Abstract
Von Hippel-Lindau (VHL) syndrome is caused by germline mutations in the
Keywords
Introduction
Von Hippel-Lindau (VHL) syndrome is a rare hereditary tumor syndrome that manifests with various neoplasms in individuals with
Clarithromycin (CAM) is a new type of 14-ring macrolide antibiotic commonly used in the clinic as an anti-inflammatory drug. 4 Evidence has revealed that CAM may also preserve body weight and physical independence, and prolong survival in patients with lung cancer,5,6 possibly associated with its anti-inflammatory effect.7–9 CAM has also been shown to suppress corneal neovascularization by reducing vascular endothelial growth factor (VEGF) expression, 10 thus demonstrating a role in the regulation of angiogenesis and implying a potential anti-angiogenic effect in addition to its known anti-inflammatory function. 11 For instance, CAM has demonstrated a positive role in the treatment of some hematological cancers via its immunomodulatory and anti-cancer effects.12–14 We therefore speculated that CAM might be an effective treatment in patients with VHL syndrome.
In this study, we present the novel case of a 38-year-old female patient with VHL syndrome who experienced significant improvement after CAM administration. We also discuss this case in the context of the published literature, and consider the possible mechanism of CAM action in the treatment of VHL syndrome.
Case report
We report on a 38-year-old female patient who provided consent for publication of this case report. She was routinely admitted for a check-up on 26 May 2007. A pancreatic abnormality was detected via B-mode ultrasonography. The patient’s history revealed a transitory experience of seeing objects in shades of grey as far back as 1987. She became dizzy when tired or underwent mental stress and preferred to rest in a dark place if possible. The patient had a syncopal attack lasting for 2 to 3 minutes in an elevator in May 1996 and had experienced persistent episodes of vertigo or syncope and tinnitus since the age of 18 years. She developed gradual hypoacusis in her left ear in 2003 and experienced her most recent episode of syncope in June 2003, when she was totally deaf in her left ear. Furthermore, two renal cysts approximately 1 × 2 cm were discovered in 2003, though the precise details were unknown. A mucus cyst was found in her right ovary in May 2005 and she underwent surgical removal of the right ovary by laparoscopy on 8 August 2005. The patient was married when she was 26 years old, and had a healthy daughter in 2005. The patient’s father and aunt had no history of Meniere’s syndrome.
B-mode ultrasound conducted on 29 May 2007 revealed a pancreatic polycyst with partial consolidation, suggestive of a mucinous cystadenoma or cystadenoma. The possibility that it was partly malignant or bleeding could not be excluded. A retroperitoneal polycyst was considered as a disseminated polycystic kidney. The patient was generally in good condition and no abnormalities were found in the lung, abdomen, thyroid, blood, urine, and feces. Tumor markers including CEA, CA199, CA72.4, CA242, and CA125 were all within normal ranges, except for CA153 which was slightly elevated. Gastrin norepinephrine, epinephrine, and dopamine were all within normal levels. Head computed tomography (CT) and fundus examination showed no abnormalities. Abdominal and pelvic CT scans on 30 May 2007 revealed a pancreatic polycyst-occupying lesion below the front head of the pancreas, which was considered to be a cyst-solitary papilloma; occupying lesions below the back of the pancreas head, which were considered to be islet cell tumors; polycysts in both kidneys with an occupying lesion in the inferior pole of the right kidney, which was identified as a hematoma or RCC; and a node in the left adrenal, which was judged as an adenoma. Recurrence of a cystadenoma in the bilateral adnexal nodes was not excluded. A comprehensive analysis of the above pathological changes indicated a likely diagnosis of VHL syndrome. A chest CT performed on 6 June 2007 showed multiple lymphoid knots in the mediastinum, suggesting the need for a re-examination; the twelfth thoracic vertebra presented with high-definition sub-nodes, suggesting the need for a bone scan. Cephalic CT and magnetic resonance imaging carried out on 4 June 2007 revealed no abnormalities. A fundus examination performed on 8 June 2007 showed no abnormality of the papilla of the optic nerve or retina in either eye.
