Abstract
Objective
To examine the prevalence of rheumatic manifestations among patients with inflammatory bowel disease (IBD).
Methods
This prospective study enrolled patients with IBD in whom the diagnosis and extent of IBD were confirmed by colonoscopy and histopathology. Patients were interviewed and examined by a rheumatologist. A complete rheumatological examination, X-rays of the lumbosacral and sacroiliac joints and HLA-B27 blood tests were performed.
Results
A total of 127 adult patients were recruited: 46 (36.2%) with Crohn’s disease (CD) and 81 (63.8%) with ulcerative colitis (UC). Rheumatic manifestations of any type were present in 57.5% (73 of 127 patients) with no significant differences between CD and UC. Peripheral manifestations were present in 43.3% (55 of 127 patients), four patients (3.1%) had axial arthritis alone and 14 patients (11.0%) had both types. Among those with peripheral manifestations, five patients (7.2%) had type 1 arthritis (pauciarticular) and one patient (1.4%) had type 2 arthritis (polyarticular). A higher proportion of patients with CD had axial manifestations with or without peripheral manifestations (eight of 46; 17.4%) compared with patients with UC (10 of 81; 12.3%), but no difference was observed in patients with peripheral manifestations alone.
Conclusions
Rheumatic manifestations in patients with IBD in Qatar are more prevalent than in other regions of the world. Peripheral manifestations were more prevalent than axial.
Introduction
Inflammatory bowel diseases (IBD), which includes ulcerative colitis (UC) and Crohn's disease (CD), are inflammatory conditions affecting the gastrointestinal tract. 1 These chronic diseases have complex genetic, immune and environmental components, with an aetiology that has yet to be determined.2,3
Musculoskeletal symptoms accompanying a diagnosis of IBD, which are seen in 6–46% of cases, are numerous and include articular, osteoporosis, fibromyalgia, periarticular and muscular symptoms. 1 These arthropathies can be classified into two main categories: peripheral and axial. Peripheral arthropathies include peripheral arthritis type 1 (pauciarticular) and type 2 (polyarticular), enthesitis, dactylitis and arthralgia. Axial arthropathies include isolated sacroiliitis, inflammatory back pain and ankylosing spondylitis (AS). 2
A previous study reported that joint involvement was observed in 62% of patients with UC, 18–45% of IBD patients meet the criteria for spondyloarthropathy (SpA) and 3–9.9% meet the criteria for AS. 4 Another study demonstrated that patients with CD who have colonic involvement have a higher risk of developing synovitis compared with those with isolated small bowel disease, with males and females being equally affected. 5 The researchers also showed that subclinical gut inflammation was observed in two-thirds of patients with SpA. 5
A study conducted in 350 patients found that 129 had at least one musculoskeletal SpA feature. 6 Axial SpA was found in 27% of the sample and peripheral SpA was seen in 30%. 6 No significant differences were seen between patients with UC and CD. 6 In a study involving 79 patients with UC, researchers found articular involvement in 62%, with three major clinical manifestations: peripheral arthritis, AS and unclassified spondylitis. 7 HLA-B27 was significantly more frequently observed among those with arthritis. 7 In addition, HLA-B27 was seen in 50–75% of cases with axial arthritis. 8 A systematic review of 71 studies reported a pooled prevalence of 13% for peripheral arthritis, 10% for sacroiliitis, 13% for spondyloarthritis and 3% for AS among patients with IBD. 9
There are very few studies from the Middle East that have evaluated the prevalence of rheumatic manifestations in IBD patients. A study in Kuwait showed that among 130 patients with IBD (34.6% with UC and 65.4% with CD), the prevalence of rheumatic symptoms was comparable to other global studies. 10 The results showed no significant difference in the existence of rheumatic symptoms between the two diseases. 10 Peripheral arthritis was observed in 31.5% of patients and 8.5% had axial skeletal complications. 10 A Study in Tunis of 50 patients with IBD found that 26% had SpA and 4% had isolated sacroiliitis. 11 The study reported a significant association between colonic involvement in CD and the existence of SpA. 11
This current study provides additional prevalence data for rheumatic manifestations in patients with IBD living in Qatar, which has a unique population structure, with most people coming from the Middle East and Asia.
