Abstract
Objectives
To evaluate changes in cuff pressure and position of tapered-cuff and cylindrical-cuff tracheal tubes (TTs) during laparoscopic cholecystectomy; to compare the frequency of endobronchial intubation and airway complaints with the two types of TT.
Methods
Patients were randomly assigned to intubation with a TT with a cylindrical cuff (group C) or a tapered cuff (group T). Anaesthesia was maintained with sevoflurane, O2 and N2O after intubation. TT cuffs were inflated to 20 cm H2O; changes in cuff pressure and volume were measured up to 30 min after the start of N2O use. Distance between the TT tip and the carina was measured before and after pneumoperitoneum and position change. Frequency of sore throat, dysphagia and hoarseness in the two groups was recorded.
Results
Cuff volume and pressure were significantly lower in group T than in group C (n = 32 per group). Cuff pressure and volume significantly increased 30 min after start of N2O use in both groups. Distance from the TT tip to the carina decreased during surgery in both groups. There were no cases of endobronchial intubation, and there were no between-group differences in the frequency of airway complaints.
Conclusions
The tapered cuff was associated with a smaller change in cuff pressure during laparoscopic cholecystectomy than the cylindrical cuff, and therefore may be associated with increased preservation of tracheal mucosal perfusion.
Introduction
Endotracheal intubation using a tracheal tube (TT) is an essential step during general anaesthesia. The design of TT cuffs has evolved since the mid-20th century. Cuffs require proper sealing for positive ventilation, and are maintained using minimal pressure and volume to protect the perfusion of tracheal mucosa, minimizing airway complications such as oropharyngeal aspiration, sore throat and tracheal stenosis.1–3 In order to prevent oropharyngeal aspiration, which often resulted from leakage occurring with the conventional cylindrical cuff, a tapered cuff has been developed.4,5 This cuff has a variable cuff diameter (which is 120% of the tracheal diameter at its widest point) a taper angle of 14°, and creates a ‘sealing zone’ where the cuff diameter corresponds to the tracheal diameter.4,5
Laparoscopic surgery is popular because it is associated with the relief of postoperative pain, a rapid recovery and a shortened hospital stay. 6 Abdominal CO2 gas inflation, positional changes required to provide a good surgical field during laparoscopic surgery and N2O use for anaesthesia may all contribute to endobronchial intubation or postoperative airway complications (due to changes in cuff pressure or in the position of the TT).7,8
This prospective, randomized, double-blind study aimed to evaluate changes in cuff pressure and TT position, and occurrence of endobronchial intubation and postoperative airway complications, using a tapered-cuff TT compared with a conventional cylindrical-cuff TT during laparoscopic cholecystectomy.
Patients and methods
Patients
Patients aged 20–60 years with American Society of Anesthesiologists (ASA) physical status I or II who were undergoing laparoscopic cholecystectomy at Korea University Anam Hospital, Seoul, Republic of Korea, between July 2013 and January 2014 were enrolled in the study. Patients with a history of upper airway surgery, laryngeal disease, nasogastric tube insertion or expected difficulty with intubation were excluded.
All patients provided written informed consent during the preoperative visit. The study protocol was approved by the institutional review board of the Korea University Anam Hospital (ED 13065) and the study was registered with the Clinical Research Information Service (KCT-0000965).
Anaesthesia
After premedication with 0.2 mg glycopyrrolate intramuscularly and 2 mg midazolam intramuscularly 1 h before anaesthesia, patients were monitored using noninvasive arterial pressure, electrocardiography, pulse oximetry and bispectral index. After preoxygenation with O2 at a flow rate of 6 l/min, all patients received 2 mg/kg propofol and 0.6–0.9 mg/kg rocuronium intravenously for tracheal intubation.