Nucleotide changes in the resected tumor tissues indicated heterozygosity of the
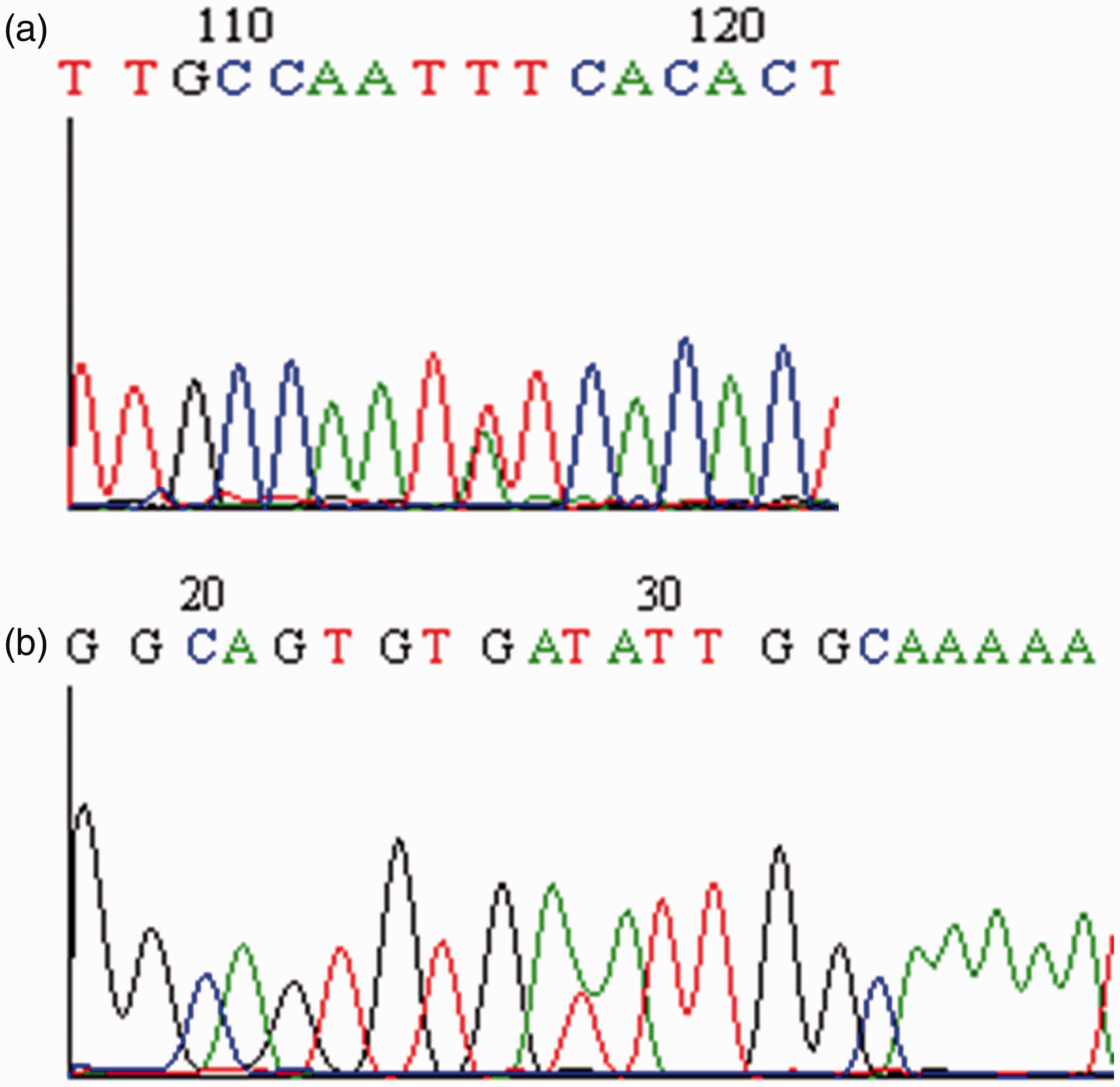
Genetic testing of the patient with VHL and the normal person. a: Sequence change in forward primer region of the patient with VHL and the normal person. b: Sequence change in reverse primer region of the patient with VHL and the normal person.
