Abstract
Objective
To evaluate the safety profile of blood sugar limits in intensive care unit (ICU) patients.
Methods
Adult patients with ICU stay >36 h, more than two blood sugar measurements and antibiotic therapy concordant with locally adapted guidelines were included. For analyses, one study cohort was defined in two ways: as a narrow group, euglycaemic patients’ blood sugar levels 80–150 mg/dl; as a moderate group, euglycaemic patients’ blood sugar levels 80–180 mg/dl. Dysglycaemia was defined as blood sugar levels <80 mg/dl for >5% of measurements, and >150 mg/dl or >180 mg/dl (narrow or moderate groups, respectively) for >10% of measurements. The primary endpoint was ICU mortality (euglycaemia versus dysglycaemia).
Results
The study comprised 668 patients. When defined as a narrow group, ICU mortality was 3% (four of 135) euglycaemic versus 10% (54/533) dysglycaemic patients (odds ratio [OR] 3.692, 95% confidence interval [CI] 1.313, 10.382). When defined as a moderate group, ICU mortality was 6% (21/351) euglycaemic versus 12% (37/317) dysglycaemic patients (OR 2.077, 95% CI 1.188, 3.630). Frequency of severe hypoglycaemia (blood sugar <40 mg/dl) was not different between the narrow and moderate euglycaemic ranges.
Conclusions
Euglycaemia was associated with lower ICU mortality than dysglycaemia, and incidence of hypoglycaemia was low overall in this study. Based on current published evidence, therapeutic targets should be defined according to individual patient characteristics.
Introduction
Blood glucose irregularities are common problems encountered in the intensive care unit (ICU). 1 In 2001, a milestone was set with the first comprehensive study concerning the control of blood sugar levels in ICU patients. 2 The study showed that stringent control of blood sugar levels reduces mortality and morbidity in the critically ill. 2 Further studies confirmed these data and normoglycaemia became a major goal in the ICU, since tight blood sugar control was shown to reduce mortality rates by one third, and to lower the incidence of postoperative sepsis and multiple organ failure.3–5 In contrast, other studies (sometimes from the same centre), showed that blood sugar margins that were too tight often ended in higher rates of hypoglycaemia and higher mortality, compared with more flexible margins.6–8 In a prematurely stopped multicentre study, intensive insulin therapy was associated with a higher risk of adverse events related to hypoglycaemia, with no effect on mortality rates, compared with less-intensive insulin therapy. 9
The Normoglycaemia in Intensive Care Evaluation Survival Using Glucose Algorithm Regulation (NICE SUGAR) study explored over 6000 patients with a tight and liberal blood sugar control and showed an increase of 14% in mortality risk in the tight control group compared with the liberal group, probably because of a higher risk of hypoglycaemia. 10 Effects on other key parameters, such as length of stay on ICU, were not evaluated in this study. 10 Thus, the development of hypoglycaemic events is of major concern, when intensive insulin therapy is administered, in order to achieve normoglycaemia.
Different bodies, for example those involved with the Surviving Sepsis Campaign, provide blood sugar control recommendations that are less precise for the upper blood glucose concentration, since evidence is sparse regarding the safety of upper limits.9,11–14 Hypo- and hyperglycaemia may cause great harm to the critically ill patient,15,16 with evidence of adverse effects on outcome even with mild hypoglycaemia just below 80 mg/dl. 17 Experts agree that the upper level should not exceed a defined point, but the threshold remains to be determined. Since protocols for continuous glucose monitoring are under development for the critically ill, 18 upper limits for blood sugar levels should be rethought for the daily clinical setting and for randomised controlled clinical trials.
The aim of the present study was to investigate the association between an upper limit for blood sugar control and outcome, in a general ICU population.
Patients and methods
Study population and design
This retrospective observational cohort study was performed as a secondary analysis of prospectively collected data, based on a study of infection control measures (Trial registration: German studies register DRKS00003171). 19 These interrupted series evaluated repetitive time periods at the Charité – Universitätsmedizin Berlin, Berlin, Germany (a tertiary medical care centre with 3 200 beds). Three periods were evaluated for the present analyses: between 1 January 2006 and 31 March 2006; between 1 February 2007 and 30 April 2007; between 1 February 2009 and 31 March 2009. Patients from three mixed ICUs, comprising 61 mainly surgical ICU beds under anaesthesiological management, were included.
