Abstract
Objective:
To investigate the long-term outcome of discectomy and relevant factors associated with clinical outcome.
Methods:
Patients who underwent lumbar discectomy by fenestration were evaluated retrospectively, using the Oswestry disability index (ODI; 0 - 20 minimal, 21 - 40 moderate, > 41 severe disability) and the Stauffer-Coventry criteria (‘excellent’, ‘good’, ‘fair’, ‘poor’) to measure clinical and radiographic outcomes.
Results:
Sixty patients (mean follow-up, 214 months) were included in the analysis. At final follow-up, patients were rated as ‘excellent’ (n = 31), ‘good’ (n = 13), ‘fair’ (n = 5) and ‘poor’ (n = 11) using the Stauffer-Coventry criteria; the latter group included six patients who underwent reoperations. The mean ODI score was 11.2. The height of the operative intervertebral space was significantly inversely correlated with the follow-up ODI value. Heavy manual work, smoking and a long duration of aggressive preoperative symptoms were significantly associated with unsatisfactory outcomes.
Conclusions:
The long-term outcome of lumbar discectomy by fenestration was satisfactory in the majority of patients. Heavy manual work, smoking and the duration of aggressive preoperative symptoms were negative predictors of a good clinical outcome.
Introduction
Lumbar discectomy as a treatment for herniated lumbar intervertebral discs was first reported in the 1920s. It is the most common surgical spine procedure to be performed in the USA. 1 Extensive published data indicate that surgical results are generally excellent; however, the success rate for lumbar discectomy ranges between 49% and 90%.2,3 This variability in clinical outcome emphasizes the importance of identifying preoperative factors that could predict outcome accurately, following lumbar discectomy. Studies indicate that clinical outcome after discectomy tends to be less positive with long-term follow-up.2,4,5
The development of spinal surgery and microsurgery has heralded a number of mini-invasive surgical techniques for lumbar discectomy, such as percutaneous lumbar discectomy, chemonucleolysis, percutaneous laser disc decompression and microendoscopic discectomy. Indications for these techniques are limited, however, and the devices are very expensive, making these procedures less desirable than more traditional approaches. A large number of lumbar discectomies are performed annually in the USA and Europe to treat disc herniation.1,6– 8 Open discectomy remains the most common surgery for lumbar disc herniation.
Long-term follow-up studies that explore clinical outcomes of lumbar discectomy by fenestration are rare. The present study investigated the long-term (> 15-year) outcomes following discectomy, and the relevant factors associated with surgical outcome.
Patients and methods
Study Population and Data Collection
This retrospective study, conducted in 2006, reviewed all single-level, first-time lumbar discectomies by fenestration performed at the Department of Orthopaedics, The First Affiliated Hospital of Soochow University, Jiangsu, China, between June 1986 and June 1991. Patients underwent discectomy if they met the following criteria: radicular pain or numbness in the lower extremity attributable to the disc level; unrelieved symptoms after ≥ 6 weeks' conservative treatment (including bed rest, nonsteroidal anti-inflammatory drugs or physical therapy); preoperative imaging clearly demonstrating lumbar disc herniation that could lead to clinical symptoms. All of the patients were contacted by mail to answer a detailed questionnaire that included the Oswestry Disability Index (ODI) 9 and items related to occupation, educational level, treatment satisfaction, pain relief in the leg and back, residual pain, ability to work, level of activity, reoperations, smoking, alcohol consumption and rehabilitation exercise. All patients had standard anterior–posterior and lateral radiographical assessments of the lumbar spine, along with dynamic flexion– extension lateral views. Patients who underwent laminectomy, hemilaminectomy or presented with concomitant spinal pathologies were excluded from the study. Patients who responded to the questionnaire were examined in the outpatient department. Two years later, the reliability of the questionnaire was assessed by resending it to all of the patients who had initially responded. Patients were excluded from the study if they reported substantial inconsistencies in their responses about their pre- and postoperative situations.
Study Assessments
The height of the operative intervertebral space (HIS) was measured using a method described previously. 10 The ratio of the HIS to the upper vertebrae body was measured on lateral radiographs using the method described by Mochida and Arima. 11 The flexion–extension radiographs were analysed for segmental stability using the angle between the endplates of the operative segment. Instability was defined when the angle in flexion differed ≥ 10° from the angle in extension.
The level of disability in the back was assessed using the ODI method,
9
and graded as minimal (score 0 – 20), moderate (21 – 40) or severe (> 41). The total results were then classified according to the Stauffer–Coventry evaluating criteria (Table 1).
