Abstract
Objective
Epicardial fat tissue thickness (EFT) and the neutrophil/lymphocyte ratio (NLR) are associated with atherosclerosis. Few studies have focused on the relationship between these parameters in patients with newly diagnosed hypertension. In this study, we examined the relationship between EFT and the NLR in patients with newly diagnosed hypertension detected by 24-hour ambulatory blood pressure monitoring (ABPM).
Methods
Eighty consecutive patients without chronic illness who were diagnosed with hypertension according to ABPM results and 80 otherwise healthy subjects were enrolled in the study. EFT of each participant was measured echocardiographically. The C-reactive protein (CRP) concentration and NLR were measured from venous blood samples.
Results
The 24-hour average systolic blood pressure was significantly higher in the hypertension group than in the control group (143±17 vs. 117±7 mmHg, respectively). There were no significant differences in age, sex, or body mass index between the two groups. EFT, the NLR, and the CRP concentration were significantly higher in the hypertension group than control group. Additionally, a significantly positive correlation between EFT and the NLR was found in both the control group and hypertension group.
Conclusion
A higher EFT and NLR were detected in patients with newly diagnosed hypertension than in healthy subjects.
Keywords
Introduction
Hypertension is a global public health problem and one of the most common chronic diseases. Hypertension is related to cardiac disease, stroke, renal disease, premature death, and morbidity, all of which are substantial burdens to health care and the economy. 1 However, hypertension is a preventable and treatable disease.
Twenty-four-hour ambulatory blood pressure monitoring (ABPM) is the gold standard method for assessment of the efficiency of diagnosis and treatment of hypertension. 2 Treatment is directed according to the mean 24-hour blood pressure value, the average night and day blood pressure values, and the dipper/non-dipper characteristics of the blood pressure pattern.
Epicardial fat tissue is a visceral fat tissue with paracrine, vasocrine, and inflammatory effects located around the heart and coronary arteries. In healthy individuals, its thickness is about 5 mm. Previous studies have demonstrated that epicardial fat tissue is associated with coronary artery disease, metabolic syndrome, insulin resistance, and hypertension. In physiological conditions, epicardial fat tissue acts as a buffer, protecting the heart from exposure to high free fatty acid levels by absorbing those free fatty acids. Additionally, epicardial fat tissue has protective effects on vascular function and contributes to the myocardial energy requirement.1–3 However, an increase in epicardial fat tissue may change this tissue to a lipolytic, prothrombotic, and proinflammatory organ.
The white blood cells (WBCs) and their subtypes are the most basic cells of inflammation. These cells are considered responsible for adverse events in patients with cardiovascular disease and are used as markers of inflammatory conditions. 4
Epicardial fat tissue thickness (EFT) and the neutrophil/lymphocyte ratio (NLR) are newly established cardiovascular risk markers currently used in the clinical setting. They indicate exposure to long-term risk factors. Therefore, these parameters may give information about the duration of hypertension in patients who have been newly diagnosed by ABPM. They may also be helpful in determining the intensity of treatment. In this study, we assessed the relationship between EFT and the NLR in patients who had been newly diagnosed with hypertension by ABPM.
Methods
Inclusion and exclusion criteria
In this prospective study, patients aged 18 to 55 years who had been admitted to the Cardiology Department from November 2015 to May 2016 for echocardiography and underwent 24-hour ABPM were included in the study. We excluded the following patients from the study: patients with a history of anti-hypertensive drug use in the past 6 months or with a diagnosis of systemic hypertension or secondary hypertension; patients with chronic renal disease (glomerular filtration rate of <60 ml/min), type 1 or 2 diabetes mellitus, known coronary artery disease, congestive heart failure, a left ventricular ejection fraction (LVEF) of <50%, moderate or severe heart valvular disease, hypertrophic cardiomyopathy, pericardial disease, chronic pulmonary disease, or pulmonary hypertension (pulmonary arterial systolic pressure of >30 mmHg); patients undergoing cardiac surgery for any reason; patients with congenital heart disease; patients followed for malignancy; patients with active infection or infection during the last 2 weeks; and patients with a hemoglobin level of <11.0 g/dl or WBC count of >12 × 103/µl or <4 × 103/µl.
