Abstract
Objective
Use of a catheter lock solution plays a decisive role in vascular access. The effects of different concentrations of heparin and different types of catheter lock solutions are controversial. Therefore, this study aimed to compare the efficacy and safety of sodium citrate and sodium heparin catheter lock solutions.
Methods
A total of 120 patients were divided into four groups (30 patients per group) according to the use of catheter lock solution as follows: 6250 U/mL sodium heparin, 5000 U/mL sodium heparin, 2500 U/mL sodium heparin, and 4% sodium citrate. Coagulation function and the incidence of catheter occlusion, hemorrhage, and catheter-related infections were recorded.
Results
The different catheter lock solutions were significantly related to conduit blockage, hemorrhage, infection, and leakage levels. In the 4% sodium citrate group, the odds ratio was 0.688 for conduit blockage (95% confidence interval [CI], 0.206–2.297), 0.286 for hemorrhage (95% CI, 0.091–0.899), 0.266 for infection (95% CI, 0.073–0.964), and 0.416 for leakage (95% CI, 0.141–1.225) compared with the 6250 U/mL sodium heparin.
Conclusions
The solution 4% sodium citrate can effectively reduce the risk of catheter obstruction, bleeding, infection, and leakage better than sodium heparin in patients with long-term intravenous indwelling catheters.
Keywords
Introduction
Hemodialysis is an important treatment for acute and chronic renal failure and various toxic diseases. 1 Toxins are removed by dispersion, convection, and adsorption by means of a solute gradient and a water pressure gradient on both sides of the membrane. 2 Stable and reliable vascular access is an essential prerequisite for patients undergoing hemodialysis. Vascular access guarantees normal operation of hemodialysis treatment and forms a lifeline for maintaining hemodialysis. 3 Frequent puncture of a temporary catheter increases the infection rate in the catheter. Once infection occurs, it seriously hinders the treatment’s effect, even threatening the patient’s life. Because of an increase in older patients and other vascular diseases, a permanent central venous catheter is a good choice for promoting safe vascular access. Maintaining a central venous catheter’s patency is important and the type of catheter lock solution plays a decisive role. 4 The quality of sealing a catheter directly affects the establishment of vascular access, and thus the outcome of treatment and the quality of life of patients in the intensive care unit. Therefore, maintaining the patency of vascular access, ensuring adequate blood flow, and avoiding complications of vascular access are important. 5
Sealing catheters with an anticoagulant plays a role in establishing vascular access, hemodialysis treatment, and preventing complications.6,7 At present, commonly used catheter lock solutions in clinical practice include heparin and sodium citrate. Heparin has several important functions. 8 These functions include enhancing the affinity between antithrombin III and thrombin, and accelerating inactivation of thrombin, 9 inhibiting adhesion and aggregation of platelets, 10 enhancing the activity of protein C, and stimulating vascular endothelial cells to release anticoagulant and fibrinolytic substances. 9 Heparin also has anti-inflammatory and anti-allergic effects. However, heparin overflow can increase the risk of systemic anticoagulation. 11 Therefore, finding a safe and effective alternative catheter lock solution is required.
With the increasing use of sodium citrate anticoagulation in continuous hemodialysis, it has also received attention as a catheter lock solution. Starch substances are fermented to form citric acid, and then neutralized with alkaline substances to produce sodium citrate, which has many excellent properties. 6 Importantly, citrate and calcium ions can form soluble complexes that can be used as anticoagulants and blood transfusion agents to preserve and process blood products.
Studies have shown that sealing catheters with sodium citrate can reduce the incidence of catheter-related bloodstream infections, while reducing the risk of bleeding in patients. 12 Therefore, this study was designed to analyze the clinical data of patients who received hemodialysis treatment in the intensive care unit, which used different catheter lock solutions (6250 U/mL sodium heparin, 5000 U/mL sodium heparin, 2500 U/mL sodium heparin, and 4% sodium citrate). We aimed to examine the sealing effect of different concentrations of heparin and sodium citrate and provide more references for clinical application.
Material and methods
Ethics statement
The research conformed to the Declaration of Helsinki and was authorized by the Human Ethics and Research Ethics Committees of the Fourth Hospital of Hebei Medical University. Informed consent was obtained from all participants.