12
Patients with
Stauffer–Coventry criteria, 12 used to determine clinical outcome for patients undergoing lumbar discectomy
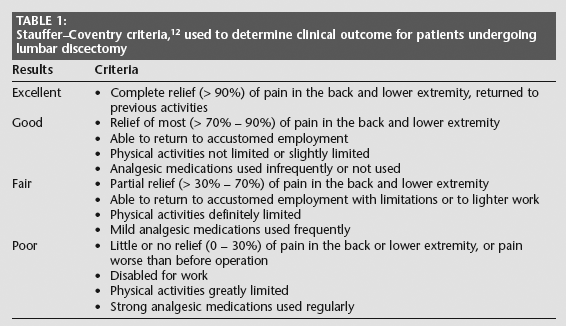
Occupational workload was divided into three categories according to the criteria of physical involvement needed: light work (office job); medium strenuous work (sales clerk, household tasks); heavy work (construction work, agriculture).
Patients were also classified according to education level (whether or not they had attended high school), sex, age, body mass index (BMI), alcohol consumption, surgical segment level, types of herniation, rehabilitation exercise and timing of follow-up.
Statistical Analyses
All analyses were conducted using SAS® software, version 9.2 (SAS Institute Inc., Cary, NC, USA). Descriptive statistics were expressed as mean ± SD for continuous variables, and as percentages for categorical variables. Student's t-test was used for analysis of continuous variables and the χ2-test was used for analysis of categorical variables. The relationship between the ODI value and the HIS was analysed using Pearson's correlation coefficient and logistic regression modelling. Corresponding 95% confidence intervals were calculated via confidence interval estimation. A P-value < 0.05 was considered to be statistically significant.
Results
In total, 65 patients responded to the questionnaire and were examined in the outpatient department. Two years later, the reliability of the questionnaire was assessed by sending the same questionnaire to all 65 patients. Five patients were excluded due to substantial inconsistencies in their responses about their pre- and postoperative situations. The remaining 60 patients had no such differences in their responses and were therefore included in the analyses.
Of the 60 patients included in the study, 37 (61.7%) were men and 23 (38.3%) were women, with a mean operative age of 38 years (range 21 – 64 years). The mean onset of preoperative pain was 56 months (range 2 – 116 months), and the mean follow-up period was 214 months (range 183 – 249 months).
Six patients required repeat back surgery, giving a reoperation rate of 10%. Reasons for reoperation were recurrent disc herniation at the same level (n = 3), recurrent contralateral disc herniation at the same level (n = 1), and recurrent adjacent lower level ipsilateral disc herniation (n = 2). Repeat operation was performed at a mean of 4.6 years (range 2 months to 14 years) after the first discectomy. At last follow-up, the mean ± SD ODI score of these six patients was 10.8 ± 4.6 compared with 11.3 ± 5.3 in the other 54 patients; there was no significant difference between the reoperation group and patients undergoing a single operation.
According to the Stauffer–Coventry criteria, 12 31 (51.7%) patients were rated ‘excellent', 13 (21.7%) were rated ‘good', five (8.3%) were rated ‘fair' and 11 (18.3%), who included the six reoperation patients, were rated ‘poor' at the last follow-up. On this basis, 44 (73.3%) patients were considered to have had a satisfactory outcome and 16 (26.7%) an unsatisfactory outcome, following discectomy.
At the time of last follow-up, the overall mean ODI ± SD score was 11.2 ± 13.3, with 50 patients (83.3%) classified with minimal disability (mean ± SD ODI of 6.3 ± 5.8), eight with moderate disability (mean ± SD ODI of 31.4 ± 11.52), and two with severe disability (mean ± SD ODI of 54.0 ± 18.69).
Before the operation, 15 patients (25.0%) were engaged in light work, 24 (40.0%) in medium strenuous work and 21 (35.0%) in heavy manual work. Occupational workload before surgery significantly influenced clinical outcome. Significantly more patients employed in light and medium work had a satisfactory outcome, compared with those employed in heavy work (P < 0.05; Table 2).
Relationship between occupation and clinical outcome according to Stauffer–Coventry criteria 12 in patients undergoing lumbar discectomy (n = 60)
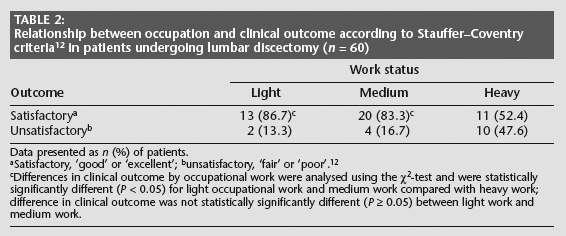
Data presented as n (%) of patients.
Satisfactory, ‘good' or ‘excellent';
unsatisfactory, ‘fair' or ‘poor'. 12
Differences in clinical outcome by occupational work were analysed using the χ2-test and were statistically significantly different (P < 0.05) for light occupational work and medium work compared with heavy work; difference in clinical outcome was not statistically significantly different (P ≥ 0.05) between light work and medium work.