Patients and methods
Study population and design
This prospective study enrolled consecutive patients with IBD who were being followed up at the IBD Gastroenterology Clinic, Hamad General Hospital, Doha, Qatar, a tertiary university hospital, between 1 February 2015 and 30 July 2016. The diagnosis and extent of IBD (UC or CD) was confirmed by colonoscopy and histopathology. Patients were then interviewed; a detailed rheumatological history was taken and an examination conducted by one of two expert rheumatologists at the Rheumatology Clinic at the same institution. A physical examination was conducted in a private room with the presence of a research team member and a nurse.
The study was approved by the Institutional Review Board of Hamad Medical Corporation, Doha, Qatar (no. 14440/14). Patients provided written informed consent.
Demographic and clinical data collection
The instruments for data collection included the following items: (i) demographics including age, sex, nationality, marital status and educational level; (ii) smoking history, family history of IBD; (iii) diagnosis, duration and extent of IBD; (iv) previous or present history of peripheral arthritis, dactylitis, arthralgia, enthesitis, tenosynovitis, back pain, skin lesions, eye symptoms and relationship of those symptoms with the onset of IBD. A clinical examination was completed, radiographs of the sacroiliac joints and lumbar spine were undertaken and a blood test for HLA-B27 was performed. An ophthalmology consultation was undertaken if required. The Assessment of SpondyloArthritis International Society classification criteria for spondyloarthropathy was used to classify the patients into peripheral and axial spondyloarthritis. 12
Statistical analyses
All statistical analyses were performed using the IBM SPSS® Statistics for Windows, Version 22.0 (IBM Corp, Armonk, NY, USA) and Epi Info™ 2000 (Centers for Disease Control and Prevention, Atlanta, GA, USA). Qualitative and quantitative data are expressed as n of patients (%), mean ± SD and median (range). Descriptive statistics were used to summarize demographic, anthropometry, medical history and all other clinical characteristics of the study participants. The primary outcome variable was the prevalence of rheumatic manifestations among IBD patients and this was estimated and presented along with the 95% confidence interval (CI). Associations between two or more qualitative variables were assessed using χ2-test and Fisher’s exact test as appropriate. Quantitative data between two independent groups were analysed using unpaired t-test and Mann–Whitney U-test as appropriate.
Univariate and multivariate logistic regression methods were used to determine and assess the predictive values of each predictor or probable risk factors for rheumatic manifestations among IBD patients. In addition, the logistic regression method was also used to determine potential predictors and risk factors for IBD. For multivariate logistic regression models, variables were considered if statistical P < 0.10 level in univariate analyses or if determined to be clinically important. The results of logistic regression analyses were presented as odds ratio (OR) with corresponding 95% CI. A two-sided P-value < 0.05 was considered statistically significant.
Results
A total of 127 adult patients with IBD consented to participate in the study: 46 (36.2%) with CD and 81 (63.8%) with UC. Among the sample, 66% (84 of 127 patients) were Arabs, 27% (34 of 127 patients) were Asians and 7% (nine of 127 patients) were of other nationalities. Table 1 presents the demographic and clinical characteristics of the study population. A total of 74 of 127 patients (58.3%) were males; the majority were married (83.1%; 103 of 124 patients); and 36.4% (44 of 121 patients) had a university degree. A family history of IBD was present in 19 of 125 patients (15.2%).
