Abstract
Objective
To evaluate the clinical features, risk factors, and prognostic significance of different Stanford types of acute aortic dissection (AAD).
Methods
We retrospectively analyzed the clinical data and prognostic predictors in 105 patients with AAD (37 with Stanford type A and 68 with Stanford type B) at Tianjin Medical University General Hospital and Tianjin 4th Central Hospital from January 2014 to November 2015.
Results
Patients with Marfan syndrome and bicuspid aortic valve constituted 24.3% and 8.1%, respectively, of patients with type A AAD; these proportions were significantly higher than those of patients with type B AAD (7.4% and 0.0%, respectively). The proportion of iatrogenic causes of type A AAD (8.1%) was significantly higher than that of type B AAD (0.0%). Computed tomography angiography showed that the proportion of involvement of the aortic arch and pericardial effusion (86.5% and 18.9%, respectively) in patients with type A AAD were higher than those in patients with type B AAD (23.5% and 5.9%, respectively). Endovascular treatment was performed in a higher proportion of patients with type B than A AAD (70.6% vs. 5.4%, respectively).
Conclusion
Systolic blood pressure, pericardial effusion, periaortic hematoma, conservative treatment, and open surgery were independent predictors of increased mortality in patients with AAD.
Introduction
Acute aortic dissection (AAD) is part of acute aortic syndrome and a life-threatening aortic catastrophe with high morbidity and mortality due to complications. Early diagnosis and management of AAD may improve the prognosis. The International Registry of Aortic Dissection (IRAD) investigators previously described the clinical profiles and outcomes of AAD; however, most patients in the IRAD are from developed countries with advanced medical care. The data from the IRAD do not reflect the current condition of Chinese patients with AAD. In the present study, we evaluated the epidemiological factors and outcomes of AAD in China and explored the prognostic risk factors.
Material and methods
This was a single-center, retrospective study of 105 patients presenting with AAD at Tianjin Medical University General Hospital and Tianjin 4th Central Hospital from January 2014 to November 2015. The diagnosis was determined from the history, physical examination findings, and imaging findings according to the 2014 European Society of Cardiology Guidelines on the diagnosis and treatment of aortic diseases. 1 The acute stage was defined as the initial 14 days after symptom onset. Patients with subacute aortic dissection (>14 days) and chronic aortic dissection (>60 days) were excluded. The patients were divided into two groups according to the Stanford classification system: those with AAD involving the ascending aorta (type A dissection group) and those with AAD not involving the ascending aorta (type B dissection group). 2 Of all patients, 37 were diagnosed with type A AAD and 68 with type B AAD. The mean age of the patients was 53.39 years (range, 31–87 years). The male:female ratio was approximately 2.38:1.00.
The clinical data included patient demographics, clinical symptoms and signs, imaging findings, treatment, outcomes, and prognostic risk factors.
Continuous variables are expressed as mean and standard deviation or median. Categorical variables are expressed as frequency and proportion. An unpaired t-test was used to compare continuous variables, while the χ2 test and Fisher’s exact test were used to compare categorical variables. Multivariate analysis of the potential risk factors for death was performed using a logistic regression model. The data analysis was performed using SPSS version 19.0 (IBM Corp., Armonk, NY). A
Results
Patients’ baseline characteristics.

Data are presented as mean ± standard deviation or n (%).
There was no difference in the interval between symptom onset and definitive diagnosis between patients with type A and B AAD. The incidence of chest pain in patients with type A AAD (91.9%) was higher than that in patients with type B AAD (75.0%) (
Clinical manifestations and imaging findings.

Data are presented as mean ± standard deviation or n (%).
ECG, electrocardiography
Treatment and imaging findings.

Data are presented as n (%).
Mortality.
