Abstract
Objective
This study was performed to establish an optimized beagle model for maxillary sinus floor augmentation via a mini-lateral window with simultaneous implant placement.
Methods
Twelve beagles underwent maxillary sinus floor augmentation via a mini-lateral window with simultaneous implant placement through sites selected by analyzing preoperative cone beam computed tomography (CBCT) images. During the experiment, no maxillary teeth were extracted and the infraorbital nerve was not severed. The osteotomy was only 5 mm in diameter. The implant stability quotient was measured, and postoperative CBCT was used to detect the condition of the sinus membrane and bone augmentation.
Results
The site corresponding to the tip of the highest dental cusp of the maxillary fourth premolar was suitable for the procedure, and the implant site was on the palatal bone plate. All implants achieved good primary stability. Postoperative CBCT showed no sinus membrane perforation, and the implants penetrated into the sinus cavity surrounded by bone substitute.
Conclusion
The herein-described optimized model with mini-lateral osteotomy and without extraction or severing of the infraorbital nerve was minimally invasive, retained more lateral bone of the sinus, and achieved good sinus floor-lifting results. This model is highly reproducible and merits wider application.
Keywords
Introduction
Placement of dental implants in the posterior maxillary region is often challenging because of the atrophic alveolar bone. Maxillary sinus floor augmentation has been developed to increase the bone volume and quality, thus providing long-term success for dental implants in this region. 1 The lateral window approach remains a classic method since Tatum first reported it in 1986. 2 Numerous clinical and preclinical studies have verified the effectiveness of the technique. Many researchers are still performing extensive work to improve this approach and test newer biomaterials. 3 Because any improvement in a bone augmentation technique is best confirmed by histological analysis, and because human histological studies are limited by ethical restrictions, animal models such as beagles, pigs, sheep, rabbits, and monkeys are often used. Hence, it is crucial to thoroughly understand the anatomical details of animals’ maxillary sinus and establish a reasonable animal model.
Beagles have forward-positioned maxillary sinuses that are above the fourth premolar (PM4) and first molar (M1). The sinus is lined by a complete membrane that is easily removed. Beagles have large oral clefts, with the angulus oris located at the distal plane of the maxillary second molar in occlusion. Furthermore, beagles are abundantly available, easy to maintain, adaptable to their environment, and durable, and they have immunity against infections.4–6 These advantages make beagles suitable models for intraoral surgery in the maxillary sinus region. 6 Kent and Block (quoted by Liu et al. 6 and Convertino et al. 7 ) first reported the modified Caldwell–Luc procedure, which involves raising of the sinus floor in beagles. Since then, increasing numbers of researchers have carried out sinus floor augmentation via the lateral window in beagles for preclinical tests.
The traditional beagle model for maxillary sinus floor augmentation with the lateral window approach is characterized by removal of the maxillary PM4 and M1 teeth 3 months before maxillary sinus floor augmentation, severing of the vascular bundles of the infraorbital nerve to expose the buccal bone plate of the maxillary sinus, and creation of a large osteotomy measuring >6 × 10 mm on the lateral wall of the sinus.5,8 Although these characteristics are widely accepted, this model still has some shortcomings. First, teeth need to be extracted followed by a 3-month-long healing process, increasing the time and cost of this model implementation. Second, severing of the vascular bundles of the infraorbital nerve is not only unethical but also overlooks the influence of nerve injury on bone regeneration in the maxillary sinus. Third, the osteotomy results in bone particle loss.
Therefore, on the basis of the principle of minimally invasive trauma for the animal, ensuring lower experimental costs, and reducing complications, we herein propose an optimized beagle model for maxillary sinus floor augmentation via a mini-lateral window with simultaneous implant placement. Accordingly, the primary aim of this study was to choose the optimal osteotomy and implant sites according to cone beam computed tomography (CBCT) measurements and thus establish an optimized beagle model. The secondary aim was to evaluate the primary stability of the implant and the postoperative CBCT image of the maxillary sinus.