Demographic and clinical characteristics of patients (n = 127) with inflammatory bowel disease (IBD) who participated in a study to investigate the rheumatological manifestations associated with IBD.a
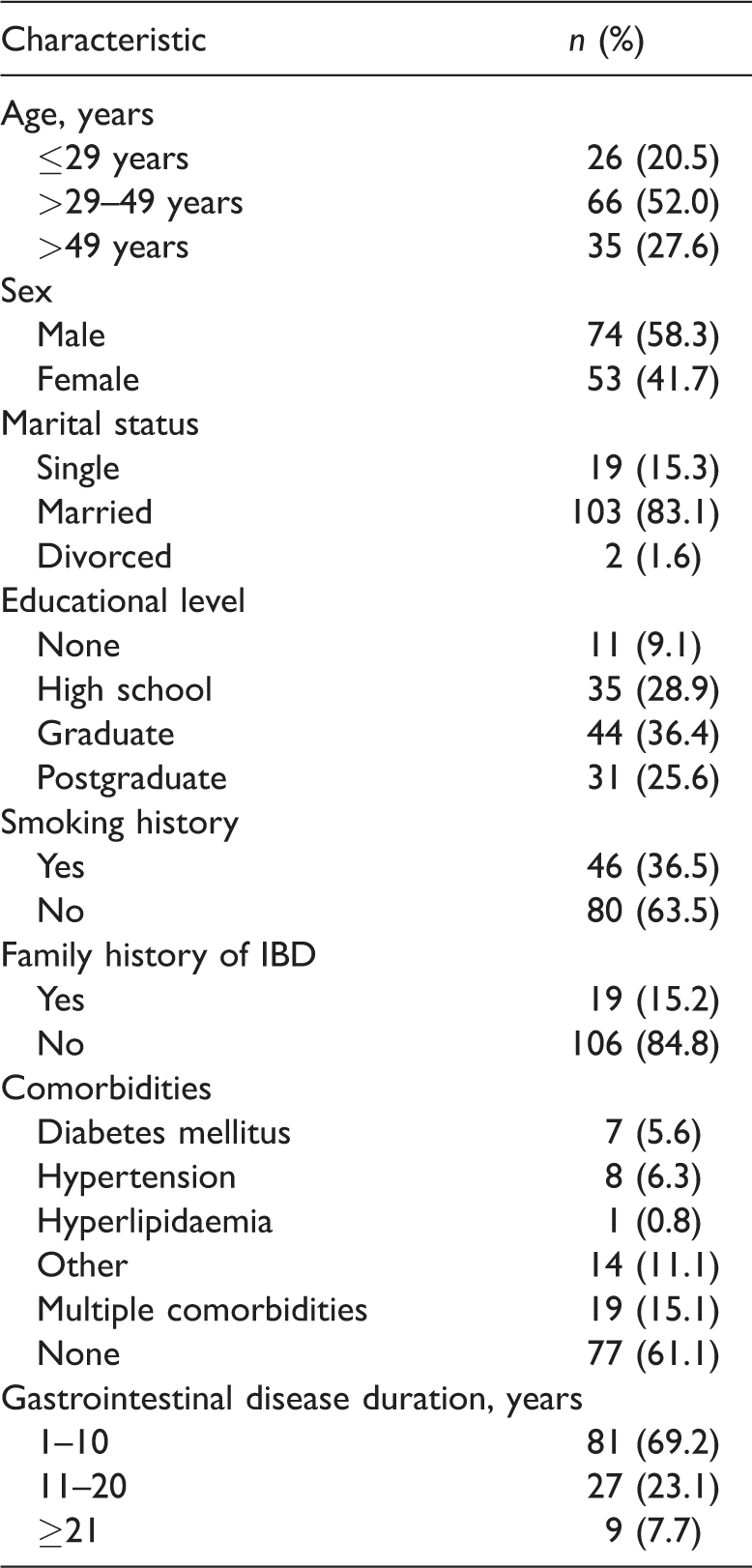

Data presented as n of patients (%).
aFor some variables, the sum may not equal n = 127 due to missing observations. All percentages computed and reported above are based on the available values.
Table 2 shows the prevalence of the rheumatic manifestations of IBD and disease duration. The percentage of rheumatic manifestations was numerically but not significantly higher in patients with CD (27 of 46 patients; 58.7%) compared with UC (46 of 81 patients; 56.8%).
Rheumatic manifestations of patients (n = 127) with inflammatory bowel disease (IBD) who participated in a study to investigate the rheumatological manifestations associated with IBD.a

Data presented as n of patients (%).
aFor some variables, the sum may not equal n = 127 due to missing observations. All percentages computed and reported above are based on the available values.
