Abstract
Abstract
Objectives
To determine the knowledge of falls risk factors among home healthcare (HHC) professionals and the practice patterns of HHC professionals regarding falls prevention.
Methods
A modified version of a survey designed and validated for use in home healthcare settings was distributed to HHC professionals for self-completion. Responses were collected and analysed using descriptive methods.
Results
Out of 80 surveys distributed to 23 HHC centres, 52 returned surveys were included for analyses (completed by physicians, physical therapists [PTs] and nurses). In terms of practice patterns, 82.7% of participants always asked older adults if they have a history of falls, 81% always identified falls risk factors, 73% documented risk factors for falling and 71% always provided interventions to address falls risk factors. Environmental hazards were the most common risk factor identified by HHC professionals. Approximately one quarter of nurses felt they had little knowledge of falls risk factors.
Conclusion
Over 70% of HHC professionals acknowledged the importance of falls, and over 80% of participants displayed knowledge of falls prevention factors. As HHC professionals most likely to encounter patients requiring intervention for falls prevention, physical therapists may benefit from training programmes to help identify important falls risk factors.
Introduction
Falls are associated with increased age,1,2 and have been correlated with deconditioning and early admission to long-term settings.3–5 The costs of treating falls among older adults can be very expensive, for example, the US Center for Medicare and Medicaid services estimated falls-related cost in the USA to be $31 billion USD for 2015. 6
Life expectancy has increased in Saudi Arabia over the last decade, leading to an increase in the elderly population, which is expected to have doubled by 2020. 7 The elderly population in Saudi Arabia represented 3.5% of the total Saudi population in 2003,8,9 and is projected to make up 18.4% of the total Saudi population by 2050.10,11 This projected proportional increase in the older population will have direct and indirect impacts on the Saudi healthcare system. 7
Beside the impact on the healthcare system, falls have an impact on a person’s social life, leading to reduced social participation and quality of life. 7 Home healthcare (HHC) professionals need to perform fall preventive assessments in older adults to assess who is at risk of falling, to help prevent new or recurrent falls events, and decrease fall-related injuries. Fall reduction programmes and home hazards assessments for older adults have been suggested to lead to reduced mortality by two years,12,13 and falls can be prevented by managing risk factors and addressing these factors in a plan of care. 14
Risk factors should be addressed by HHC professionals during the start of care in order to deliver better care that enhances the elderly person’s quality of life. 15 A panel of experts in prevention of falls in older adults have identified modifiable risks factors, such as home hazards, psychotropic or multiple medications, weakness in the lower extremities, walking disorders, loss of balance, vestibular disorders, orthostatic hypotension, loss of sensation related to diabetes mellitus, and use of sedative medications.15–17
A survey of physical therapists (PTs) involved in geriatric rehabilitation at home, 14 that used a validated questionnaire to obtain responses about the risk of falling and possible fall prevention strategies, revealed that most PTs assessed falls risk and provided balance training and strengthening exercises as interventions to decrease the risk of falls. Moreover, PTs also utilized interventions like environmental adjustments and education about falls. 14
A systematic review and meta-analysis showed that most PTs rank environmental threats, orthostatic hypotension, multiple medications (polypharmacy) and muscle weakness as the main reasons for falls among the elderly. 18 In this same study, however, 47% of PTs responded that fall prevention interventions used by therapists don’t directly address risk factors among fallers. For example, 30% of PTs felt that health specialists addressing foot and footwear problems would help reduce incidence among fallers. Locomotor and balance disturbances are risk factors directly related to physical therapy, but multiple medications, postural hypotension, and foot or footwear issues may better be addressed by other specialists. Despite these views, the majority of PTs didn’t refer potential individuals to a specialized healthcare team. Non-referral was associated with lack of understanding of other healthcare teams or inability to execute the referral. It was noted that PTs with less than 14 years of experience referred patients more frequently than therapists with more experience. 18
In a recent study concerning the older Saudi population, 8 73% of older people were shown to have three or more comorbidities that increase the risk for falling and pose a burden to HHC expenditure in Saudi Arabia, however, there are limited published studies that address fall prevention approaches in the HHC setting in Saudi Arabia. The purpose of the present study was to determine the knowledge among HHC professionals of falls risk factors and to determine the practice patterns of HHC professionals regarding a falls preventive approach. HHC professionals have an essential role in falls prevention, thus, knowledge of falls prevention approaches is essential in preventing injuries and reducing falls-related health care expenditure.
