Abstract
Objectives
We aimed to compare the effects of general anesthesia with combined epidural and general anesthesia in patients with early-stage non-small cell lung carcinoma (NSCLC).
Methods
Patients scheduled to undergo tumor resection with adjuvant chemoradiotherapy were eligible. Patients in the control group received general anesthesia during surgery, and those in the observation group received combined epidural and general anesthesia. The hemodynamic factors mean arterial pressure (MAP), heart rate, end-tidal carbon dioxide, and oxygen saturation were measured. Serum levels of pro-inflammatory cytokines interleukin (IL)-1, IL-8, high-sensitivity C-reactive protein (hs-CRP), and tumor necrosis factor (TNF)-α as well as β-endorphin were measured by enzyme-linked immunosorbent assay. Serum malondialdehyde (MDA) was measured using the thiobarbituric acid method.
Results
The incidence of specific adverse events was reduced and overall and disease-free survival were improved in the observation group compared with the control group. MAP was generally lower in the observation group compared with the control group, as were the serum levels of IL-1, IL-8, hs-CRP, TNF-α, and MDA.
Conclusions
Compared with general anesthesia, combined epidural and general anesthesia may inhibit the occurrence of short-term adverse events and improve long-term outcomes by inhibiting inflammatory responses in patients with early-stage NSCLC after tumor resection.
Keywords
Introduction
Although various treatment methods such as chemotherapy, radiation therapy, and targeted therapy have been developed for the treatment of malignancies, surgical resection remains the most effective and the only radical treatment, especially for patients with early-stage disease. 1 However, stress stimulations that arise during surgery may induce the abnormal synthesis of various inflammatory cytokines, thus inducing inflammatory responses, which can have a significant effect on both short-term adverse events and long-term treatment outcomes. 2 Apart from surgical trauma, anesthesia used during surgery can also induce inflammatory responses. Different types of anesthesia have been shown to influence the balance of inflammatory cytokines to varying degrees, 3 while general anesthesia including inhalational anesthetics, intravenous medications, or a combination of both have been found to modulate the immune system.4,5 For example, anesthetics may impact the neuroendocrine response related to the hypothalamal-pituitary-adrenal axis, thereby indirectly influencing the immune response via the secretion of immunomodulatory hormones such as glucocorticoids and catecholamines. 6 General anesthesia and combined epidural and general anesthesia are two commonly used types of anesthesia. Previous studies have shown that combined epidural and general anesthesia is superior to general anesthesia in modulating the immune system during surgical treatment of certain types of malignancies. 7 Moreover, studies on the effects of different types of anesthetics on the outcome or prognosis of cancer have been carried out in various types of cancer, including colon, ovarian, prostate, breast, and rectal cancer.8,9 Several retrospective studies have shown that, in comparison with general anesthesia, combined anesthesia is associated with better outcomes.10,11 These comprehensive evaluations of the impact of anesthetic regimens on the immune system can inform current perioperative management. However, the effects of these regimens during tumor resection in patients with early-stage non-small cell lung carcinoma (NSCLC) remain unclear. We therefore compared the effects of general anesthesia with combined epidural and general anesthesia in this patient population.
Materials and methods
Patients
Patients with early-stage NSCLC diagnosed by pathological examinations and imaging tests were enrolled from January 2010 to January 2012 at the Second People's Hospital of Banan District, Chongqing. All patients underwent thoracotomy and with voluntary propofol use. The ethics committee of the Second People’s Hospital of Banan District, Chongqing approved the study protocol (approval no. SPHBD200910013753), and all patients provided written informed consent prior to participation. All patients were followed for 5 years after surgery or until death. Criteria for inclusion in the study were as follows: WHO diagnosis of NSCLC, 12 TNM stage T1–2/N0 or non-hilar N1/M0; normal heart, liver, and kidney function; no prior surgery for NSCLC; willingness to adhere to the study protocol. The exclusion criteria were history of diabetes, hypertension, cardiovascular disease, or endocrine diseases; inability to undergo surgery; history of mental illness; other factor which in the investigator's opinion compromises the patient’s ability to participate in the study.
