Abstract
Objective
To compare the outcomes of patients with and without a mean serum potassium (K+) level within the recommended range (3.5–4.5 mEq/L).
Methods
This prospective cohort study involved patients admitted to the medical intensive care unit (ICU) of Siriraj Hospital from May 2012 to February 2013. The patients’ baseline characteristics, Acute Physiology and Chronic Health Evaluation II (APACHE II) score, serum K+ level, and hospital outcomes were recorded. Patients with a mean K+ level of 3.5 to 4.5 mEq/L and with all individual K+ values of 3.0 to 5.0 mEq/L were allocated to the normal K+ group. The remaining patients were allocated to the abnormal K+ group.
Results
In total, 160 patients were included. Their mean age was 59.3±18.3 years, and their mean APACHE II score was 21.8±14.0. The normal K+ group comprised 74 (46.3%) patients. The abnormal K+ group had a significantly higher mean APACHE II score, proportion of coronary artery disease, and rate of vasopressor treatment. An abnormal serum K+ level was associated with significantly higher ICU mortality and incidence of ventricular fibrillation.
Conclusion
Critically ill patients with abnormal K+ levels had a higher incidence of ventricular arrhythmia and ICU mortality than patients with normal K+ levels.
Introduction
Potassium (K+) is an important electrolyte that has been proven essential for normal functioning of the cardiovascular system, skeletal muscle, internal organs, and nervous system. The intracellular proportion of K+, which represents more than 98% of the total body K+, controls cell metabolism and the resting membrane potential. Intracellular K+ is essential for excitability and automaticity of myocardial cells and for the normal functioning of other cells. The normal serum K+ level is 3.5 to 4.5 mEq/L.1,2 An abnormal K+ level predisposes a patient to serious complications, especially cardiac arrhythmia and muscle weakness, which may provoke sudden cardiac arrest and/or respiratory failure. Critically ill patients are at risk for alterations in their serum K+ level. Reduced kidney function, the presence of metabolic acidosis, use of mechanical ventilation, and increases in cell turnover promote K+ accumulation. Certain medications such as insulin, sympathomimetic agents, and diuretics decrease serum K+, while spironolactone, angiotensin-converting enzyme inhibitors, and angiotensin receptor antagonists increase serum K+. Hypokalemia and hyperkalemia can both induce cardiac arrhythmias.3–5 Previous reports have revealed an association between the K+ level and outcomes of acute myocardial infarction 6 and cardiac surgery. 7 McMahon et al. 8 reported an increased 30-day mortality rate among patients with a high serum K+ level at the initiation of critical care. Based on our review of the literature, however, no study has compared the effects of normal and abnormal mean serum K+ levels in critically ill patients during medical intensive care unit (ICU) admission. Therefore, we conducted a prospective cohort study at our center to compare normal and abnormal serum K+ levels and to characterize the relationship between serum K+ and patient outcomes in critically ill patients admitted to the medical ICU of our institution.
Methods
This prospective cohort study involved critically ill patients admitted to the medical ICU of Siriraj Hospital from May 2012 to February 2013. Siriraj Hospital is Thailand’s largest university-based national tertiary referral center. Written informed consent was obtained from the patient or a legal guardian prior to inclusion in this study. The protocol for this study was approved by the Siriraj Institutional Review Board, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand (approval no. Si 424/2012). This study complied with all of the principles set forth in the Declaration of Helsinki (1964) and all of its subsequent provisions.
Patients aged >18 years who were expected to remain alive in the ICU for longer than 24 hours were included. Patients with active coronary artery disease or who were pacemaker-dependent were excluded. Patients admitted to the ICU after a major operation were also excluded. Recorded patient information included age, sex, underlying medical conditions, Acute Physiology and Chronic Health Evaluation II (APACHE II) score within the first 24 hours, and indications for ICU admission. The findings of essential investigations including 12-lead electrocardiogram (ECG) results and baseline laboratory data were also recorded. Certain therapeutic details were noted, such as the use of vasopressors, ventilatory support, and renal replacement therapy. Finally, patient outcomes including mortality, the ICU and hospital length of stay, and the presence of cardiac arrhythmias were recorded and included in the analysis.
