Abstract
Objective
To investigate the impact of goal-oriented hemoperfusion (HP) with monitoring of the paraquat concentration on the prognosis of patients with acute paraquat poisoning.
Methods
This prospective observational study involved patients with acute paraquat poisoning admitted from March 2012 to September 2015. The patients received either goal-oriented or routine HP. All other treatments were the same between the two groups. The primary endpoint was 28-day mortality after poisoning. The secondary endpoints were the incidence of organ dysfunction within 7 days and 7-day mortality.
Results
Eighty-four patients were enrolled (49 in the control group and 35 in the goal-oriented group). The two groups were similar in terms of clinical characteristics. There was no significant difference in the incidence of organ dysfunction between the two groups within 1 week of admission. Mortality on day 7 was significantly lower in the goal-oriented than control group, but there was no difference on day 28. However, 28-day mortality was significantly lower in the goal-oriented group among patients with an oral dose of ≤50 ml.
Conclusions
HP with monitoring of the urine paraquat concentration as goal-oriented therapy can reduce the early mortality of paraquat poisoning.
Introduction
Paraquat is a herbicide widely used for agricultural production in developing countries because of its rapid effect and low environmental residues; however, paraquat is very toxic to humans. 1 Oral ingestion of 5 to 15 ml of 20% paraquat can be fatal. There is no specific antidote, and the mortality rate after ingestion of 40 to 50 ml can thus reach >90%.2–4 Paraquat poisoning is one of the most common causes of pesticide poisoning in China. 5
The clinical course of paraquat poisoning depends upon the quantity ingested.6,7 Ingestion of large amounts of paraquat (40–50 ml at 20% concentration) leads to fulminant organ failure due to fulminant oxidative stress, lipid peroxidation, mitochondrial toxicity, oxidation of nicotinamide adenine dinucleotide phosphate, activation of nuclear factor κB, and apoptosis. 3 Ingestion of small amounts of paraquat (5–15 ml at 20%) will usually lead to kidney and lung toxicity over the next 2 to 6 days. 3
In the early treatment of acute paraquat poisoning, besides routine detoxification strategies such as gastric lavage, absorption, and catharsis, removal of blood paraquat through blood purification is an important procedure. Studies have shown that hemoperfusion (HP) is one technique with which to remove blood paraquat and that it can improve the prognosis of some patients.8,9 The clinical efficacy of HP is based on early and complete removal of blood paraquat.3,10 In clinical practice, however, HP is often carried out without dynamic monitoring of the paraquat concentration.2,3,8,9 This blind approach could affect the clinical results because the completeness of paraquat clearance is difficult to ascertain.
This prospective observational study proposes an HP blood purification regimen with monitoring of the urine paraquat concentration as goal-oriented therapy. The prognosis of patients with paraquat poisoning treated with goal-oriented HP was compared with that of routine HP + continuous venovenous hemofiltration (CVVH).
Materials and methods
Study design and patients
This was a prospective observational study. Patients with acute oral paraquat poisoning admitted to the Department of Emergency Medicine of our hospital from March 2012 to September 2015 were consecutively recruited.
The inclusion criteria were as follows: (1) The patients or their families provided a clear history of paraquat ingestion (for those patients who refused to admit to poison ingestion, paraquat ingestion was considered in the circumstantial presence of a suicide note and empty paraquat container, dark green clothing or skin residue, or clinically unexplained vomiting, bleeding, or ulceration of the oral mucosal after a few hours and with positive qualitative determination of paraquat in the urine); and (2) the patients had an expected survival time of >24 h after admission. The exclusion criteria were as follows: (1) The time from poison ingestion to hospital admission was >24 h, (2) the patients were <16 or >75 years of age, (3) a semi-quantitative test of urinary paraquat was negative, (4) the time from taking paraquat to HP was >24 h, (5) the paraquat had been ingested in combination with any other poison, (6) the patients had a history of chronic disease or end-stage disease (such as New York Heart Association Class IV heart failure or the uremic stage of renal failure), (7) the patients did not receive HP for various reasons, (8) the patients did not complete the conventional therapy, or (9) follow-up was not performed within 28 days.
