Abstract
Objective
This study was performed to introduce a new method of minimally invasive subtalar arthrodesis (MISA) and assess its clinical effects on traumatic subtalar arthritis (TSA).
Methods
Fifteen patients (8 male and 7 female; age range, 36–56 years; mean age, 48.67 years) with TSA who underwent MISA were included. All patients were treated using a series instrument. The intraoperative and postoperative indexes were recorded.
Results
Among all patients, the mean operation time was 59.67 ± 16.31 minutes and the mean intraoperative blood loss was 43.33 ± 52.87 mL. Four patients underwent iliac crest bone graft surgery, and one patient developed a complication involving fat liquefaction of the iliac crest wound. The mean bony fusion time among all patients was 3.5 months. According to the American Orthopaedic Foot and Ankle Society standard, an excellent outcome was obtained in eight patients and a good outcome was obtained in seven patients. The operation time and intraoperative blood loss were significantly different between patients who did and did not undergo iliac crest bone graft surgery.
Conclusion
MISA is a simple and effective method for the treatment of TSA.
Introduction
The subtalar joint has a complex anatomical structure and plays an important role in varus–valgus movement. 1 A long-term risk of traumatic subtalar arthritis (TSA) still exists after surgery and conservative treatment, resulting in walking-related pain or weight-bearing pain and other symptoms that can affect patients’ quality of life. 2 Four main methods for treatment of calcaneal fractures are currently available: conservative treatment, open reduction and internal fixation, minimally invasive fixation, and early subtalar arthrodesis. 3 However, all non-fusion treatments are likely to result in TSA. 4 A series of clinical studies on TSA caused by intra-articular calcaneal fractures showed that subtalar arthrodesis was an effective treatment that did not increase the risk of degeneration of the adjacent joints.1,5 However, several studies have suggested that subtalar joint fusion can lead to asymptomatic tarsal bone arthritis, degeneration, and limited joint motion. 6
Various types of incisions are currently used for subtalar joint arthrodesis, including lateral incisions such as an arc incision across the tarsal sinus, an oblique incision from the lateral malleolus point to the fourth metatarsal, and the traditional L-shaped incision.5,7 Selection of the most appropriate incision is based on any previous surgeries, the soft tissue condition, and any internal diseases. A lateral incision and iliac crest bone graft are usually applied in conventional subtalar arthrodesis.5,8 Previous studies have suggested that conventional subtalar arthrodesis with three types of lateral incisions has a satisfactory therapeutic effect; however, because the lateral incision is relatively large, the skin condition is poor, and an adequate blood supply is lacking, this technique may still be associated with complications such as incision infection, nerve or vascular injury, and delayed union. 9 Other incisions such as those used in the posterior approach, plantar approach, and medial approach have the same disadvantage of large surgical trauma.
The present study was performed to investigate the clinical effects of a new method of minimally invasive subtalar arthrodesis (MISA) with a series instrument that does not require arthroscopy and avoids the complications associated with the conventional lateral incision in patients with TSA.
Materials and methods
Patients
This study was approved by the local Ethics Committee of The Third Hospital of Hebei Medical University, and all participants provided informed consent. Patients with TSA who underwent MISA with a trephine from July 2011 to July 2014 were enrolled. The inclusion criteria were as follows: 1) a history of type I, II, or III calcaneal fracture according to the Zwipp classification; 2) no accompanying severe deformity after early surgical treatment; 3) subtalar joint pain affecting normal daily life; and 4) normal or mildly deformed calcaneal morphology, uneven subtalar joint surface, subchondral sclerosis of the articular surface, and hypertrophy of the joint edge as shown by radiographs or computed tomography (CT). The exclusion criteria were as follows: 1) type V calcaneal malunion according to the Zwipp classification, 2) more than one joint fusion, 3) treatment with drugs that might impact fracture healing and functional scores, and 4) peripheral bone fusion and joint trauma that affect the functional score.