Serum K+ measurements and outcomes
All serum K+ values measured during the first 14 days of ICU admission for each patient were recorded and used to calculate the average serum K+ level (Ka+) for each patient. To avoid errors in serum K+ measurement, the measured serum was drawn from a central or arterial line containing no K+ solution. The specimen was collected in a heparin-coated plastic tube and transferred directly to the central laboratory. The serum K+ level was then measured by an ion-selective electrode. A 14-day interval was used in this study because almost all arrhythmias reportedly occur within 14 days of ICU admission. 9 Patients were classified into two groups according to their serum K+ level. Patients with a Ka+ level of 3.5 to 4.5 mEq/L and with all individual K+ levels of 3.0 to 5.0 mEq/L were allocated to the normal K+ group. Patients who did not meet the aforementioned K+ criteria were allocated to the abnormal K+ group.
The primary outcome in this study was ICU and hospital mortality, and the secondary outcome was the incidence of arrhythmia and the ICU and hospital length of stay. During ICU admission, continuous ECG monitoring was performed and the results recorded by the IntelliVue Information Center of the Philips Patient Care System (Philips Healthcare, Best, Netherlands). Arrhythmia was suspected if the heart rate was <50 beats/min, >120 beats/min, or irregular. Once arrhythmia was suspected, a 12-lead ECG was performed. Diagnosis of arrhythmia was made by an attending critical care physician and confirmed by a cardiologist.
Statistical analysis
Data analysis was performed using SPSS Statistics version 20 (IBM Corp., Armonk, NY, USA). Continuous variables are shown as mean ± standard deviation, and categorical variables are reported as the percentage of the total number of patients in that group. To detect a difference in clinical characteristics between two groups, Student’s t-test was used for continuous variables and Fisher’s exact test or Pearson’s chi-square test was used for categorical variables. A two-sided
Results
Serum K+ levels and patient characteristics
In total, 160 critically ill patients were included. Their mean age was 59.3±18.3 years, 52.5% were men, and the mean APACHE II score was 21.8±14.0. The mean ICU and hospital lengths of stay were 11.8±14.0 and 30.8±32.4 days, respectively. The mean serum K+ level was 3.9 mEq/L. Seventy-four patients were allocated to the normal K+ group, while 86 patients were allocated to the abnormal K+ group.
The baseline demographic and clinical characteristics of patients in both groups are shown in Table 1. There were no significant differences in age, sex, or underlying conditions between the groups. The mean APACHE II score and proportion of patients with previously diagnosed coronary artery disease were both higher among patients in the abnormal K+ group. Severe sepsis or septic shock was the leading cause of ICU admission, followed by acute respiratory failure, requirement for mechanical ventilatory support, shock from other causes, and congestive heart failure.
Baseline demographic and clinical characteristics of patients in the normal and abnormal serum K+ groups

Data are presented as mean ± standard deviation or n (%).
The patients’ baseline laboratory results revealed an increased serum creatinine level in both groups. The serum chloride and bicarbonate levels were significantly lower in the abnormal than normal K+ group (
Serum K+ level and hospital outcomes
The mean serum K+ level during ICU admission was significantly higher in the normal than abnormal K+ group. Most (46.5%) patients in the abnormal K+ group had a Ka+ level of <3.5 mEq/L. About 40.7% of patients with an abnormal K+ level had a mean serum K+ level in the normal range (3.5–4.5 mEq/L) but had an individual K+ level of >5.0 or <3.0 mEq/L. Only 12.8% of patients in the abnormal K+ group had a Ka+ level of >4.5 mEq/L.