Patients
From January 2009 to December 2016, a total of 120 patients were selected to be studied who underwent long-term (≥3 months) hemodialysis in the intensive care unit of the Fourth Hospital of Hebei Medical University. The sample included 90 men and 30 women whose ages ranged from 25 to 89 years and who were a mean age of 52.4 ± 14.3 years. There were 44 cases of septic shock after the operation, 26 cases of postoperative rectal cancer complicated by sepsis, 14 cases of postoperative gastric cancer with abdominal infection, 16 cases of acute severe pancreatitis, 10 cases of acute organophosphorus poisoning, and 10 cases of chronic bronchitis with multiple organ dysfunction syndrome.
Patients were included if they 1) had a central venous catheter, 2) had normal coagulation function and no bleeding tendency before catheterization, and 3) had chronic renal failure (combined with anuria or serum creatinine levels ≥707 µmol/L, serum potassium levels >6.5 mmol/L, or metabolic acidosis). The exclusion criteria were 1) an allergy to the catheter lock solution, 2) abnormal coagulation function, 3) hypothrombocythemia, and 3) a high bleeding risk, with a recent history of surgery or subarachnoid hemorrhage.
Groups and procedure of catheter lock
The subjects were divided into four groups according to different catheter lock solutions as follows: 6250 U/mL sodium heparin (12500 U/2 mL; Nanjing Xinbai Pharmaceutical Co., Ltd., Nanjing, China), 5000 U/mL sodium heparin, 2500 U/mL sodium heparin, and 4% sodium citrate (Nanjing Xinbai Pharmaceutical Co., Ltd.). These concentrations of solutions have been cited in previous studies.6,7 Additionally, 6250 U/mL sodium heparin, 5000 U/mL sodium heparin, and 2500 U/mL sodium heparin are frequently used concentrations of catheter lock solutions in clinical practice. The catheterization and sealing methods were the same for all four groups. After regular disinfection and surgical draping, 2% lidocaine anesthesia was applied. The intensive care unit physician then inserted a large-diameter, single-needle, double-cavity catheter (model: 12Fr 16 cm; ARROW Company, New York, NY, USA) in the femoral vein, while attempting to avoid blood vessel damage. For difficult insertions, the catheter was inserted under the guidance of B-ultrasound. Finally, the success or failure of catheterization was recorded, and the catheter was secured with sutures and covered with a sterile dressing.
Before hemodialysis, a 5-mL disposable syringe was used to draw back the liquid in each cavity of the catheter, to check whether the catheter was unblocked. A 20-mL 0.9% sodium chloride solution was then used to flush the two cavities in a pulsed manner. The blood was connected to a blood filter (model: Prismaflex, AN-69 membrane blood filter and M-100 pipeline; Fresenius Kabi, Baden Humboldt, Germany) for hemodialysis treatment. After the end of hemofiltration, pulsed positive pressure was used to seal the catheter. When the catheter was closed again, the stock solution was taken out. The physician observed whether the catheter was unobstructed. The residual blood in the lumen of the catheter was thoroughly washed with 20 mL of a 0.9% sodium chloride solution. A volume of 2 mL of the corresponding concentration of catheter lock solution was then injected into the arterial and venous cavities of the catheter under positive pressure, and the catheter was sealed every 8 hours. Finally, the heparin cap was screwed on. All operators received standardized training, followed strict aseptic operation principles, and recorded the sealing process and observation period indicators in detail.
Indicators for further observation
The following variables were recorded. (1) Indicators of coagulation function were determined after treatment. Four hours after sealing catheters, peripheral venous blood samples were collected to detect the activated partial thromboplastin time (APTT), prothrombin time (PT), coagulation thrombin time (TT), fibrinogen (FIB), and international normalized ratio (INR). (2) Conduit blockage was identified. The criteria for conduit blockage were unobstructed suction because of coagulation at the arteriovenous end of the catheter or without hemodialysis and no improvement, even after adjusting the catheter position and repeated suction with heparin saline. (3) Hemorrhage was defined as oozing or hematoma at the central venous catheter. (4) The patients were determined as having infection if they had the following: symptoms, such as chills and fever, during the initial stage of hemodialysis or non-hemodialysis, and there was no other cause; blood culture of the catheter was positive; and local skin of the tube showed red, swollen, painful, and purulent secretions; and other inflammatory manifestations. Any of these criteria were used to determine infection. (5) Leakage was defined as when the sealing liquid leaked within 48 hours.