Every consecutive adult patient (aged ≥18 years) admitted to participating ICUs during the three time periods was screened. Only patients with an ICU treatment >36 h and with more than two blood sugar measurements performed were included for analysis. To a priori exclude the confounding factor of anti-infective treatment,19,20 an additional inclusion criterion was quality of anti-infective treatment. The study cohort included patients with sufficient anti-infective control (comprising diagnostic and therapeutic procedures) defined as >65% adherence to guidelines and local standards. The Charité – Universitaetsmedizin Berlin ethics committee and the data safety authorities approved this study. The ethics review board waived the need to obtain informed consent from patients, due to the observational nature of the study.
Data collection and measurement
The present study used prospective data that were collected daily from medical records, the hospital mainframe computer, and the patient data management system (COPRA System GmbH, Berlin, Germany) during patients' ICU stay.
Data relating to laboratory findings (including blood sugar values from blood gas analyses), use of anti-infective, vasopressor and steroid agents, ventilation, vital signs, microbiological and radiological diagnostics, pulmonary gas exchange, urine output, and fluid balance were retrieved from the patient data management system.
Cases of insulin dependent diabetes mellitus and noninsulin dependent diabetes mellitus were recorded and grouped as pre-existing metabolic disease.
To assess blood sugar control, every consecutive blood sugar measurement performed during the ICU stay was analysed. Blood sugar measurements were routinely performed via blood gas analyses at least every 2 h in all study ICUs, and at shorter time intervals for therapeutic control following blood sugar interventions. Venous and arterial blood samples were analysed using a Radiometer ABL800 FLEX point-of-care blood gas analyser (Radiometer Medical ApS, Brønshøj, Denmark). At time periods during the study periods, consistent target values for blood sugar control were between ≥80 mg/dl and <150 mg/dl (narrow parameters) or between ≥80 mg/dl and <180 mg/dl (moderate parameters), depending on the preference of the attending physician. There were no defined patient-related factors for determining which parameter was used for blood sugar control. Due to the consistent use of two possible target ranges for blood sugar control, each patient included in the study received treatment for blood sugar control targets that varied between ≥80 mg/dl and <150 mg/dl, and between ≥80 mg/dl and <180 mg/dl during their stay in the ICU. Blood sugar levels were managed with continuous application of intravenous insulin via syringe pump systems, and continuous application of 5–10% glucose (administered intravenously) if the patient was not fed in other ways.
The Simplified Acute Physiology Score (SAPS)-II system 21 was measured regularly in the study ICUs, to estimate disease severity.
Infections were defined according to modified definitions of the Centres for Disease Control and Prevention 22 and American Thoracic Society guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia. 23 Duration of ventilation was defined as the period of mechanical ventilation support during each patient’s ICU stay (intubated or via tracheostomy). ICU stay was defined as the number of days a patient remained in the ICU during one hospital stay, including readmissions from regular wards at Charité -- Universitätsmedizin Berlin, but not from other hospitals.
Adherence to guidelines 24 was recorded and assessed on a daily basis while data collection took place. The following points, alone or in combination, were regarded as guideline discrepancies: missing attention to prior antibiotic regimen, insufficient diagnostic proceedings, delayed antibiotic application, unsuitable combinations, missing combination partner or inappropriate antibiotic, lacking indication, and neglect of de-escalation strategies. The study day was evaluated as ‘adherent’ if all related parts of the guideline were fulfilled (i.e. no guideline discrepancies). Following initial data collection, the data set was reevaluated by an expert team who had the final decision for recording adherence or nonadherence, and these data were used for statistical analyses. The binary variable of daily adherence ‘nonadherent’ versus ‘adherent’ was transformed into a relative variable. Adherence rates were defined as days following the guidelines divided by the total number of days on ICU, and patients who received sufficient anti-infective control with >65% adherence to guidelines and local standards were included in the study analyses. 19
Study endpoints
The primary outcome parameter was ICU mortality rate. Secondary outcome parameters were hospital length of stay, ICU length of stay, duration of mechanical ventilation, and frequency of infections in ICU.