After intubation, anaesthesia was maintained using O2 at 1.5 l/min, air at 1.5 l/min and 1–3% sevoflurane. Immediately before skin incision, O2 at 1.5 l/min, N2O at 1.5 l/min and 1–3% sevoflurane were given to maintain a bispectral index monitoring value of 45. Patient position change (30° reverse Trendelenburg with right side up) and gas insufflation for inducing pneumoperitoneum were performed within 10 min after the start of N2O use. Ventilation was controlled at a tidal volume of 7–10 ml/kg. The ventilator rate was adjusted around an end-tidal CO2 of 35 mmHg and peak inspiratory pressures around 25 cm H2O. The intra-abdominal pressure for pneumoperitoneum was automatically maintained at 12 mmHg using an electronic laparoflator (Karl Storz, Tuttlingen, Germany). If the mean arterial pressure increased to 20% above baseline values, fentanyl 1 µg/kg or labetalol 10–20 mg were administered intravenously for haemodynamic stability; a decrease in mean arterial pressure of a similar magnitude was treated with ephedrine 4–8 mg or phenylephrine 100 µg intravenously.
Intubation
Detailed specifications for the cylindrical-cuff and tapered-cuff tracheal tubes used in the study.
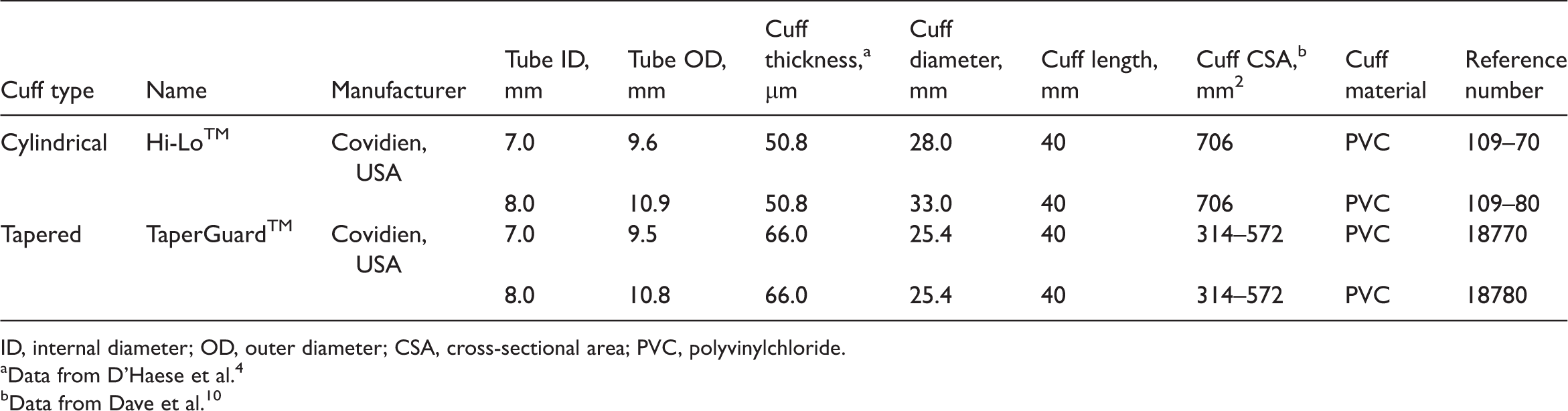
ID, internal diameter; OD, outer diameter; CSA, cross-sectional area; PVC, polyvinylchloride.
Data from D’Haese et al. 4
Data from Dave et al. 10
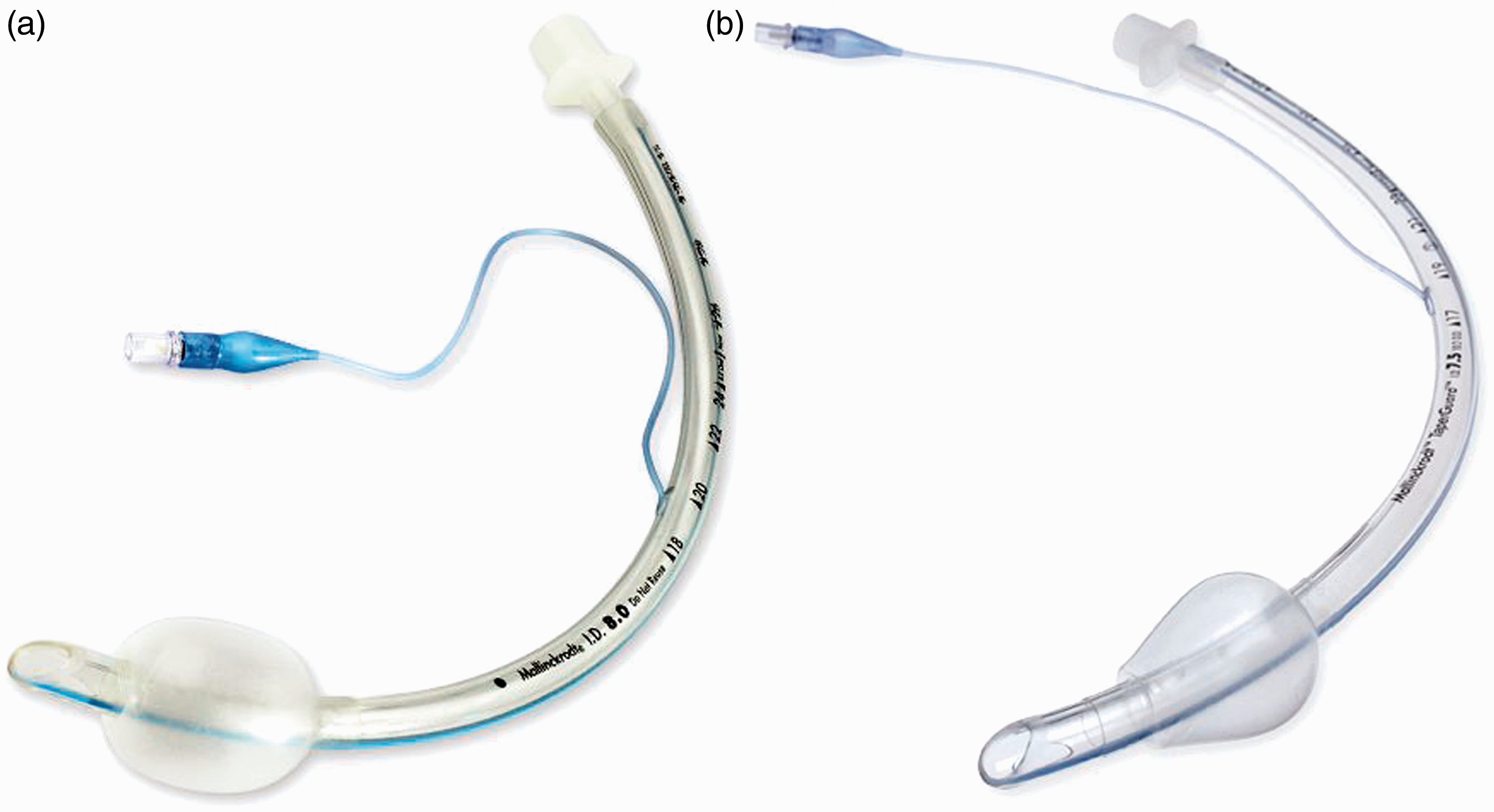