General assessment and measurements
All patients’ medical history and physical examination findings were obtained and recorded. The waist circumference, body weight, and body height were measured, and the body mass index (BMI) was calculated using the following formula: BMI = weight (kg)/height (m) 2 . A BMI of >30 kg/m2 was considered to indicate obesity. A waist circumference of ≥102 cm for men and ≥88 cm for women was accepted as an increased waist circumference. 5
Echocardiographic examination
Echocardiographic examinations were performed at the Echocardiography Laboratory of the Cardiology Department using an EPIQ 7 echocardiography device (Philips, Amsterdam, Netherlands). The measurements were performed in the left lateral decubitus position as recommended by American Society of Echocardiography. 6
The epicardial fat tissue was accepted as the relatively nonechogenic space between the visceral pericardium and right ventricle. The maximum EFT was obtained by measuring the thickness of the space between the visceral pericardium and right ventricle in the parasternal long-axis view with the help of a two-dimensional image containing a line drawn perpendicular to the midventricular wall of the right ventricle at the end of systole. 7 Discrimination between systole and diastole was performed using the patients’ echocardiographic records. Measurements were performed by cardiologists blinded to the patient data. An EFT of ≥7 mm was considered high. 8
To determine the interobserver variability, 20 of the study patients were selected for echocardiographic evaluation, and EFT measurements were repeated after 1 week. Reproducibility of the measurements was statistically very significant (intraclass correlation coefficient of 0.921, p<0.001).
ABPM
ABPM was performed using an oscillometric GE CardioSoft Tonoport V (V6.51) blood pressure monitor (GE Healthcare, Milwaukee, WI, USA). Standard device settings were used for all patients between 08:00 and 23:00 for daytime measurements and between 23:00 and 08:00 for nighttime measurements. The blood pressure was automatically recorded by the device every 30 minutes during the day and every hour during the night. The patients were informed about these daytime and nighttime measurement periods. From the obtained ABPM values, the 24-hour mean systolic blood pressure (SBP) and diastolic blood pressure (DBP) (measured daily between 08:00 and 23:00 and nightly between 23:00 and 08:00) were automatically measured and recorded. Similarly, the average 24-hour daily and nightly pulse pressure values and 24-hour daily and nightly mean pulse rates were automatically measured by the device. The patients were divided into a control group and a hypertension group according to their 24-hour mean SBP and DBP values. Patients with a 24-hour mean SBP and DBP of ≥130 mmHg and/or ≥80 mmHg, respectively, were included in the hypertension group. Patients with SBP and DBP values lower than these thresholds comprised the control group. Patients with a decrease of >10% in the mean daytime SBP and/or DBP when compared with the mean nightly SBP and/or DBP were defined as dippers. Patients with a ≤10% decrease were defined as non-dippers.
Laboratory measurements
After the first admission and following a 12-hour fast, blood samples were obtained from the antecubital vein. Full blood counts were analyzed within 45 minutes of obtaining blood sample. The venous blood samples obtained for biochemical analysis were centrifuged at 3000 rpm. They were then stored at −80°C until analysis. Biochemical analyses were performed with an Architect Ci8200 (Abbott Laboratories, Lake Bluff, IL, USA), and full blood counts were performed with an XN-1000 Automated Hematology Analyzer (Sysmex, Tokyo, Japan). All analyses were performed by a laboratory technician who was blinded to the patient data. The following parameters were measured during the biochemical analysis: fasting blood glucose, creatinine, albumin, total protein, sodium, potassium, blood urea nitrogen, aspartate transaminase, alanine transaminase, uric acid, calcium, C-reactive protein (CRP), thyroid-stimulating hormone, total cholesterol, low-density lipoprotein, very-low-density lipoprotein, high-density lipoprotein, and triglycerides. The full blood count included measurement of the red blood cell count, hemoglobin, hematocrit, red cell distribution width (RDW), platelet count, platelet distribution width, WBC count, neutrophil count, and lymphocyte count. The ratio of the neutrophil count over the lymphocyte count was recorded as the NLR.