Group assignment
To specifically assess the dynamic of glycaemic control in ICU patients, single blood sugar measurements were evaluated and classified as normal, too low (<80 mg/dl) or too high (>150 mg/dl or 180 mg/dl). Optimal glycaemic management was expected to achieve <5% of all measured blood sugar levels as too low over the whole patient stay. Euglycaemia was defined as <5% of all measured blood sugar levels to be <80 mg/dl over the whole patient stay and <10% of all measured blood sugar levels to be above the defined upper therapeutic limit. Values of >5% blood sugar levels <80 mg/dl for hypoglycaemia and >10% over the specified upper threshold, for the narrow and moderate groups respectively, for hyperglycaemia, were chosen to exclude single erroneous measurements.
Data for the study cohort were analysed in two distinct ways: as a narrow group, in which euglycaemia was defined as <5% of all measured blood sugar levels <80 mg/dl and <10% above 150 mg/dl, and dysglycaemia was defined as patients with blood sugar levels outside the narrow euglycaemic range; and as a moderate group, in which euglycaemia was defined as <5% of all measured blood sugar levels <80 mg/dl and <10% above 180 mg/dl, and dysglycaemia was defined as all patients with blood sugar levels outside the moderate euglycaemic range. In addition, mean ± standard deviation (SD) blood glucose level over ICU stay was calculated for each patient. Mean and SD values were then summarized as median and interquartile range for the study groups.
Tighter blood sugar control was hypothesized to be associated with a higher incidence of hypoglycaemia. The number of patients who experienced at least one severe hypoglycaemic event (defined as blood sugar levels <40 mg/dl) 25 was, therefore, analysed in the subgroup of euglycaemic patients within data defined as a narrow group (80–150 mg/dl). To compare this rate with less tight blood glucose parameters, i.e. data defined as a moderate group (80–180 mg/dl), patients within the narrow euglycaemic subgroup were subtracted from patients within the moderate euglycaemic subgroup. This resulted in two separate subgroups for analysis: patients whose blood glucose fell within a narrow range and patients whose blood glucose fell within a moderate range. Since an upper blood sugar limit of 180 mg/dl is thought to be associated with a higher level of patient safety, 11 the number of patients who experienced at least one severe hypoglycaemic event was evaluated for patients in this adjusted moderate euglycaemic subgroup (80–[151–180] mg/dl), that excluded patients whose blood sugar levels fell within the narrower range.
Statistical analyses
Categorical variables were presented as absolute numbers and relative frequency, and were tested for statistical significance using χ2-test. Continuous data were evaluated graphically for distribution and deviation from normality. Normally distributed variables were presented as mean ± SD and were analysed using Student’s t-test. For ordinal data, or in cases of deviation from normality, data were presented as median, 25th and 75th percentiles and were analysed using Wilcoxon’s rank sum test. Since three time periods of consecutive patient allocation were evaluated, group allocation of patients was analysed using χ2-test, to exclude an effect of time period. Multivariate logistic regression analysis was performed for the primary outcome measure, ICU mortality. Variables that were identified as different between the study groups, based on basic characteristic analyses (age, sex, initial SAPS-II score, underlying metabolic disease, occurrence of infections) were used in the regression model. A backward stepwise selection method was applied to identify the most important factors contributing to ICU mortality. Hosmer–Lemeshow’s goodness-of-fit test was used to assess the quality of the model. All analyses were performed between independent study groups using IBM SPSS® software, version 20.0 (IBM Corporation, Armonk, NY, USA) with a two-tailed type I error margin alpha value of P = 0.05. Post-hoc power analyses were performed using nQuery Advisor® software, version 5.0 (Statistical Solutions Ltd. Boston, MA, USA) to assess the achieved power of the primary outcome parameter. A P-value <0.05 was considered statistically significant.
Results
Patient demographics
Data from 1001 patients underwent primary screening. Following the exclusion of 333 patients who did not meet the inclusion criteria, 668 patients were included in the analysis (Figure 1). Since this study took place during three time periods, patterns of population classification were analysed between them and revealed that there was no statistically significant difference in patterns of population classification (P = 0.178). Patients were admitted for surgical and for medical reasons, and baseline characteristics for the whole study population are shown in Table 1. Glycaemic characteristics for the study population when defined as either a narrow group or a moderate group are displayed in Table 2.
Selection flow chart of patients aged ≥18 years, admitted to an intensive care unit (ICU) for >36 h, who received anti-infective control in accordance with guidelines for >65% of days treated in the ICU. Baseline characteristics of 668 patients aged ≥18 years, admitted to an intensive care unit (ICU) for >36 h, and received anti-infective control in accordance with guidelines for >65% of days treated in the ICU. Data presented as median (25th–75th percentile) or n (%) patient incidence. SAPS-II, Simplified Acute Physiology Score-II.