Tracheal tubes used in the study: (A) Hi-Lo™ tracheal tube (group C); (B) TaperGuard™ tracheal tube (group T). The tubes are shown with the cuff inflated at a pressure of 20 cmH2O.
A TT with an internal diameter of 7.0 mm was used for female patients and 8.0 mm was used for male patients. The TT was secured in the centre of the mouth with a bite block at 20 cm from the upper incisors for female patients and at 22 cm for male patients. TT cuffs were completely deflated using a syringe until there was no forward or backward movement of the plunger. The pilot balloon of the tube was then connected to a pressure manometer (Microcuff, Weinheim, Germany) by means of a three-way stopcock. Air was slowly inflated into the cuff to 20 cm H2O (a reasonable lower limit for cuff pressure in adults) 9 by compressing the manometer inflation bulb. The volume of air needed to reach a cuff pressure of 20 cm H2O was measured by deflating it using a 10 ml syringe. The cuff was then re-inflated to a pressure of 20 cm H2O. The pressure in the TT cuff was measured using the pressure manometer via the three-way stopcock 5, 10, 20 and 30 min after the start of N2O use. The volume of the TT cuff was measured by deflating it using a 10 ml syringe 30 min after the start of N2O use. The TT, manometer and cuff syringe were exposed to air to prevent N2O diffusion before each measurement.