Materials and methods
Animals
This study involved 12 beagles aged 12 months and weighing about 12 kg. The sample size was calculated for the primary outcome (i.e., one of the measurement parameters was the thickness of the palatine plate) in the MedSci Sample Size tools software program based on a previous study 6 to evaluate the measurements of the candidate osteotomy and implant sites in CBCT coronal sections. The calculated number of samples was 24, and these samples were obtained from 12 beagles. All beagles had complete dentition, no dental defects, and no pathologic changes caused by local or systemic diseases. The beagles were acclimatized for more than 1 week to ensure that they were in good condition. They were fed in cages during the experiment. The study was conducted in accordance with the Ethics Committee of the First Affiliated Hospital, College of Medicine, Zhejiang University. The Ethics approval number was (2017) Rapid Trial (212). We adhered to the Animal Research: Reporting of In Vivo Experiments (ARRIVE) guidelines and completed the ARRIVE checklist.
All beagles were fasted for 8 hours before anesthesia. For all procedures involved in the study, the dogs were first sedated with subcutaneous Su Mian Xin II (Institute of Veterinary Medicine, Agricultural and Animal Husbandry University of the PLA, China) at a dose of 0.1 mg/kg body weight. Before surgery or any interventional manipulation, general anesthesia was administered using pentobarbital sodium (Abbott Laboratories, North Chicago, IL, USA) at a dose of 30 mg/kg. Upon completion of this experiment, we planned to continue feeding and maintaining the beagles until further histological studies.
Preoperative CBCT scan analysis
CBCT scans of each beagle were obtained with the NewTom VGi (Cefla s.c., Bologna, Italy) before the floor of the maxillary sinus was raised. With the onset of general anesthesia and establishment of steady breathing in the beagles, the maxillary sinus position was adjusted into the field of vision, which measured 15 × 15 cm. The CBCT scanning parameters were as follows: voltage, 110 kV; current, 1.97 mA; effective exposure time, 3.6 seconds; rotation, 360 degrees; and complete scanning time, 18 s. NewTom NNT (Cefla s.c.) was used to read and analyze the scan data by reconstructing coronal tomograms vertical to the occlusal plane and the nasal septum plane. The measurement plane across the tip of the highest dental cusp of PM4 was defined as P1, and the measurement plane across the crest of the distal alveolar ridge of PM4 was defined as P2. The measurements on plane P1 were set as the experimental group, and those on plane P2 were set as the control group. The base points and baselines of measurement were set as follows (Figure 1):