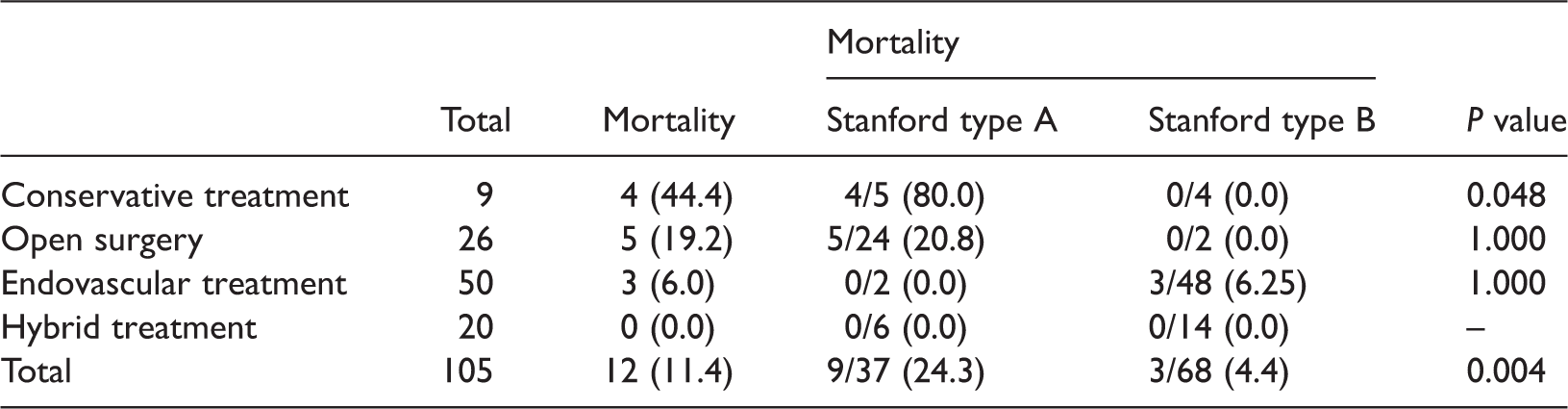
Data are presented as n (%).
Risk factors for death.
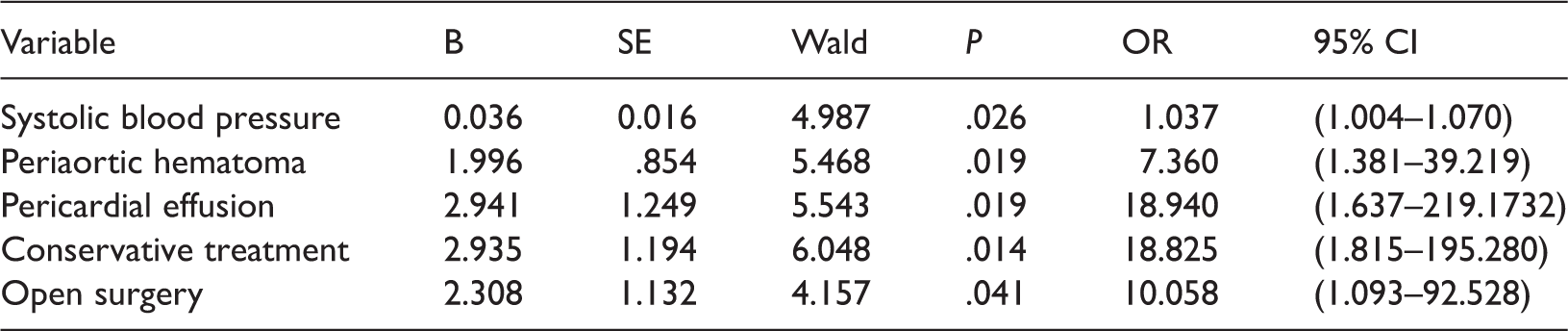
CI: confidence interval, OR: odds ratio, SE: standard error
Discussion
AAD is the most common fatal aortic catastrophe, and the malignant course of AAD is the main cause of cardiovascular morbidity and mortality. The estimated annual incidence of AAD in the United States ranges from 10 to 15 per 100,000 adults. 3 Population-based studies have estimated that the annual incidence of AAD is about 3 per 100,000 people. 4 Although no epidemiological data have been confirmed, the number of patients with AAD has increased in China in recent years.
