Abstract
Objective
Nocturnal hypoventilation (NH) is a complication of respiratory involvement in neuromuscular disorders (NMD) that can evolve into symptomatic daytime hypercapnia if not treated proactively with non-invasive ventilation. This study aimed to assess whether NH can be detected in the absence of other signs of nocturnal altered gas exchange.
Methods
We performed nocturnal transcutaneous coupled (tc) pCO2/SpO2 monitoring in 46 consecutive cases of paediatric-onset NMD with a restrictive respiratory defect (forced vital capacity < 60%). Nocturnal hypoventilation was defined as tcPCO2 > 50 mmHg for > 25% of recorded time, and hypoxemia as tcSpO2 < 88% for > 5 minutes. Daytime symptoms and bicarbonate were recorded after overnight monitoring.
Results
Twenty-nine of 46 consecutive patients showed NH. Twenty-three patients did not have nocturnal hypoxemia and 18 were clinically asymptomatic. In 20 patients, PaCO2 in daytime blood samples was normal. Finally, 13/29 patients with NH had isolated nocturnal hypercapnia without nocturnal hypoxia, clinical NH symptoms, or daytime hypercapnia.
Conclusions
Paediatric patients with NMD can develop NH in the absence of clinical symptoms or significant nocturnal desaturation. Therefore, monitoring of NH should be included among nocturnal respiratory assessments of these patients as an additional tool to determine when to commence non-invasive ventilation.
Keywords
Introduction
Neuromuscular weakness often leads to a chronic restrictive respiratory deficiency. This deficiency is characterized by a reduction in vital capacity (VC), total lung capacity, and functional residual capacity with a variable course among different disorders. 1 , 2 The first manifestation of chronic respiratory insufficiency in neuromuscular disorders (NMD) is nocturnal hypoventilation (NH) occurring in rapid eye movement sleep. Various definitions of NH have been proposed, but which definition best relates to prognosis remains unclear.3,4 In patients with NMD, a correlation between a reduction in VC and progression of sleep-disordered breathing has been shown. 5 Because clinical symptoms of NH can be insidious and not always present, daytime clinical assessments can be unreliable in early detection of respiratory failure. 6 Early recognition of NH is crucial because, if undiagnosed and thus untreated by non-invasive ventilation (NIV), NH can progress to daytime hypercapnia (partial carbon dioxide pressure [PaCO2] > 45 mmHg in blood gases1–3) or clinical symptoms related to hypoventilation.1,3,7 Prompt use of NIV is effective in reducing nocturnal hypoventilation and its progression towards daytime hypercapnia.8,9 Despite published guidelines, there is still debate regarding the correct timing to start NIV10–12. Few studies have specifically evaluated whether nocturnal hypercapnia is present in clinically asymptomatic patients with NMD.13–15 If this is the case, this finding could further expand the indications for NIV support.
The main aim of this study was to assess whether the current indicators of impairment of gas exchange, namely nocturnal hypoxemia, daytime PaCO2, and clinical symptoms, may underestimate the presence of NH in paediatric-onset NMD.
Patients and methods
We performed a retrospective study of 46 consecutive inpatients with NMD who were referred to the Neuromuscular Unit at G. Gaslini Pediatric Institute, Genova over a 6-year period from 2009 to 2014. All of the patients had genetically confirmed paediatric-onset NMD and a concomitant restrictive respiratory deficiency, defined as a forced vital capacity (FVC) below 60% of the predicted value. As per British Thoracic Society guidelines, 1 this threshold is considered an indicator to commence nocturnal respiratory assessment in NMD. Patients with acute upper or lower airway infections were excluded. Nocturnal evaluation was performed during the evening of the scheduled hospital admission.
The study protocol was approved by Giannina Gaslini Institute Ethics Committee in accordance with Italian legislation and according to the principles of the Helsinki Declaration. No patients’ consent was required because of the retrospective nature of the study.
