Abstract
Objectives
To investigate the clinical value of B-type natriuretic peptide (BNP) in the assessment of severity and prognosis in acute lung injury/acute respiratory distress syndrome (ALI/ARDS).
Methods
Plasma BNP level, arterial blood gases, serum C-reactive protein level, alveolar–arterial oxygen tension difference and oxygenation index were measured in patients with and without ALI/ARDS within 24 h of admission to an intensive care unit. Patients with ALI/ARDS were divided into mild, moderate or severe groups according to the degree of hypoxaemia. Survival >28 days was recorded.
Results
A total of 59 patients with ALI/ARDS and 14 patients without ALI/ARDS were included in the study. Of the patients with ALI/ARDS, 18 had mild hypoxaemia, 20 had moderate hypoxaemia and 21 had severe hypoxaemia. The mean ± SD BNP level was significantly higher in all three ALI/ARDS groups (92.41 ± 28.19 pg/ml, 170.64 ± 57.34 pg/ml and 239.06 ± 59.62 pg/ml, respectively, in the mild, moderate and severe groups) than in the non-ALI/ARDS group (47.27 ± 19.63 pg/ml); the increase in BNP level with increasing severity was also statistically significant. When divided according to outcome, the BNP level in the death group (267.07 ± 45.06 pg/ml) was significantly higher than in the survival group (128.99 ± 45.42 pg/ml).
Conclusions
The BNP level may be of value in evaluating severity and prognosis in patients with ALI/ARDS.
Keywords
Introduction
Acute lung injury (ALI) and its severe form acute respiratory distress syndrome (ARDS) are characterized by acute respiratory insufficiency resulting from noncardiac diseases. Accurate criteria for the objective evaluation of the severity and prognosis of ARDS are currently unavailable. B-type natriuretic peptide (BNP) was first identified by Sudoh et al. 1 in porcine brain, but in humans the main source of BNP is the cardiac ventricle. 2 As the volume and pressure in the ventricle increase, the level of BNP in the blood increases in direct proportion, making BNP an important marker for assessing the severity and prognosis of congestive heart failure. 3 It has been suggested that BNP may be involved in a number of pathophysiological processes in vivo. 4 In particular, it has been reported that pulmonary intravascular microthrombosis and thromboembolism (occurring 12 h after the onset of ARDS and leading to pulmonary disorders and pulmonary hypertension) are accompanied by an increase in the blood BNP level. 5 There are few published studies of the involvement of BNP in noncardiac diseases, and the relationship between BNP level and the diagnosis and prognosis of ARDS has not been reported. The present prospective cohort study aimed to investigate the clinical value of the BNP level in assessing the severity and prognosis of ARDS.
Patients and methods
Patients
Patients with ALI/ARDS, diagnosed using the criteria set out by the American–European Consensus Conference on ARDS 6 and admitted to the intensive care unit of Yantai Yuhuangding Hospital, Yantai, Shandong, China, between 1 January 2011 and 31 December 2012 were recruited to the study. Non-ALI/ARDS patients for comparison were recruited from the same intensive care unit over the same time period. Patients with heart disease, hepatic insufficiency, renal insufficiency, acute cerebrovascular disease or underlying diseases with a poor prognosis that could potentially be the main cause of death were excluded from the study.
Within 24 h of admission, arterial blood gases including arterial oxygen partial pressure (Pa
Patients with ALI/ARDS were divided into three groups according to the degree of hypoxaemia, in accordance with guidelines set by the American–European Consensus Conference on ARDS:
6
those with a Pa
All patients with ALI/ARDS underwent noninvasive haemodynamic determination, including measurement of heart rate, blood pressure, cardiac output, cardiac index, stroke volume, stroke index, systemic vascular resistance and systemic vascular resistance index. Survival of patients with ALI/ARDS was recorded after 28 days.
Written informed consent was obtained from all study participants. The study protocol was approved by the Ethics Committee of Yantai Yuhuangding Hospital, Yantai, Shandong, China.
Statistical analyses
The sample size was determined according to a power analysis of multisample mean comparisons. Data were presented as the mean ± SD. Results from the ALI/ARDS and non-ALI/ARDS groups were compared using analysis of variance; results from the survival and death groups were compared using Student’s t-test. A P-value < 0.01 was considered to indicate statistical significance. All statistical analyses were performed using SPSS® software version 12.0 (SPSS Inc., Chicago, IL, USA).