To evaluate the position of the TT tip, the distance between the TT tip and the carina was measured with a fibreoptic bronchoscope (Olympus LF-GP™, Olympus Optical Co., Tokyo, Japan) using three tight rubber rings (A, B and C). The patient’s head was placed in a neutral position resting on a head ring. Before intubation, the length of the TT (34 cm for internal diameter of 7.0 mm, 36 cm for internal diameter of 8.0 mm) was marked on the fibreoptic bronchoscope using ring A. Once the tip of the fibreoptic bronchoscope reached the carina, the upper part of the TT was marked on the bronchoscope using ring B immediately after intubation, and using ring C 15–20 min after pneumoperitoneum and position change. The distance between rings A and B and between A and C indicated the difference in the TT tip position after pneumoperitoneum and position change. These measurements were performed by two investigators (H.W.S. and D.H.K.) at the end of expiration.
After surgery
After the surgery had been completed, residual muscle paralysis was antagonized with 0.4 mg glycopyrrolate and 10 mg pyridostigmine, administered intravenously. All anaesthetics were turned off, and ventilation was controlled with O2 at a flow rate of 6 l/min. Patients were extubated when they showed adequate spontaneous ventilation and responded to verbal commands; they were then transferred to the postanaesthesia care unit (PACU). Patients were asked about airway complaints (sore throat, dysphagia and hoarseness) using a four-point scale (0, none; 1, slight; 2, moderate; 3, severe) at the time of discharge from the PACU (∼50 min after arrival at the PACU) and at 12 h after surgery.
Statistical analyses
The minimum number of patients required to show a change in TT cuff pressure at 30 min after the start of N2O use with an initial cuff pressure of 20 cm H2O, with the assumption that a 25% increase between the groups would be clinically relevant, was calculated to be 24 patients per group (α = 0.05, power = 0.80) (PS software, version 3.0, Department of Biostatistics, Vanderbilt University, Nashville, TN, USA).
Data were presented as mean ± SD. Variables between groups were compared using Student’s t-test or Mann–Whitney U-test. Variables at each timepoint within groups were compared using repeated measures analysis of variance, and post-hoc comparisons were performed using Dunnett’s test. Categorical variables were analysed using Fisher’s exact test. A P-value < 0.05 was considered to be statistically significant. All statistical analyses were performed using SPSS® software, version 20 (IBM, Somers, NY, USA).
Results
A total of 70 patients undergoing laparoscopic cholecystectomy were recruited to the study to allow for methodological difficulties that could lead to exclusion from the study. Of these, six patients were excluded (five patients did not meet the inclusion criteria and one patient refused to participate). The remaining 64 patients were randomized; of these, four patients were excluded from the study (two patients due to accidental disconnection between the pilot balloon and the manometer, one patient with a short operation time, and one patient due to conversion to laparotomy). Results from the remaining 60 patients were available for analysis (Figure 2).
CONSORT flow diagram of the study comparing cuff pressure and volume changes in patients intubated with a tracheal tube with either a cylindrical cuff (group C) or a tapered cuff (group T).
Demographic characteristics and anaesthesia and surgery durations in patients undergoing laparoscopic cholecystectomy, intubated with a tracheal tube with a cylindrical cuff (group C) or a tapered cuff (group T).