The ICU mortality and hospital mortality rates were 32.5% and 43.8%, respectively. Compared with the normal K+ group, abnormal mean serum K+ levels were associated with significantly higher ICU mortality (24.3% vs. 39.5%,
Outcomes of patients in the normal and abnormal serum K+ groups
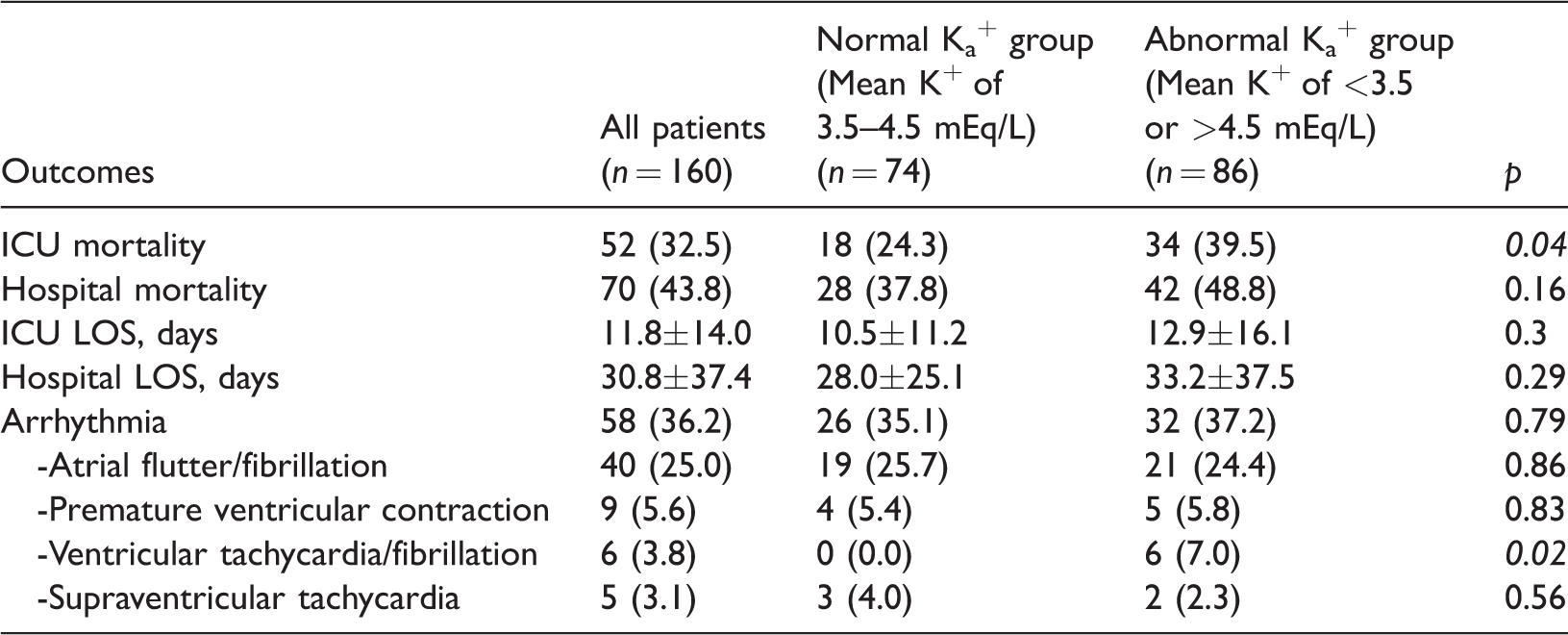
Data are presented as mean ± standard deviation or n (%).
Serum K+ levels and cardiac arrhythmias
Cardiac arrhythmia was detected in 36.2% of patients. The leading type of arrhythmia was atrial fibrillation in 39 patients (24.8%), followed by premature ventricular contraction in 10 patients (5.7%), supraventricular tachycardia in 6 patients (3.7%), and ventricular tachycardia or fibrillation in 6 patients (3.7%). The incidence of overall arrhythmia was not significantly different between the groups. However, a significantly higher incidence of malignant arrhythmia (i.e., ventricular tachycardia and ventricular fibrillation) was found among patients in the abnormal K+ group (
Predictive factors significantly associated with ICU mortality
A univariate analysis was performed to identify independent factors associated with ICU mortality. Eight independent factors were identified: an APACHE II score of ≥20, ICU admission diagnosis of septic shock, presence of metabolic acidosis, baseline creatinine level of ≥2 mg/dL, abnormal serum Ka+ level, requirement for vasopressor support, requirement for mechanical ventilator support, and requirement for renal replacement therapy. All eight parameters were then included in the multivariate analysis, which showed that a requirement for vasopressor therapy (
Factors associated with ICU mortality

Discussion
The findings of this study demonstrate that an abnormal serum K+ level during the first 2 weeks of ICU admission is associated with adverse patient outcomes. ICU mortality was significantly higher among patients in the abnormal Ka+ group. Hospital mortality was also higher in the abnormal group, but the difference did not achieve statistical significance. This can be partially explained by the increased incidence of malignant arrhythmia, especially ventricular tachycardia and ventricular fibrillation, in the abnormal K+ group. These findings support the evidence that serum K+ has a significant impact on patient outcomes, including critically ill patients.