For each patient, we collected clinical information regarding NMD diagnosis, age, FVC, presence of scoliosis, and clinical symptoms of NH. We specifically asked about the presence of headache, nausea, sleep quality, and daytime sleepiness.
FVC was measured using a standard spirometer (Micro Loop; MicroMedical, Rochester Kent) and analysed using Spida5 software V 1.61 (MicroMedical). Lung function tests were performed according to The American Thoracic Society and the European Respiratory Society guidelines, in an upright position. 16 Nocturnal PCO2 and SpO2 values were recorded using the SenTec Digital Monitoring System (SenTec AG, Therwil, Switzerland), which is able to continuously measure transcutaneous coupled PCO2 (tcPCO2) and SpO2 (tcSpO2) from a single probe. Calibration of the transcutaneous monitoring equipment was performed on the evening before application of the SenTec sensor. Patients with missing or unreliable data were not included in the study.
NH was defined as tcPCO2 > 50 mmHg for > 25% of the total sleep time according to the American Academy of Sleep Medicine guidelines. 17 According to the American College of Chest Physicians definition, significant hypoxia was defined as tcSpO2 < 88% for > 5 consecutives minutes of recording time. 18 Mean overnight tcPCO2 and tcSpO2 were also calculated from the Sentec transcutaneous monitor using the drift corrected value. The morning after the overnight sleep study, PaCO2 and bicarbonate values from capillary arterial blood gases were recorded. Daytime hypercapnia was defined as PaCO2 > 45 mmHg.1–3
Patients with and without NH were compared in terms of age, lung function (FVC), mean nocturnal tcPCO2 and tcSpO2, presence of hypoxemia, levels of daytime bicarbonate, presence of daytime symptoms, and presence of daytime hypercapnia.
Finally, among patients who started NIV because of detection of impairment of gas exchange, a follow-up nocturnal study was performed after 6 months. Values of tcPCO2 and tcSpO2, daytime bicarbonate, and PaCO2, and the presence of daytime symptoms were collected and compared with pre-ventilation values.
Statistical analysis
Data were analysed by GraphPad Prism® software version 7.02 (La Jolla, CA, USA). Descriptive statistics were generated for each measure. For all of the reported variables, a test of normality was performed. Variables that were not normally distributed were reported as median with 25–75 percentiles. Comparisons of the clinical characteristics among each diagnostic group were made by either ANOVA or the Kruskall–Wallis test according to the distribution of data. Comparison of baseline values between patients with NH and non-NH patients was performed by either parametric or non-parametric tests for independent variables. Similarly, comparison between baseline and follow-up data among patients undergoing NIV was made by either parametric or non-parametric tests for dependent variables. Chi square test was used for comparison between categorical values.
Results
The total number of patients who attended our Unit within the study period was 58. Twelve patients were excluded either because of an ongoing acute exacerbation or because they were affected by a life-threatening underlying muscular condition.
Study population (n = 46; 33 male, 13 female) included 14 patients with Duchenne muscular dystrophy (DMD), 12 with spinal muscular atrophy type 2 (SMA 2), nine with congenital myopathy (CM), six with Becker muscular dystrophy (BMD), and five with congenital muscular dystrophy (CMD). Median age at nocturnal evaluation was 14.9 years (11.9–17.1 years). Age at baseline was significantly different according to NMD diagnosis (p = 0.008); patients with SMA 2 were the youngest and those with BMD were the oldest (Table 1). In 17 of the 46 patients (7 DMD, 7 SMA 2, 2 BMD, 1 CMD) nocturnal gas exchange measures were within the normal range. Additionally, these patients also had normal daytime PaCO2 and bicarbonate levels.
Clinical features of the study population (n = 46)

DMD = Duchenne muscular dystrophy, SMA 2 = spinal muscular atrophy type 2, BMD = Becker muscular dystrophy, CM = congenital myopathy, and CMD = congenital muscular dystrophy.