Table 3 shows the prevalence of rheumatic manifestations in patients with IBD categorized according to demographic and clinical characteristics. The overall prevalence of rheumatic manifestations was 57.5% (73 of 127 patients; 95% CI 48.8, 65.7). The prevalence of rheumatic manifestations among CD patients was 58.7% (27 of 46 patients; 95% CI 44.3, 71.7) compared with 56.8% (46 of 81 patients; 95% CI 45.9, 67.0) in UC patients. Peripheral rheumatic manifestations were observed in 36 of 81 patients (44.4%) with UC compared with 19 of 46 patients (41.3%) with CD. Axial rheumatic manifestations were observed in one of 81 patients (1.2%) with UC compared with three of 46 patients (6.5%) with CD. Nine of 81 patients (11.1%) with UC compared with five of 46 patients (10.9%) with CD had both axial and peripheral manifestations. There was a higher prevalence of rheumatic manifestations among patients ≤29 years of age compared with patients >49 years of age; and a higher prevalence occurred in females, in those with a body mass index (BMI) >25 kg/m2, in those with no education, in those with a comorbidity, in those using biologics and in those with a family history of IBD. However, none of the differences between the groups were significant. The sample size was small and confidence intervals were wide in the statistical comparisons, suggesting that a larger study with more statistical power is needed to detect statistical significant differences, if any.
Prevalence of rheumatic manifestations of patients (n = 127) with inflammatory bowel disease (IBD) categorized according to demographic and clinical characteristics.
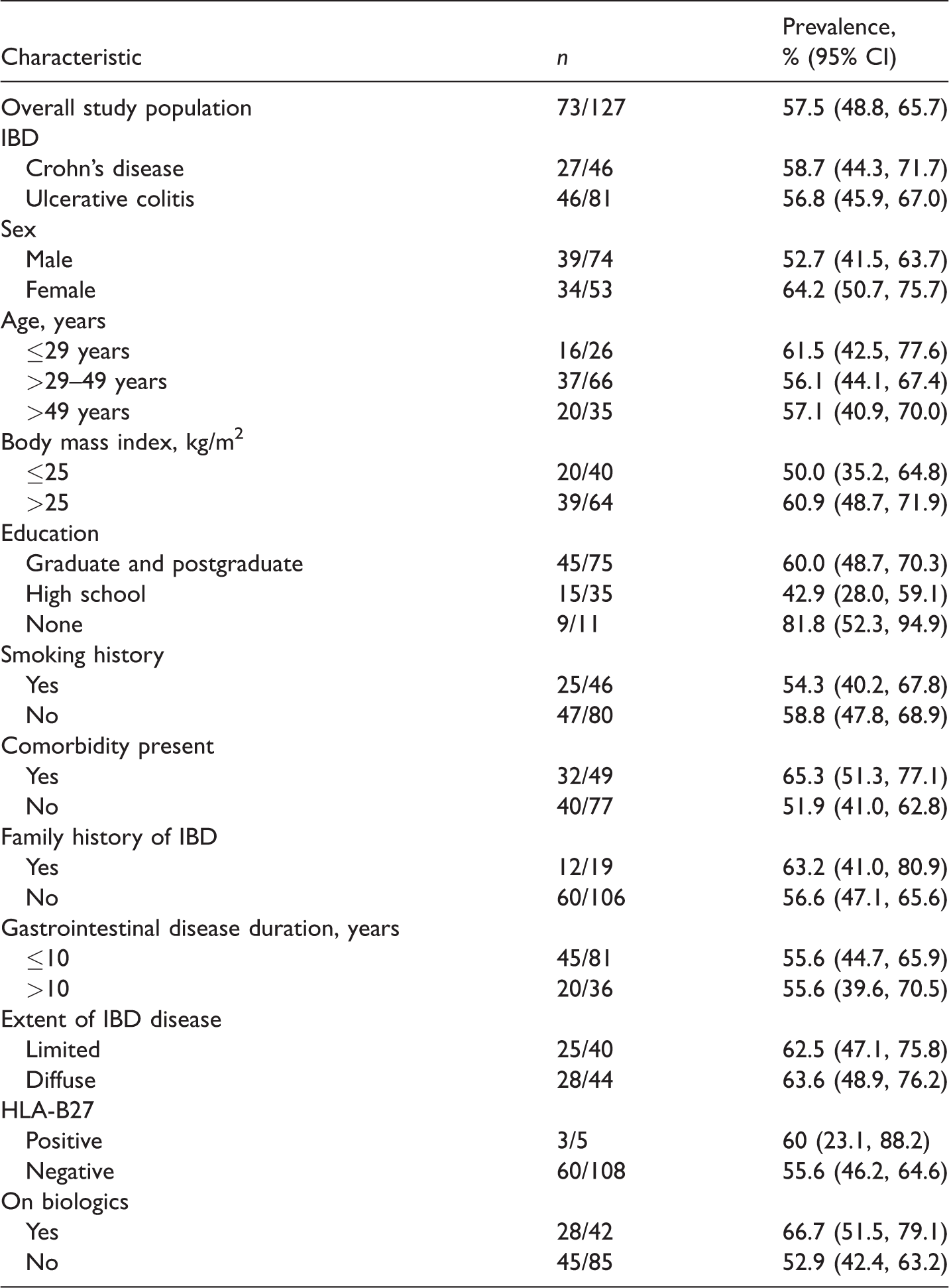
Data presented as n of patients (%).
No significant between-group differences (P ≥ 0.05).
CI, confidence interval.
The results of logistic regression analysis testing for each predictor and their possible association with rheumatic manifestations among IBD patients are presented in Table 4. Age >49 years was associated with a decreased risk for rheumatic manifestations (OR 0.83; 95% CI 0.30, 2.35). Being female (OR 1.61; 95% CI 0.78, 3.31), having a BMI >25 kg/m2 (OR 1.56; 95% CI 0.70, 3.46), the presence of comorbidity (OR 1.74; 95% CI 