Information from previous studies has suggested that the K+ level at both admission and during post-admission is associated with the outcomes of patients with acute myocardial infarction and those who have undergone cardiac surgery, but not of those who have undergone general surgery. Goyal
Data from a large prospective observational case-control study of 2,402 patients who underwent elective coronary artery bypass surgery showed an association between the preoperative serum K+ level and patient outcomes. 7 The incidence of perioperative arrhythmia, intraoperative arrhythmia, postoperative atrial fibrillation/flutter, and the need for cardiopulmonary resuscitation were higher among patients with a preoperative serum K+ level of <3.5 mEq/L. However, this association was not observed in patients who underwent general abdominal surgery 10 or elderly surgical patients. 11
Critically ill patients, who are frequently affected by organ dysfunction and often receive multiple medications that affect K+ regulation, are at high risk of developing abnormal K+ levels. A large retrospective observational study of critically ill medical and surgical patients who were admitted to the ICU showed that a K+ level at ICU admission of >4.5 mEq/L was a strong independent predictor of 30-day all-cause mortality.
8
The risk of death in that study increased with an increasing K+ level. However, the authors did not mention the post-admission K+ levels. They also did not report the incidence of cardiac arrhythmias or other complications associated with abnormal K+ levels Hessels
Although the mean post-admission K+ level was selected as the parameter with which to determine patient outcomes in some previous studies, some patients whose mean K+ level was within the normal range may have had individual K+ levels outside the normal range. Transient abnormality in the K+ level, either too low or too high, may affect patient outcomes. Cardiac arrhythmia can occur during hypokalemic or hyperkalemic states, and the results of our study confirm this hypothesis. Our study showed that the incidence of life-threatening arrhythmia (specifically ventricular tachycardia/fibrillation) was significantly different between the two groups (
The association between an abnormal K+ level and increased ICU mortality may be influenced by other factors. The univariate and multivariate analysis results of eight parameters (APACHE II score of ≥20, presence of septic shock, presence of metabolic acidosis, creatinine level of >2 mg/dL, abnormal mean serum K+ level, requirement for vasopressor support, requirement for mechanical ventilator support, and requirement for renal replacement therapy) are presented in Table 3. In the multivariate analysis, a requirement for vasopressor therapy and requirement for renal replacement therapy were identified as independent factors associated with ICU mortality. An abnormal mean serum K+ level alone was not found to be significantly associated with ICU mortality. This finding suggests that an abnormal serum K+ level is not a direct or independent cause of death among patients in the medical ICU. Rather, patient conditions and required treatments that affect the serum K+ level are the main factors that determine patient outcome. Renal failure, which requires renal replacement therapy, may cause an abnormal K+ level that in turn increases ICU mortality. Vasopressors, which mainly activate adrenergic receptor agonists, cause a shift of extracellular K+ into intracellular fluid that, in turn, aggravates hypokalemia. 13
This study has some mentionable limitations. First, we had no information regarding the primary outcome between the abnormal and normal K+ groups, and we did not perform a sample size calculation. This might have been a limitation of this study. Second, no structured protocol or schedule for blood chemistry examination was established for this study. Electrolytes, including K+, were tested once a day in the morning in almost every patient (excluding those with a signed do-not-resuscitate order. Additional blood sampling was performed at the discretion of the attending physician and based on each individual patient’s condition. As such, we were unable to analyze the timing relative to when the serum K+ level was outside the normal range. Third, we did not include the treatment modality employed to correct abnormal K+ levels in our analysis. This is another factor that could affect patient outcomes. Finally, the hyperkalemic stage is characterized by a typical ECG pattern 14 ; thus, patients with a high serum K+ level may be detected and treated early before they develop a significant arrhythmia. Given that there is no specific ECG pattern for detecting hypokalemia, the resulting delay in detection and treatment facilitates the development of complications.
Conclusion
An abnormal serum K+ level itself was not found to be an independent predictive factor for ICU mortality; however, critically ill patients with abnormal K+ levels had a higher incidence of ventricular arrhythmia and ICU mortality than patients with normal K+ levels. Individual patient conditions and treatments were found to be associated with ICU mortality. The multivariate analysis showed that a requirement for vasopressor administration and renal replacement therapy were the two factors significantly associated with ICU mortality in this study.
Footnotes
Authors’ contributions
ST developed the study protocol, performed and statistical analysis, and drafted the manuscript. TV took part in the data collection and manuscript preparation. CP carried out the protocol development and manuscript preparation. All authors read and approved the final manuscript.
Acknowledgment
The authors gratefully acknowledge Dr. Kevin P. Jones for considerable help with language correction and the medical ICU nurses and physicians for their support.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research was supported by the Siriraj critical care research fund, which had no role in the conducting of the study or reporting of the results.