The ethics committee of our hospital approved the present study. All patients provided written informed consent after treatment and before discharge (Ethical approval number: LS20120307). The work described herein was carried out in accordance with The Code of Ethics of the World Medical Association (Declaration of Helsinki) for experiments involving human subjects.
Grouping
The patients were divided into two groups according to the paraquat blood purification regimen: the control group and the goal-oriented group. The control group comprised patients who underwent two routine HP sessions after admission and sequential CVVH. The goal-oriented group comprised patients who underwent HP therapy guided by urine paraquat monitoring after admission (the number of HP sessions was dependent on the paraquat urinary level) together with non-conventional sequential CVVH treatment after HP. Any other conventional treatments were the same between the two groups. The patient chose the treatment regimen after discussion among the patient, his or her family, and the attending physician. The patient’s financial status and medical insurance were also taken into consideration.
Data collection
The patients’ demographic characteristics, oral dose, time interval from poisoning to gastric lavage, time interval from poisoning to HP, number of HP sessions, and medical history were recorded. After undergoing emergency treatments at our hospital, the laboratory data of the patients (worst values within 24 h) for routine blood tests, liver and kidney function, blood gas analysis, blood lactic acid, and Acute Physiology and Chronic Health Evaluation II scores were recorded. 11
Semi-quantitative detection of paraquat in urine
Sodium dithionite reagent coloration was used to semi-quantitatively detect the urine paraquat concentration. According to the final degrees of coloration of the urine samples, the corresponding paraquat contents were obtained after comparison with the color chart (Figure 1). The detection kit was manufactured by Syngenta (Beijing, China).

Color scale for semi-quantitative analysis of urine paraquat concentration.
Blood purification regimen in the goal-oriented group
HP was started within 2 h after admission to the emergency room, and each HP session lasted 2 h. The perfusion system was a Zhuhai Jafron HA230 system (Jafron Biomedical Co., Ltd., Zhuhai City, China). Anticoagulation was performed with unfractionated heparin. An Arrow 12-Fr dual-lumen hemodialysis catheter (Arrow International Inc., Wayne, PA, USA) was placed in the femoral vein, and the blood flow velocity was controlled at 200 to 250 ml/min. Measurement of the urine paraquat concentration was repeated after completion of each HP session. If the results suggested that the content was ≥3 µg/ml, HP was continued until the urine detection turned negative. During the subsequent 48 h, the urine paraquat concentration was detected every 6 h, and if the concentration was again ≥3 µg/ml, another HP session was performed. This protocol was repeated until negative urine detection was achieved as the standard of stopping HP. If the patients did not develop acute renal injury, sequential CVVH was not performed after HP.
Blood purification regimen in the control group
HP was started within 2 h after admission to the emergency room using the same methods as for the goal-oriented group. After two sessions of HP, sequential CVVH was performed using a Prismaflex M100 system (GAMBRO Industries, Meyzieu Cedex, France). The blood flow rate was set at 100 to 150 ml/min and the filtration rate at 1500 to 2000 ml/h. If no renal injury occurred, then the procedures were continued for 2 to 3 days.