Surgical technique
All surgeries were performed by the same surgeon with two assistants. Figure 1 shows the series instruments that were used in the surgeries. The patients were placed in the prone position after combined spinal and epidural anesthesia. A pneumatic tourniquet (300 mmHg) was applied around the mid-thigh. The specific surgical technique was as follows. First, a 2-cm longitudinal incision was made in the outer edge of the Achilles tendon and above the calcaneal tuberosity (Figure 2(a)). The subcutaneous tissue was retracted bilaterally by a mosquito clamp, avoiding the small saphenous vein, sural nerve, and other tissues. The subtalar joint surface was confirmed by advancing a needle through the posterior articular surface and tarsal sinus to the middle tarsal joint under the guidance of C-arm fluoroscopy (Figure 2(b)). Next, a core was drilled to the subtalar joint along the needle and the joint space was entered as confirmed by C-arm fluoroscopy. A cannulated trephine was then inserted and screwed into the joint, and its depth did not extend beyond the tarsal sinus level; the trephine was removed when the hole seemed satisfactory based on radiographic examination (Figure 2(c)). Maintaining the trephine in a stable position was helpful to distinguish the articular surface of the talus from that of the calcaneus. The columnar bone was harvested when the drilled core could be pushed like a syringe (Figure 3(a)). Gross examination of the columnar bone showed hardened bone substance and edges of articular cartilage and/or normal bone substance (Figure 3(b)). The medial and lateral angle was adjusted to 20° to 25° and the subtalar joints were drilled as described above, thus maximizing the fusion area. If patients presented with a prominent lateral mound, a tunnel was drilled along the lateral face of the calcaneus to reduce the calcaneal width (Figure 3(c)). Finally, we evaluated the fusion area of the subtalar joint and removed the soft tissue from the columnar bone, and the remaining bone was used for a bone graft. The soft tissue was removed by hemostatic forceps and a scalpel under direct vision. The next procedure involved insertion of the bone graft sleeve into the joint gap along the drill path, implantation of the remaining bone into the drill tube, and consolidation with a bone graft stick (Figure 4(a)). If the bone quantity was inadequate, iliac crest graft surgery was necessary. Finally, we performed compression osteosynthesis with two cannulated screws (6.5 mm × 60–70 mm) (Figure 4(b)). The incision healed well after the operation (Figure 4(c)).

Pictures of the series instruments. ① Bone graft sleeve. ② Trephine. ③ Drilled core. ④ Orientation needle. ⑤ Bone graft stick. (These instruments were personally made by the doctor.)

Clinical pictures of surgical technique. (a) A 2-cm longitudinal incision was made on the outer edge of the Achilles tendon above the calcaneal tuberosity. (b) The needle was punctured into the joint. (c) A hole was drilled to the subtalar joint along the needle, and the drilled core was observed under radiographic guidance.

The condition of the bone column and deformity. (a, b) The bone column was well. (c) The deformity of the prominent lateral mound was recovered.

Fixation was performed with two cannulated screws. (a) The bone graft sleeve was inserted into the joint gap along the drill path. (b) Compression osteosynthesis was performed with two cannulated screws. (c) The incision healed well postoperatively.