The mean ± SD duration of severe preoperative symptoms in all patients was 76.7 ± 126.6 days (range 0 – 730 days). In patients with a satisfactory outcome, the mean ± SD duration of preoperative symptoms was significantly lower (47.6 ± 75.6 days [range 0 – 150 days]) than in patients with an unsatisfactory outcome (156.8 ± 193.2 days [range 97 – 730 days]); P < 0.05).
Of the 44 patients who were considered to have had a satisfactory outcome, eight (18.2%) were current smokers; of the 16 patients who were considered to have had an unsatisfactory outcome, seven (43.8%) were current smokers (P < 0.05, χ2-test).
At final follow-up, the mean ± SD HIS was 6.82 ± 2.23 mm and the mean ± SD ratio of the HIS to the upper vertebrae body was 0.27 ± 0.09.
Pearson's correlation coefficient showed a significant inverse correlation between HIS and the follow-up ODI value (γ = -0.416, P < 0.05). The equation of linear regression was ODI = 26.098 - 2.105 × HIS (P < 0.05), which demonstrated that the ODI value became smaller as the HIS increased, indicating improved back function in patients.
The difference in mean ± SD ODI values between patients with unstable lumbar spine segments (n = 10), according to lumbar spine flexion–extension lateral views, and patients with stable lumbar spine segments (n = 50) was not significant (12.0 ± 11.9 versus 9.5 ± 8.2, respectively). The stability of the lumbar spine was, therefore, not relevant to the clinical outcome.
Other factors including sex, age, BMI, educational level, alcohol consumption, surgical segment level, type of herniation, rehabilitation exercise and timing of follow-up were determined to be insignificant variables for clinical outcome, using logistic regression analysis.
Discussion
Although lumbar discectomy is still the most common surgery for disc herniation, the clinical outcome of the procedure is difficult to evaluate definitively. Different questionnaire designs have been used to evaluate the outcome of lumbar spinal surgery, but results vary by 37%. 13 Replicated testing shows the ODI system to have a very significant correlation between surgery and outcome, with a coefficient of correlation ranging between 0.90 and 0.99,14 – 17 and is a reliable and effective method for patients with back or leg pain. 14 The present study showed that the mean ODI score was 11.2 at the time of follow-up, with 83.3% of patients classified as minimally disabled; this indicated that back function and pain relief were satisfactory. The proportion of patients with a satisfactory outcome (73.3%) according to the Stauffer–Coventry criteria was similar to previous studies.18 – 20
As reported elsewhere,21,22 preoperative occupational workload is known to influence surgical outcome and residual symptoms significantly, with patients engaged in heavy manual work having significantly more functional disability compared with those engaged in light or medium-strenuous work. Heavy work increases flexion–extension and torsional movements of the lumbar spine, increasing load and shear forces on the spine that could lead to facet joint injury and disc degeneration. Some studies have reported no obvious relationship between occupational workload and clinical outcome; however, this may be related to different approaches to classifying workload and quantifying outcome.23,24
Several factors have been reported as predictive of a successful outcome following lumbar discectomy, including: male sex; age < 41 years old; duration of sciatica < 7 months; no previous lumbar surgery. 25 It has also been shown that surgical outcome is unsatisfactory in patients with preoperative leg pain associated with lumbar disc herniation for > 8 months, due to the fact that patients were unable to return to their previous work status. 26 The duration of severe preoperative symptoms in the present study had a significant impact on clinical outcome; a long duration of symptoms resulted in more severe nerve root lesions and poorer outcomes than a short duration of symptoms.
A rat model investigating the impact of smoking on intervertebral discs showed that smoking caused degenerative intervertebral disc disease. 27 This was attributed to the increased local production and release of inflammatory cytokines caused by tobacco smoke inhalation, which reduces chondrocyte activity.
Many studies attribute recurrent pain after discectomy to overloaded facet joints, due to a loss of height in the intervertebral disc.5,10,28,29 The loss of disc height increases the pressure on nerve roots and outer annular layers, leading to degeneration of facet joints as they compensate for the increased load. Similar results were evident in the present study: at long term follow-up, the intervertebral space was narrower after discectomy and the HIS was inversely correlated with the follow-up ODI value, which suggests that back function will improve if the HIS is maintained.
The impact of sex on clinical outcome remains controversial. There have been some reports that clinical outcome is less satisfactory in females compared with males,4,30 especially in L4 – L5 discectomy. 30 This might be due to sociological, biological or psychological factors affecting female patients. Other studies have reported better outcomes in females compared with males, however.23,31 Sex had no significant influence on surgical outcome in the present study.
In summary, the long-term outcome of single-level first-time lumbar discectomy by fenestration was satisfactory in the majority of patients. It is important to evaluate long-term effects following lumbar discectomy. The ODI is a useful tool to quantify subjective symptoms, whereas the HIS correlates with residual back or leg pain. Heavy manual work, smoking and duration of preoperative symptoms significantly influenced clinical outcome.
Footnotes
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