Grouping and method of anesthesia
Patients were randomized 1:1 to receive general anesthesia (control group) or combined epidural and general anesthesia (observation group). Patients in both groups had general anesthesia induced by intravenous administration of propofol (target plasma concentration 4 μg · mL−1), fentanyl (5 μg · kg−1), and rocuronium (0.8 mg · kg−1). Following orotracheal intubation, anesthesia was maintained using 1.5% to 3.5% sevoflurane. Anesthesia was monitored by bispectral index (BIS), which was maintained between 40 and 60, and fentanyl combined with propofol were used if necessary. In addition to general anesthesia, patients in the observation group first underwent epidural puncture between T8 and T10 and insertion of an epidural catheter. Lidocaine (3 mL, Jincheng Hayes Pharmaceutical Co., Ltd., Jincheng, China; approved H14023559) was administered via the epidural catheter, and block was achieved when anesthesia reached T4–T12. General anesthesia was subsequently performed, followed by epidural administration of 1% lidocaine (5–10 mL) and 0.375% ropivacaine (Guangdong Shunfeng Pharmaceutical Co., Ltd., Foshan, China; approval No.: H20050325) using a micro-pump at a rate of 5 to 8 mL/hour. Ramsay scoring was used to measure postoperative agitation at 0, 10, 20, and 30 min in the intensive care unit. Delayed recovery was measured using days of postoperative hospital stay. Visual analogue scale (VAS) scores were recorded at 6, 12, 24, and 48 h after surgery.
Measurement of hemodynamic factors
Mean arterial pressure (MAP), heart rate (HR), end-tidal carbon dioxide (PETCO2), and oxygen saturation (SpO2) were measured at Ta1 (immediately prior to anesthesia), Ta2 (immediately after intubation), Ta3 (10 min after initiation of surgery), and Ta4 (30 min after initiation of surgery).
Measurement of serum factors
Venous blood (5 mL) was collected from each participant at Tb1 (immediately prior to anesthesia), Tb2 (2 hours after initiation of surgery), Tb3 (immediately after surgery), Tb4 (24 hours after surgery), Tb5 (48 hours after surgery), Tb6 (72 hours after surgery), Tb7 (96 hours after surgery), and Tb8 (120 hours after surgery). Serum levels of pro-inflammatory cytokines interleukin (IL)-1, IL-8, high-sensitivity C-reactive protein (hs-CRP) and tumor necrosis factor (TNF)-α plus β-endorphin (EP) were measured by enzyme-linked immunosorbent assay (ELISA). Serum levels of malondialdehyde were measured using thiobarbituric acid.
Long-term outcomes
All patients were followed up for 5 years after surgery for the assessment of overall survival and disease-free survival, which was defined as survival without local, regional, or distant relapse.
Statistical analysis
All statistical analyses were performed using SPSS 19.0 software (SPSS Inc., Chicago, IL, USA). Measurement data were expressed as mean ± standard deviation (x¯ ± s). Student's t‑test was performed to compare two independent groups. Two-way ANOVA with a Bonferroni post-hoc test was used for group comparisons of hemodynamic factors, inflammatory cytokines, and levels of β-EP and MDA. Counting data were expressed as rate, and a χ2 test was used for comparisons between the control and observation groups. Values of P < 0.05 was considered statistically significant.
Results
Comparison of related information between two groups
A total of 149 patients were included in this study, of which 77 were male and 72 were female. There were 75 patients in the control group and 74 patients in the observation group. The mean patient age was 51±11.4 years (range 23–76 years). As shown in Table 1, no significant differences in age, gender, body mass index (BMI), T stage, or pathologic stage were found between the two groups. Furthermore, no significant differences in anesthesia time or surgical duration were found between the two groups. However, postoperative extubation time was significantly shorter in the observation group than in the control group (p < 0.05).
Comparison of patient characteristics between the control and observation groups.

Comparison of short-term adverse events between the two groups
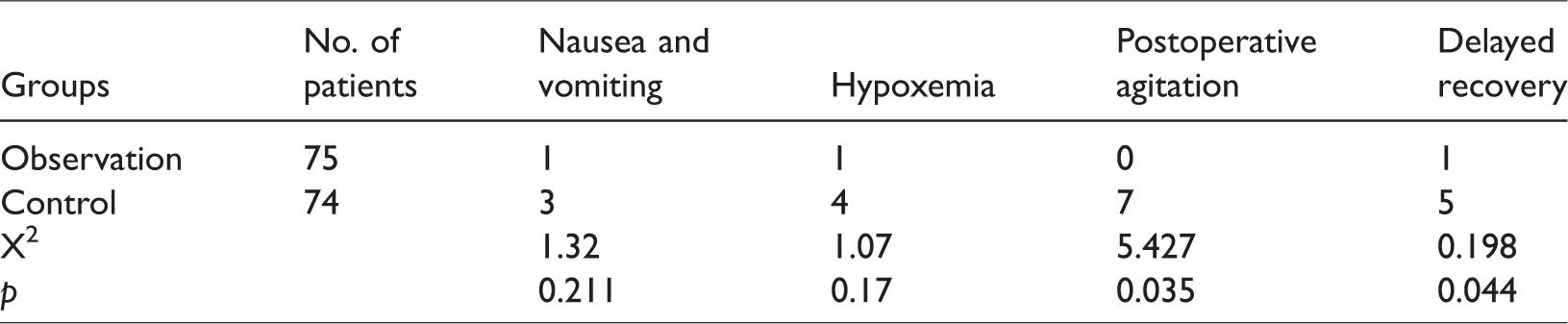
The occurrence of adverse events within 1 week after surgery was recorded during the real-time monitoring and in the nursing data for each patient, and was compared between the two groups. All AEs were coded using the Medical Dictionary for Regulatory Activities (MedDRA) version 17, and the severity of events was graded according to the Common Terminology Criteria of Adverse Events (CTCAE). As shown in Tables 2 and 3, no significant differences were observed between the groups in the incidence of nausea, vomiting, or hypoxemia. Moreover, compared with the control group, the incidence of postoperative agitation, delayed recovery (assessed as days of postoperative hospital stay), and VAS score were significantly reduced in the observation group. Those data indicate that combined epidural and general anesthesia may result in a reduced incidence of certain adverse events.
