited mouth opening due to application of a fitted neck collar combined with performance of manual in-line stabilization techniques. In addition, a jaw thrust maneuver, which is generally used in lightwand intubations, was completely prohibited because it could have resulted in narrowing of the spinal cord and distraction at the level of cervical injury.2,10 These factors might have contributed to the slightly lower success rate in Group L. In contrast, in Group VL, the blade of the video laryngoscope could lift the tongue base, providing space for more controlled movement of the lightwand. In addition, the camera at the tip of the video laryngoscope served as a guide to place the lightwand at the midline of the epiglottis. These factors might have resulted in the 26% higher intubation success rate on the first attempt in Group VL despite the fact that first- or second-grade residents with relatively little experience performed the tracheal intubation.
No correlation was found between the number of intubation attempts and the four parameters used to predict difficult airways in Group L. In other words, single lightwand intubation was not influenced by anatomical variability. However, in the analyses of patients with failed intubations, the BMI was a significant predictor of failed intubation in Group L. These results are consistent with previous studies showing that extreme obesity was associated with lightwand intubation failure.20–22 In contrast to Group L, the interincisor distance and thyromental distance in Group VL showed significant and negative correlations with the number of intubation attempts. Because of the space needed to insert the video laryngoscope and lightwand, anatomical factors associated with space might have affected the outcomes.
Kim et al. 19 recently performed a study of similar design to compare conventional lightwand intubation and direct laryngoscope-assisted lightwand intubation in patients with cervical immobilization. Their study showed an 89% success rate on the first attempt with lightwand-assisted direct laryngoscopy. This is comparable to the success rate of 90% on the first attempt in the video laryngoscope-guided lightwand group in the present study. However, our study showed a significantly lower incidence of postoperative complications associated with intubation in the video laryngoscope-guided lightwand group than in the single lightwand group, which differs from a previous study. 16 Although a direct laryngoscope or video laryngoscope can create space in which to control the lightwand, direct laryngoscope-assisted lightwand intubation is a blind procedure, similar to conventional lightwand intubation. The better visibility provided by the video laryngoscope might reduce postoperative complications.
Our study had several limitations. First, neither the intubator nor in-room outcome assessor was blinded to the patient’s group assignment; therefore, performance of the intubation and in-room outcome measurements might have been biased. Second, we did not measure actual cervical movement, such as that caused by the radiological evaluation during intubation. However, we made an effort to minimize cervical movement through use of a fitted neck collar combined with manual in-line stabilization. Third, we only measured the interincisor distance before applying the neck collar, not after applying the neck collar. Limitations in mouth opening after neck collar application might have affected the difficulty of intubation. Fourth, among many kinds of video laryngoscopes, we used the UESCOPE®. Different results might have been obtained with other types of video laryngoscopes.
In conclusion, tracheal intubation using a video laryngoscope-guided lightwand showed a higher success rate on the first attempt with a lower complication rate than use of a single lightwand in simulated difficult airway conditions. Thus, video laryngoscope-guided lightwand intubation can be a useful alternative under difficult airway situations, especially when performed by a non-expert.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
