Abstract
Objective
This study aimed to determine the effect of repeated antivenom therapy compared with that of single antivenom therapy for treating snakebite-related systemic complications.
Methods
A retrospective medical record review from January 2008 to September 2016 was performed. Patients with snakebite injury who visited the Emergency Department in one tertiary center of Korea were included. The primary outcome was the survival rate. The secondary outcome was the effect of repeated antivenom therapy for treating snakebite-related systemic complications compared with that of single antivenom therapy on hospital length of stay.
Results
A total of 110 patients with snakebites were included. All patients survived to discharge. Twenty-nine (26.4%) patients had snakebite-related systemic complications. Of these, nine patients received repeated antivenom therapy and 20 patients received single antivenom therapy. The length of stay was significantly longer in those who received repeated antivenom therapy compared with those who received single antivenom therapy (10.0 [4.0–11.0] vs. 3.5 [0–7.0] days).
Conclusion
We were unable to demonstrate any superiority of repeated versus single antivenom therapy. However, repeated antivenom therapy is associated with a longer hospital stay. The reason for this finding is unknown.
Keywords
Introduction
Snakebites continue to account for life-threatening injuries worldwide 1 and sometimes require intensive care. 2 The total number of snakebites each year might exceed 5 million, with a snakebite-related mortality rate of 125,000 annually worldwide. 3 Accurate statistics on venomous snakebites in Korea are lacking. However, Lim et al. 4 reported that in Korea, an average of 192 to 621 people are injured by venomous snakebites and five people die annually because of snakebites. Because many cases are not reported in the statistics for several reasons, the number of patients with snakebites is expected to be higher than reported. Additionally, the incidence of snakebite may increase as the number of people participating in outdoor activities (e.g., camping, hiking, and climbing) increases.
Treatment of venomous snakebites is sometimes difficult for clinicians in Korea because sufficient guidelines, including administration of antivenom, have not been provided in clinical practice.5,6 Although previous studies have provided various recommendations for administration of antivenom,3,7,8 many clinicians have used repeated antivenom therapy and transfusion of coagulation factor, although there is weak evidence for such practice. Moreover, in Korea, we have observed that repeated administration of antivenom for systemic complication is not effective. 4 We hypothesize that this lack of effectiveness results from the different characteristics of snakebites (e.g., different characteristics of poisonous snakes, antivenom) in Korea.
Therefore, we examined the effectiveness of repeated antivenom therapy compared with that of single antivenom therapy for treating snakebite-related systemic complications in terms of length of hospital stay.
Methods
Participants
Patients who presented with snakebite injury at the Emergency Department of a tertiary center in Korea between January 2008 and September 2016 were included. Grade classification for mamushi bites is clinically used to determine the severity of injuries as follows:7,9,10 Grade I, redness and swelling around the bitten area; Grade II, redness and swelling of the wrist or foot joint; Grade III, redness and swelling of the elbow or knee joint; Grade IV, redness and swelling of the whole extremity; and Grade V, redness and swelling in parts beyond the extremity or exhibiting systemic symptoms. Rhabdomyolysis was defined as a serum creatine kinase level greater than 1000 U/L. 11 The definition and diagnostic features of venom-induced consumption coagulopathy (VICC) were referenced from a previous study. 12 Thrombocytopenia was defined as a platelet count below the lower limit (150,000/mm3). 13 Patients with a previous history of coagulopathy or insufficient data were excluded. The study protocol was approved by the Institutional Review Board of Hanyang University Seoul Hospital (HYUH 2017–07–028–001). Written informed consent was waived because data were collected by retrospective medical record review.
Data collection
Medical records were retrospectively reviewed. Data collected included age, sex, location of injury, presence of systemic complications (rhabdomyolysis, VICC, thrombocytopenia, and bleeding), dose of antivenom, survival discharge, and length of stay. All patients were managed on the basis of existing published studies and the authors’ experiences. The type and severity of the bite wound were evaluated immediately at the Emergency Department and followed up continuously. Laboratory tests that were performed included a complete blood count, general chemistry, coagulation profile, and creatinine kinase level measurement.
Antivenom was administered on the basis of clinical assessment by following the World Health Organization guideline. 3 Assessment included the following: 1) hemostatic abnormalities, neurotoxic signs, cardiovascular abnormalities, acute kidney injury, hemoglobinuria, myoglobinuria, and supporting laboratory evidence of systemic envenoming; 2) local swelling involving more than half of the bitten limb and swelling after bites on the digits; and 3) rapid expansion of swelling. Antihistamine (chlorpheniramine maleate 4 mg) was provided to protect against complications associated with antivenom use. Antivenom (Kovax Freeze-dried Agkistrodon antivenom injection; Korea Vaccine, Seoul, Korea) was administered intravenously according to the manufacturer’s instructions for avoiding the bite site at an initial dose of 6000 IU, followed by additional laboratory tests and wound reexamination.