Participants and methods
This observational, descriptive study included HHC professionals (physicians, PTs, occupational therapists, nurses, and speech and hearing pathologists) working in HHC settings in the Aseer region of Saudi Arabia, and was conducted between June 2017 and August 2017.
Anonymous self-administered questionnaires were sent by one of the researchers (SA) to all registered HHC professionals (n = 80) working at 23 HHC centres in the Aseer region. Survey distribution and collection was conducted over a two-month period. The study did not include patients and was therefore exempt from institutional review board approval and any requirement for informed consent.
The questionnaire was a modified version of a survey administered by a team at the University of Alabama to acquire information on knowledge, attitudes, and self-reported practice behaviour related to assessment and management of falls risk among PTs working at home care agencies. 14 The survey comprised eight items with a combination of open and closed-ended questions: Questions 1–4 obtained information about current practice; Questions 5 and 6 acquired information on falls risk factors and their importance; Question 7 related to the management of falls, including falls prevention strategies; and in Question 8, participants were asked to rate their knowledge of falls risk factors. 14
The survey used in the current study was amended to fit other medical professions in the home care medical team including physicians, nurses, occupational therapists and speech therapists, as well as PTs. Also, questions 5 and 6 from the original survey were combined, so that the current questionnaire comprised seven questions. Following amendment, the survey underwent a point-by-point review and agreement between three researchers (FA, SA, and MA) who are experts in the field of falls prevention. The complete survey used in the current study is provided in the Appendix.
All data are presented as n (%) prevalence and were assessed using descriptive statistics. Proportions were calculated based on the total number of responses for each question. Participants’ responses to question 5 were grouped into 13 categories, as shown in results Table 4. Some participants gave several responses that fitted into one category (different terms with the same meaning), or several responses that were grouped under one category (e.g., ‘slippery floor’ and ‘uneven surfaces’ were considered to be ‘Environmental hazards’). Each of the 13 categories comprised the total number of responses for that category, i.e., each category may contain >1 response per participant.
Results
The self-administered survey was distributed to 80 HHC professionals and 60 surveys were returned (response rate, 75%). Of the 20 unreturned surveys, 13 were due to employees being on vacation and seven employees were covering at establishments other than HHC centres. Out of the 60 returned surveys, eight were excluded because of major missing data, leaving 52 surveys that were either fully completed or had only minor missing data. Thus, questionnaires from a total of 52 participants (33 male and 19 female) were included in the final analyses.
The professional healthcare group represented by the highest proportion was nurses (n = 24 [46.2%]), followed by physicians (n = 20 [38.5%]), and PTs (n = 7 [13.5%]) (Table 1). Regarding hours spent caring for the elderly, 17/44 participants who responded to the question (38.6%) spend 10–20 h in elderly patient care, equating to 32.7% of participants included in the study (Table 2). Only 4.5% of those who responded to the question (2/44) reported spending < 10 h per week for elderly patient care, equating to 3.8% of participants included in the study (Table 2).
