Abstract
Objectives
To assess the relationship between sleep quality, daytime sleepiness and health-related quality-of-life (HRQoL) in Chinese patients undergoing maintenance haemodialysis (MHD).
Methods
This cross-sectional study enrolled patients undergoing MHD. Self-reported sleep quality (Pittsburgh Sleep Quality Index [PSQI]), daytime sleepiness (Epworth Sleepiness Scale [ESS]) and HRQoL (36-item Short Form [SF-36]) were recorded for all patients.
Results
Sixty eight patients (mean ± SD age = 61.75 ± 16.56 years; 43 male/25 female) who regularly received MHD were included. The prevalence of poor sleepers was 69.1% (47/68) and daytime sleepiness was 11.8% (eight of 68). Poor sleepers had a significantly lower Physical Component Scale (PCS) score, Mental Component Scale (MCS) score and total SF-36 score than good sleepers. The PSQI score correlated inversely with both the PCS and MCS scores and correlated positively with age. Independent variables associated with total SF-36 score were duration of MHD, ESS score and PSQI score.
Conclusions
Poor sleep quality is a common and severe issue for MHD patients in east China. Both sleep quality and daytime sleepiness were associated with lower HRQoL scores.
Introduction
Sleep disorders are common in patients with end stage renal disease (ESRD) who undergo long-term maintenance haemodialysis (MHD). 1 Studies have found that 50–80% of patients undergoing conventional MHD report some sleep complaints or excessive daytime sleepiness.2,3 Sleep complaints (which characteristically include insomnia,4,5 difficulty in initiating sleep, early morning awakenings and feeling unrefreshed in the morning), are particularly common in patients undergoing MHD. Poor sleep quality in patients undergoing MHD is associated with male sex, high phosphate level, caffeine intake, advanced age, depression, cardiovascular disease, MHD duration, poor-quality MHD and poor health-related quality-of-life (HRQoL).3,5–8 Excessive daytime sleepiness is defined as the inability to stay awake or alert during the major waking episodes of the day, resulting in unintended lapses into drowsiness or sleep. 9 The consequences of daytime sleepiness can range from decreased productivity at work to an increased risk of motor vehicle accidents. Many studies have addressed the relationship between sleep quality, daytime sleepiness and HRQoL in patients with ESRD.2,7,10 However, previous studies have not confirmed any association between these issues and MHD in particular, therefore, the aim of the present study was to investigate this relationship in Chinese patients undergoing MHD.
Patients and methods
Patients
This cross-sectional study enrolled consecutive patients aged >18 years who received MHD in the Blood Purification Centre of the Department of Nephrology, Zhejiang Provincial People’s Hospital, Hangzhou, Zhejiang Province, China, for >3 months between March 2013 and June 2013. Patients with known obstructive sleep apnoea, psychiatric illness, severe cognitive impairment, inability to answer the questionnaires, in-hospital admission within 4 weeks of the study and those unwilling to participate were excluded.
Patients received MHD two or three times per week (duration, 4.5 h if given twice per week and 4 h if given three times weekly). Patients were dialysed with a standard bicarbonate-containing dialysate bath, using a synthetic membrane (Polyflux®, Polyflux® 14 L; Gambro Dialysatoren, Hechingen, Germany). Dialysate flow rates were set at 500 ml/min; blood flow rates were kept between 200 and 300 ml/min.
The study protocol was approved by the Medical Ethics Committee of Zhejiang Provincial People’s Hospital (no. KY2012001). All of the study participants provided written informed consent before enrolling in this study.
Sleep quality, daytime sleepiness and HRQoL measurement
After each patient received a brief explanation of the study instruments used, sleep quality was measured using the Pittsburgh Sleep Quality Index (PSQI), daytime sleepiness was measured using the Epworth Sleepiness Scale (ESS) and HRQoL was measured using the Medical Outcomes Study 36-item Short Form (SF-36) during regularly scheduled MHD treatments.11–13 Assistance was available for illiterate patients.