Base points and baselines of measurement on cone beam computed tomography.
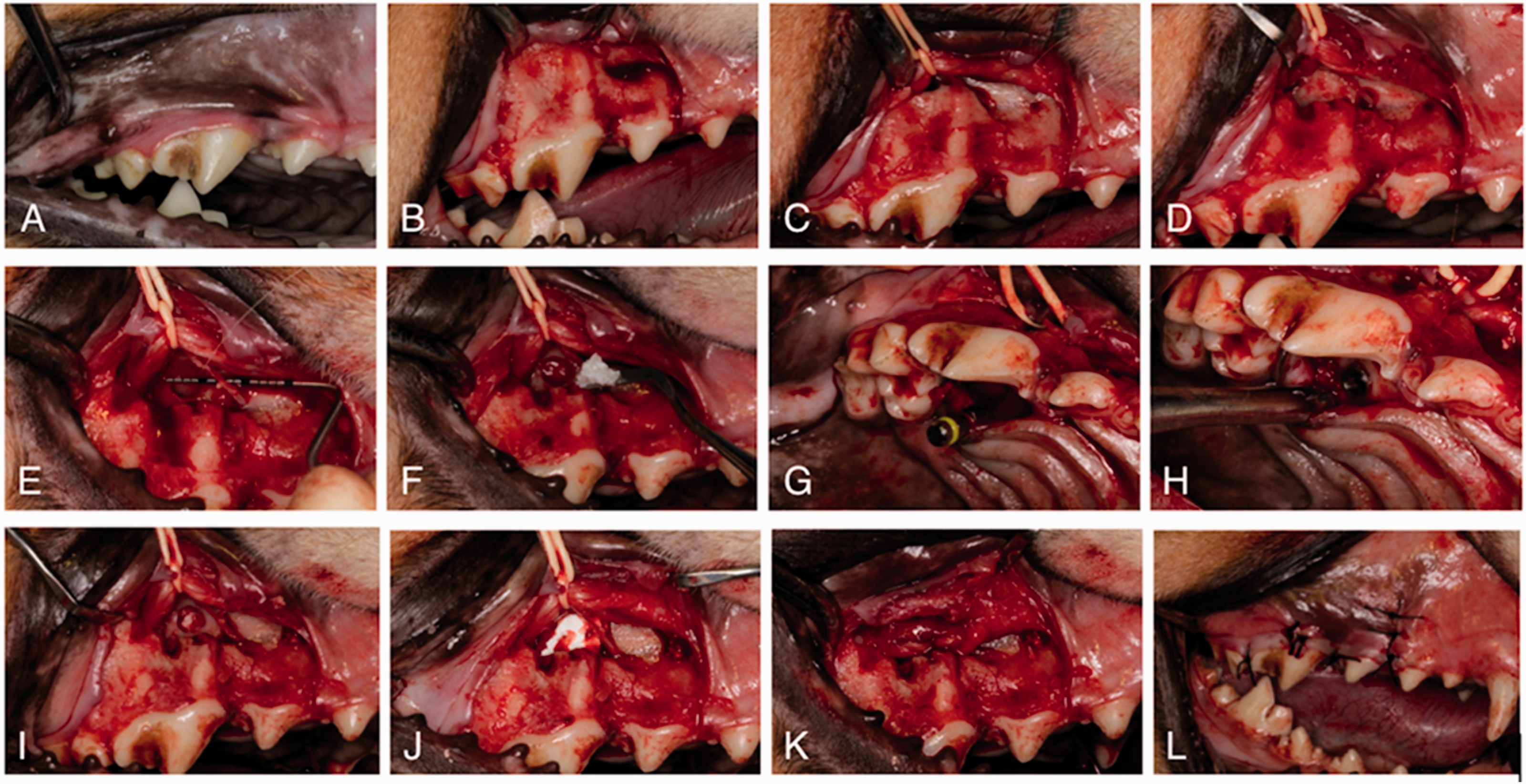
Surgical procedure for maxillary sinus floor augmentation via a mini-lateral window with simultaneous implant placement (A–L: steps of the surgery).
Point A: Lowest point of the maxillary sinus floor relative to the occlusal plane
Baseline L1: Interconnecting line between the medial wall and the lateral wall of the maxillary sinus, perpendicular to the nasal septum and 1.5 mm above Point A
Point B: Midpoint of baseline L1
Baseline L2: Straight line running parallel to the nasal septum and passing through Point B
Point C: Intersection of baseline L2 and maxillary sinus floor
Point D: Intersection of baseline L2 and palatal surface
Point E: Intersection of baseline L2 and maxillary sinus roof
Point F: Crest of the palatal alveolar ridge on the P1 or P2 plane
Point G: Lowest point of the infraorbital nerve tube
Point H: Highest point of the infraorbital nerve tube
Point I: Midpoint on the buccal bone plate of the infraorbital nerve tube
The measurement parameters were as follows:
Length of baseline L1 (width of the maxillary sinus floor) Length between Point C and Point E (height of the maxillary sinus) Length between Point C and Point D (thickness of the palatine plate) Vertical distance between Point F and baseline L2 Vertical distance from Point G to the buccal bone surface of the infraorbital nerve tube (thickness of the buccal bone plate of the lower portion of the infraorbital nerve tube) Vertical distance from Point H to the buccal bone surface of the infraorbital nerve tube (thickness of the buccal bone plate of the superior portion of the infraorbital nerve tube) Vertical distance from Point I to the buccal bone surface of the infraorbital nerve tube (thickness of the buccal bone plate of the middle portion of the infraorbital nerve tube) Thickness of the maxillary sinus mucosa
Establishment of optimized beagle model for maxillary sinus floor augmentation via a mini-lateral window with simultaneous implant placement (Figure 2)
Penicillin was administered preoperatively. Anesthesia was supplemented by local administration of 4% articaine HCl with 1:100,000 epinephrine (Acteon, Mérignac, France). Before surgery, the animals underwent dental prophylaxis, and all of the surgical sites were washed with 1% povidone iodine solution. The surgeries were performed under sterile conditions. According to the statistical results of the preoperative CBCT analysis, we chose the site corresponding to the tip of the highest dental cusp of PM4 as the lateral window osteotomy and implant site.