Clinical evaluation
All surgical information was recorded, including the operation time, bleeding volume, and rate of iliac crest graft surgery. The operative time was defined as the time from cutting the skin to stitching the wound and was obtained from the operation notes in the patients’ medical records. The bleeding volume was the volume of blood in the drainage apparatus and the estimated amount of blood contained in the gauze after the operation. Postoperatively, all patients performed active ankle exercises on postoperative day 2, remained non-weight-bearing for 6 weeks, and then were allowed to perform partial-weight-bearing ambulation with a walking aid for the following 6 weeks. All patients were allowed to perform full-weight-bearing walking 12 weeks after the procedure. The patients were clinically and radiographically followed up at 1, 3, 6, 12, and 24 months after surgery (Figure 5). The postoperative data collected included complications, the fusion area (determined by lateral and axial radiographs or CT scans), and American Orthopaedic Foot and Ankle Society (AOFAS) scores. 10
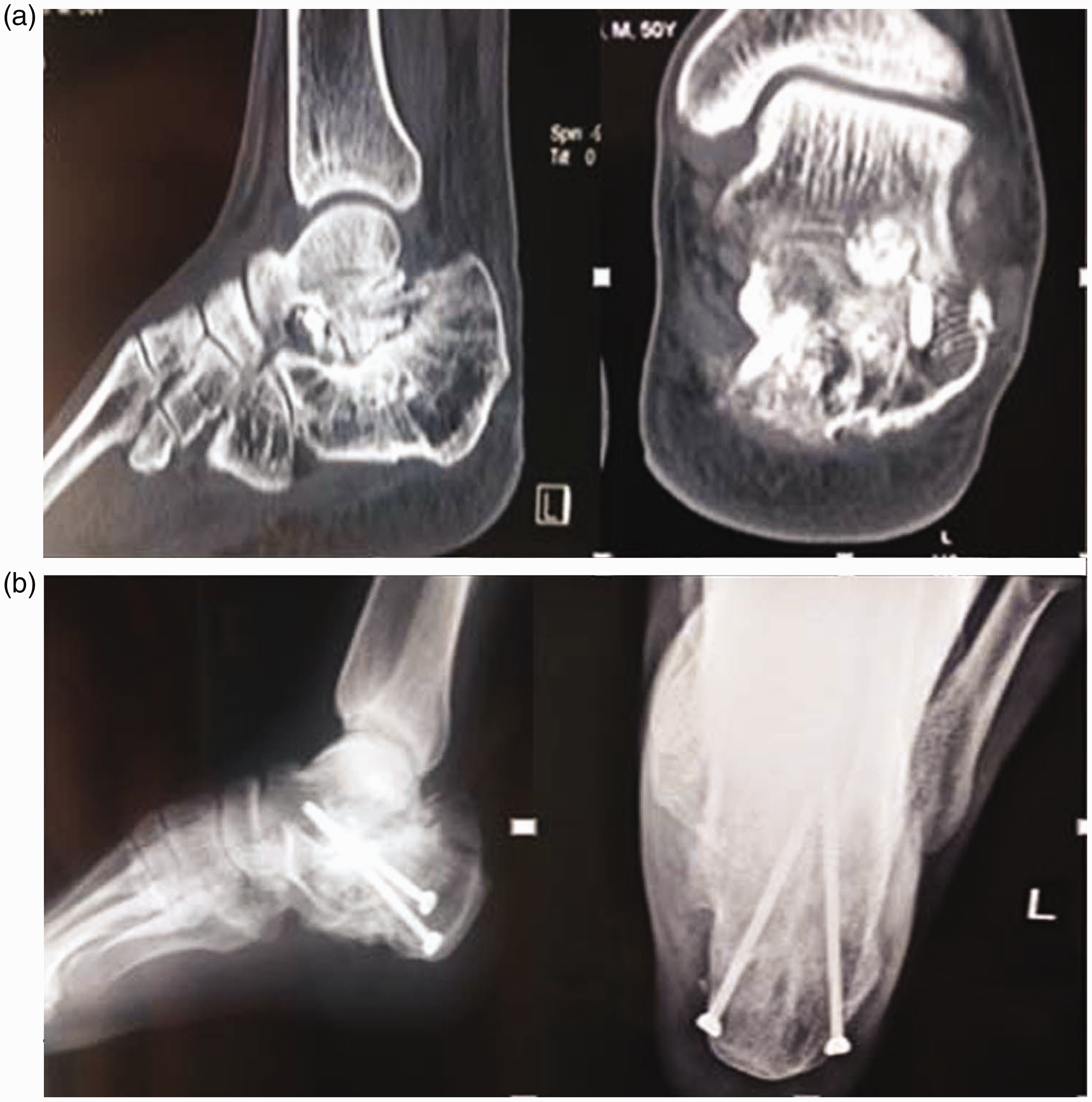
Postoperative radiographic inspection. (a) Computed tomography image of the subtalar joints after the operation. (b) One year after surgery, the subtalar joints achieved bony healing.