Conventional therapy
According to the relevant clinical studies,3,10,12–14 a treatment protocol for paraquat poisoning was designed, and all enrolled patients underwent the following management regimen. (1) Immediate gastric lavage: early and thorough gastric lavage with water was performed at admission. (2) Adsorption and catharsis: 100 g of activated charcoal and 250 ml of 20% mannitol were immediately injected via the gastric tube after gastric lavage. Subsequently, 50 g of activated charcoal was intragastrically injected every 4 h alternating with 100 ml of 20% mannitol. Adsorption and catharsis were stopped after 24 h when charcoal was seen in the stool. (3) Antioxidant free radical therapy: acetylcysteine (Fluimucil; Zambon S.P.A., Bresso, Italy) was orally administered at 70 mg/kg every 4 h for a total of 17 doses, with a double dose administered the first time. Reduced glutathione was intravenously infused at 50 mg/kg/d for 24 h. Vitamin C was intravenously infused at 4 g/d for 24 h. (4) Immunomodulatory treatment: 500 mg of methylprednisolone was perfused every 12 h for 3 days together with sequential dexamethasone at 5 mg every 6 h by an intravenous drip for 14 days. The oxygen partial pressure was maintained at >80 mmHg; if the oxygen partial pressure was <60 mmHg, then 500 mg of methylprednisolone was injected once every 12 h for 3 days. The sequential reduction was to be maintained for 1 to 2 months. Cyclophosphamide (10–15 mg/kg/d) was intravenously infused for 6 h for 2 days. (5) Respiratory support: Conventional oxygen therapy was avoided unless the oxygen partial pressure was <40 mmHg or acute respiratory distress syndrome occurred, and an excessively high oxygen partial pressure was avoided when inhaling oxygen (the partial pressure was maintained at 60–90 mmHg). The blood lactic acid level was maintained in the normal range, and noninvasive/invasive respiratory support was given if needed. (6) Renal support: early hemodynamic monitoring was performed to ensure effective renal perfusion. Timely continuous renal replacement therapy was performed when the criteria of the Acute Kidney Injury Network (AKIN1) were met 15 or an irreversible internal environmental disturbance occurred. (7) A proton pump inhibitor and sucralfate were administered to protect the digestive tract mucosa.
Study endpoints
The primary endpoint was 28-day mortality after poisoning. The secondary endpoints were the incidence of organ dysfunction within 7 days and 7-day mortality. Acute respiratory failure was defined as the presence of hypoxemia (oxygen partial pressure of <60 mmHg without oxygen therapy or a decrease to ≥30% compared with baseline). 16 Acute circulatory failure was defined as systolic blood pressure of <90 mmHg, mean arterial blood pressure of <65 mmHg, or blood lactate level of >2 mmol/L combined with cyclic hypoperfusion of an organ (oliguria, consciousness change, pale skin, etc.). 17 Acute renal injury was defined according to the AKIN1 criteria. 15
Stratification analysis
According to the relevant literature, a 40- to 50-ml oral dose of 20% paraquat represented severe poisoning.3,8,18 Therefore, a 50-ml oral dose of paraquat was selected as the stratification standard in this study.
Statistical methods
Normality of continuous data was analyzed using the Kolmogorov–Smirnov test. If a normal distribution was satisfied, the data were analyzed using Student’s t test and are presented as mean ± standard deviation. Categorical data were analyzed using Fisher’s exact test and are presented as percentages. Kaplan–Meier survival curves were used to compare the survival rates between the two groups. Statistical analysis was performed using SPSS 19.0 (IBM Corp., Armonk, NY, USA). Two-sided P-values of <0.05 were considered statistically significant.
Results
Patients’ characteristics
In total, 139 patients were admitted during the study period, and 84 were eligible (49 in the control group and 35 in the goal-oriented group) (Figure 2). All patients had been poisoned by oral ingestion of 20% paraquat. There were no significant differences in the clinical baseline data between the two groups (Table 1).

Flowchart of patients. HP, hemoperfusion.
Comparison of relevant clinical data of the two groups of patients at admission (n = 84)

Except sex, data are presented as mean ± standard deviation. HP: hemoperfusion; APACHE II: Acute Physiology and Chronic Health Evaluation II; PaO2: partial pressure of oxygen; PaCO2: partial pressure of carbon dioxide.
HP in the goal-oriented group
Among the patients in the goal-oriented group, one underwent five sessions of HP and five underwent four sessions (Figure 3). No HP-related complications occurred in the two groups.