Statistical analyses
The data are expressed as the percentage of the total or mean ± standard deviation. The Student’s t-test was used to determine statistical significance when two groups were compared. One-way analysis of variance was performed when three groups were compared.
Pearson’s chi-squared test was used to determine associations between the different measures for catheter locking and clinicopathological variables. To identify residual distribution, a histogram was created and the Shapiro–Wilk test was conducted. We concluded that residuals well modeled a normal distribution. The Wilcoxon signed-rank test was performed to compare clinicopathological variables. Univariate logistic regression analysis was used to calculate the odds ratios (ORs) of each variable for different measures for catheter locking. All statistical analyses were conducted using SPSS software, version 23.0 (IBM Corp., Armonk, NY, USA). A p value < 0.05 was considered statistically significant.
Results
Associations of different measures for catheter locking with clinicopathological variables
Associations between different measures for catheter locking and clinicopathological variables are shown in Table 1. No significant correlations were found between different measures for catheter locking and other clinicopathological variables, including APTT, PT, TT, FIB levels, and the INR (Figure 1). The rate of conduit blockage in the 4% sodium citrate group was significantly lower than that observed in the other groups (P < 0.001) (Table 1, Figure 2a). In the 4% sodium citrate group, the rate of hemorrhage was significantly lower than that in the other groups (P < 0.001) (Table 1, Figure 2b). In the 4% sodium citrate group, infection (P = 0.001) and leakage levels (P < 0.001) were significantly lower than those in the other groups (Table 1, Figure 2c, 2d).

Relative quantity of indicators of coagulation function among different groups.

Occurrence of catheter-associated complications in relation to different measures for catheter locking. (a) Conduit blockage; (b) hemorrhage; (c) infection; (d) leakage.
Clinicopathological variables and different measures for catheter locking.

Pearson’s chi-squared test was used for analysis. APTT: activated partial thromboplastin time; PT: prothrombin time; TT: thrombin time; FIB: fibrinogen; INR: international normalized ratio.
Univariate logistic regression for proportional hazards analysis of different catheter locking solutions and clinicopathological variables
Table 2 shows the univariate ORs and 95% confidence intervals (95% CIs) for the clinicopathological variables of individuals. The OR for conduit blockage was 0.688 (95% CI, 0.206–2.297) in the 4% sodium citrate group, 4.125 (95% CI, 1.387–12.270) in the 5000 U/mL sodium heparin group, and 6.417 (95% CI, 2.084–19.755) in the 2500 U/mL sodium heparin group compared with the 6250 U/mL sodium heparin group (P < 0.001). The OR for hemorrhage was significantly lower in the 4% sodium citrate group than in the 6250 U/mL sodium heparin group (0.286, 95% CI, 0.091–0.899, P < 0.001). Subjects in the 4% sodium citrate group also had a significantly lower risk of infection than did subjects in the 6250 U/mL sodium heparin group, with an OR of 0.266 (95% CI, 0.073–0.964, P = 0.002). The OR for leakage was significantly lower in the 4% sodium citrate group than in the 6250 U/mL sodium heparin group (0.416, 95% CI, 0.141–1.225, P = 0.001). However, there was no significant disadvantage of the different catheter locking methods for APTT, PT, TT, FIB, and INR values.
Different measures for catheter locking and their effect on clinicopathological variables based on univariate logistic regression analysis.