Every maxillary sinus (12 in total) was incised on the buccal gingival margin from the mesial side of the third premolar (PM3) to the distal side of M1, along with a vertical releasing incision on the mesiobuccal surface of PM3. The full-thickness mucoperiosteal flap was elevated to expose the buccal lateral wall of the infraorbital nerve tube. Using a round diamond burr under continuous saline irrigation, a rectangular osteotomy measuring about 20 × 6 mm was prepared on the buccal lateral wall of the infraorbital nerve tube, extending from the outlet of the infraorbital nerve tube to the mesiobuccal side of M1. The bony window was removed to expose the infraorbital nerve. The infraorbital nerve was then gently pulled to one side to expose the lateral wall of the maxillary sinus, which was located palatally on top of the PM4 and M1 roots. A circular bone window with a diameter of about 5 mm was created on the sinus lateral wall corresponding to the tip of the highest dental cusp of PM4 (i.e., a mini-lateral window). The sinus membrane was subsequently peeled and slightly pushed upward.
Next, an incision was made on the palatal gingival margin from the mesial side of PM4 to the mesial side of M1, and the full-thickness mucoperiosteal flap was raised to expose the palatal bone plate corresponding to PM4. The implant site was on the palatal bone plate corresponding to Point D on the P1 plane. The osteotomy was prepared for the implant according to the manufacturer’s standard procedures.
The raised spaces between the membrane and the sinus floor were then filled with Bio-Oss (Geistlich Biomaterials, Wolhusen, Switzerland) and one ZDI® implant measuring 3.3 mm in diameter and 8 mm in length (Zhejiang Guangci Medical Device Company, Zhejiang, China), which was placed with an insertion torque at >20 cNm. A collagen membrane (Bio-Gide; Geistlich Biomaterials AG) was positioned to cover the access osteotomy of the sinus, and the infraorbital nerve was repositioned. Finally, the mucoperiosteal flap was repositioned and sutured.
Measurement of implant stability quotient
After implantation, the implant stability quotient (ISQ) was measured by a resonance frequency analyzer (Osstell ISQ®; Osstell AB, Gothenburg, Sweden) to assess the implant stability. First, the SmartPeg was installed on the implants, and the probe was then aimed in the two directions vertical to the SmartPeg from the buccal–palatal direction and mesial–distal direction. The obtained resonance frequency results were converted to 1 to 100 values and displayed on the screen of the instrument; these were the ISQ values.
Postoperative CBCT scan analysis
Postoperative CBCT scans were obtained for all beagles immediately after the operation to verify the efficacy of the procedure. CBCT scanning measurements and parameters were the same as those used for the preoperative scan. The data were also entered into the NewTom NNT software program to detect perforation of the sinus membrane and the condition of bone augmentation in the sinus.
Statistical analysis
The paired Student’s t-test in the SAS 9.0 software package (SAS Institute, Cary, NC, USA) was used to calculate the mean and standard deviation of all measurements. P values of <0.05 were accepted as significant.
Results
In this experiment, 12 beagles were examined by CBCT, and 24 maxillary sinuses were measured and analyzed. Of these, 12 maxillary sinuses underwent sinus floor augmentation via a mini-lateral window with simultaneous implant placement.
Results of preoperative CBCT imaging analysis
All measurement parameters except the maxillary sinus width on plane P1 were significantly different from those on plane P2. The detailed data are shown in Table 1. On plane P1, no significant differences in the measurement parameters were found between the left and right sinuses (Table 2).
Comparison of maxillary sinus measurement results between plane P1 and plane P2 (P < 0.05).

P1: plane across the tip of the highest dental cusp of PM4; P2: plane across the crest of the distal alveolar ridge of PM4; a: width of the maxillary sinus floor; b: height of the maxillary sinus; c: thickness of the palatine plate; d: distance from the crest of the palatal alveolar ridge of PM4 to the point set as the implant site on the palatal bone surface; e: thickness of the buccal bone plate of the infraorbital nerve tube lower portion; f: thickness of the buccal bone plate of the infraorbital nerve tube superior portion; g: thickness of the buccal bone plate of the infraorbital nerve tube middle portion; h: thickness of the maxillary sinus mucosa.