21
Univariate analysis of basic characteristics and outcome values for patients aged ≥18 years, admitted to an intensive care unit (ICU) for >36 h, who received anti-infective control in accordance with guidelines for >65% of days treated in the ICU. Patient data were analysed as either a narrow group (blood glucose target, 80–150 mg/dl) or a moderate group (blood glucose target, 80–180 mg/dl) to assess glycaemic control and euglycaemic and dysglycaemic subpopulations. Data are presented as n (%) incidence or median (25th–75th percentile). Mean blood glucose, median (interquartile range) of the means of all blood glucose measurements for each patient taken during their ICU stay. Standard deviation of blood glucose, median (interquartile range) of standard deviation of all blood glucose measurements for each patient, taken during their ICU stay. SAPS-II, Simplified Acute Physiology Score-II.
21
NS, no statistically significant differences (P > 0.05).


When defined as a narrow group, the euglycaemic subpopulation differed significantly from the dysglycaemic subpopulation in terms of age, initial SAPS-II, and metabolic disorders (P ≤ 0.001). When defined as a moderate group, age, sex and metabolic disorders were found to be significantly different between the euglycaemic and dysglycaemic subpopulations (P < 0.05).
ICU stay, mechanical ventilation, frequency of infection
When data were defined as a narrow group, duration of intensive care unit stay was significantly different between the euglycaemic subpopulation (median, 3 [25th–75th percentiles, 2–6] days) and the dysglycaemic subpopulation (4 [2–9] days, P = 0.002). However, when defined as a moderate group, there was no statistically significant difference between the two subgroups (3 [2–9] days for the euglycaemic subpopulation versus 4 [2–9] days for the dysglycaemic subpopulation, P = 0.234).
When defined as a narrow group, duration of mechanical ventilation was significantly lower in the euglycaemic subpopulation (16 [8–34] h) versus the dysglycaemic subpopulation (25 [10–110] h, P = 0.006). However, when defined as a moderate group, there was no statistically significant difference between the two subgroups (euglycaemic subpopulation, 21 [9–94] h versus dysglycaemic subpopulation, 25 [11–102] h, P = 0.733).
When defined as a narrow group, frequency of infections during ICU stay was significantly higher in the dysglycaemic subpopulation (253/533 [47%]) compared with the euglycaemic subpopulation (50/135 [37%], P = 0.033). However, when defined as a moderate group, there was no statistically significant difference between the two subgroups (euglycaemic subpopulation, 159/351 [45%] versus dysglycaemic subpopulation, 144/317 [45%], P > 0.999).
ICU mortality
Overall mortality in the present study cohort was 8.7% (58/668 patients, 95% confidence interval (CI) 6.5, 10.8). When the data were defined as a narrow group, mortality rate was four of 135 patients (3.0%) in the euglycaemic subgroup compared with 54/533 patients (10.1%) in the dysglycaemic subgroup (P = 0.006). When data were defined as a moderate group, mortality rate was 21/351 patients (6.0%) in the euglycaemic subgroup compared with 37/317 patients (11.7%) in the dysglycaemic subgroup (P = 0.013). The corresponding univariate odds ratios (ORs) were 3.692 (95% CI 1.313, 10.382) for the narrow group and 2.077 (95% CI 1.188, 3.630) for the moderate group.
Influence of different blood sugar control limits
In addition to the blood sugar levels defined in the narrow and moderate analysis groups, alternative upper limits for blood sugar control were analysed, ranging between 140 and 180 mg/dl using 10 mg/dl steps. The resulting ORs (Figure 2) revealed an upper limit of 150 mg/dl to have the strongest association between mortality and blood sugar control. Furthermore, the achieved post-hoc power for this analysis was found to be 1 − β = 80% for the 80–150 mg/dl blood sugar level range and 1 − β = 69% for the 80–180 mg/dl blood sugar level range.
Univariate logistic regression analyses of 668 patients aged ≥18 years, admitted to an intensive care unit (ICU) for >36 h, who received anti-infective control in accordance with guidelines for >65% of days treated in the ICU: ICU mortality as the dependent variable; euglycaemic versus dysglycaemic status as the covariable. Each bar represents odds ratio (OR) and 95% confidence interval (CI) for an independent regression analysis in the study population, with a different cut off for hyperglycaemia, between140 and 180 mg/dl using 10 mg/dl steps. Resulting ORs show increased risk for dysglycaemic, compared with euglycaemic, patients.