0.83, 3.65), family history of IBD (OR 1.31; 95% CI 0.48, 3.60), HLA-B27 positive (OR 1.2; 95% CI 0.19, 7.47) and biologics (OR 1.8; 95% CI 0.82, 3.84) were all positively associated with an increased risk for rheumatic manifestations. In multivariable logistic regression analysis controlling for all other potential predictors and covariates such as age, sex, educational status, BMI, comorbidity, family history of IBD, IBD disease duration, extent of IBD disease, HLA-B27 status and biologics, it was observed that female sex (adjusted OR 4.73; 95% CI 1.13, 19.71; P = 0.033), IBD duration > 10 years (adjusted OR 3.65; 95% CI 0.81, 16.38), BMI > 25 kg/m2 (adjusted OR 2.61; 95% CI 0.64, 10.63) and CD (adjusted OR 2.23; 95% CI 0.47, 10.65) remained positively associated with an increased risk of rheumatic manifestations.
Logistic regression analysis of predictors and potential risk factors of rheumatic manifestations in patients (n = 127) with inflammatory bowel disease (IBD) categorized according to demographic and clinical characteristics.

CI, confidence interval; NS, no significant association (P ≥ 0.05).
Reference group: non-rheumatic manifestations.
Table 5 shows the results of the logistic regression analysis testing for each predictor and their possible association with UC. Patients older than 49 years of age (OR 9.13; 95% CI 2.77, 30.13; P < 0.0001) and aged between 29 and 49 years (OR 3.53; 95% CI 1.36, 9.16; P = 0.010), male (OR 2.6; 95% CI 1.24, 5.47; P = 0.012) and the presence of comorbidity (OR 2.44; 95% CI 1.11, 5.38; P = 0.027) were significantly associated with an increased risk for UC. In multivariable logistic regression analysis controlling for all other potential predictors and covariates such as age, sex, educational status, BMI, comorbidity, family history of IBD, disease duration, rheumatic manifestations, being >49 years of age (adjusted OR 14.61; 95% CI 1.39, 154.01; P = 0.026), aged >29–49 years (adjusted OR 7.61; 95% CI 1.26, 46.04; P = 0.027), having a family history of IBD (adjusted OR 7.09; 95% CI 1.01, 49.84; P = 0.049) and the presence of comorbidity (adjusted OR 4.91; 95% CI 1.1, 22.21; P = 0.039) were significantly associated with an increased risk of UC.