Statistical analysis
All data were analyzed using SPSS 19.0 statistical software (IBM Corp., Armonk, NY, USA). The results are expressed as mean ± standard deviation, and significant differences were determined by Student’s t-test. Pearson’s chi-squared test was used to compare categorical variables. Statistical significance was accepted for P-values of <0.05.
Results
Fifteen patients (15 feet) with TSA were enrolled in this study. Table 1 shows the baseline and follow-up data of every patient, including sex, age, operation time, blood loss, iliac grafting, complications, bone fusion, and AOFAS score. The patients comprised eight men and seven women with a mean age of 48.67 ± 5.11 years (range, 36–56 years), mean operation time of 59.67 ± 16.31 min (range, 40–85 min), and mean intraoperative blood loss volume of 43.33 ± 52.87 mL (range, 10–150 mL). Four patients (6.7%) required iliac crest bone graft surgery, and one patient developed a complication involving fat liquefaction at the iliac crest wound. The mean follow-up period was 21 months (range, 12–34 months). All posterolateral incisions healed smoothly in an average of 10 to 12 days. Bone fusion was confirmed in all patients within 3.5 months (range, 2–4 months) after the surgery. According to the AOFAS standard, an excellent outcome was obtained in eight patients and a good outcome in seven patients.
Baseline data of all patients.

F/M, Female/Male; Y/N, Yes/No.
Tables 1 and 2 show the data of four patients who underwent iliac crest bone graft surgery with a mean blood loss of 125 ± 28.87 mL (range, 100–150 mL), mean operation time of 83.75 ± 4.79 minutes (range, 40–85 minutes), and mean age of 49 ± 5.60 years (range, 44–56 years). The other 11 patients who did not require iliac crest bone graft surgery had a mean blood loss of 13.64 ± 5.05 mL (range, 10–20 mL), mean operation time of 50.91 ± 7.01 minutes (range, 40–60 minutes), and mean age of 48.55 ± 5.20 years (range, 36–56 years). In addition, the operation time and intraoperative blood loss were significantly different between patients who did and did not undergo iliac crest bone graft surgery (P < 0.01). In brief, Table 2 shows that MISA was associated with a lower autogenous iliac bone extraction rate and more sufficient bone recovery than the traditional surgical methods.
Comparison of patients with and without an iliac graft.

**P < 0.01.
Discussion
Previous research on the complications of TSA has focused on arthroscopy and other techniques such as multidetector CT imaging, a posterior two-portal approach, and a posterior three-portal arthroscopic approach. Eid et al. 11 researched a method of minimally invasive, no-hardware subtalar arthrodesis with a percutaneous posterolateral approach for treatment of patients with TSA and found that this technique could decrease the morbidity associated with late complications of calcaneal fracture. However, effective utilization of the subtalar joint bone was not achieved because it was mushily drained away along the tunnel. Furthermore, the method was only locally minimally invasive; it did not avoid trauma and the risks of autogenous grafts, and it still relied on arthroscopy. In the present study, we used the trephine to make an incision via the posterior-lateral approach, which is similar to the report by Eid et al. 11 This avoided the lateral area of the calcaneus, where the tissue lacks a blood supply and complications readily occur. At the outer edge of the tendon, this approach induces no damage to the lateral area, sural nerve, or small saphenous vein structures. All incisions healed smoothly without early complications. According to these results, MISA indeed reduced trauma and the complication rate.