The mean age of the patients with AAD in the present study was lower than that reported by the IRAD 5 because of the inadequate control of hypertension in China. Zhao et al. 6 found that the proportion of patients with hypertension whose blood pressure improved was only 6.1%, which is much lower than that reported by European countries and the United States. The male:female ratio in the present study (2.38:1.00) was higher than that reported by the IRAD (1.88:1.00). 7 This difference may have occurred because men in China have more risk factors, such as smoking, hypertension, and arteriosclerosis. In China, the smoking rate in men was higher than that reported by the IRAD (50% vs. 20%–39%, respectively). 8 The percentage of patients with AAD who had hypertension in the present study (67.8%) was higher than that described by the IRAD investigators. The reason for this difference might have been the high-salt diet in our geographical area. Our study revealed that in patients with AAD, the risk of death increased by about 3.7% when the systolic blood pressure increased by 1 mmHg.
Pain is a typical symptom of AAD and may include anterior chest pain, back pain, abdominal pain, and leg pain. Chest pain occurred more often in patients with type A AAD, while abdominal pain and leg pain occurred more often in those with type B AAD. The proportion of patients with no pain in our study was 4.76%, which is lower than that reported by Imamura et al. 9 In another study, the mortality rate was higher in patients without than with pain because of the more severe symptoms in nonpainful patients (e.g., syncope, heart failure, and shock). 10
According to the imaging findings in the present study, involvement of the aortic arch and pericardial effusion was more frequent in patients with type A than B AAD. There was no significant difference in the development of pleural effusion, periaortic hematoma, or false lumen thrombosis between patients with type A and B AAD. The risk of death in patients with AAD who had a periaortic hematoma was 7.4 times higher than that of patients without a periaortic hematoma. The risk of death in patients with AAD who had pericardial effusion was 18.9 times higher than that of patients without pericardial effusion. These two imaging findings were more likely to predict AAD rupture.
The initial management of AAD is performed in the emergency room. The systolic blood pressure must be lowered and the heart rate must be decreased to decrease the shear force on the vessel wall. 11 Beta-blockers are the first-line drugs to lower the heart rate, and angiotensin-converting enzyme inhibitors are recommend to lower the blood pressure because these drugs decrease the possibility of AAD rupture and cerebral apoplexy. 12 In the present study, the proportion of patients who underwent open surgery was much higher among those with type A AAD (64.9%) than type B AAD (2.9%), while the proportion of patients who underwent endovascular surgery was much lower among those with type A AAD (5.4%) than type B AAD (70.6%). The reasons for performing conservative treatment in five patients with AAD included older age (n = 2), the presence of significant comorbid conditions (n = 2), and the patient’s refusal of invasive treatment (n = 1). Endovascular treatment (fenestrated thoracic endovascular aortic repair) was performed in two patients with type A AAD in whom thoracotomy was impossible due to relevant comorbidities. Among the 48 patients with type B AAD, the indications for endovascular treatment included intractable pain in 17, uncontrolled hypertension in 11, presentation with paraplegia in 2, and malperfusion syndrome in 18. Open surgery might be applicable to type A AAD, while endovascular surgery may be more applicable to type B AAD.
The mortality of patients with type A AAD who underwent conservative management was much higher than that of patients with type B AAD. Therefore, we recommend that clinicians first consider active open surgery or endovascular treatment for patients with type A AAD. There was no significant difference in mortality between patients who underwent open surgery and endovascular treatment. Additionally, no death occurred among all patients who underwent hybrid procedures. Hybrid surgeries were commonly performed in patients with complicated arch dissection or a short landing zone for thoracic endovascular aortic repair. Hybrid treatment decreased the risk of open surgery to replace the diseased aorta.
We identified systolic blood pressure as an independent predictor of increased in-hospital mortality. Thus, better control of blood pressure might be associated with a decrease in relevant complications and mortality in patients with AAD. Imaging findings of a periaortic hematoma and pericardial effusion were both predictors of increased mortality, which might indicate a high risk of impending aortic rupture. These high-risk factors should be considered when making treatment decisions for patients with AAD.
Although our data provide an outline of AAD in China, the retrospective, observational design of our study has some limitations. Some variables were missing, and some parameters were unavailable in the reviewed charts. The small sample size was another limitation of this study. Multicenter, prospective, large-scale studies are therefore needed to fully elucidate the clinical situation of AAD in China.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