Multivariate analyses of mortality
Two multivariate logistic regression analyses (using backward stepwise selection) with ICU mortality as dependent variable in 668 patients aged ≥18 years, who attended an intensive care unit (ICU) for >36 h and received anti-infective treatment in accordance with guidelines for >65% of days treated in the ICU. The same patient data were analysed as either a narrow group (blood glucose target, 80–150 mg/dl) or a moderate group (blood glucose target, 80–180 mg/dl).
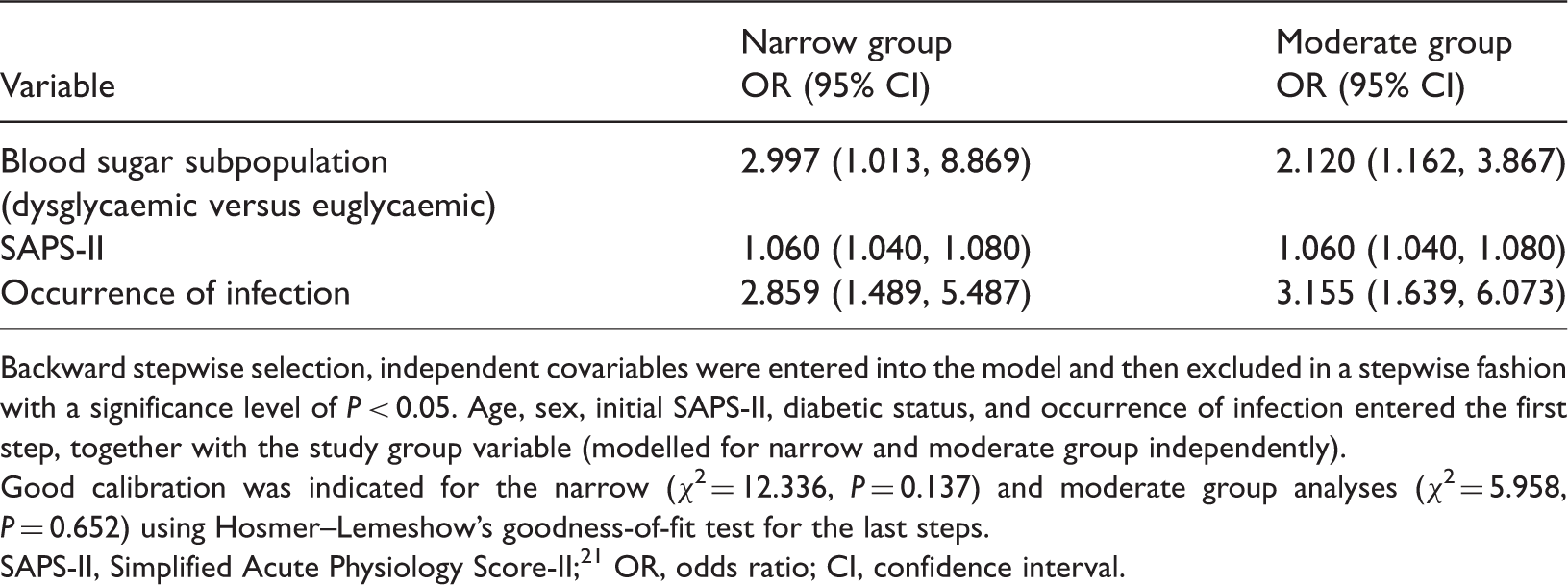
Backward stepwise selection, independent covariables were entered into the model and then excluded in a stepwise fashion with a significance level of P < 0.05. Age, sex, initial SAPS-II, diabetic status, and occurrence of infection entered the first step, together with the study group variable (modelled for narrow and moderate group independently).
Good calibration was indicated for the narrow (χ2 = 12.336, P = 0.137) and moderate group analyses (χ2 = 5.958, P = 0.652) using Hosmer–Lemeshow’s goodness-of-fit test for the last steps.
SAPS-II, Simplified Acute Physiology Score-II; 21 OR, odds ratio; CI, confidence interval.