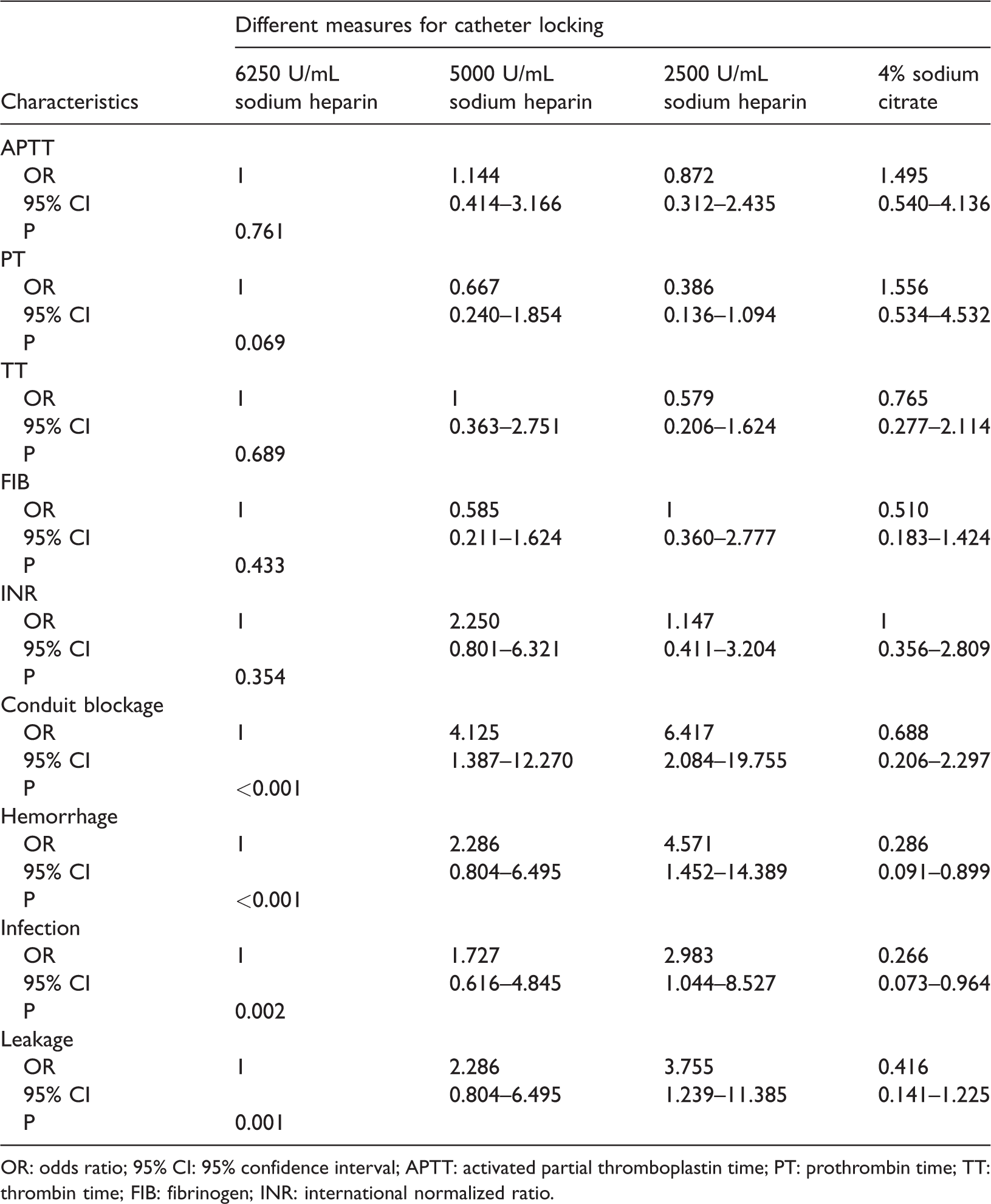
OR: odds ratio; 95% CI: 95% confidence interval; APTT: activated partial thromboplastin time; PT: prothrombin time; TT: thrombin time; FIB: fibrinogen; INR: international normalized ratio.
Discussion
Our study showed that there was no significant difference in the coagulation function (APTT, PT, TT, FIB, and INR) of patients in each group after the use of different concentrations of heparin and sodium citrate. The risks of conduit blockage, hemorrhage, infection, and leakage were significantly reduced with 4% sodium citrate compared with sodium heparin.