Results
A total of 59 patients with ALI/ARDS and 14 patients without ALI/ARDS were recruited to the study. Among the 59 patients with ALI/ARDS, 28 had severe pneumonia, four had multicostal fractures, seven had severe acute pancreatitis, eight had undergone gastrointestinal surgery, six had undergone renal surgery, four had pesticide intoxication, one had an abdominal aneurysm and one had acute cholangitis. Of these, 18 patients (10 male and eight female; mean age 57.6 ± 16.3 years; age range 26–81 years) had mild hypoxaemia, with a mean Pa
The non-ALI/ARDS group comprised seven male and seven female patients, aged 26–79 years (mean age 58.6 ± 15.9 years). Diagnoses held by the non-ALI/ARDS patients included recovery from Guillain-Barré syndrome, sustained sedation after surgery for obstructive sleep apnoea syndrome and postsurgery for gastric or colorectal cancer.
Clinical parameters in patients with and without acute lung injury/acute respiratory distress syndrome (ALI/ARDS) on day 1 in the intensive care unit.

Data presented as mean ± SD.
P(A–a)
P < 0.01 compared with non-ALI/ARDS group; Student’s t-test.
P < 0.01 compared with mild ALI/ARDS group; Student’s t-test.
P < 0.01 compared with moderate ALI/ARDS group; Student’s t-test.
Level of B-type natriuretic peptide in patients with acute lung injury/acute respiratory distress syndrome on day 1, 3 and 5 in the intensive care unit according to outcome after 28 days.
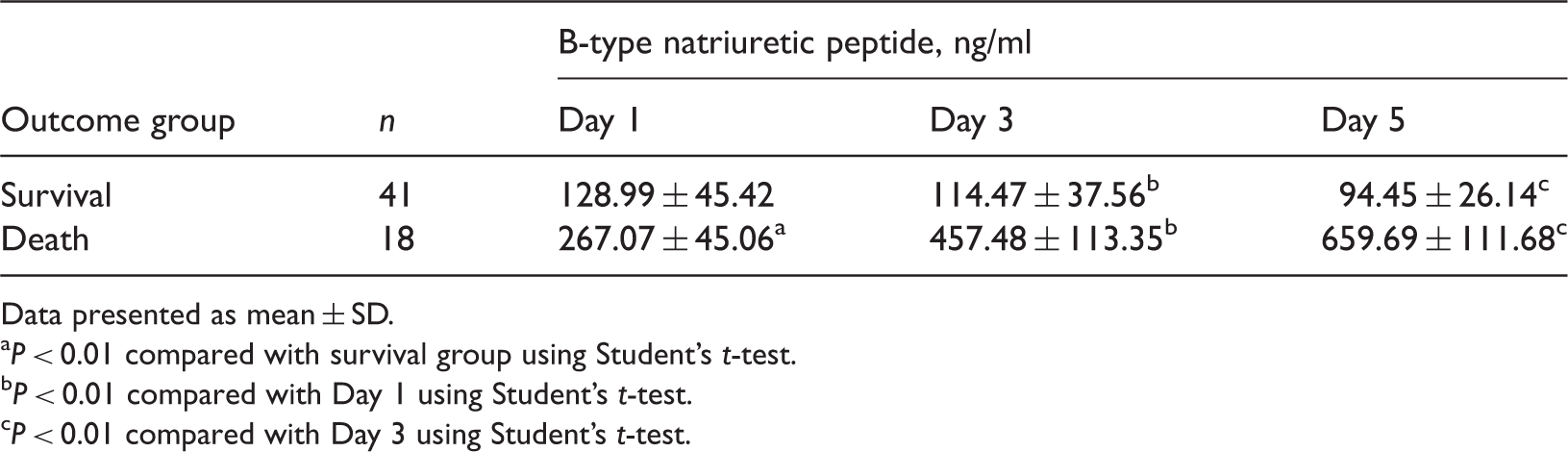
Data presented as mean ± SD.
P < 0.01 compared with survival group using Student’s t-test.
P < 0.01 compared with Day 1 using Student’s t-test.
P < 0.01 compared with Day 3 using Student’s t-test.