Statistical analysis
PASW Statistics for Windows, Version 18.0 (SPSS Inc., Chicago, IL, USA) was used for the statistical analysis. Categorical variables are shown as percentages, while numerical variables are shown as arithmetic mean ± standard deviation. The one-sample Kolmogorov–Smirnov test was used to determine whether the numerical variables showed a normal distribution. The following variables were not normally distributed: age; RDW; aspartate transaminase; sodium; potassium; albumin; neutrophil count; NLR; triglycerides; thyroid-stimulating hormone; creatinine; calcium; mean 24-hour SBP and DBP; mean arterial blood pressure (MAB); mean daytime SBP, DBP, MAB, and pulse pressure; mean nightly SBP, DBP, MAB, and pulse pressure; aortic diameter; aortic velocity;, left ventricular end-systolic diameter (LVESD); interventricular septum end-diastolic thickness (IVSd); posterior wall diastolic thickness; LVEF; left atrial (LA) diameter; pulmonary velocity; mitral E/A ratio; E/Em ratio; tissue Doppler imaging Am and Sm; and Em/Am ratio. The existence of a linear relationship between parameters with a normal distribution was assessed using Pearson’s correlation test, while the existence of a linear relationship between parameters without a normal distribution was evaluated using Spearman’s correlation test. For assessment of differences between the groups, Student’s t test was used for parameters with a normal distribution, while the Mann–Whitney U test was used for parameters without a normal distribution. The results were considered statistically significant at a p value of <0.05.
Ethics
The present study was approved by the Research and Ethics Committee of Bozok University (Yozgat, Turkey) (Approval year: 2015). All participants provided written informed consent before enrollment. If the participants were illiterate, written informed consent was obtained from their proxies. This study was performed according to the principles of the Declaration of Helsinki.
Results
Eighty consecutive normotensive patients (control group) and 80 consecutive hypertensive patients (hypertension group) were matched and analyzed in this study. Both groups were statistically similar in age, body weight, height, and waist circumference (Table 1). Although the number of patients with an increased waist circumference was higher in the hypertension group (n=48) than control group (n=43), the difference was not statistically significant. The number of obese patients in the hypertension group (n=31) was similar to that in the control group (n=33). There was an expected positive correlation between waist circumference and BMI (r=0.762; p<0.001).
Demographic and clinical data.

Data are presented as mean ± standard deviation or n (%).
CAD: coronary artery disease
Among all patients included in the study, the mean LVEF was 63%±2% and the mean EFT was 0.58±0.16 cm. In both groups, the LVEDD, LVESD, LVEF, and pulmonary artery systolic pressure were statistically similar (Table 2). The EFT in the hypertension group was significantly higher than that in the control group (p<0.001).
Echocardiographic measurements.

Data are presented as mean ± standard deviation or n (%).
EF: ejection fraction; EFT: epicardial fat tissue thickness; IVS: interventricular septum; TDI: tissue Doppler imaging; Em: early diastolic velocity; Am: late diastolic velocity; Sm: peak systolic velocity; LVEDD: left ventricular end-diastolic diameter
The 24-hour mean SBP, DBP, and MAB in the hypertension group were significantly higher than those in the control group (Table 3). Among the patients with newly diagnosed hypertension, the EFT of dippers was significantly lower than that of non-dippers (0.59±0.12 and 0.66±0.15 cm, respectively; p<0.05). Similarly, the NLR of dippers was significantly lower than that of non-dippers (2.50±1.52 and 3.45 ± 2.37, respectively; p<0.05).
Ambulatory blood pressure values.
