Abstract
We report a unique case of Sjögren’s syndrome complicated with Fanconi syndrome and Hashimoto’s thyroiditis in a 53-year-old Chinese woman, initially found to have proteinuria, fatigue and multiple old costal fractures. Distal tubular dysfunction is the most common renal damage in Sjögren’s syndrome, while Fanconi syndrome (which is caused by proximal tubular dysfunction) and Hypothyroidism are rare complications of Sjögren’s syndrome.
Introduction
Sjögren’s syndrome is a chronic inflammatory autoimmune disease, characterized by lymphocytic infiltration of exocrine glands, which is often underdiagnosed but affects between 1 and 3% of the general population. 1 The ratio of female to male patients with Sjögren’s syndrome is about 9:1, 2 with peak incidence occurring in people between the ages of 50 and 80 years. Besides the most common involvement of salivary and lacrimal glands, Sjögren’s syndrome can affect the skin, lungs, gastrointestinal tract, central and peripheral nervous systems, and the musculoskeletal apparatus. The incidence of osteomalacia in Sjögren’s syndrome patients with renal tubular acidosis ranges between 25 and 45%. 3 We report a unique case of Sjögren’s syndrome complicated with Fanconi syndrome, Hashimoto’s thyroiditis and multiple old costal fractures in a 53-year-old Chinese woman.
Case report
A 53-year-old female was admitted to Sir Run Run Shaw Hospital (Hangzhou, China) in March 2014, because of proteinuria and glycosuria, which she had for ∼3 years and which had not been diagnosed in other hospitals. She also complained of dryness of her mouth and eyes, and had pain in her bilateral hypochondrium that later spread to her shoulders, elbows, knees and proximal metatarsophalangeal and metacarpophalangeal joints, and was reported to worsen in winter. The red rash on her face also worsened in winter.
Standard laboratory and clinical workup showed glycosuria (++++), proteinuria (+), hypothyroidism, substernal goitre, multiple old costal fractures and slightly dysfunctional salivary glands; 24-h urine protein quantitation was 2430.4 mg. The anion gap was normal, serum pH was 7.34 and urinary pH was 5.5. Serum bicarbonate was 18.7 mmol/l, serum potassium was 3.07 mmol/l, serum calcium was 2.17 mmol/l and alkaline phosphatase was 74 U/l. Total thyroxine was decreased to 49.6 nmol/l, free thyroxine was decreased to 6.89 nmol/l, high sensitivity thyrotropin was increased to 5.51 nmol/l, thyroglobulin was decreased to 1.21 µg/l, antithyroglobulin antibody was increased to 774.60 IU/ml and antithyroperoxidase antibody was increased to 94.61 IU/ml. Computed tomography (CT) scanning revealed substernal goitre and multiple old costal fractures (Figure 1). A labial salivary gland biopsy (Figure 2) showed a focal lymph follicle in the sampled tissue. A kidney biopsy (Figure 3) was also performed. Periodic acid-Schiff and periodic acid-silver methenamine staining showed lymphocytic infiltration. Further examination of the kidneys showed one glomerulus out of 14 had become sclerotic, and slight mesangial proliferation of the glomeruli. There was calcified sediment and protein inside the tubule, which were red with Masson staining.
Computed tomography scan illustrating multiple old rib fractures (arrows) in a 53-year-old Chinese woman presenting with Sjögren’s syndrome complicated with Fanconi syndrome and Hashimoto’s thyroiditis. Focal lymph follicle infiltration (star) revealed in a labial salivary gland biopsy (haematoxylin and eosin stain, 400 × magnification) in a sample taken from a 53-year-old Chinese woman presenting with Sjögren’s syndrome complicated with Fanconi syndrome and Hashimoto’s thyroiditis. The colour version of this figure is available at: http://imr.sagepub.com Lymphocytic infiltration (star; 400 × magnification), in a kidney biopsy sample stained with periodic acid-Schiff (PAS) and periodic acid-silver methenamine (PASM), taken from a 53-year-old Chinese woman presenting with Sjögren’s syndrome complicated with Fanconi syndrome and Hashimoto’s thyroiditis. The colour version of this figure is available at: http://imr.sagepub.com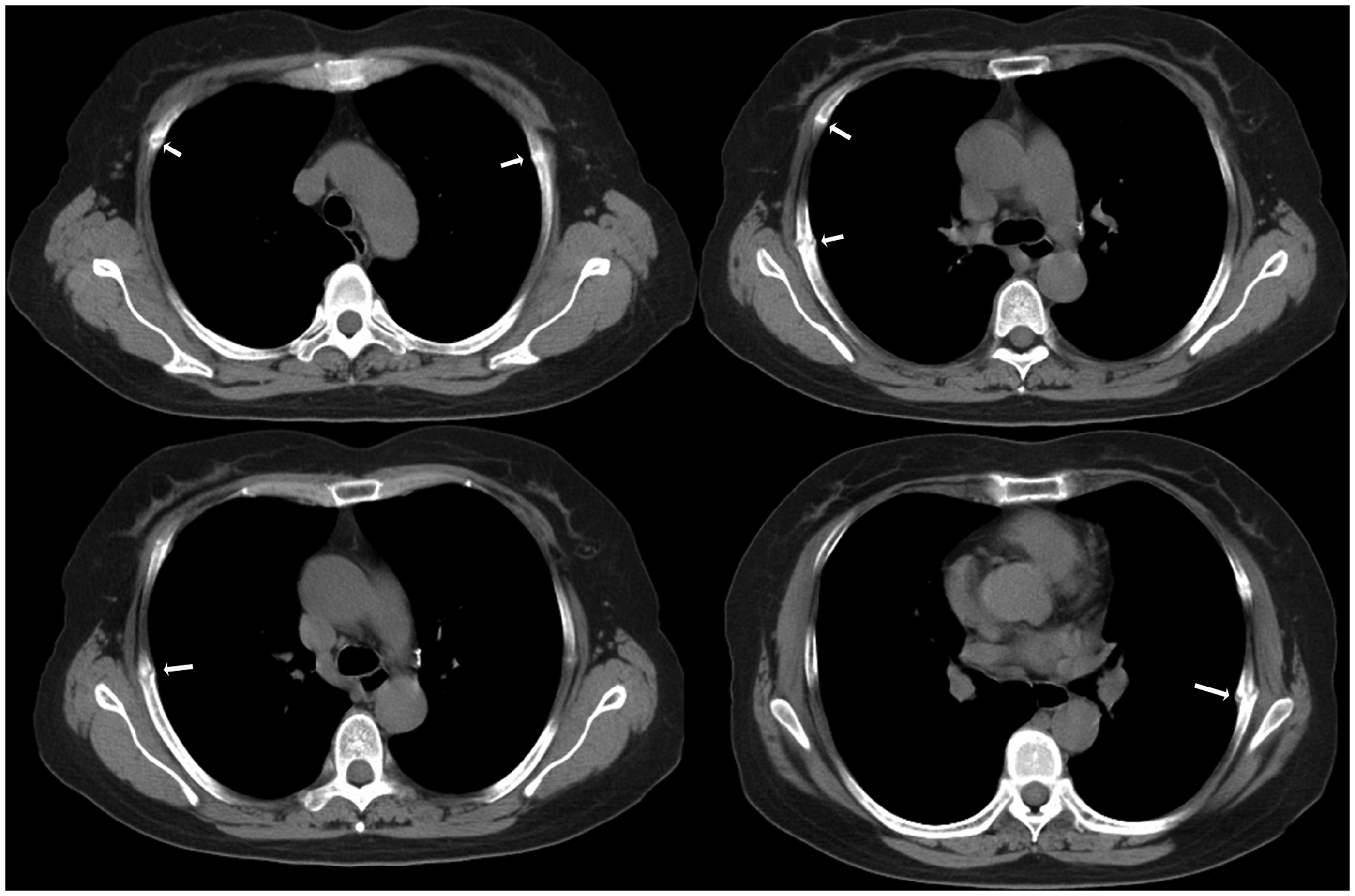