Comparison of short-term adverse events between the control and observation groups.

Comparison of visual analog scale score between the control and observation groups.

*p < 0.05: compared with control group.
Comparison of hemodynamic factors between the two groups at different time points
HR decreased significantly during surgery. Furthermore, an initial decrease in SpO2 was observed, followed by an increase at Ta4. No significant changes in PETCO2 were observed during the entire procedure. MAP increased initially, followed by a further increase at Ta3 and Ta4. No significant differences in HR, PETCO2, and SpO2 were recorded between the two groups before and during anesthesia. However, although there was no difference in MAP between the groups prior to anesthesia, MAP was significantly lower in the observation group than in control group at various time points during anesthesia (Figure 1).

Comparison of hemodynamic factors between the two groups at different time points.
Comparison of inflammatory cytokines between the two groups
As shown in Figure 2, there was no significant differences in the serum levels of IL-1, IL-8, hs-CRP, and TNF-α between the two groups prior to anesthesia. Serum levels of IL-1, IL-8, hs-CRP, and TNF-α were increased initially and then decreased in both groups. Although significant differences were not observed for all cytokines at all time points, serum levels of IL-1, IL-8, hs-CRP, and TNF-α were generally lower in the observation group than in the control group.

Comparison of serum inflammatory cytokine levels between the two groups.
Comparison of β-EP and MDA levels between the two groups
There were no significant differences in serum levels of β-EP and MDA between the two groups prior to anesthesia. The levels of β-EP and MDA increased after anesthesia and then decreased after surgery. Compared with the control group, serum levels of β-EP were significantly higher and serum levels of MDA significantly lower in the observation group compared with the control group at various time points during anesthesia (Figure 3).
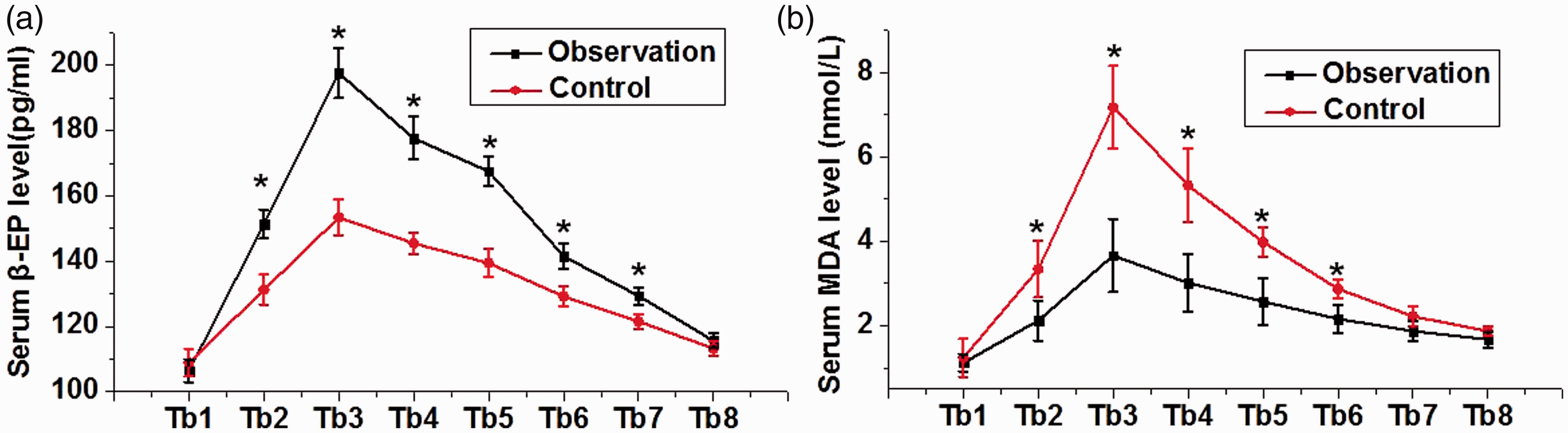
Comparison of serum β-EP and MDA levels between the two groups.