Correlation analysis between BNP level and oxygenation index, C-reactive protein level and alveolar–arterial oxygen tension difference [P(A–a)

Discussion
B-type natriuretic peptide is a cardiac neurohormone secreted by the ventricle in response to ventricular expansion and wall pressure overload. The level of BNP in the blood can therefore specifically and sensitively reflect the function of the left ventricle, 7 and is used to evaluate cardiac failure and as an important marker for assessing the treatment and prognosis of congestive heart failure. 8
In the emergency ward and intensive care unit, BNP is often used to identify the fundamental cause of expiratory dyspnoea. 9 As cardiogenic pulmonary oedema and ALI/ARDS have very similar signs and symptoms, it is hard to diagnose ALI/ARDS in patients who have underlying heart disease combined with another cause of expiratory dyspnoea. The diagnosis of ALI/ARDS is increasingly made using the guidelines set by the American–European Consensus Conference on ARDS in 1994, 6 which is based on a comprehensive analysis of hypoxaemia as demonstrated by the oxygenation index, chest X-radiography, the presence of certain risk factors, and the exclusion of cardiogenic pulmonary oedema by a pulmonary capillary wedge pressure <18 mm Hg and the absence of clinical evidence of raised left atrial pressure. This diagnostic method is relatively limited; for example, measuring the pulmonary capillary wedge pressure requires the insertion of a Swan–Ganz catheter, which is invasive and expensive. Given the clinical importance of distinguishing cardiogenic pulmonary oedema and ALI/ARDS, which have different treatments and prognoses, a simple and noninvasive method is required. Due to the high sensitivity and specificity of BNP in cardiovascular diseases, it is of great clinical value in the identification of acute dyspnoea. 10 Abroug et al. 11 measured troponin T and aminoterminal proBNP in 148 intensive care unit patients with acute exacerbation of chronic obstructive pulmonary disease, and compared the levels with diagnoses made by physicians. The BNP level was found to have potential for distinguishing between cardiac and noncardiac causes.
In acute pulmonary embolism, the BNP level has been shown to help evaluate severity; this is especially important in patients with stable haemodynamics, as it could identify high-risk subgroups with right ventricular dysfunction.12,13 In patients with sepsis, the BNP level significantly rises regardless of whether or not they experience traumatic shock, possibly due to septic myocardial damage.14–16 BNP could therefore be a biomarker for sepsis-associated myocardial dysfunction. In patients with sepsis, a higher BNP level indicates a worse prognosis. 17 BNP levels are similar in patients with septic shock and cardiac emergencies; therefore BNP cannot be used to differentiate cardiac and septic shock. 18 BNP could also help determine the optimum time for weaning from mechanical ventilation: Mekontso-Dessap et al. 19 reported that among 102 patients undergoing ventilation weaning, patients who failed the weaning or who had successful ventilation weaning but failed extubation had a significantly higher BNP level than patients with successful ventilation weaning and extubation. This could help identify patients who required delayed ventilation weaning due to a high risk of ventilation weaning failure. 20 Other studies found that in patients with severe sepsis, the BNP level in nonsurvivors was significantly higher than in survivors; BNP could therefore be used to predict death regardless of the cause of hypoxaemic respiratory failure.21,22
In the present study, the blood BNP level in patients with ALI/ARDS was significantly higher than in patients without ALI/ARDS. One possible mechanism for this is that under various stresses the release of inflammatory factors and anoxia can cause damage in myocardial cells. Increased BNP synthesis and release, as well as pulmonary dysfunction and increased pulmonary pressure caused by pulmonary vascular microthrombosis following ARDS onset, could lead to the increase in BNP level.
C-reactive protein is a nonspecific marker of inflammation and tissue damage that has been widely used in clinical practice since the 1980s. Studies show that the CRP level significantly increases in patients with ALI/ARDS. 23 In light of its mechanism of action, it is likely that the CRP level will increase with the severity of disease. In the present study, CRP levels in all three ALI/ARDS groups were significantly higher than in the non-ALI/ARDS group. As the severity increased, the CRP level rose, with significant differences between each severity group.
The P(A–a)
The present study could be improved by using parameters acquired from a pulmonary artery catheter or pulse contour cardiac output in the assessment of cardiac function, which have higher accuracy. However, these techniques are both invasive and expensive, therefore noninvasive haemodynamic determination was used. In addition, the present study could benefit from a larger sample size. Although patients were recruited over a 2-year period, the sample size may not be optimal. However, the present data should be sufficient to draw conclusions that could potentially guide clinical practice. Since the plasma BNP level can also be affected by multiple disorders (including cardiac diseases, shock, pulmonary hypertension, acute pulmonary embolism, chronic obstructive pulmonary disease and renal failure), 24 caution should be taken when using BNP in the evaluation of patients with ALI/ARDS in combination with such conditions.
In conclusion, in the present study the BNP level, CRP level and P(A–a)
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