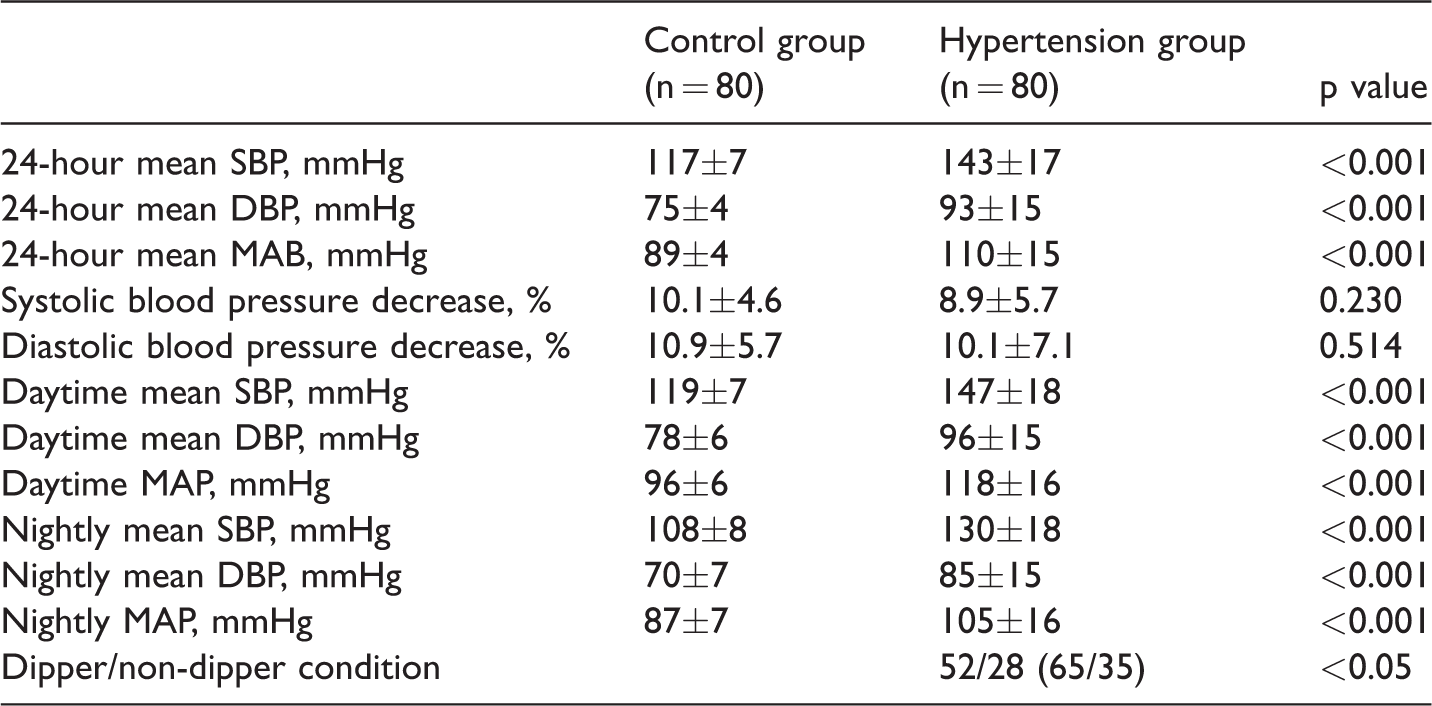
Data are presented as mean ± standard deviation or n (%).
DBP: diastolic blood pressure; MAP: mean blood pressure; SBP: systolic blood pressure
The laboratory values in each group are shown in Table 4. The neutrophil count and NLR in the hypertension group were significantly higher than those in the control group (p<0.001 for both). However, the lymphocyte count in the hypertension group was significantly lower than that in the control group (p<0.005). The CRP level in the hypertension group was significantly higher than that in the control group (p<0.001).
Laboratory values.
