Abstract
Objective
These authors contributed equally to this work.
Methods
PubMed® and Embase® databases were searched for relevant studies. Data were extracted using a standardized data collection form. The primary effect measure was the odds ratio (OR) of postoperative infectious complications. Summary OR were calculated.
Results
The analysis included 10 cohort studies with a total of 147 263 participants. Statin use was associated with a lower incidence of postoperative infectious complications in all studies (summary OR 0.917, 95% confidence intervals [CI] 0.862, 0.975, fixed-effects model; summary OR 0.731, 95% CI 0.584, 0.870, random-effects model); cardiac surgery (summary OR 0.673; 95% CI 0.535, 0.847); treatment in the USA (summary OR 0.678; 95% CI 0.597, 0.770); retrospective cohort studies (summary OR 0.664; 95% CI 0.521, 0.846).
Conclusion
Preoperative statin use is associated with a reduced risk of postoperative infectious complications.
Introduction
Postoperative infections prolong hospital stay and increase mortality rates. Despite prophylactic antibiotic therapy, between 5% and 21% of patients develop postoperative infectious complications.1–4 Statins (3-hydroxy-3-methylglutaryl coenzyme A [CoA] reductase inhibitors) have antioxidant,5–7 anti-inflammatory8–10 and antithrombogenic effects, 11 as well as lipid-independent effects including direct inhibition of pathogenic micro-organisms.12,13 The effect of preoperative statin therapy on the incidence of postoperative infectious complications is unclear, with some studies finding a significant reduction in postoperative infections14,15 and others reporting no effect on infection risk.16,17 A meta-analysis of six cohort studies of patients undergoing cardiac surgery was performed in 2012, and found no association between statin use and postoperative infectious complications. 1 The aim of the present meta-analysis was to evaluate the association between statin use and postoperative infectious complications by analysing all available cohort studies, including those published since 2012.14,18–20
Materials and methods
Search strategy
The procedures used for the meta-analysis were consistent with MOOSE guidelines. 21 Electronic databases, including PubMed® and Embase®, were searched from inception to September 2014, to identify relevant studies, using a combination of keywords related to the type of statin (“hydroxymethylglutaryl coenzyme A reductase inhibitors” or “anticholesteremic agents” or “statin” or “simvastatin” or “rosuvastatin” or “pravastatin” or “atorvastatin” or “fluvastatin” or “cerivastatin” or “pitavastatin” or “lovastatin”) and the type of infection-associated disease (“infection” or “sepsis” or “bacteremia” or “pneumonia”). An English language restriction was imposed. Study selection was based on an initial screening of identified abstracts or titles and a second screening of full-text articles. The reference lists of relevant review articles and meta-analyses were examined, to identify other potentially eligible studies.
Eligibility criteria
Eligibility criteria were: (i) observational study design, i.e., patients were assigned into statin and control groups; (ii) study investigated the association between statin use for any indication and incidence of postoperative infections; (iii) study quantified outcomes with adjusted odds ratios (ORs), relative risk, or number of events and corresponding 95% confidence intervals (CIs). When studies did not report adjusted OR, authors were contacted to obtain missing information. Exclusion criteria were: (i) experimental group undergoing other therapy; (ii) review articles; (iii) data unavailable for meta-analysis.
Data extraction and quality assessment
Data were extracted using a standardized data collection form. Data extracted included: last name of first author, publication year, country, number of cases, and adjusted OR. Two reviewers (B.-X. M. and H. L.) worked independently and in duplicate; both extracted and recorded data. Disagreements between the two reviewers were resolved by consensus. Unresolved issues were referred to a third author (J.-S. L.).
The methodological quality of included studies was assessed with the Newcastle–Ottawa Scale (NOS), which comprises three quality parameters: selection, comparability, and outcome (cohort studies) or exposure (case–control studies). 22 Methodological quality was independently assessed by two reviewers (B.-X. M. and H. L.), and any discrepancies were addressed by a joint revaluation of the original article with the third author (J.-S. L.).
Statistical analyses
The primary effect measure was the OR of postoperative infectious complications. Heterogeneity and publication bias were assessed with I2 and Begg’s analysis, respectively. 23 Statistical significance was set at P < 0.05 (two-tailed). The fixed-effects model was applied in the case of no significant difference, and the random-effects model was used in the case of significant difference. Statistical analyses were performed with STATA® version 11 (STATA Corp., College Station, TX, USA).