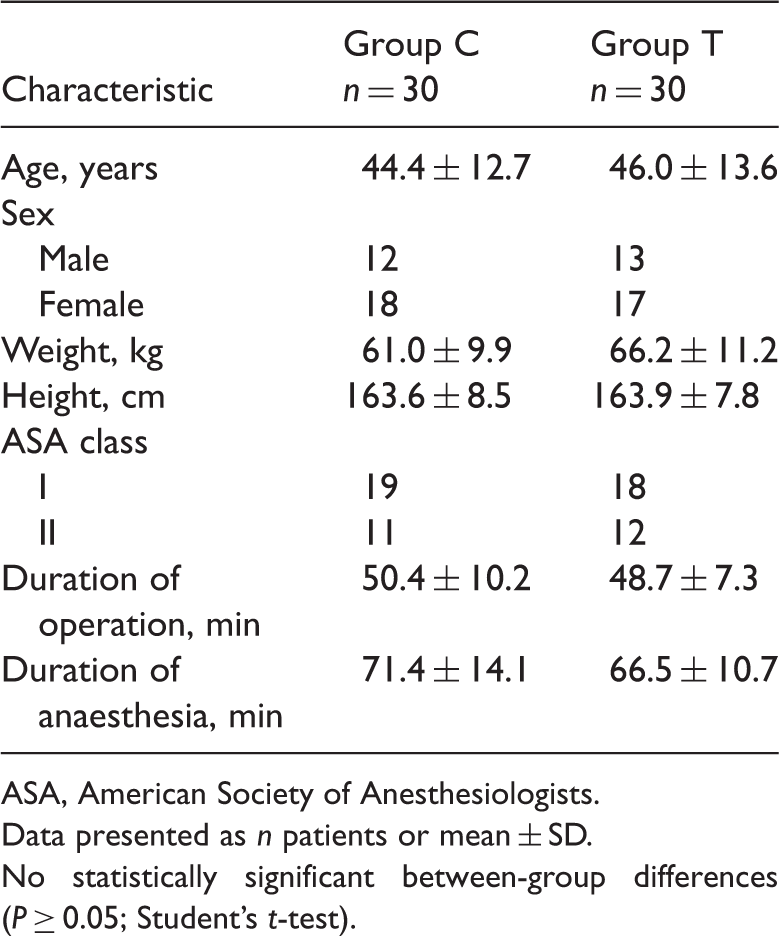
ASA, American Society of Anesthesiologists.
Data presented as n patients or mean ± SD.
No statistically significant between-group differences (P ≥ 0.05; Student’s t-test).
Cuff volume in patients undergoing laparoscopic cholecystectomy, intubated with a tracheal tube with a cylindrical cuff (group C) or a tapered cuff (group T).

Data presented as mean ± SD.
P < 0.05 compared with group C (Student’s t-test); bP < 0.05 compared with baseline value (repeated measures analysis of variance with post-hoc Dunnett’s test).
Cuff pressures in group T were significantly lower at 5, 10, 20 and 30 min after the start of N2O use than those in group C (P < 0.001 for all; Figure 3). Cuff pressures in both groups were significantly increased at 5, 10, 20 and 30 min after N2O use compared with the baseline value of 20 cm H2O (P < 0.001 for all; Figure 3).
Changes in cuff pressure in patients undergoing laparoscopic cholecystectomy, intubated with a tracheal tube with a cylindrical cuff (group C) or a tapered cuff (group T). Data presented as mean ± SD. *P < 0.05 compared with baseline value (repeated measures analysis of variance with post-hoc Dunnett’s test); +P < 0.05 compared with group C (Student’s t-test or Mann–Whitney U-test according to test for normality).
Distance between tracheal tube tip and carina in patients undergoing laparoscopic cholecystectomy, intubated with a tracheal tube with a cylindrical cuff (group C) or a tracheal tube with a tapered cuff (group T).

Data presented as mean ± SD.
No statistically significant between-group differences (P ≥ 0.05; Mann–Whitney U-test).
P < 0.05 compared with baseline value (repeated measures analysis of variance with post-hoc Dunnett’s test).
Postoperative airway symptoms after discharge from the postanaesthesia care unit (PACU) and 12 h postoperatively in patients undergoing laparoscopic cholecystectomy, intubated with a tracheal tube with a cylindrical cuff (group C) or a tapered cuff (group T).

Data presented as n patients.
No statistically significant between-group differences (P ≥ 0.05).