CT and MRI were performed during CAM treatment to monitor changes in the tumors in the abdomen and inner ear. Postoperative follow-up CT after 3 months showed that the inner ear tumors had stopped growing and the kidney cysts had shrunk. Further basic maintenance of the pancreatic tumors, including treatment with CAM and regular monitoring, showed no significant increases. The patient underwent several subsequent reviews, which showed little change in pancreas size (Table 1). A review on 13 February 2009 showed that the pancreatic tumor, cystic renal lesions, and solid nodules were all significantly diminished in both size and number. The nodules at the lower pole of the right kidney were reduced compared with the previous examination; their last estimated size was approximately 1.6 × 1.9 cm, and this remained unchanged for 4 further years, with no new solid components. A renal cortex lesion measuring 1.8 × 1.6 cm in the central area was narrower than before (Table 1). Annual examinations thereafter revealed that pancreas and kidney functions were within normal ranges, indicating no significant pancreas or kidney damage, and there was no subsequent sign of recurrence on CT scans. The changes in the patient’s left lymph node are shown in Figure 2. No gut flora imbalances were found after drug administration. There were no adverse effects of CAM.

Computed tomography scans showing left endolymphatic sac (arrow) after treatment with clarithromycin on 26 March 2008 (a), 8 September 2009 (b), 9 September 2010 (c), 17 March 2011 (d), and 27 December 2011 (e).
Changes in lesions after treatment with clarithromycin.

Discussion
VHL syndrome was officially named by Melmon and Rosen in 1964. This syndrome is characterized by CNS hemangioblastoma accompanied by cysts of the pancreas and kidney, pheochromocytoma, renal carcinoma, and skin adenoma. Thus, VHL syndrome is identified as a genetic condition involving renal carcinoma and renal clear cell neoplasm. VHL syndrome is an autosomal dominant genetic disease with an incidence of 1/36,000. 15 One report based on 47 cases across four generations showed that VHL syndrome-related diseases mainly included retinal angioma (27.8%), CNS hemangioblastoma (50.0%), renal cysts and carcinoma (55.6%), and pancreatic cysts (38.9%). The incidence of lymph sac tumors in the general population is very low, but the morbidity in VHL patients is approximately 11%, and VHL syndrome is the only disease characterized by bilateral lymph sac malignancies.15,16 CNS hemangioblastoma and RCC are the most common causes of VHL-associated death. Surgery is currently the main therapeutic option for VHL disease, but given the presence of the disease in multiple organs and its high recurrence rate after resection, surgical treatment is difficult and cannot remove all lesions or prevent its recurrence. There is also no specific drug for targeting VHL to date.
The current clinical diagnostic criteria for VHL syndrome include a family history of hemangioblastoma or visceral lesions, while patients without a family history are diagnosed by the presence of more than two hemangioblastomas or one hemangioblastoma accompanied by one visceral tumor.
17
A genetic diagnosis is the gold standard for VHL diagnosis. The current case was diagnosed definitively by genetic analysis, which confirmed a
Inflammation is considered to play a critical role in the multiple pathogenesis of VHL. The immune systems in individuals expressing heterozygous
CAM is a new type of 14-ring macrolide antibiotic widely used in the clinic as an anti-inflammatory drug.
20
In addition to its anti-inflammatory effects, its biological response regulatory effects have also caused increasing interest in recent years.
21
CAM can regulate angiogenesis by affecting cytokine biology, and might thus possess potential anti-angiogenic effects. Considering these effects of CAM, we tested the hypothesis that long-term treatment with CAM may thus inhibit the expression of relevant inflammatory factors affected by
The
The present report describes a patient with VHL syndrome who was treated with CAM. Follow-up observations suggested that her renal tumor decreased and then remained unchanged for 5 years. There were no obvious side effects of oral CAM. This case highlights the potential effectiveness of CAM for the treatment of VHL syndrome. However, large clinic trials involving more types of tumors are needed to verify the curative effect of CAM, which has the potential to become an effective therapy for VHL-associated lesions.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