Results
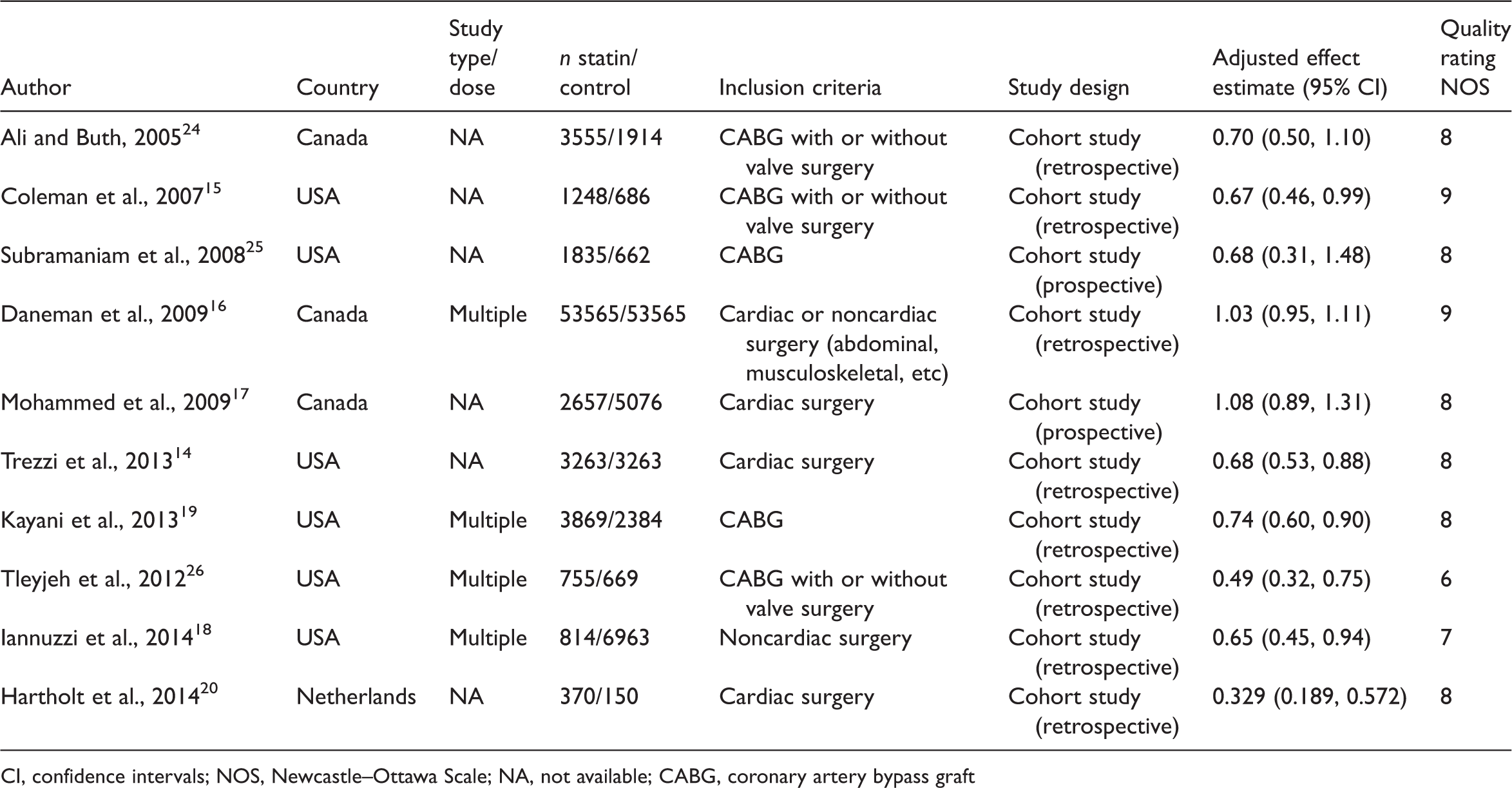
A flow chart showing the study selection process is presented in Figure 1. The analysis included 10 studies with 147 263 patients (71 931 of whom received statins).14–20,24–26 The characteristics and quality assessment of the included studies are presented in Table 1. According to NOS criteria, two studies were of high quality, 15,16 six were medium quality,14,17,19,20,24,25 and two were low quality.18,26
Flow diagram of eligible studies showing the number of citations identified, retrieved, and included in the final meta-analysis. Studies included in a meta-analysis to evaluate the relationship between preoperative statin use and the incidence of postoperative infectious complications. CI, confidence intervals; NOS, Newcastle–Ottawa Scale; NA, not available; CABG, coronary artery bypass graft
Results of meta-analysis including all 10 studies are shown in Figure 2 and Table 2. The use of statins in the preoperative period was associated with a lower incidence of postoperative infections using both a random-effects model (OR 0.731; 95% CI 0.584, 0.870) and a fixed-effects model (OR 0.917; 95% CI 0.862, 0.975).