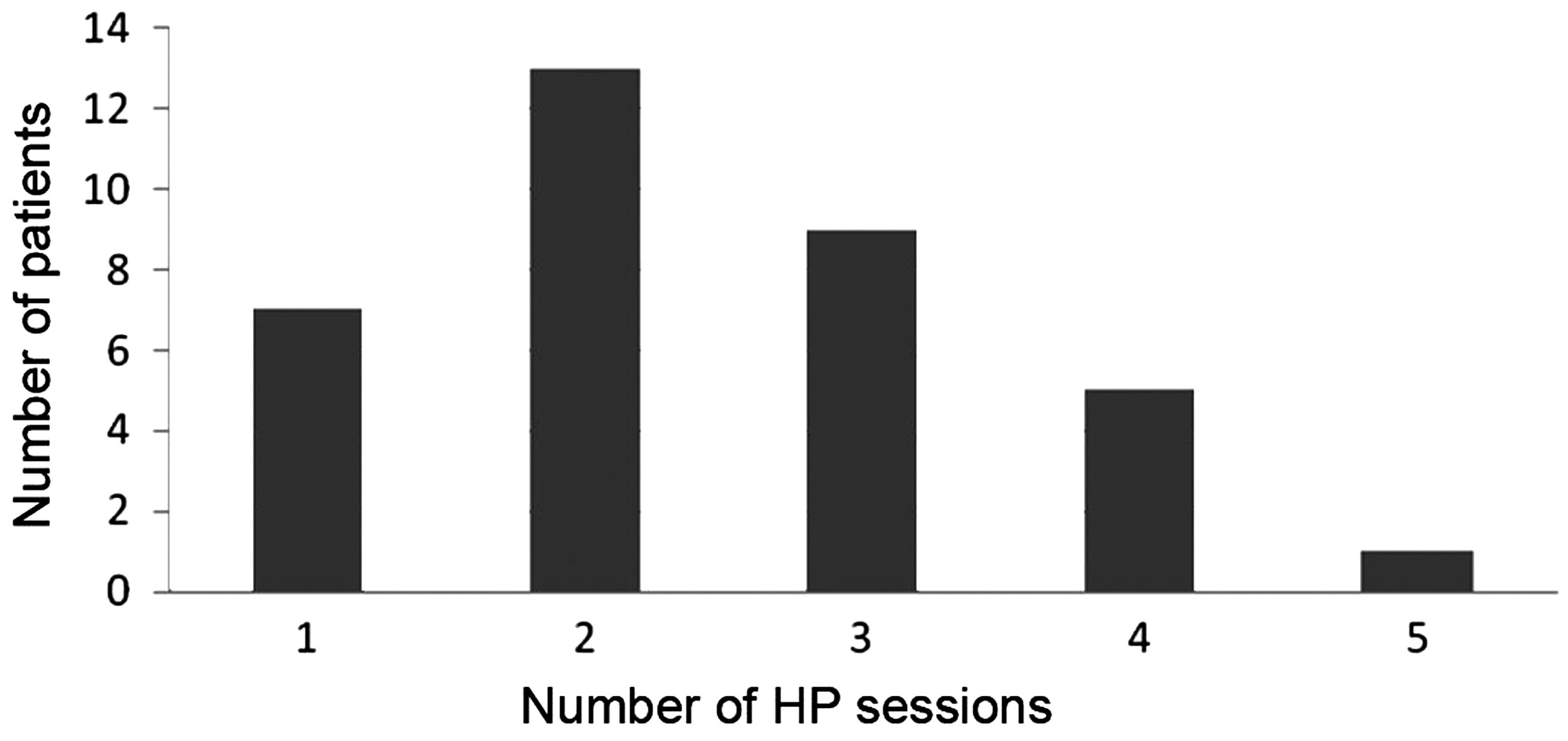
Number of hemoperfusion sessions in the goal-oriented group. HP, hemoperfusion.
Prognosis
There was no significant difference in the incidence of organ dysfunction between the two groups within 1 week of admission. The 7-day mortality rate in the goal-oriented group was significantly lower than that in the control group (P = 0.024). There was no significant difference in the 28-day mortality rate between the two groups (Table 2 and Figure 4).
Comparison of prognosis between the two groups

Data are presented as n (%).