Characteristics of home healthcare professionals from the Aseer region of Saudi Arabia included in a survey on falls prevention
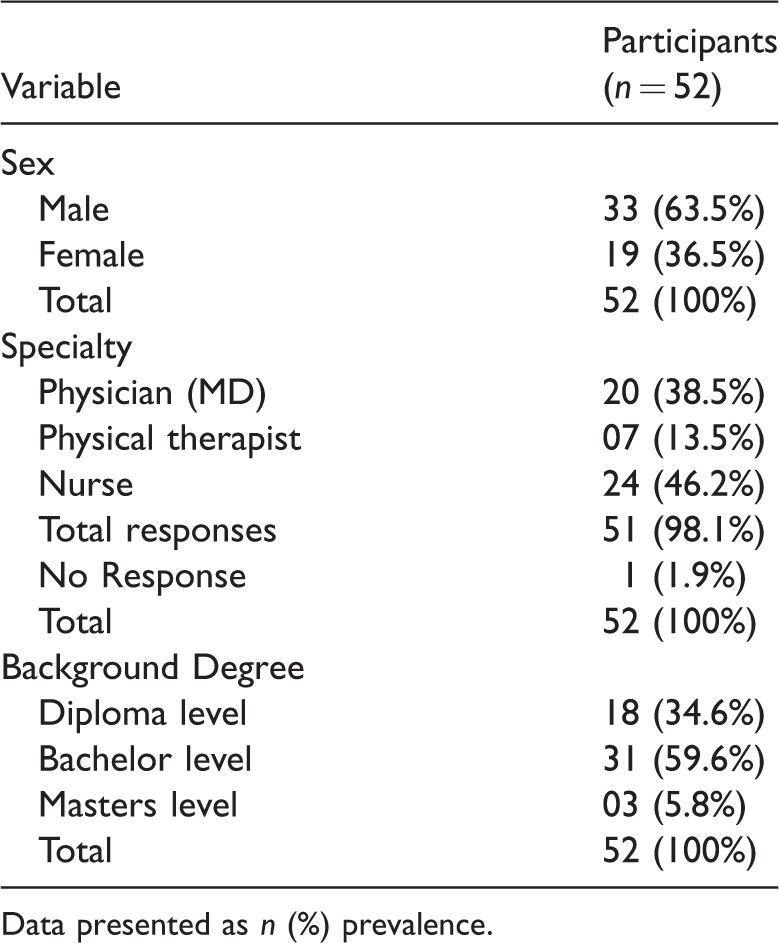
Data presented as n (%) prevalence.
Work characteristics of home healthcare professionals from the Aseer region of Saudi Arabia included in a survey on falls prevention

Data presented as n (%) prevalence.
MD, physician; PT, physical therapist.
The majority of HHC professionals (48/51 [94.1%]) responded that taking a falls history is important in elderly patient care. In response to the question regarding practice patterns, 43/51 participants who responded to the question (84.3%) always or almost always ask older adults if they have a history of falls, equating to 82.7% of participants included in the study (Table 3). A total of 42/51 participants who responded to the question (82.4%) stated that they always or almost always identified risk factors for falling (80.8% of study participants), while 38/51 participants who responded to the question (74.5%) always or almost always documented risk factors for falling (73.1% of study participants). Finally, 36/51 participants who responded to the question (70.6%) always or almost always provided interventions to address fall risk factors (69.2% of study participants) (Table 3).
Practice patterns in home healthcare professionals from the Aseer region of Saudi Arabia included in a survey on falls prevention

Data presented as n (%) prevalence.
MD, physician; PT, physical therapist.
Based on professional specialty, the highest proportion of HHC professionals who ask for falls history, who identify falls risk factors, document the risk of falls and provide some form of falls intervention were nurses, followed by physicians and then PTs (Table 3). Physicians and nurses were shown to spend more weekly time with elderly patients compared with PTs (Table 2).
A total of 348 items listed by participants as falls risk factors were categorized into 13 sections. Of these, environmental factors had the highest number of responses (108 [31%]), followed by improper or limited use of assistive devices or aids, multiple medications, and foot/footwear problems. Impaired functional status had the lowest number of responses, identified by only one participant response (0.3%) (Table 4).
Falls risk factors identified by home healthcare professionals from the Aseer region of Saudi Arabia included in a survey on falls prevention

Data presented as n (%) prevalence of responses (responses were grouped into 13 categories; each category may contain > 1 response per participant).
MD, physician; PT, physical therapist.
According to the general level of knowledge about specific risk factors for falls, 46% of participants (23/50) stated they had some knowledge of falls risk factors in older adults, 40% of participants (20/50) stated that they were very knowledgeable and only 14% (7/50) stated they had little knowledge of falls risk factors (Table 5). Thus, 60% of participants who responded to the question had only some or little knowledge regarding specific risk factors for falls in older adults. In terms of profession type, just over one quarter of nurses have little knowledge regarding falls compared with 14% of PTs and none of the physicians (Table 5).
Level of falls knowledge according to specialty in home healthcare professionals from the Aseer region of Saudi Arabia included in a survey on falls prevention

Data presented as n (%) prevalence.
MD, physician; PT, physical therapist.