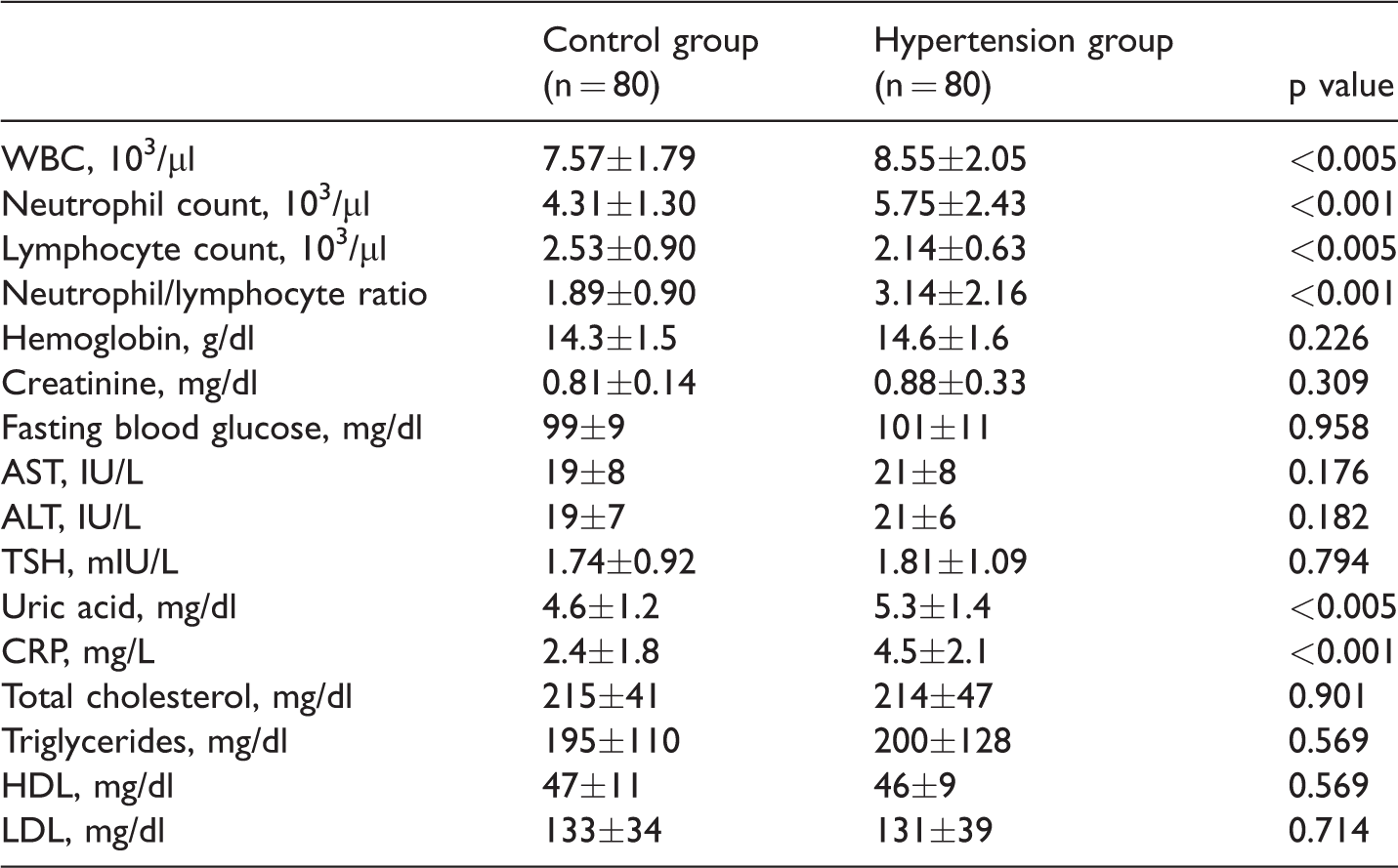
Data are presented as mean ± standard deviation.
ALT: alanine transaminase; AST: aspartate transaminase; CRP: C-reactive protein; HDL: high-density lipoprotein; LDL: low-density lipoprotein; TSH: thyroid-stimulating hormone; WBC: white blood cell
Among all patients, age was positively correlated with EFT (r=0.228, p<0.005) but showed no correlation with the NLR (r=0.011) or CRP (r=0.023). A positive correlation was observed between EFT and the NLR (r=0.409, p<0.001). Similarly, CRP was positively correlated with both EFT (r=0.349, p<0.001) and the NLR (r=0.343, p<0.001). In a correlation analysis including all patients, the 24-hour mean SBP was positively correlated with CRP (r=0.372, p<0.001), EFT (r=0.434, p<0.001), and the NLR (r=0.423, p<0.001) values. However, the 24-hour mean SBP showed no correlation with age (r=0.020).