Outcomes
The primary outcome was the rate of survival discharge. The secondary outcome was the effect of repeated antivenom therapy for snakebite-related systemic complications compared with that of single antivenom therapy on hospital length of stay.
Statistical analysis
All data were compiled using Microsoft Excel (Microsoft Corp., Redmond, WA, USA) and analyzed using IBM SPSS software (version 21.0; IBM Corp., Armonk, NY, USA). Categorical variables are reported as absolute numbers and percentages. Continuous variables are described as means ± standard deviations for normally distributed data and as median values and interquartile ranges when data were not normally distributed. Student’s t-test (parametric data) and the Mann–Whitney test (nonparametric data) were used to evaluate differences between the two treatments. The Jonckheere–Terpstra test was used to analyze the trend of the occurrence of complications according to the severity grade. For all analyses, differences with a P value of <0.05 were considered statistically significant.
Results
Patients’ characteristics
A total of 110 patients with snakebites were included in this study. The general characteristics of the patients are shown in Table 1. The mean age of the patients was 51.8 ± 17.2 years and male patients comprised 65.5% (n = 72) of the study population. Of the 110 patients, 85 (77.3%) received antivenom for several reasons (local swelling: n = 52, neurological symptoms: n = 9). There were no complications associated with antivenom. Twenty-nine (26.4%) patients experienced systemic complications, including rhabdomyolysis, VICC, and thrombocytopenia. The incidence of rhabdomyolysis and VICC showed a significantly increasing trend as the grade of severity increased (both P = 0.014) (Table 2). Bleeding complications occurred in four patients, three of whom had serious bleeding complications (one case of hemoperitoneum, two cases of gastrointestinal bleeding). The mean hospital length of stay was 2.30 ± 3.91 days.
Characteristics of the patients.
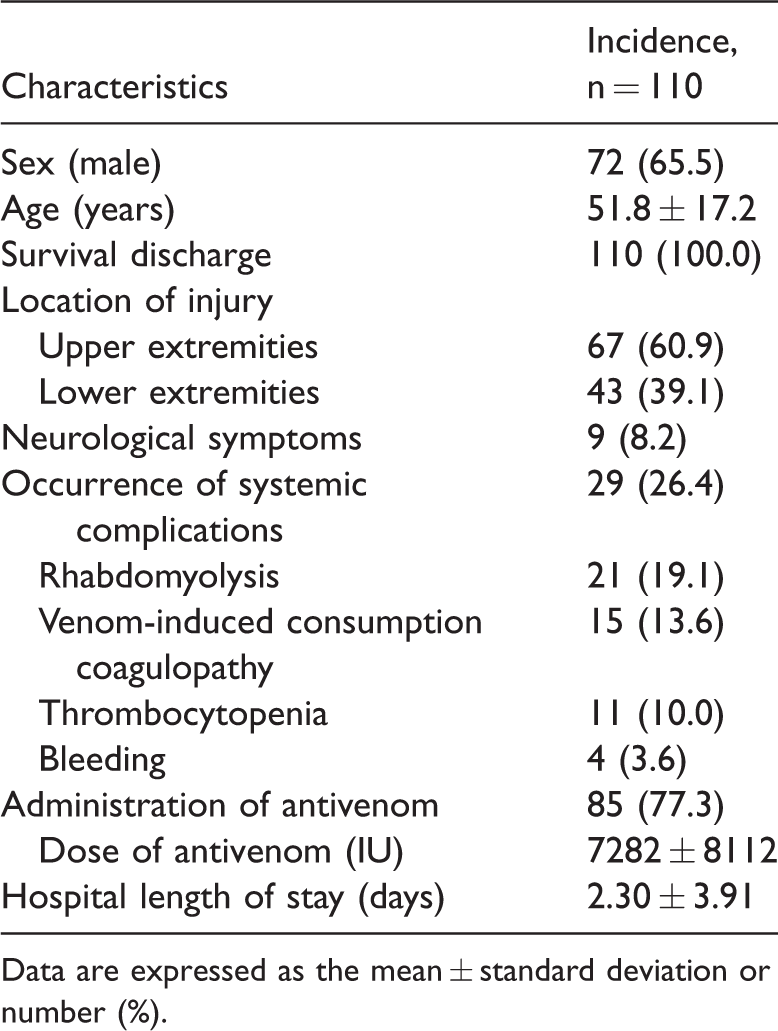
Data are expressed as the mean ± standard deviation or number (%).
Characteristics of the patients with snakebite injury according to grade classification for mamushi bites.

Data are expressed as the mean ± standard deviation or number (%). VICC: venom-induced consumption coagulopathy.