Forest plot of a meta-analysis to evaluate the relationship between preoperative statin use and the incidence of postoperative infectious complications. Data are pooled odds ratios (OR) for postoperative infections in statin users versus nonusers, determined using a random-effects model. Error bars indicate 95% confidence intervals. Total and subgroup meta-analysis of the relationship between preoperative statin use and the incidence of postoperative infectious complications. OR, odds ratio; 95% CI, 95% confidence intervals.

Results of subgroup analyses are shown in Table 2. Statin use was associated with a lower incidence of postoperative infectious complications in cardiac surgery (summary OR 0.673; 95% CI 0.535, 0.847), in the USA (summary OR 0.678; 95% CI 0.597, 0.770) and in retrospective cohort studies (summary OR 0.664; 95% CI 0.521, 0.846). There was significant heterogeneity in cardiac surgery (P < 0.001) and in retrospective cohort studies (P < 0.001). There was no significant heterogeneity in studies conducted in the USA or Canada, or in prospective cohort studies.
The funnel plot (Figure 3) and Begg’s test (P = 0.283) indicated the absence of publication bias.
Funnel plot of studies included in a meta-analysis to evaluate the relationship between preoperative statin use and the incidence of postoperative infectious complications. Area of each circle represents the contribution of the study to the pooled odds ratio (OR).
Discussion
Findings of our systematic review and meta-analysis show that preoperative statin therapy is associated with reduced numbers of postoperative infections. The large degree of heterogeneity in the present analysis indicates that further investigation is warranted, however.
A systematic review published in 2012 did not find sufficient evidence to support an association between statin use and postoperative infection. 1 Since that time, four additional studies have been published regarding the association between statin use and postoperative infectious complications,14,18–20 all of which found a reduced risk of postoperative infections with statin therapy. In contrast, however, a retrospective cohort analysis indicated that statin use was associated with an increased incidence of common infections in the general population. 27 Our analysis clearly shows that statin use was significantly associated with a reduced risk of infectious complications in patients who underwent surgery.
Statins possess pleiotropic properties,28,29 including cholesterol lowering, anti-inflammatory, immunomodulatory and antioxidant properties.5–13,30–33 High-sensitivity C-reactive protein levels are reduced by statin therapy, 30 and statins modulate the function of immune cells by downregulating various cell receptors and cytokines involved in inflammation, activating natural killer cells, and enhancing phagocytosis.31–35 In addition, studies have demonstrated that statins exert direct antibacterial and antiviral effects on pathogenic micro-organisms.12,13,36
The present meta-analysis has several limitations. First, observational cohort studies were included in this analysis, and their statistical power may not be as strong as that of randomized controlled trials. Secondly, the high degree of heterogeneity complicated interpretation of our findings. Subgroup analyses were conducted to explore the sources of heterogeneity, and determined that country or study design may have been contributing factors. Thirdly, infectious complications included sternal wound infection, organ space infection, pneumonia, urinary tract infection and sepsis; these have different protocol definitions and therefore may be an additional source of heterogeneity. No attempt was made to recategorize types of infection retrospectively. Finally, statin type and dosage varied between the studies, so we were unable to evaluate the influence of the duration and dosage of preoperative statin therapy on the incidence of postoperative infection.
In conclusion, preoperative statin use is associated with a reduced risk of postoperative infectious complications.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not for-profit sectors.