Discussion
Falls prevention programmes should be addressed by a multidisciplinary health-care team, and several factors must be considered when dealing with elderly patients. The main risk factors for falling stated in the published literature are home hazards, psychotropic or multiple medications, weakness of the lower extremities, walking disorders, loss of balance, vestibular disorders symptoms, orthostatic hypotension, loss of sensation related to diabetes mellitus, visual disorders, and use of sedative medications.15–17
Falls intervention provided to patients should be multifactorial, and should include balance and coordination exercises, exercises to strengthen weak muscles, correction of any visual deficit, suggestion/provision of proper footwear and intervention to improve functional status, all of which have been associated with reduced fall events.19–21 HHC professionals in the present study felt that impaired functional status, muscle weakness, cognitive impairment, gait problems, balance deficit, and postural hypotension played a lesser role in falls in elderly patients, which seems to contradict published studies showing strong relationships between these factors.22–25 However, environmental hazards were identified by HHC professionals in the Aseer region of Saudi Arabia as important factors in falls among the elderly, and concurred with the published literature regarding the associations between environmental hazards and falls. 26 Any modifications in environmental hazards have been shown to reduce the risk of falls.19,20,27
Based on participant responses, improper or limited use of assistive devices or aids was considered by HHC professionals in the present study to be the second most important identified falls risk factor. Several published studies have shown that most patients who use assistive devices or aids are not doing so in the proper manner,28–30 possibly due to patients buying these devices by themselves without specialist consultation,31,32 and very few patients being trained to use them,31,32 which may increase the risk of falling. 33 Proper use of assistive devices can reduce the risk of falls in elderly patients, and make them feel more balanced and secure, which leads to improved independence.28,29
In elderly patients, a strong relationship has been observed between multiple medications and falls. 34 In the present study, use of multiple medications was identified by HHC professionals as the fourth most important risk factor for falls. Foot and footwear problems are also important considerations in falls prevention when dealing with elderly patients. Footwear that is well-fitted, low-heeled, properly designed and of good material has been shown to potentially reduce the risk of falling.35,36
According to the American Geriatrics Society/British Geriatrics Society clinical practice guideline for prevention of falls in older persons, educational programmes for HHC patients must implement the multicomponent or multifactorial approach. 37 Increasing patient educational programmes regarding exercise and physical activity have been shown to reduce the chances of fall events in elderly. 18 In particular, exercises and physical activities that improve muscle strength, balance and coordination can minimize the risk of falls. Although the present results are supported by the literature, in terms of the importance of taking the fall history, and identifying and documenting falls risk factors, the interventions provided must be customized for each patient.14,38
In the present study, nurses regarded themselves to have lower levels of knowledge regarding falls risk factors compared with other HHC professionals. PTs are required to be knowledgeable about the risks of falls, since they are most likely to encounter patients for fall prevention and management. Based on the present results (Table 4), PTs did not identify the common falls risk factors described in the literature and discussed here. 37 Therefore, an educational training programme designed for PT professionals is required in order to help them identify the most important risk factors for falls. In the present study, 60% of HHC professionals who responded to the question had only some or little knowledge of falls risk factors in older adults. This needs to be addressed in educational programmes on falls prevention approaches that target HHC staff.
The present study was a pilot project to identify issues related to fall prevention knowledge and practice patterns in HHC professionals. The results are limited by several factors, such as the relatively low response rate among professionals, the restriction of the study to the Asser region of Saudi Arabia, which affects the generalizability of results, and the relatively small sample size. In addition, this type of survey is prone to recall bias and is restricted to the self-reported opinions of professionals, some of whom (24 participants) in the present study had less than 4 years’ experience. Future studies should be conducted on a larger scale at a national level in Saudi Arabia, to facilitate the provision of national guidelines for falls prevention in the home healthcare settings in Saudi Arabia.
In conclusion, more than 70% of HHC professionals included in the present study addressed falls during their plan of care and acknowledged the importance of falls. Environmental hazards were the most common risk factor identified by the HHC professionals, and over 80% of participants self-reported that they had some knowledge or were very knowledgeable about factors associated with fall prevention. Among HHC professionals, approximately one quarter of nurses regard themselves as having little knowledge of falls risk factors. Among HHC professionals, PTs are required to be most knowledgeable of falls risks since they are the most likely to encounter patients for fall prevention and management.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not for-profit sectors.