Efficacy of repeated antivenom therapy for treating snakebite-related complications
Of the 29 patients with complications, 20 received single antivenom therapy and the remaining nine patients were treated with repeated antivenom therapy. Table 3 shows the characteristics of the two groups. All patients in both groups survived and were discharged. There were no significant differences in sex, age, location of injury, and severity of grade between the two groups. However, the median length of hospital stay was significantly longer in those who received repeated antivenom therapy compared with those who received single antivenom therapy (P = 0.029).
Repeated antivenom therapy for treating snakebite-related systemic complications.

Data are expressed as the median (interquartile range) or number (%).
Discussion
Antivenom is the recommended standard treatment for snake envenoming. Antivenom is used to prevent aggravation of local swelling and to reduce hematological abnormalities and systemic envenoming. After an initial response to antivenom (cessation of bleeding, restoration of blood coagulability), signs of systemic envenoming may recur within 24 to 48 hours. 3 Recurrence of systemic envenoming is attributable to the following: 1) continued absorption of venom from the site of the bite; 14 2) redistribution of venom from the tissues into the vascular space as the result of antivenom treatment; 15 and 3) an insufficient dose of antivenom. 4 The 2016 World Health Organization guideline recommends repeating the initial dose of antivenom if the following criteria exist: 1) when the blood remains uncoagulable 6 hours after the initial dose of antivenom, the same dose should be repeated; 2) in patients who continue to bleed profusely, the dose of antivenom should be repeated within 1 to 2 hours; or 3) in case of deteriorating neurotoxicity or cardiovascular signs. 3
The characteristics of snakebite injury in Korea may vary. The signs of systemic envenoming are relatively rare, and there is a high risk of local complications.16,17 Most patients with hematological abnormalities rarely experience clinically life-threatening bleeding, and most recover without active bleeding sequelae after administration of antivenom. 18 Antivenom is usually sufficient to elicit a therapeutic effect on bleeding complications. 4 Therefore, close observation and monitoring are required to reduce the use of unnecessary antivenom. Consequently, we doubt the effectiveness of repeated antivenom therapy for snakebite-related systemic complications in Korea where the characteristics of the indigenous snakes are different. In the current study, repeated antivenom therapy for patients with snakebite-related complications was associated with a longer hospital stay than that of single antivenom therapy. Therefore, further studies on the effects of repeated antivenom therapy for treating systemic complications are required.
The antivenom used in Korea is not manufactured to reflect snakes that are indigenous to Korea. Only four species of snakes are poisonous in Korea. These include three species of the genus Gloydius (G. brevicaudus, G. saxatilis, G. ussuriensis) and one species of the genus Rhabdophis (R. tigrinus). 19 Kovax freeze-dried Agkistrodon antivenom was developed in horses against the species A. halys in China. 4 Compared with Agkistrodon, there are some common antigens between toxins of the Gloydius species, as well as cross-reactions with the venom of other snakes. 20 Although the antivenom developed against A. halys is effective for treating snakebite injury in Korea, it may not fully address the characteristics of snakebite injury in this country. Moreover, this antivenom cannot be used when the patient is bitten by the genus Rhabdophis because there is no cross-reaction. 4 Because different species of snakes inhabit different countries and regions, guidelines should be established regarding antivenom therapy that more accurately reflect regional characteristics of snakes.
The limitations of this study are as follows. First, this study included the results of only one Emergency Department and it was based on retrospective medical record review. The sample size was small, and there were insufficient factors to identify confounding variables to determine the association between the administration of antivenom and outcomes of patients. The study was underpowered, and it is not applicable to a wider population. Second, abnormal blood test results are an important indicator for evaluating and treating patients with snakebites. However, this study did not show an association of clinical symptoms with blood tests in patients. Third, although there was no significant difference in sex, age, location of injury, or severity of grade between single and repeated antivenom therapy, there were several uncontrolled factors (e.g., type of snakes and timing of antivenom administration and transfusion) that could have affected the patients’ outcomes.
Although there are various recommendations for treating venomous snakebites and administration of antivenom, the evidence for which snakebite treatment is effective is still weak for such practice. Larger and more rigorous prospective multi-institutional studies on appropriate management of venomous snakebites are necessary.
Conclusion
There does not appear to be any superiority of repeated versus single antivenom therapy, However, repeated antivenom therapy is associated with a longer hospital stay. The reasons for this finding remain unknown.
Footnotes
Authorship
Kang H, Kim C, and Yoo K contributed to the study design and data collection. Shin H and Oh J analyzed the data. Park KH and Shin H drafted the manuscript. Kang H, Choi HJ, and Lim TH contributed to editing of the manuscript. Shin H and Kang H take equal responsibility for the manuscript. All authors read and approved the final manuscript.
Availability of data and materials
The primary data used in the analysis can be provided if requested.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Human rights
The study protocol conforms to the ethical guidelines of the 1975 Declaration of Helsinki as reflected in a priori approval by the institution’s human research committee.