In the remaining 29 patients (9 CM, 7 DMD, 5 SMA 2, 4 CMD, 4 BMD) some degree of altered nocturnal gas exchange was present, and these individuals were categorized as nocturnal hypoventilators. Within this group, six patients showed NH with hypoxaemia, while nine had daytime hypercapnia and high bicarbonate levels. Eleven patients complained of clinical symptoms of NH as morning headaches (n = 5), daytime sleepiness (n = 3), and frequent arousals (n = 3). Finally, 13 out of the 29 patients showed isolated nocturnal hypercapnia (Figure 1).

Flow diagram outlining sleep study results according to detection of nocturnal hypoventilation, the presence of significant hypoxemia, daytime hypercapnia, and daytime symptoms
Mean age was similar in patients with NH and non-NH patients (p = 0.55). However, mean baseline FVC (p = 0.007) and tcSpO2 (p = 0.02) were significantly lower in patients with NH than in non-NH patients. Conversely, mean tcPCO2 (p = 0.0001) and daytime bicarbonate (p = 0.01) were significantly higher in patients with NH than in non-NH patients. As reported above, while no patient had daytime hypercapnia among non-NH patients, nine patients with NH had daytime hypercapnia (Table 2).
Comparison between baseline demographic and nocturnal results between patients with NH and non-NH patients

NH = nocturnal hypoventilation, DMD = Duchenne muscular dystrophy, SMA 2 = spinal muscular atrophy type 2, BMD = Becker muscular dystrophy, CM = congenital myopathy, and CMD = congenital muscular dystrophy, FVC = forced vital capacity, tc = transcutaneous coupled.
All of the 29 patients with indications for NIV based on daytime hypercapnia or NH started therapy and were re-evaluated after 6 months. In 24 patients, a Pressure Support mode was used, while five were placed on an Assist Controlled Pressure Mode because of either younger age or a more severe muscle involvement. Twenty-four patients used a nasal interface (of these, four nasal pillows were used), while five used a full-face mask.
At 6-months follow-up, there was an overall significant improvement in nocturnal gas exchange (tcPCO2, p < 0.0001; tcSpO2, p = 0.009) and in daytime PaCO2 and bicarbonate levels (p = 0.03 and p = 0.01, respectively). Eleven patients who previously complained of NH symptoms reported complete resolution of symptoms (Table 3).
Comparison of gas exchange (tcPCO2 and tcSpO2), daytime clinical symptoms, daytime bicarbonate levels, and PaCO2 values in patients with NH at baseline and after 6 months of NIV treatment.
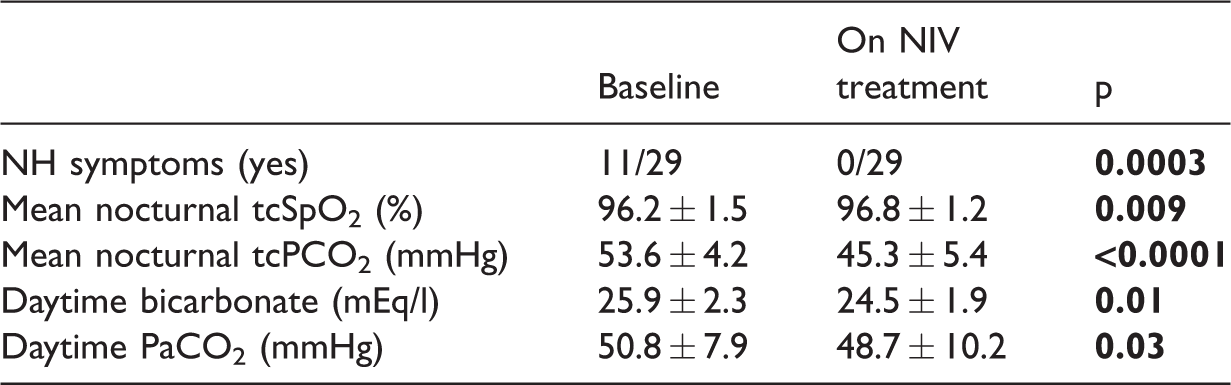
NH = nocturnal hypoventilation, NIV = non-invasive ventilation.