Discussion
Hypertension is a common public health problem and an important cause of both morbidity and mortality. Hypertension usually progresses asymptomatically until it causes clinical end-organ damage, and this characteristic of the disease delays the diagnosis. Detection of end-organ damage in the subclinical period therefore has great importance for the treatment of hypertension. For this purpose, arterial stiffness and an increased carotid intima–media thickness are used as markers of subclinical atherosclerosis in hypertensive patients.9,10 Unfortunately, no study has focused on the importance of EFT and the NLR in hypertensive patients. Thus, in the present study, EFT and the NLR were compared between hypertensive patients and a control group. We found that EFT and the NLR were significantly higher in the newly diagnosed hypertensive patients than in the control group.
In patients with systemic hypertension that has been poorly controlled for a long period of time, diastolic dysfunction initially develops, and left ventricular hypertrophy with an increase in the LA diameter and loss of aortic elasticity occurs as a result of continuous high blood pressure.11,12 Similarly, both the LA diameter and aortic diameter (a marker of aortic stiffness) were increased in the present study. Additionally, the left ventricular wall thickness was higher in the hypertensive patients than in the control group. In mitral flow samples, the pseudonormal pattern frequency was also significantly higher in the hypertensive patient group. All of these findings are caused by the direct effect of high blood pressure on the heart. 13
The epicardial fat tissue is the fatty tissue between the visceral pericardium and epicardium and is independent of the mechanical or direct effects of blood pressure. 14 A relationship between the epicardial fat tissue and atherosclerotic cardiovascular disease has been demonstrated. Additionally, the epicardial fat tissue has been shown to be associated with some clinical conditions including diabetes, metabolic syndrome, and psoriasis, which may become risk factors for coronary artery disease.15,16 In the present study, EFT in the newly diagnosed hypertension group was significantly higher than that in the control group (p<0.001). This finding reflects the cardiovascular risk in patients newly diagnosed with hypertension. Hypertension itself triggers inflammation of vascular structures and increases the risk of atherosclerosis.17,18 The epicardial fat tissue is not a simple fat tissue because it has metabolic and endocrine functions and secretes proinflammatory cytokines such as interleukin 1, interleukin 8, interleukin 6, and tumor necrosis factor α. Moreover, its vasocrine function allows for regulation of vascular tonus. 19 All of these characteristics reflect the dynamic structure of the epicardial fat tissue. In the present study, we used CRP as a marker of inflammation and found that the CRP levels in patients with newly diagnosed hypertension were significantly higher than those in the control group (p<0.001).
Previous studies have assessed the role of EFT in patients with hypertension. Those studies were generally performed in hypertensive patient populations and did not include comparison with healthy individiuals.20,21 Zhou et al. 20 found that the epicardial fat tissue volume measured via tomography was significantly higher in non-dippers than in dippers. Sengul et al. 21 reported that EFT as measured by echocardiography was significantly higher in non-dippers than in dippers in a population of patients with newly diagnosed hypertension. In the present study, we included both patients with newly diagnosed hypertension as well as normotensive individuals. Additionally, in our subgroup analysis, EFT as measured by echocardiography was significantly lower in dippers than in non-dippers in our population of patients with newly diagnosed hypertension (0.59±0.12 vs. 0.66±0.15 cm, respectively; p<0.05). Because the EFT was significantly higher in non-dippers, our study results are consistent with the literature. Additionally, in a correlation analysis including all patients, EFT showed a significant correlation with 24-hour SBP (r=0.434, p<0.001), IVSd (r=0.332, p<0.001), and LA diameter (r=0.265, p<0.001). According to these results, measuring EFT in addition to performing a standard echocardiographic examination in patients presenting with high blood pressure might be helpful to determine whether these patients have had long-term hypertension. Considering that the effects of hypertension on the heart (increased LA diameter, increased LV muscle mass, etc.) take at least 6 months to develop, wide-range randomized studies are required to determine the role of increased EFT as a structural marker for deciding the treatment intensity in hypertensive patients. 22
The waist circumference and BMI were compared between the hypertension and control groups. In study, we used the World Health Organization criteria to set cut-off points defining abnormal values. 5 However, other criteria for waist circumference also exist. 23 We found no significant difference in the waist circumference or BMI between the groups.