The PSQI is a standardized tool used for assessing sleep quality; 11 it consists of 19 self-rated questions and five questions rated by the bed partner or roommate. This scale has seven components, each dealing with a major aspect of sleep: (a) subjective quality of sleep; (b) sleep onset latency; (c) sleep duration; (d) habitual sleep efficiency; (e) sleep disturbances; (f) use of hypnotic-sedative medication; (g)daytime disturbances. The tool has four items that are open-ended questions, and five items on a rating scale between 0 and 3 (0 represents no trouble in sleeping over the past week; 1 refers to presence of trouble once; 2 is presence of trouble twice; 3 is presence of trouble three times over the past week). A global PSQI score ≥ 5 indicates a ‘poor’ sleeper. Daytime sleepiness was assessed by the ESS, which is a validated questionnaire containing eight items that inquire about expectation of dozing in eight hypothetical situations. 12 Responses are provided on a scale between 0 and 3 (0 represents no chance of dozing; 1 represents slight chance of dozing; 2 represents moderate chance of dozing; 3 represents high chance of dozing). An ESS score ≥ 10 indicates excessive daytime sleepiness. HRQoL was measured with the SF-36, 13 which consists of 36 items assigned to eight dimensions: (a) physical functioning; (b) role physical; (c) bodily pain; (d) general health; (e) vitality; (f) social function; (g) role emotional; (h) mental health. Each dimension is scored with a range between 0 and 100, with higher scores indicating better functioning. While the first four items constitute the Physical Component Scale (PCS), the remaining four items constitute the Mental Component Scale (MCS). This scale has been validated and is commonly used in patients with ESRD.14,15
Patients’ sociodemographic and clinical characteristics including age, sex, MHD duration, marital status, living status (living alone or with a partner), education status (illiterate, elementary school, secondary school, high school, university graduate), employment, smoking status, MHD shift (morning or afternoon shift), vascular access, previous renal transplantation (present or absent), aetiology of renal disease, presence of diabetes mellitus, hypertension, coronary artery disease and cerebrovascular disease were recorded.
Other data collected
Laboratory parameters including pre-MHD haemoglobin, albumin, total cholesterol, triglyceride, high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), calcium, phosphorus, blood urea nitrogen, ferritin and intact parathyroid hormone (iPTH) levels were measured before the beginning of each MHD session. Post-MHD blood urea nitrogen (BUN) was also measured to calculate single-pool Kt/V (spKt/V) and urea reduction ratio (URR). The post-MHD sample was drawn from the arterial vascular access needle after the cessation of MHD. 16 All biochemical analyses were performed using an oxidase-based technique and were measured using an Olympus AU5400™ Chemistry-Immuno Analyser (Olympus America, Melville, NY, USA) in the Central Biochemistry Laboratory of Zhejiang Provincial People’s Hospital.
The MHD dose was evaluated using the following formula: spKt/V = −Ln(R − 0.008 × t) + (4 − [3.5 × R]) × UF/W where spKt/V is a single-pool Kt/V, R is the ratio of post- to pre-MHD BUN, t is time on MHD in h, UF is the amount of ultrafiltration in litres and W is post-MHD body weight in kg. 17 Calculation of URR used the formula URR = (preBUN– postBUN)/preBUN. 18
Statistical analyses
All statistical analyses were performed using the SPSS® statistical package, version 16.0 (SPSS Inc., Chicago, IL, USA) for Windows®. Data are presented as mean ± SD, unless otherwise specified. Student’s
Results
Sociodemographic and clinical characteristics of patients (

Data presented as mean ± SD or
HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; iPTH, intact parathyroid hormone; spKt/V, single-pool Kt/V, estimated from urea reduction rate; URR, urea reduction rate.
Mean and median PSQI scores were 8.2 ± 5.1 and 7.5 (range, 0–20), respectively. The prevalence of poor sleepers was 69.1% (47/68), and the prevalence of daytime sleepiness was 11.8% (eight of 68).