Patients with congenital myopathies had the lowest baseline tcSpO2. In this group, non-invasive ventilation was effective for nocturnal tcSpO2 (p = 0.008) and tcPCO2 (p = 0.008). Conversely, patients with DMD only showed improvement in tcPCO2 (p = 0.03) after the start of NIV treatment. Table 4 shows the baseline differences in age and nocturnal gas exchange according to diagnostic category.
Differences in respiratory involvement according to neuromuscular disease in patients with NH (n = 29)
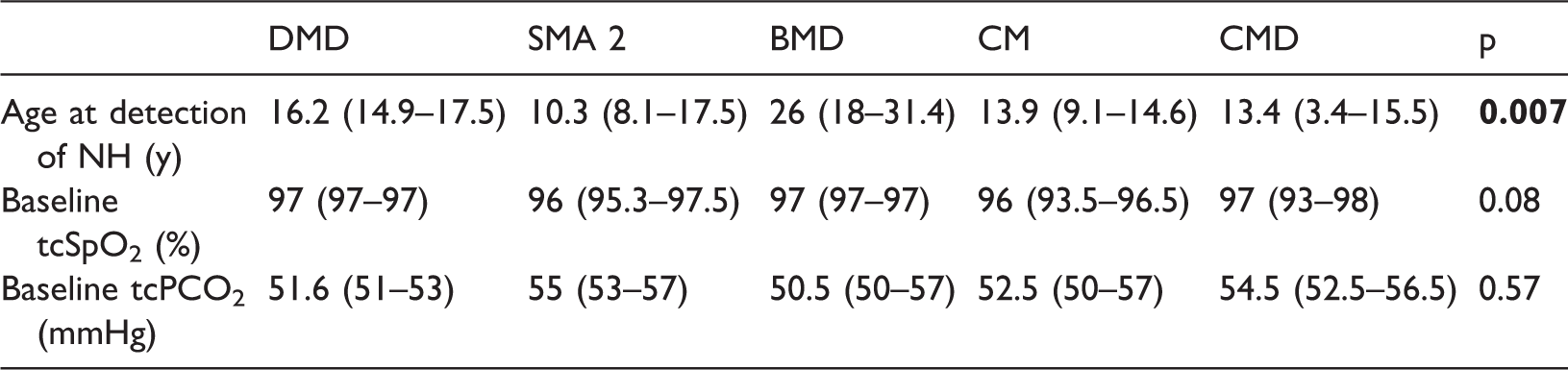
NH = nocturnal hypoventilation, DMD = Duchenne muscular dystrophy, SMA 2 = spinal muscular atrophy type 2, BMD = Becker muscular dystrophy, CM = congenital myopathy, and CMD = congenital muscular dystrophy.