The mean area of the posterior subtalar surface was about 667.3 mm2. Wu et al. 12 explored the use of a posterolateral incision in subtalar joint arthrodesis. They used a 12-mm dynamic hip screw to drill the joint and concluded that the dynamic hip screw with a slant angle of 25° could achieve talus union area of 433 ± 19 mm2 and calcaneus union area of 515 ± 19 mm2, accounting for 64.3% and 76.1% of the posterior talar surface, respectively. In the present study, we used the trephine (12-mm outer diameter and 10-mm inner diameter) to dill the articular surface at the tarsal sinus level as described by Wu et al. 12 and achieved maximization of the fusion area. The method with the trephine ensured removal of the required depth and area of subchondral bone and preserved the articular surface of the calcaneus and talus side of the subtalar joint. We were able to visually evaluate the joint fusion area and bone situation when checking the bone column. Furthermore, this technique was inexpensive and maneuverable because it eliminated the dependence on arthroscopy.
There was no clear predictor of bone nonunion in the subtalar joint fusion, but an effective and adequate bone graft was considered to be a determinant factor of the postoperative time to union and restoration of the talocalcaneal relationship. 13 A recent study showed that the use of porous tantalum, a freeze-dried xenograft, and a spinal cage with a local graft achieved satisfactory results of subtalar joint fusion and reduced donor site complications. 14 For patients with subtalar nonunions, some experts have used an iliac bone free flap to realize radiographic bony union with no recurrence of infection or wound healing problems. 15 Niedhart et al. 16 reported that an autogenous iliac graft was the gold standard clinical bone graft for subtalar joint fusion but that it may lead to donor site complications. Whether by traditional surgery, arthroscopic surgery, or other methods of minimally invasive surgery, most patients underwent autogenous iliac grafting procedures that increased the trauma, intraoperative bleeding, and risk of complications.
In the present study, most of the bone could be retained and planted into the bone defect area after sorting (merging of the bone of the lateral mound), which met the requirements for patients with bone grafts and reduced the iliac bone mass. The iliac crest harvest rate was 26.7%, which is significantly lower than that of other surgical methods. The blood loss volume was significantly higher in patients with than without iliac grafts, and one patient with an iliac bone graft developed fat liquefaction in the iliac bone incision. Therefore, the risk of trauma and incision complications associated with iliac crest grafts cannot be ignored, and an in situ autograft may be a better choice. In addition, some researchers have suggested the use of a tricortical iliac bone graft to avoid collapse of the bone graft area and loss of heel height. 17 In the present study, the subtalar joint hardening structure was not completely destroyed, and strong support for hardening bone remained; thus, the implanted bone did not need to completely bear direct pressure. No collapse of the bone graft area appeared, and the bone graft sleeve ensured the accurate location of bone. The bone condition was stable after tamping with the bone graft stick, and the hemorrhage was controlled after loosening the tourniquet. The surgery achieved a satisfactory union rate and AOFAS score although without a high-quality cancellous bone graft. 18
This study has several limitations. First, the indications for surgery were relatively narrow because malformations of the calcaneus, valgus deformities, and other abnormalities needed to be corrected at the same time; the effect of MISA remained unclear; and patients with type V calcaneal fracture malunion were excluded. Second, most of the procedures needed to be carried out under fluoroscopy, and the patients and medical staff required necessary protection. Third, subtalar fusion was required to improve the calcaneal position in the sagittal and frontal planes; however, this surgical technique did not achieve this goal. Fourth, this study had a relatively low sample size and short follow-up. Therefore, in future we will selected larger samples including patients with type V calcaneal fracture malunion or subtalar arthritis that develops after calcaneal intra-articular fracture to further study clinical outcomes using appropriate clinical scoring systems.
Conclusion
MISA is a simple and effective treatment method for TSA. Its advantages include a satisfactory osseous fusion rate and foot function score, low iliac crest bone rate, minimal trauma, minimal bleeding, accurate and effective bone grafting, and no need for arthroscopy.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