Hypoglycaemic events
To compare the frequency of hypoglycaemic events in two unique subgroups described in the methods, the number of patients who experienced a single severe hypoglycaemic event (<40 mg/dl) was examined. In the narrow euglycaemic subgroup, with blood sugar margins between 80 and 150 mg/dl, three of 135 patients (2.2%) experienced severe hypoglycaemia; in the adjusted moderate euglycaemic subgroup, with blood sugar margins between 80 and 151–180 mg/dl, four of 216 patients (1.9%) experienced severe hypoglycaemia (P > 0.999).
Discussion
Treatment of hyperglycaemia to a reasonable degree is widely accepted to improve outcomes in critically ill patients. However, optimal therapeutic targets for blood glucose control remain controversial.10,13 The most important finding of the present study was that a blood sugar level between 80 and 150 mg/dl was associated with a lower risk of mortality than other ranges, and levels within this range were not associated with a higher number of patients experiencing severe hypoglycaemic events. A lower maximum limit for blood sugar control has been associated with better patient outcomes,26,27 however, hyperglycemia may only be an independent risk factor in patients without diabetic history in cardiac, cardiothoracic, and neurosurgical ICUs. 28 In the present dataset, distribution of basic characteristics was unbalanced in terms of age, sex, initial SAPS-II, and pre-existing metabolic disease. Consequently, all these factors were included in multivariate logistic regression analyses to identify the isolated association between blood sugar population (dysglycaemic versus euglycaemic) and mortality, without the influence of these cofactors. After adjusting for relevant factors contributing to variability in blood sugar management, an independent and statistically significant association between blood sugar control and mortality remained, for data defined as a narrow or a moderate range (Table 3). In addition, length of stay and duration of mechanical ventilation were significantly different between subpopulations in patients defined as a narrow group, both being longer in the dysglycaemic population. These results concur with a large database from the USA, which concluded that patients with deviations from normoglycaemia experience a prolonged length of ICU stay and duration of mechanical ventilation. 27 In addition, tighter blood sugar control has been associated with a shorter duration of mechanical ventilation and ICU stay.27,29 Other studies were unable to show an association between blood sugar control and duration of hospital stay or mechanical ventilation,9,10 but those studies had a different focus and the ranges for blood sugar control diverged widely.9,10 Patients in the present study were admitted to ICU mainly following surgery and, in this subgroup of patients, control for hyperglycaemia appears to be more important compared with medical ICU patients. 30
In the present study, incidence of infections during ICU stay was distributed differently when data were defined as a narrow group, with higher infection incidence in the dysglycaemic population. Duration of antibiotic therapy has been shown to be reduced in patients who receive intensive insulin therapy 29 and tight glycaemic control was associated with lower risk of infection in a study including surgical patients. 5 Interestingly, this finding was also described in a meta-analysis, albeit this effect was limited to the subgroup of surgical patients. 31 The present study aimed to evaluate mortality in a mixed critical care population with different factors possibly interacting with study conclusions. Preliminary works from the Charité – Universitätsmedizin Berlin showed that infection control management was a relevant cofactor for outcome measures.19,20 To exclude this confounding factor, quality of antiinfective treatment was one of the inclusion criteria in the present study.
Overall mortality in the present analysis is consistent with that observed in previous studies undertaken in predominantly surgical ICUs. When blood sugar data were defined as a narrow group, mortality rate was <4% of patients in the euglycaemic population compared with a three-fold increase in mortality in the dysglycaemic population, and when defined as a moderate group, mortality rate was 6% of patients in the euglycaemic population compared with a two-fold increase in mortality in the dysglycaemic population. A meta-analysis found no difference in mortality between tight glucose control and standard care, but a higher risk for hypoglycaemia in the tight glucose control groups, although most of the studies included had an upper cut-off that was <110 mg/dl. 31 One point that might associate the present findings with previous studies is that only patients with an ICU stay >36 h were examined, and a previous study has shown that blood sugar levels become more important in patients requiring longer ICU treatment. 2 One large dataset analysis from the USA found a higher mortality rate the higher the mean blood glucose measurement. In the group with a level between 70–110 mg/dl the mortality rate was below the overall mortality rate observed in the study, whereas the mortality rate in the 111–145 mg/dl group was almost equal to overall mortality, increasing to nearly twice the overall mortality rate in patients with a mean glucose level above 300 mg/dl. 32 Although this finding was not consistent in all subgroup analyses, the described association was high in patients with sepsis and pneumonia. Similarly, in the present study population, infections were diagnosed in the majority of patients.