Comparison of measurement results between the left and right maxillary sinus on plane P1 (P < 0.05).

P1: plane across the tip of the highest dental cusp of PM4; a: width of the maxillary sinus floor; b: height of the maxillary sinus; c: thickness of the palatine plate; d: distance from the crest of the palatal alveolar ridge of PM4 to the point set as the implant site on the palatal bone surface; e: thickness of the buccal bone plate of the infraorbital nerve tube lower portion; f: thickness of the buccal bone plate of the infraorbital nerve tube superior portion; g: thickness of the buccal bone plate of the infraorbital nerve tube middle portion; h: thickness of the maxillary sinus mucosa.
Values of ISQ
All implants showed good initial stability, and the ISQ was >50 (mean, 53.6).
Results of postoperative CBCT imaging detection
CBCT clearly showed the osteotomy on the buccal bone plate of the maxillary sinuses, and no bone substitute particles were scattered from the windows. The maxillary sinus membrane was completely lifted, and the space underneath was filled with bone substitute particles to form tents. No obvious perforation or bone substitute loss was observed. The implants penetrated into the maxillary sinus cavity but did not touch the roof wall, palatal wall, or buccal wall, which were surrounded by bone substitute (Figure 3).
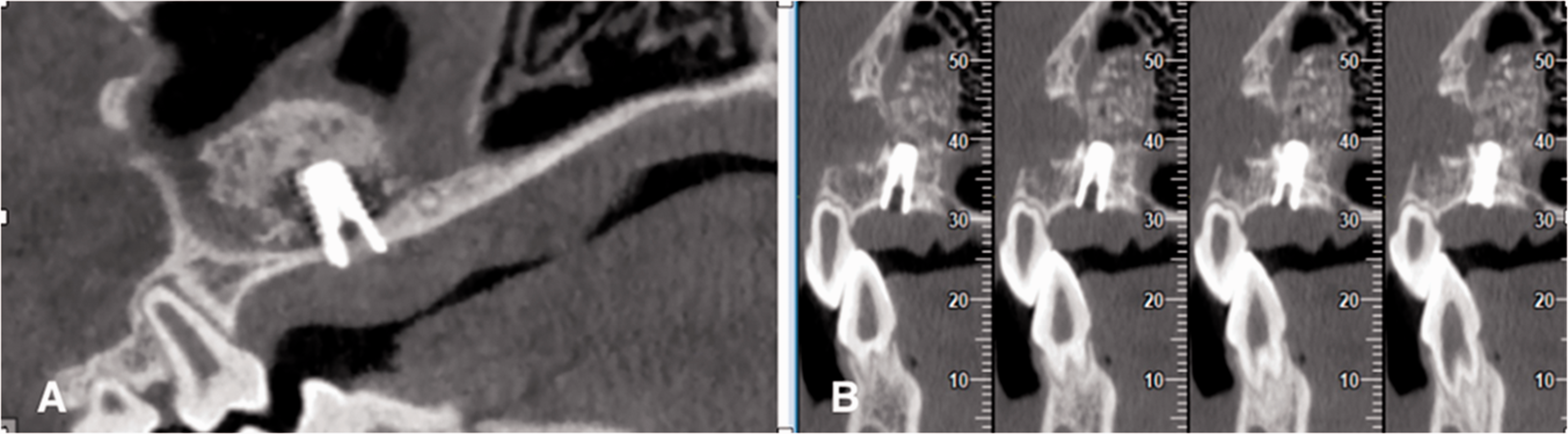
Postoperative cone beam computed tomography imaging (A: coronal tomogram; B: sagittal tomogram).
Discussion
As more in-depth studies of maxillary sinus floor augmentation are performed, the establishment of animal models is also increasing. A good maxillary sinus animal model is the basis for evaluation of maxillary sinus floor augmentation. One of the most commonly used animal models for maxillary sinus floor augmentation via the lateral window is the beagle model. However, the traditional beagle model has many shortcomings, including the need to extract additional teeth and sever the infraorbital nerve, thereby inducing more surgical trauma and postoperative complications. The optimized beagle model described in this article overcomes these limitations.