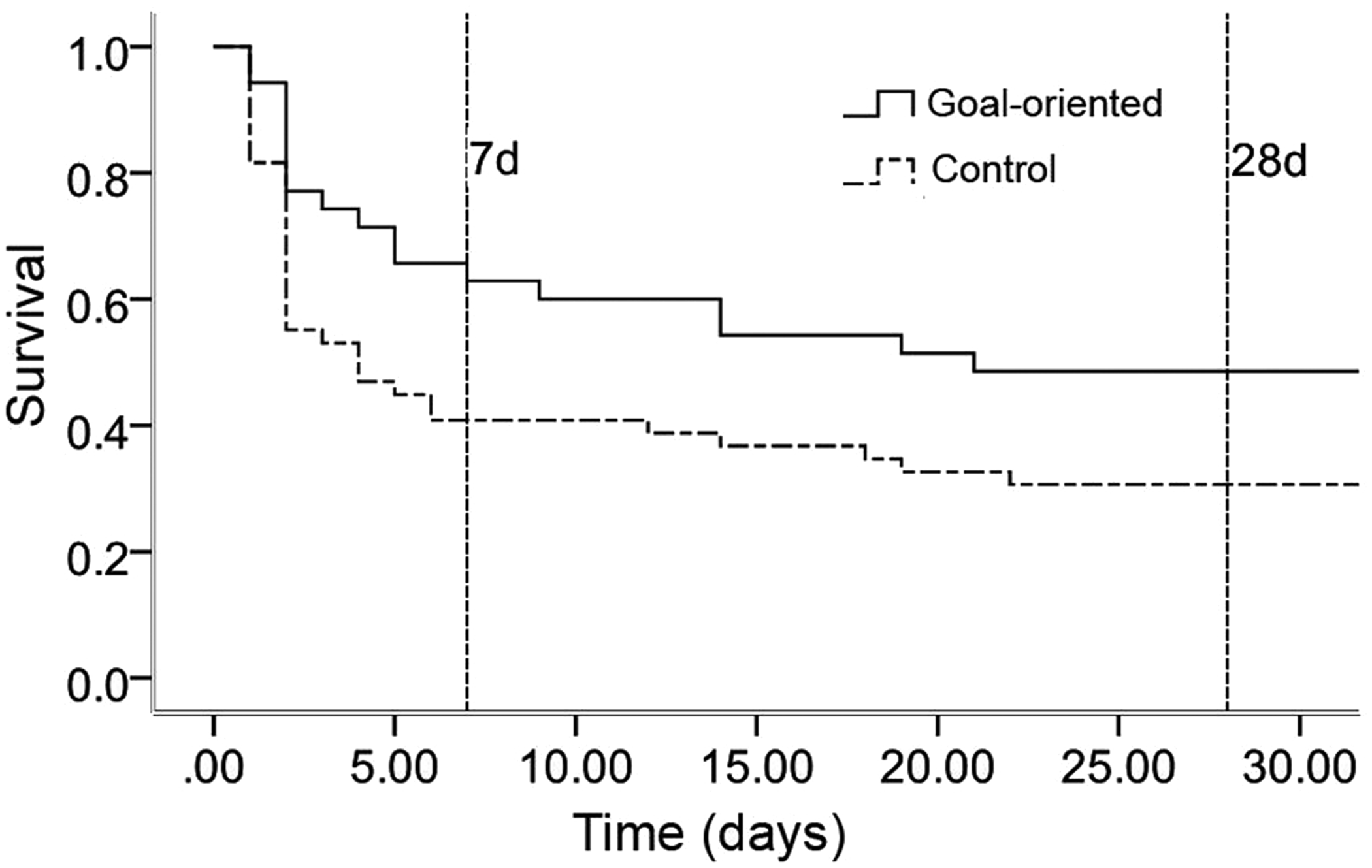
Kaplan–Meier survival analysis of the patients in the two groups.
Comparison of 28-day prognosis after stratification
The two groups were stratified based on the oral dose of paraquat. No significant difference was observed in the demographic characteristics, poisoning status, or laboratory test results (Table 3). The 28-day mortality rate of patients with an oral dose of ≤50 ml in the goal-oriented group was significantly lower than that in the control group (P = 0.034) (Figure 5).