Discussion
Adequate functioning of the TT cuff is essential for proper sealing for positive pressure ventilation while preserving adequate perfusion of the tracheal mucosa.1–3 The cylindrical cuff has a diameter equivalent to 150% of the tracheal diameter and is prone to fluid leakage, due to the presence of folds.2,3 The newly developed tapered cuff has a diameter that is 120% of the tracheal diameter and a taper angle of 14° for proper sealing. 10 Dave et al. 10 reported that the cross-sectional area of the cylindrical cuff is 706 mm2, while that of the tapered cuff varies between 314 and 572 mm2 (Table 1). The varying area provided by the tapered cuff provides an efficient seal despite natural variations in tracheal size,10,11 and may adjust better to age-related anatomical differences in the trachea, especially in children.12,13
Inadvertent high pressure in the TT cuff can cause complications such as sore throat, tracheal ulceration, tracheal stenosis, tracheomalacia and tracheal rupture.13–15 A widely accepted ideal cuff pressure for a polyvinylchloride TT is 20–30 cm H2O; the upper limit of cuff pressure for mucosal perfusion is 30 cm H2O.9,16 In the present study, the tapered cuff required a lower volume of air to achieve a cuff pressure of 20 cm H2O; however, the change in cuff volume 30 min after the start of N2O use was greater in the tapered cuff than in the cylindrical cuff (0.8 ml versus 0.6 ml), but this difference was not statistically significant. In addition, the tapered cuff showed smaller changes in cuff pressure after N2O use compared with the cylindrical cuff. The cuff pressure in both groups significantly increased after N2O use, but the tapered cuff had a smaller increase in pressure than the cylindrical cuff. In a study examining the pressure exerted within a cylinder wall by different types of TTs, the average force on the wall was 527 gf for the cylindrical cuff and 373 gf for the tapered cuff. 17 In addition, the tapered cuff provided a more uniform pressure distribution, reducing the force exerted on the cylinder wall. 17 A second comparative study of two types of TT cuff reported that cuff compliance was greater in a cylindrical cuff compared with a tapered cuff after 60 min of 66% N2O exposure. 18 In the present study, the smaller increase in cuff pressure together with a greater increase in cuff volume in the tapered cuff compared with the cylindrical cuff might be explained by the relatively large compliance and the uneven distribution of volume in the cylindrical cuff.17,18 The findings of the present study suggest that the tapered cuff has the advantage of increased preservation of tracheal mucosal perfusion, associated with a smaller increase in cuff pressure, compared with the cylindrical cuff during surgery.
Yildirim et al. 7 reported that pneumoperitoneum and the reverse-Trendelenburg position increased TT cuff pressure during anaesthetic maintenance with 1–2% sevoflurane and 66% air in oxygen. It is possible that the cuff pressure change seen in the present study may be associated with the combined effect of N2O and pneumoperitoneum; however, it was impossible to distinguish between these two factors from the results recorded. N2O was used as an anaesthetic in order to evaluate its effect on TT cuff pressure and volume. The rate of N2O diffusion into the cuff is proportional to the permeability of the cuff material, the surface area and the partial pressure difference across the cuff, but is inversely proportional to the thickness of the cuff membrane.19,20 The TTs used in the present study were made by same manufacturer, and the patients in both groups were exposed to the same anaesthetic environments. The differences between them were the exposed surface area of the cuff and the thickness of the cuff membrane (Table 1). It is likely that the greater cuff surface area and the greater diffusion through the cylindrical cuff resulted in the greater increase in cuff volume seen with the cylindrical cuff compared with the tapered cuff. However, in the present study there was no statistically significant difference in the changes in cuff volume between the cylindrical and the tapered cuffs. A study by Tsuboi et al., 18 using a lung model, demonstrated that TT cuff pressure rapidly increased up to 80–100 cm H2O after N2O use, with the pressure increasing more in a cylindrical cuff than in a tapered cuff. However, in the present study the maximum cuff pressure recorded was ∼30 cm H2O; this may have been the result of differences between the lung model and the human trachea, including the warm body temperature, gas diffusion through mucosal membranes and the lower compliance of the human trachea.18,20
Pneumoperitoneum with position change during laparoscopic surgery has been reported to induce an increase in peak inspiratory pressure and a decrease in the distance between the TT and the carina.21–23 In the present study, cephalic displacement of the TT tip was observed without endobronchial intubation. The TT tip may have moved towards the head due to splinting or distension of the diaphragm, 24 or tracheal shortening. 8 It was speculated that the TT would be more fixable using a tapered cuff than a cylindrical cuff, but there was no significant difference in displacement between the two cuff types.
Postoperative airway complaints have been reported to be related to age, sex, intubation condition, TT diameter, type of TT cuff and TT movements.25,26 In the present study, the incidence of sore throat was not significantly different in the two groups, which is consistent with previous studies.27,28 The relatively low incidence of sore throat in the present study may have been due to the initial cuff pressure of 20 cm H2O and the short duration of surgery.
In conclusion, the tapered cuff was associated with a smaller change in cuff pressure during laparoscopic cholecystectomy than the cylindrical cuff. In order to prevent airway complications as a result of pressure changes in the TT cuff, frequent monitoring and control of the cuff pressure is necessary.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