Logistic regression analysis of predictors and potential risk factors of ulcerative colitis in patients (n = 127) with inflammatory bowel disease (IBD) categorized according to demographic and clinical characteristics.

CI, confidence interval; NS, no significant association (P ≥ 0.05).
Reference group: Crohn’s disease.
Discussion
The current study investigated the prevalence of rheumatic manifestations among patients with IBD followed at the IBD Gastroenterology Clinic in a tertiary university hospital in Qatar. These current results showed that 57.5% of the study population had some type of rheumatic manifestation. This percentage is higher than many studies in the region and in other countries.10,11,13 In our opinion, this prevalence rate was accurate because a detailed history was taken from each patient, which recorded any history of any rheumatic manifestations at any time, whether prior to or post-IBD onset. In addition, a thorough rheumatological physical examination was carried out by one of two expert rheumatologists who sat together in the clinic for the first few months of patient enrolment so that the quality of the data obtained was consistent.
A study in Kuwait reported a UC and CD prevalence of rheumatic manifestations of 34.6% and 65.4%, respectively. 10 The difference in prevalence of rheumatic manifestations between patients with UC and CD in this current study was not significant, similar to the difference reported by the study from Kuwait. 10 Other reports indicate that patients with CD were more likely to develop extraintestinal manifestations than patients with UC. 14 Similarly, another report observed that SpA was significantly more common among patients with CD compared with patients with UC. 15
Peripheral manifestations (55 of 127 patients; 43.3%) were more prevalent than axial manifestations (18 of 127 patients; 14.2%) in the current study population. This is comparable with the study from Kuwait, which reported a prevalence rate of 31.5% and 8.5% for peripheral and axial manifestations, respectively. 10 Fourteen patients (11.0%) of the current study population had both axial and peripheral manifestations. A self-reported study on spondyloarthritis among patients with IBD from the Netherlands reported that peripheral SpA were present in 30.3% of the sample, while 27.3% had axial SpA. 6
Among those with peripheral manifestations in the current study; 7.2% had type 1, 1.4% had type 2, 15.9% had enthesitis, 11.6% had arthralgia, 8.7% tenosynovitis, 13% had plantar fasciitis, 8.7% had other peripheral manifestations and 31.9% had multiple peripheral manifestations. Among those with axial manifestations: 16.7% had isolated sacroiliitis, 61.1% had inflammatory back pain and 22.2% had AS.
A Turkish study reported a prevalence rate of 8.2% for AS and a rate of 28.7% for spondyloarthritis among 122 patients with IBD. 15 Another study reported that 30% of the patients sampled (n = 103) had inflammatory back pain, while 10% had synovitis. 16 A study in Saudi Arabia reported the presence of arthritis in 16.4%, osteopenia in 31.4% and osteoporosis in 17.1% of patients with UC. 17 The differences in the prevalence rates of the rheumatic manifestations of IBD among these studies might be attributed to the use of different criteria for diagnosing the various arthropathies and the methods used by the studies. Future studies should further investigate each of the manifestations separately.
One of the strengths of this study was the consistency of obtaining the symptoms and performing the physical examination by two rheumatologists to establish the presence and diagnosis of any rheumatic manifestations among the patients with IBD. Furthermore, this is the first study in Qatar to assess the prevalence of these manifestations, which provides a foundation on which future work may be established.
In conclusion, rheumatic manifestations in patients with IBD in Qatar appear to be more prevalent than in other regions of the world. Peripheral manifestations were more prevalent than axial. Based on the findings of this study, we would recommend that rheumatologists and gastroenterologists coordinate their activities while treating patients with IBD. These results will aid in directing treatment and follow-up modalities for these patients.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