Discussion
The diagnosis of nocturnal hypoventilation is not simple in neuromuscular diseases, and to date, many different definitions have been suggested.3,14 In this study, we used the definition proposed by the American Academy of Sleep Medicine, which defines hypoventilation as pCO2 > 50 mmHg for > 25% of sleep time17,18 because it is specifically tailored for the paediatric population. Using this threshold, we found that transcutaneous monitoring of pCO2 levels could potentially detect nocturnal hypoventilation, even in asymptomatic patients and those without significant nocturnal hypoxaemia. Twenty-three of 29 patients with NH did not have nocturnal hypoxemia, and 18 were clinically asymptomatic. Furthermore, in 20 of 29 patients with NH, PaCO2 in daytime blood samples was normal. Therefore, 13 of 29 patients had isolated nocturnal hypercapnia that was not associated with significant nocturnal hypoxia, daytime hypercapnia, or clinical NH symptoms. Notably, in our population, four patients with BMD had atypically severe muscular involvement with early onset. 19
These results highlight the importance of taking into account the presence of nocturnal hypercapnia when deciding whether non-invasive support is required. Our study suggests that pulse oximetry alone is insufficient for detecting nocturnal hypoventilation in children with NMD without obstructive sleep apnoea. The current guidelines recommend that NIV should be started in the presence of daytime hypercapnia and/or clinical symptoms.20,21 Nevertheless, we showed that both of these factors may not be sensitive enough in the diagnosis of NH in NMD. Therefore, nocturnal transcutaneous monitoring of pCO2/SpO2 may help in the early detection of nocturnal hypoventilation in young NMD patients, even before the onset of ventilatory deficiency and clinical symptoms. Nevertheless, we are aware that establishment of NIV support in the absence of either clinical symptoms or impairment of daytime gas exchange could have some disadvantages, such as a lack of adherence. In our population, we did not experience such a problem. However, notably, NIV support was started at low pressures. We did not specifically collect objective data on NIV adherence post-establishment. However, we did not notice any differences in terms of subjective tolerance between the NH group and the remainder of the patients. Moreover, Raphael et al. 22 reported that patients who started NIV before the onset of daytime symptoms had a worse outcome compared with the control group. Despite this isolated report, there have since been several studies demonstrating how NIV support prolongs survival in NMD. 23 However, in our study, we were not able to relate early detection of NH and commencement of NIV with clinically relevant outcomes because of the absence of a control group. Our study also confirmed previous findings that nocturnal tcSpO2/tcPCO2 monitoring helped manage and setup NIV support in home-ventilated patients.24,25
To the best of our knowledge, our study population is the youngest population of NMD patients in whom transcutaneous CO2 data have been reported. A previous report suggested that nocturnal transcutaneous assessment of pCO2 was more reliable than CO2 measured by morning arterial blood gases. 13 In contrast, Georges et al. 15 reported similar findings to our current data but their study group included a much wider population of respiratory restrictive disorders, not only neuromuscular diseases. Finally, Ogna et al. 14 demonstrated the usefulness of tcPCO2/SpO2 monitoring among the NH diagnostic tools, and the need to better define the threshold for NH itself. However, none of these studies specifically addressed the question of whether nocturnal monitoring can be used as an additional tool in the decision to start NIV in the clinical setting.
Our study has some limitations, such as the inclusion of a heterogeneous NMD population and the relatively small sample size. Furthermore, because of the retrospective nature of the study, data regarding muscle strength (maximum inspiratory pressure and maximum expiratory pressure), cough effectiveness (peak cough flow), and lung volume in the supine position were not available. Moreover, our study specifically focussed on nocturnal tcPCO2/SpO2 monitoring. We did not include the results of overnight cardiorespiratory polygraphic studies. The first reason for not including these studies is because we did not have complete data from cardiorespiratory studies in all of the patients. The second reason is because the main purpose of the study was not to compare tcPCO2/SpO2 monitoring with respiratory polygraphy in detecting NH among patients with NMD. Instead, we aimed to evaluate whether nocturnal hypercapnia is present in clinically asymptomatic NMD. Indeed, we found that nocturnal oximetry, the presence of daytime symptoms, and daytime hypercapnia could underestimate actual impairment of nocturnal gas exchange.
In conclusion, we report the results of nocturnal tcPCO2/tcSpO2 monitoring in the youngest population of patients with NMD studied to date. Our study shows that mean nocturnal SpO2 is not sufficient for early detection of NH in NMD. Furthermore, tcPCO2/SpO2 monitoring can help clinicians in the setup of titrating NIV. Nevertheless, prospective studies are required to clarify whether early initiation of NIV for asymptomatic NH has a beneficial effect on survival.
Footnotes
Authors’ contributions
Dr. Brisca and Mrs. Tacchetti contributed to collection of data and in drafting the manuscript. Drs. Fiorillo, Carlucci, Tan, Bruno, and Minetti contributed to reviewing the manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
Dr Trucco was supported by a grant from the Italian Ministry of Health, CCM Program 2013.