In the present study, there was an association between alternative measured upper blood sugar limits and mortality. The effect size nearly doubled from an upper limit of 180 mg/dl to 150 mg/dl, and still reached statistical significance. Notably, the corresponding statistical power for the observed difference in ICU mortality achieved 82%. Most published studies on blood glucose levels have included upper target limits that were far from normoglycaemia.9,10,17 Analysis of a large database revealed that the risk of hospital mortality progressively increased as the deviation from normoglycaemia increased. 27 Like this study, the present study assessed daily blood sugar values, not mean values over time. An upper limit <150 mg/dl has been described as beneficial in at least some patients, particularly in burned or traumatized patients, or following cardiac surgery.33,34 Based on these data, it seems reasonable to target such a blood sugar margin in future pivotal studies. 35 The lower the blood sugar limit, the higher the risk of hypoglycaemia, 14 and both moderate and severe hypoglycaemic episodes are associated with an increased risk of death. 36 To compare the risks of severe hypoglycaemia in the present study, the number of patients with these events were evaluated in two patient groups. The overall hypoglycaemia rate in the present study was lower than in other studies,10,35 and comparably low rates of severe hypoglycaemia were revealed in both blood sugar-level margins. This is contrary to other studies, in which groups with narrow blood sugar parameters had a higher incidence of severe hypoglycaemic events compared with broader parameters.6,9,31,36 The authors believe that this might, at least in part, be a problem with the upper limit, as every insulin substitution inherits a potential for hypoglycaemia, particularly regarding the variability of individual insulin response. Hypoglycaemia is also addressed in a meta-analysis, in which hypoglycaemia was less common in a moderately tight glucose control group than in a very tightly controlled group. 31 ICU mortality has been shown to increase with severity and duration of deviation from euglycemia, including incidence of hypoglycaemic events. 27
The results of the present study are limited by a number of factors. First, this was a secondary data analysis without randomization, therefore, the results advocate further prospective trials evaluating different blood sugar levels, particularly in terms of safety. The present study evaluated achieved blood glucose parameters, rather than the effects of targeting treatment to defined blood glucose parameters. Since patients who were analysed as falling within a narrow blood glucose range (80–150 mg/dl) were not specifically treated in a prespecified protocol to achieve this target range, no conclusions can be drawn regarding the safety of targeting this narrow blood glucose range when managing patients within the ICU. Secondly, since patients were not specifically treated to achieve the varying blood sugar parameters assessed in the present study, it is not possible to draw any conclusions on whether tight glucose control leads to a favourable outcome, or whether other factors contributing to a favourable outcome ease the maintenance of tight blood sugar control. Due to the nature of retrospective observational trials, it is impossible to monitor every source of bias. Thirdly, the present study only included one hospital from one city with mainly surgical patients, and included only patients with an ICU stay >36 h, who would be expected to experience greater blood sugar variations than patients with a shorter ICU stay. 29 Consequently, the generalizability of the present results is limited. Fourthly, previous studies have led to the assumption that, for some admission diagnoses, the association between hyperglycaemia and mortality is stronger than for other diagnoses. 32 Due to the limited number of patients in the present study, no further subgroup analysis could be performed, in particular, addressing patients with diabetes mellitus. Finally, insulin dosages were not measured, although there are good reasons to believe that in terms of outcome, the level of blood glucose is the decisive factor rather than the amount of insulin used. 9
In conclusion, despite numerous randomized controlled trials, defining single blood sugar limits for overall ICU patients appears to be arbitrary and remains an individual decision. In the present study, a more favourable outcome was associated with euglycaemia compared with dysglycaemia, in patients whose data were defined according to relatively narrow blood sugar-level parameters of 80–150 mg/dl. In addition, patients whose blood sugar levels fell within this range were not associated with higher rates of single severe hypoglycaemic events compared with patients whose blood sugar levels fell within a moderate range of 80–180 mg/dl. Further prospective studies are required to understand how these results relate to extrinsic control of blood sugar levels within a similar narrow range, in ICU patients.
Footnotes
Declaration of conflicting interest
IN and ST received lecture fees from Roche GmbH and Pfizer. CS received funding from Merck Sharp and Dome GmbH, Astra Zeneca, Bristol-Myers Squibb GmbH, Pfizer, and Fresenius Kabi. AT, AR, ML, FW, FB, JB, and KDW declare no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