Comparison of long-term outcomes between the two groups
As shown in Table 4, both the overall survival rate and disease-free survival rate were higher in the observation group than in the control group, but the differences were not statistically significant. These data suggest that, compared with general anesthesia, combined epidural and general anesthesia has the potential to improve the prognosis of patients with early-stage NSCLC after tumor resection.
Comparison of long-term outcomes between the control and observation groups.

Discussion
NSCLC is the most common type of lung cancer, accounting for more than 85% of cases of lung cancer. 13 In recent year, an increased trend of NSCLC morbidity has been reported, which may potentially be attributable to changes in lifestyle and diet as well as increased air pollution. 14 In China, NSCLC is the second most prevalent among types of cancers, and is less prevalent than only breast cancer. 15 The overall 5-year survival of patients with advanced NSCLC is less than 15%. 16 Fortunately, surgical tumor resection is associated with improved outcomes in patients with early-stage NSCLC. 17 However, trauma during surgery may induce inflammatory responses, which can determine both short-term and long-term outcomes to a significant extent. 18 Furthermore, surgical trauma can cause hemodynamic instability, which in turn affects postoperative recovery. 19 In our study, MAP and serum levels of pro-inflammatory cytokines IL-1, IL-8, hs-CRP, and TNF-α increased during surgery, indicating the presence of inflammatory responses and hemodynamic instability. Anesthetic-induced activation of p38 MAPK has been implicated in proinflammatory cytokine release via the regulation of several inflammation-related genes, including TNF-α, IL-1β, and IL-6.20,21 In the present study, the combination of epidural and general anesthesia may therefore inhibit serum TNF-α, IL-1β, and IL-6 by decreasing p38 MAPK pathway activity. These results indicate that a combination of epidural and general anesthesia may reduce abnormal immune responses during NSCLC tumor resection, thus aiding recovery. It has previously been reported that surgical stress response was reduced and postoperative recovery was improved with the use of a fast-track surgery protocol. 22 Furthermore, the use of epidural anesthesia has been closely correlated with improved overall survival in patients with certain types of malignancies such as colon cancer, breast cancer, and ovarian cancer.23,24 Our data show that, although no significant differences were found, overall survival rate and disease-free survival rate were higher in the observation group than that in control group, indicating that compared with general anesthesia, the combination of epidural and general anesthesia may improve survival in patients with early-stage NSCLC after tumor resection. Moreover, previous studies have shown that the combination of epidural and general anesthesia is superior to general anesthesia alone because epidural anesthesia can block afferent neural transmission to prevent neuroendocrine stress responses. 25 Notably, the combination of epidural and general anesthesia can also inhibit cortisol secretion by reducing adverse stimuli-mediated hypothalamic-pituitary-adrenocortical excitation. 23 These findings are aligned with our data and indicate that the combination of epidural and general anesthesia may represent the optimal approach during early-stage NSCLC resection.
Levels of CRP, a non-specific acute-phase protein synthesized by the liver, are increased under conditions of trauma and stress, and postoperative CRP level may reflect the degree of surgical stress. 26 Our data indicated that hs-CRP and thus surgical stress may be reduced when using the combination of epidural and general anesthesia. IL-1 and IL-8 promote inflammatory responses in the pathogenesis of various human diseases. 27 Increased levels of TNF-α, another pro-inflammatory factor, have been associated with both higher inflammatory response and reduced immune function. 28 In the present study, although significant differences were not identified, serum levels of IL-1, IL-8, and TNF-α were generally lower in the observation group than in the control group, indicating that combined epidural and general anesthesia is superior to general anesthesia in inhibiting surgical stress-mediated inflammatory responses.
Hemodynamic instability induced by surgical stress is related to poor treatment outcomes. 29 In our study, HR, PETCO2, and SpO2 were not significantly different between the control group and the observation group during anesthesia. However, MAP was significantly lower in the observation group than in the control group at different time points after anesthesia. These data suggest that, compared with general anesthesia, combined epidural and general anesthesia may inhibit an increase MAP, thus maintaining hemodynamic stability. Our findings thus indicate that the combination of epidural and general anesthesia is superior to general anesthesia alone in inhibiting the occurrence of postoperative agitation and delayed recovery, which is consistent with the findings of Yang et al. 30 However, no significant differences in the incidence of nausea and vomitingor hypoxemia were found between the two groups, potentially because of variations in individual patient responses. Therefore, the assessment of these adverse reactions in future studies is required.
Conclusions
Combined epidural and general anesthesia appears to be superior to general anesthesia alone in preventing specific short-term adverse events, improving long-term survival, maintaining hemodynamic stability, and inhibiting surgical stress-mediated inflammatory responses in patients with early-stage NSCLC after tumor resection. However, further studies with larger sample sizes are needed to confirm these findings.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