Sjögren’s syndrome was diagnosed based on the patient’s complaint of dry eyes and dry mouth, positive Schirmer and Saxon tests, and the labial salivary gland biopsy result. Fanconi syndrome was confirmed by metabolic acidosis with hypokalaemia, hyperchloraemia and alkalinuria, indicating proximal renal tubular acidosis. Hypothyroidism was confirmed by thyromegaly (grade 2), decreased thyroxine (T4) and thyroglobulin, and elevated thyroid stimulating hormone. Since thyroglobulin antibodies and thyroid autoantibodies were significantly increased, we also considered the presence of an autoimmune thyroiditis, such as Hashimoto’s thyroiditis. After standard treatment with methylprednisolone, potassium citrate, levothyroxine sodium and symptomatic therapy, the patient gained a normal serum pH, and normal levels of bicarbonate, potassium and thyroid hormones.
The patient reported here provided written informed consent for publication of her medical details and any accompanying images. The Sir Run Run Shaw Hospital, School of Medicine, Zhejiang University, China, does not require ethical approval for reporting individual cases.
Discussion
To date and to our knowledge, there has been no previous report in the literature of a patient with concurrent Sjögren’s syndrome, Fanconi syndrome and Hashimoto’s thyroiditis. Reviewing the literature, we found that the complications mentioned in the introduction of this paper are common in worldwide reports of patients with concomitant Sjögren’s syndrome and Fanconi syndrome.
Case reports of Sjogren’s syndrome (SS) complicated with Fanconi syndrome (FS).

RTA, renal tubular acidosis.
The reported cases, along with our case, are predominantly female (82%) and over 30 years of age; this profile is high risk group for autoimmune diseases.4–11
The present patient developed Hashimoto’s thyroiditis in addition to Sjögren’s syndrome and Fanconi syndrome. Plenty of epidemiological, clinical, immunological, histological and genetic evidence support an association between the two autoimmune diseases, Sjögren’s syndrome and Hashimoto’s thyroiditis. Fractures in patients with renal tubular acidosis result from osteomalacia, and rarely occur as the presenting symptom of Sjögren’s syndrome, which is more commonly associated with proximal rather than distal renal tubular acidosis. There are several differential diagnoses. For example, myeloma can lead to proteinuria and multiple fractures. Serum electrophoresis can be helpful to differentiate between underlying diseases. In a study of 170 patients with Hashimoto’s thyroiditis, 17% had Sjögren’s syndrome. 14 In another retrospective study of patients with primary Sjögren’s syndrome, the frequency of Hashimoto’s thyroiditis was three to six times that of the general population. 15 One interpretation is that the thyroid and salivary glands share the same antigens, and the histopathological lesions reveal similar lymphocytic infiltration. Enzyme-linked immunosorbent assay analysis of serum samples from patients with Sjögren’s syndrome and Hashimoto’s thyroiditis found that the antihuman thyroglobulin in patients with both conditions overlapped one region of human thyroglobulin. This suggests that this region may be shared pathogenetically by patients with both Sjögren’s syndrome and Hashimoto’s thyroiditis. 16 Other possible explanations for the association between Sjögren’s syndrome and Hashimoto’s thyroiditis are a sharing of a common genetic predisposition 17 or environmental factors. 18 Patients with Sjögren’s syndrome require periodic examination of their thyroid function so that routine treatment can be employed as soon as hypothyroidism becomes clinically relevant.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This work received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