Comparison of clinical data of patients with an oral dose ≤50 and >50 ml of paraquat

Except sex, data are presented as mean ± standard deviation. HP: hemoperfusion; APACHE II: Acute Physiology and Chronic Health Evaluation II; PaO2: partial pressure of oxygen; PaCO2: partial pressure of carbon dioxide.

Comparison of the 28-day mortality rate between the two groups after stratification based on the paraquat dose: (a) <50 ml, (b) >50 ml.
Discussion
The clinical efficacy of HP for paraquat poisoning is based on early and complete removal of blood paraquat.2,3,8,10,19 However, it is usually performed without dynamic monitoring of the paraquat concentration.2,9,20 Therefore, we investigated the impact of HP with paraquat concentration monitoring as goal-oriented therapy on the prognosis of patients with acute paraquat poisoning. The results suggest that HP with monitoring of the urine paraquat concentration as goal-oriented therapy improved the adequacy of HP.
Monitoring of the serum paraquat level has high requirements for hardware equipment and is difficult to apply in the clinical setting because of shortcomings such as the complex process of the test and the delay in obtaining the test results.8,21 Therefore, in the present study, semi-quantitative detection of the urine paraquat concentration was performed using a colorimetric method based on sodium hyposulfite. This method is simple to perform, and the results can be obtained rapidly and directly; in addition, the semi-quantitative urinary result correlates well with the blood paraquat concentration.16,22
On this basis, we developed an HP blood purification regimen with monitoring of the urine paraquat concentration as goal-oriented therapy to improve the adequacy of paraquat clearance with HP. This was achieved by dynamically evaluating the paraquat clearance efficacy. The results of the present study strongly suggest that compared with the routine treatment (i.e., two sessions of HP with CVVH), the goal-oriented group not only received individualized treatment but also exhibited improved early survival, probably on the basis of improving the adequacy of paraquat clearance. However, there was no obvious difference in the 28-day survival rate between the two groups.
The current therapies do not significantly improve the final outcome of patients with severe paraquat poisoning.8,9,18 Therefore, we performed a stratified analysis according to the oral dose. The the results suggested that the blood purification regimen in the goal-oriented group improved the 28-day survival rate of the patients with an oral dose of ≤50 ml, but not among those with an oral dose of >50 ml. HP only removes blood paraquat; it does not prevent the absorption process of paraquat by organs. Therefore, the paraquat that has already been absorbed by the organs is enough to cause organ failure, particularly for patients who have ingested a large dose of paraquat. Some researchers have even proposed the concept of a death threshold. 8,18 Likewise, the present study showed that for patients with an oral dose of >50 ml, the 28-day survival rate did not improve even when goal-oriented HP intensified the paraquat clearance.
Treatments for paraquat poisoning still need to be improved. Indeed, immunosuppressive treatment could improve patients’ outcomes 23 as well as control oxidative stress,24–26 inflammation, 25 and lung fibrosis. 27 Even if goal-oriented HP seems to be appropriate to remove paraquat from the blood, it must be combined with damage-control treatments. The most optimal regimens still need to be defined.
The present study is not without limitations. First, this was a single-center study with a small simple size and short follow-up time. Second, paraquat is quickly absorbed from the blood by tissues and organs.3,22 Clinical studies have shown that the best timing for HP is 2 to 4 h after poisoning. 2 In the present study, the time from poisoning to HP was >4 h for 52% of the patients because of factors such as transportation. Third, although the semi-quantitative detection of urine paraquat used in this study has many advantages, it still indirectly reflects the blood paraquat concentration. Therefore, the detection method requires improvement.
In conclusion, HP with monitoring of the urine paraquat concentration as goal-oriented therapy improved the adequacy of HP, particularly in terms of 7-day survival among all patients or 28-day survival among those with an oral dose of ≤50 ml.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was funded by the Special Fund for Clinical Medicine of the Department of Science and Technology of Jiangsu Province (China) (BL2014088).