Sociodemographic and clinical characteristics of patients (
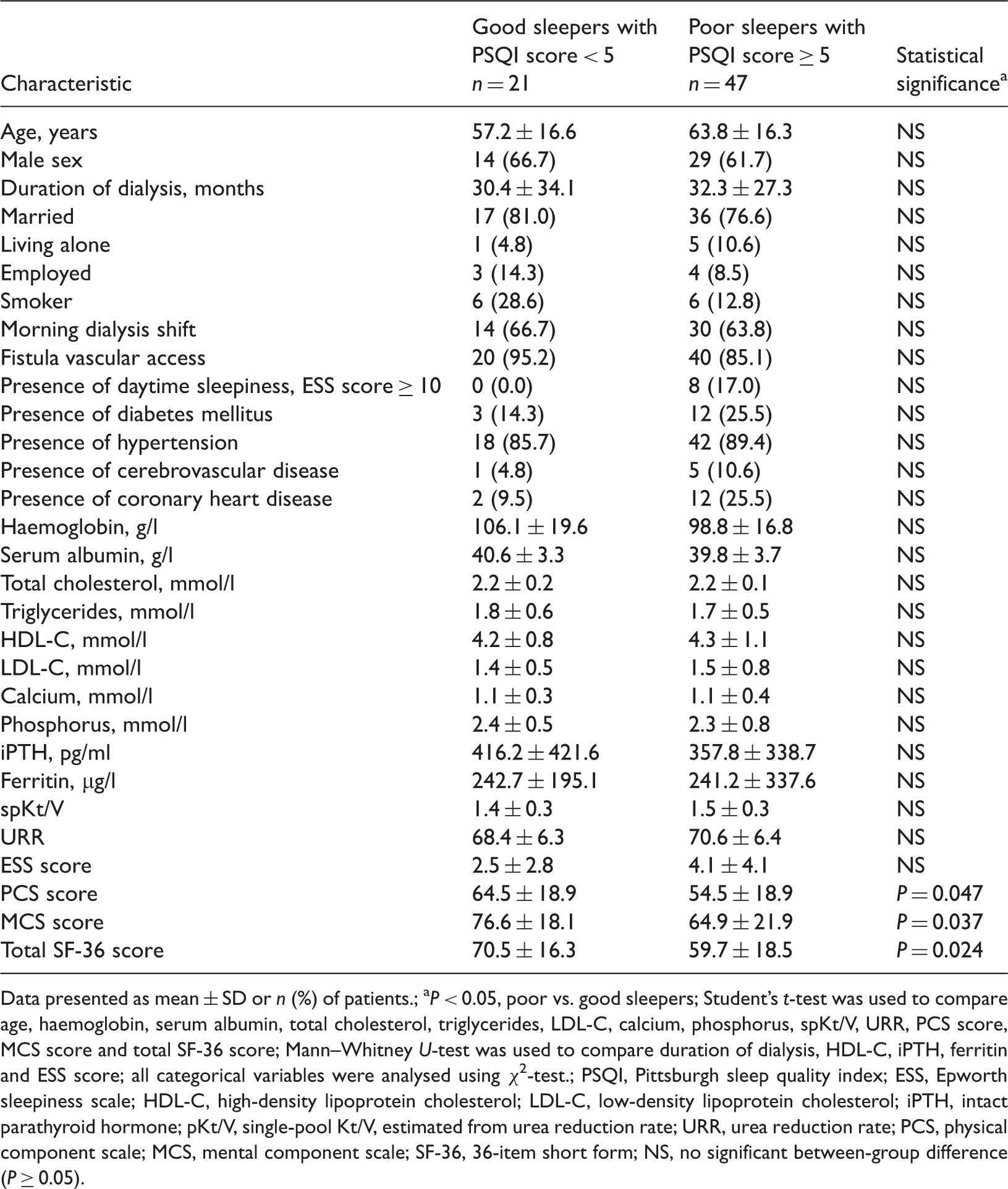
Data presented as mean ± SD or
PSQI, Pittsburgh sleep quality index; ESS, Epworth sleepiness scale; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; iPTH, intact parathyroid hormone; pKt/V, single-pool Kt/V, estimated from urea reduction rate; URR, urea reduction rate; PCS, physical component scale; MCS, mental component scale; SF-36, 36-item short form; NS, no significant between-group difference (
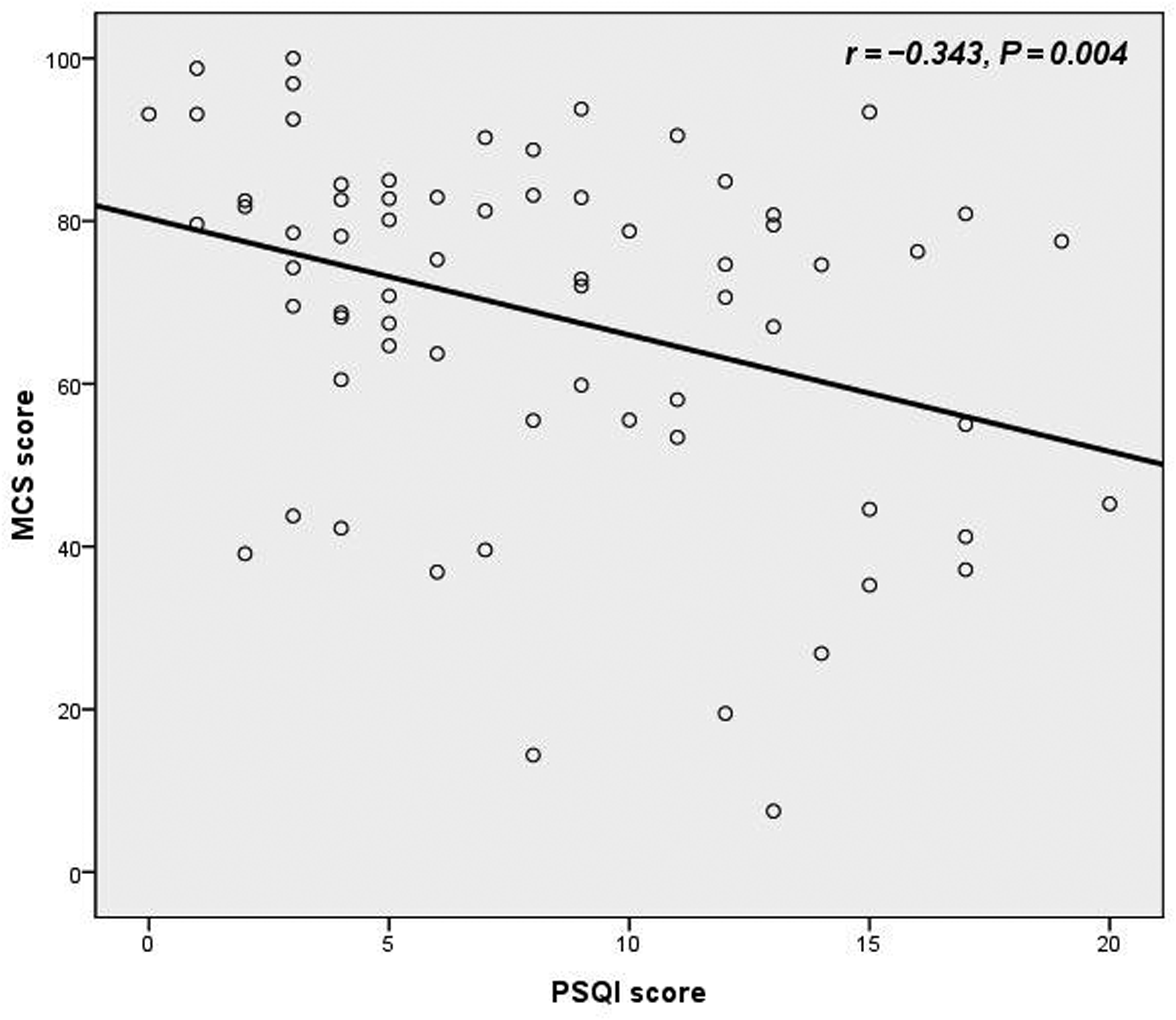
Correlations between the PSQI and other continuous variables were studied. There was a significant inverse correlation between PSQI and PCS score ( Correlation between physical component scale (PCS) score and Pittsburgh sleep quality index (PSQI) score in patients ( Correlation between mental component scale (MCS) score and Pittsburgh sleep quality index (PSQI) score in patients ( Correlation between age and Pittsburgh sleep quality index (PSQI) score in patients ( Multiple linear regression models for the association between independent sociodemographic and clinical characteristics and the total 36-item short form score in patients ( ESS, Epworth sleepiness scale; PSQI, Pittsburgh sleep quality index.


Discussion
There were four main findings in this present study. First, the prevalence rates for poor sleepers (those with a PSQI score ≥ 5) and daytime sleepers (those having an ESS score ≥ 10) were 69.1% and 11.8%, respectively, in Chinese patients undergoing MHD. Secondly, poor sleepers had significantly lower PCS, MCS and total SF-36 scores than good sleepers. Thirdly, there was a significant inverse relationship between the PSQI score and the PCS and MCS scores, but there was no correlation between the PSQI and ESS scores. Fourthly, in the multivariate analysis, the independent characteristics associated with the total SF-36 score were PSQI score, ESS score and MHD duration.
To the best of our knowledge, this is the first study to evaluate the relationship between sleep quality, daytime sleepiness and HRQoL in patients undergoing MHD in east China. The prevalence of poor sleep quality in patients undergoing MHD (69.1%) was consistent with the range previously reported (41–83%).2,19,20 However, the prevalence of poor sleep quality in the general population ranges between 7 and 40%,21–26 which demonstrates that the prevalence of poor sleep quality is higher in the MHD patient population than in the general population.