Before establishing the optimized beagle model in the present study, CBCT data of the maxillary sinus of the beagles were analyzed to determine the optimal osteotomy site and implant site. We concluded that the site corresponding to the tip of the highest dental cusp of PM4 was suitable for the procedure. This site was well located in the beagle’s mouth and could be clearly visualized, thereby making it easier to expose the buccal bone plate during the operation. Therefore, in the optimized beagle model, an incision was only required along the PM3, PM4, and M1 buccal gingival margin, along with a mesiobuccal vertical incision at PM3, exposing the entire field of view required for the operation after lifting the flap and greatly reducing surgical trauma. This site still has other advantages. First, the height and width of the sinus were about 20.67 and 5.77 mm, respectively, which can accommodate an implant with a diameter of 3.3 mm and length of 8 mm. Second, the thickness of the buccal bone plate of the infraorbital nerve tube is thinner and more easily removed. Third, the point on the palatal bone located about 6.3 mm from the crest of the palatal alveolar ridge of PM4 can be set as the implant site, which can be easily prepared because of its clear visualization. Moreover, when the implant penetrates into the maxillary sinus cavity, it does not touch the roof wall, palatal wall, or buccal wall.
This optimized animal model has the following advantages. First, the lateral bone wall osteotomy of the sinus is only 5 mm in diameter, which is much smaller than the conventional osteotomy (6 × 10 mm). Fabrication of the minimal lateral window retains more lateral bone of the maxillary sinus, thus retaining more osteogenic cells and preventing the bone substitute materials being lost from the maxillary sinus. These advantages promote the formation and maturation of new bone after maxillary sinus floor augmentation.9,10 Because the window and field of visualization are very small, lifting the sinus mucosa is more difficult. Therefore, skilled surgeons are required to perform the operation, and careful practice is needed.
Second, during the operation, the operator only needs to slightly pull the vascular bundles of the infraorbital nerve to one side to expose the field required for the minimal osteotomy, rather than severing them to expose a larger field of vision. Preservation of the infraorbital nerve not only shortens the operation time but also reduces bleeding and trauma, making the procedure more ethical and humanitarian.
Third, this optimized beagle model does not require extraction of the maxillary PM4 and M1 before sinus floor augmentation, which greatly shortens the procedure time. The maxillary sinus is located palatally on top of the PM4 and M1 roots; therefore, we placed the implant in the palatal bone instead of the alveolar ridge. The thickness of the palatal bone corresponding to the tip of the highest dental cusp of PM4 was about 1.85 mm, which is adequate for simulating the deficiency of alveolar bone height. To obtain good primary implant stability, we ensured that the implant osteotomy was smaller than the diameter of the implant. Therefore, during the operation, the ISQ of all implants was >50, indicating good stability. It is therefore feasible to place the implants simultaneously through the palatal plates when performing sinus floor augmentation via a lateral window. Retaining the maxillary PM4 and M1 increases the difficulty of operation because it becomes easier to damage the roots when grinding the buccal lateral wall of the infraorbital nerve tube. Therefore, careful and steady manipulation is required during the operation.
Conclusion
According to the CBCT analysis and surgical performance, we conclude that the site corresponding to the tip of the highest dental cusp of maxillary PM4 is suitable for maxillary sinus floor augmentation via a lateral osteotomy with simultaneous implant placement. The implant site was on the palatal bone plate and about 6.3 mm from the crest of the palatal alveolar ridge of PM4. In the herein-described optimized beagle model, there is no need to extract teeth before the experiment or sever the vascular bundles of the infraorbital nerve during the operation, thus shortening the experimental time and minimizing trauma. The lateral osteotomy is round and only 5 mm in diameter, retaining more lateral bone of the maxillary sinus to promote new bone formation and maturation. This optimized beagle model is highly reproducible and therefore worthy of wider application.
Footnotes
Acknowledgements
We thank the native English-speaking scientists of Elixigen Company (Huntington Beach, California) for editing our manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by the Zhejiang Provincial Natural Science Foundation of China (No. LQ17H140001).