Many studies have recently been performed to identify the relationships between hematological parameters and cardiovascular disease or risk factors.24,25 Examples of these hematological parameters include the NLR; RDW; platelet/lymphocyte ratio; neutrophil, monocyte, and basophil counts; hemoglobin; hematocrit; red blood cell count; and micro- and macrocytosis. 26 Considering that atherosclerosis itself is an inflammatory process that induces production of WBCs, especially neutrophils, the increase in the NLR and WBC counts in patients with atherosclerosis might be easily understood. 27 In the present study, we assessed the NLR and RDW. In a study of patients with systo-diastolic hypertension, Pusuroglu et al. 28 found that an increased RDW was related to end-organ damage (increased LV mass index, glomerular filtration rate, and urinary albumin concentration). However, their study included no control group. In the present study, the RDW was much higher in the patients with newly diagnosed hypertension than in the control group (p<0.05). Large prospective studies are required to obtain information about the course of RDW values after treatment.
The NLR has been used especially in studies of patients with acute coronary syndrome, and it has been suggested to have predictive value for estimating cardiovascular events. Only a few studies in the literature have compared patients with newly diagnosed hypertension versus healthy individuals. In a study performed by Kılıçaslan et al., 29 the highest NLR among patients with newly diagnosed hypertension was found in the non-dippers. Likewise, the highest NLR was found in the non-dippers in the present study (p<0.001). In another study of hypertensive patients, Cem et al. 30 detected a positive correlation between the NLR and aortic diameter. In the present study, we did not detect a significant correlation between the aortic diameter and NLR because we had excluded patients with an aortic diameter of >4.0 mm. In our study group, the mean aortic diameter was 3.25±0.28 cm, while this value was 4.34±0.33 cm in the study performed by Cem et al. 30 This difference may explain why there was no correlation between the NLR and aortic diameter.
The present study is different from others because the echocardiographically measured EFT, which is related to inflammatory processes and shows a correlation with atherosclerosis-associated cardiovascular risk, was compared with the NLR, another predictive cardiovascular risk marker. In the subgroup analysis of hypertensive patients, a positive correlation was observed between EFT and the NLR (r=0.534, p<0.001). This may indicate the existence of a common pathophysiological process affecting both the NLR and EFT similarly in patients with hypertension, considering that both parameters were higher in the hypertension group than in the control group. Wide-range randomized studies are required to further explore this issue.
In patients with newly diagnosed hypertension, parameters such as EFT as measured by echocardiography and the NLR and RDW obtained by a full blood count may be increased as markers that indicate long-term exposure of the cardiovascular system to high blood pressure. Additionally, measurement of the NLR is inexpensive and widely available. Thus, evaluation of these parameters in patients with newly detected hypertension in the clinical setting, before performing ABPM, may help the physician to identify patients with long-term exposure to high blood pressure without leading to a significant increase in the cost of managing hypertensive patients. Promptly referring such patients for a definitive diagnosis of hypertension by ABPM and starting appropriate treatment could prevent end-organ damage and might be useful clinically. Large-scale randomized prospective studies are required to determine the clinical importance of these findings.
Limitations
One limitation of our study is the low number of patients. Additionally, this was a cross-sectional study and included only patients admitted to polyclinics; therefore, the results may not be relevant to the general population or other patient groups. Another limitation is that this was an observational study. Thus, it may not provide efficient information or ideas about the pathophysiology of changes in the measured parameters. Additionally, the NLR and neutrophil and lymphocyte values were measured using only one blood sample of each included patient. These parameters obtained from one unique sample may not allow for long-term analysis.
Footnotes
Authors’ contributions
All authors contributed to the design, data acquisition, and data analysis. Mehmet Ali Derya, Vahit Demir, and Huseyin Ede participated in the design of the study, and Vahit Demir and Huseyin Ede performed the statistical analyses. Huseyin Ede conceived the study, participated in the study coordination, and helped to draft the manuscript. All authors read and approved the final manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