Studies have shown that sleep quality was associated with HRQoL in ESRD patients, and that MHD patients with good sleep quality were more likely to have higher MCS and PCS scores than those with poor sleep quality.6,27,28 In the present study, good sleepers had higher PCS, MCS and total SF-36 scores (i.e., better HRQoL) than poor sleepers, and there was a significant inverse correlation between the PSQI score and both the MCS and PCS scores. Multivariate analysis identified the PSQI score as an independent variable of the total SF-36 score in the present study. Ohayon et al. 29 concluded that age associations with a variety of sleep parameters and sleep quality were significantly decreased with age in healthy adults. In the present study, there was a significant positive correlation between PSQI score and age, which indicates that sleep quality was also associated with age in MHD patients.
A previous study demonstrated that among MHD patients, poor sleepers had lower haemoglobin levels compared with good sleepers. 2 In contrast, other research showed that haemoglobin levels do not play a critical role in determining sleep disorders. 5 Blood urea nitrogen, which is considered a pivotal uraemic toxin, has been associated with sleep disorders. 30 Conversion of conventional MHD patients to nocturnal MHD resulted in a significant reduction in BUN, which improved sleep apnoea and sleep quality. 30 However, kidney function could not be demonstrated as an independent variable associated with PSQI. 31 High levels of iPTH, which is a middle molecule uraemic toxin, are at major risk factor for insomnia. 5 Along the same lines, insomnia in patients with severe hyperparathyroidism on MHD was ameliorated by parathyroidectomy. 32 The present study showed that there was no relationship between sleep quality, haemoglobin levels and clearance of small molecule or middle molecule uraemic toxins, as measured by spKt/V, URR and iPTH. Thus, even after accounting for known and hypothesized predictors of poor sleep quality in patients undergoing MHD, the variation in self-assessed sleep quality remained largely unexplained in the present study.
Daytime sleepiness is very common in MHD patients and may be very serious, although without obvious clinical risk factors for the condition. Studies of MHD patients found that 13–33% of patients report excessive daytime sleepiness.33,34 This present study found that 11.8% of MHD patients had ESS scores ≥10. The ESS has been widely used in both clinical and research environments as a cost-effective measure to assess subjective daytime sleepiness and has, at times, been used as a substitute for the Multiple Sleep Latency Test.14,35–40 The current study probably underestimated the prevalence of daytime sleepiness because ESS scores may be altered by the presence of other symptoms, such as fatigue, tiredness, lack of energy
41
or common mental disorders:
42
these variables were not measured in the present study but are commonly described by MHD patients. Other renal disease- or MHD-related factors not measured in this present study may also contribute to daytime sleepiness in MHD patients. For example, subclinical uraemic encephalopathy may increase susceptibility to sleepiness because this condition has an increased association with slow-wave activity in the waking EEG43–46 and declined signal processing, shown by increased visual evoked potentials and brainstem auditory evoked potential latencies in response to external stimuli.47,48 The associations among sleep quality and daytime sleepiness associated in MHD patients have been inconsistent. For example, one study reported that sleep quality had a strong correlation with daytime sleepiness (
The current study had a number of limitations. First, because this was a cross-sectional analysis rather than a prospective controlled study, no cause-and-effect relationships can be drawn from the findings. Secondly, because of the small sample size, the study had limited power to explore potential mediators of the association between sleep disorders and clinical characteristics. Thirdly, assessments were performed only once and not on the basis of a time series. Finally, although assistance was available for MHD patients who were illiterate, these current results should be interpreted with caution because these patients might have had problems interpreting the questions.
This study demonstrated that poor sleep quality is both a common and severe issue in a population of MHD patients in east China. Poor sleepers were more likely to be affected by daytime sleepiness, although the difference between the two groups was not statistically significant. There was no relationship between sleep quality and daytime sleepiness. Sleep quality was associated with both the physical component scale and mental component scale of the HRQoL measure. These findings suggest that problems with sleep might be clinically significant for many MHD patients, and that an assessment of sleep quality and other factors (such as daytime sleepiness and HRQoL) should be undertaken as part of the management of MHD patients.
Footnotes
Acknowledgements
We would like to thank all patients and their families for participating in this study.
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This study was supported by grants from the National Natural Science Foundation of China (No. 81170691), Project of Province and the Ministry (No. WKJ2013-2-002) and Zhejiang Medical Technology Project (No. 2016KYB017).