Conduit blockage and bleeding from a central venous catheter are difficult problems for patients on hemodialysis and medical staff, mainly due to dysfunction of the body’s coagulation and anticoagulant systems. Heparin can interfere with many aspects of the coagulation process and has anticoagulant effects in vivo and in vitro. 13 The mechanism of heparin is complex, mainly through an antithrombin III combination, which it enhances to activate antithrombin II, IX, XI, and XII. The inhibitory effect of clotting factors and its consequences are involved in preventing platelet aggregation and destruction, inhibiting the formation of prothrombin activators, blocking prothrombin into thrombin formation, and inhibition of thrombin. This process then prevents formation of fibrinogen to fibrin, which plays a role in anticoagulation. 14 This process affects the whole body’s coagulation function, which may lead to coagulation disorders in the later stage and induce thrombosis or bleeding. 15
The anticoagulation mechanism of sodium citrate is that calcium ions in the blood that are chelated by citrate generate soluble complex calcium citrate, which is difficult to dissociate. This results in reduction of active calcium ions in the blood to prevent prothrombin from being transformed into thrombin, thus achieving the purpose of anticoagulation. 16 Citric acid enters the human body and participates in the tricarboxylic acid cycle in the liver. Citric acid can be quickly metabolized into bicarbonate without any residual effects. 17 Using sodium citrate for local anticoagulation does not produce systemic anticoagulant effects, and can reduce the bleeding tendency of the whole body compared with common heparin. Additionally, sodium citrate has good biocompatibility and it does not inhibit the expression of adhesion molecules or lead to a decline in white blood cells and platelets. 6 Therefore, the risk of blockage and bleeding due to sodium citrate sealing is relatively small.
Catheter-associated bloodstream infection refers to bacteremia or fungalemia in patients with intravascular catheters or catheter removal within 48 hours, and results in fever (>38°C), chills, or hypotension. 18 There are no other infections with a clear source other than vascular catheter infection. Studies have shown that up to 40% of patients on hemodialysis have experienced catheter-related bloodstream infections. 19 These infections are closely associated with the operator’s catheterization technique, device material, type of sealing fluid, and formation of biofilm in the catheter cavity. 20 Heparin cannot inhibit formation of biofilm in the lumen of a catheter, and it cannot prevent adhesion and colonization of pathogenic bacteria in the lumen. However, sodium citrate has good antimicrobial properties, and sodium citrate with a concentration of >0.5% has the function of aggregating the antimicrobial membrane and killing colonies, such as staphylococcus. 21 Therefore, sodium citrate is superior to heparin in preventing catheter-related infections.
Most patients with severe hemodialysis have complicated conditions, and there are many potential risks of catheter blockage, bleeding, and infection. Traditional heparin anticoagulation is risky for such patients and may even aggravate their complications, while an increasing amount of research has shown that citric acid is more reliable in patients on hemodialysis.7,22,23 A sodium citrate injection has the same advantages as other catheter lock solutions in a central venous catheter. From an economic point of view, use of sodium citrate injection as the sealing fluid is convenient and affordable, potentially reducing medical expenses. The application range of sodium citrate in patients on continuous renal replacement therapy will increase, which will lead to a wide range of options.
Our results have some similarities with previous findings. A previous study 7 showed that, in patients who underwent long-term hemodialysis, a lock solution of 4% sodium citrate was associated with fewer catheter-related infections, but had similar effectiveness to heparin. Furthermore, Abdel Azim et al 6 found that 4% sodium citrate might help prevent catheter-related infections because of its additional antiseptic properties compared with heparin. Citrate-based locking solutions are a promising alternative to unfractionated heparin as a locking solution for dialysis catheters.
Conclusion
In conclusion, 4% sodium citrate used for central venous catheter sealing can reduce the occurrence of catheter blockage, bleeding, and catheter-related bloodstream infections compared with sodium heparin. Our findings offer good security and provide clinical reference for selection of catheter lock solutions for central venous catheters. Our study had a small sample size and was not a randomized, controlled study Therefore, further studies are required to determine the optimal concentration and efficacy of sodium citrate and heparin.
Abbreviations
Activated partial thromboplastin time (APTT); prothrombin time (PT); coagulation thrombin time (TT); fibrinogen (FIB); international normalized ratio (INR); odds ratio (OR); 95% confidence interval (95% CI).
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
