Abstract
The aetiology and pathological mechanisms involved in the development of haematidrosis (bloody sweat) remain unclear. There is no specific treatment for this disorder. This case report describes the clinical manifestations and treatment of a 9-year-old female with haematidrosis associated with epilepsy. The diagnosis of haematidrosis was confirmed by medical personnel who observed the bleeding and were able to rule out other causes of the bloody exudate. The episodes of bleeding were spontaneous, transient, and self-limited. Smears of the bloody exudate contained all of the components of peripheral blood. A skin biopsy taken at one site of the bloody exudate was normal, showing no signs of blood extravasation or bleeding sweat glands. The bleeding events were found to be immediately preceded by tonic seizures. An electroencephalogram indicated cerebral parietooccipital epilepsy, which was characterized by an intermittent medium-high amplitude θ rhythm (5–7 Hz) with a few spikes. The symptoms of both epilepsy and haematidrosis resolved after treatment with the antiepileptic drug 150 mg oxcarbazepine, orally, twice a day, which suggests that the epileptic seizures triggered haematidrosis in this patient.
Introduction
Haematidrosis (bloody sweat) is a very rare disorder. 1 Bleeding can manifest on the intact mucosa or skin in almost any part of the body, and may occur at several points simultaneously. 2 Diagnosis can only be made if the following criteria are met: (i) spontaneous and self-limited bleeding is witnessed by medical personnel; (ii) the usual components of peripheral blood are found in the bloody exudate; and (iii) the mucosa and skin are intact without any cuts, abrasions, purpura or telangiectasia. 1 All of these criteria must be met in order to rule out bleeding resulting from bleeding disorders, self-injury and chromhidrosis.3–5
The pathogenesis of haematidrosis remains poorly understood. Holoubek and Holoubek 1 suggested a classification system that includes five categories based on causative factors: component of systemic disease; vicarious menstruation; excessive exertion; psychogenic; unknown. Acute fear and extreme levels of stress were found to be the most common causes of haematidrosis. 1 To date, there are no specific treatments for this disorder. Our previous report described a patient with haematidrosis whose syndrome was associated with sympathetic nerve activation. 6 The present case report describes a girl in whom the onset of haematidrosis might be associated with concomitant epilepsy because all of her clinical problems were successfully resolved following administration of the antiepileptic drug, oxcarbazepine.
Case report
A 9-year-old girl presented to the Department of Haematology, PLA 100th Hospital, Suzhou, Jiangsu Province, China, in March 2012 with recurrent episodes of ‘bloody sweat’ that had begun 6 months earlier. The episodes of bleeding were spontaneous, transient, and self-limited; they occurred on various parts of her body (including skin, canthi, tongue, nails or umbilicus), lasted for 1–2 min, then ceased immediately (Figure 1A). The frequency of the bleeding events was from once every few days to several times a day. During hospitalization, her recurrent bleeding was witnessed by medical personnel. Occasionally, medical personnel observed the production of white frothy secretions from her tongue and umbilicus, which were followed by oozing blood (Figures 1B and 1C). Moreover, the bleeding episodes were immediately preceded by intense headache and abdominal pain, which were often accompanied by nausea and vomiting. At the onset of an episode, the patient might have a tonic seizure for several minutes without muscle jerks, and then became unresponsive for several minutes. The patient had not yet reached menarche and had no prior history of haemorrhage or other illness. She took no medications and had no known allergies to any foods or medicines. Her family history was negative. Her physical and psychological examinations showed no abnormalities.
Spontaneous episodes of bleeding seen out of the corner of the left eye (A), on the patient’s tongue (B) and white frothy secretions that spontaneously occurred on the umbilicus (C) in a 9-year-old girl who presented with recurrent episodes of ‘bloody sweat’ suggestive of haematidrosis.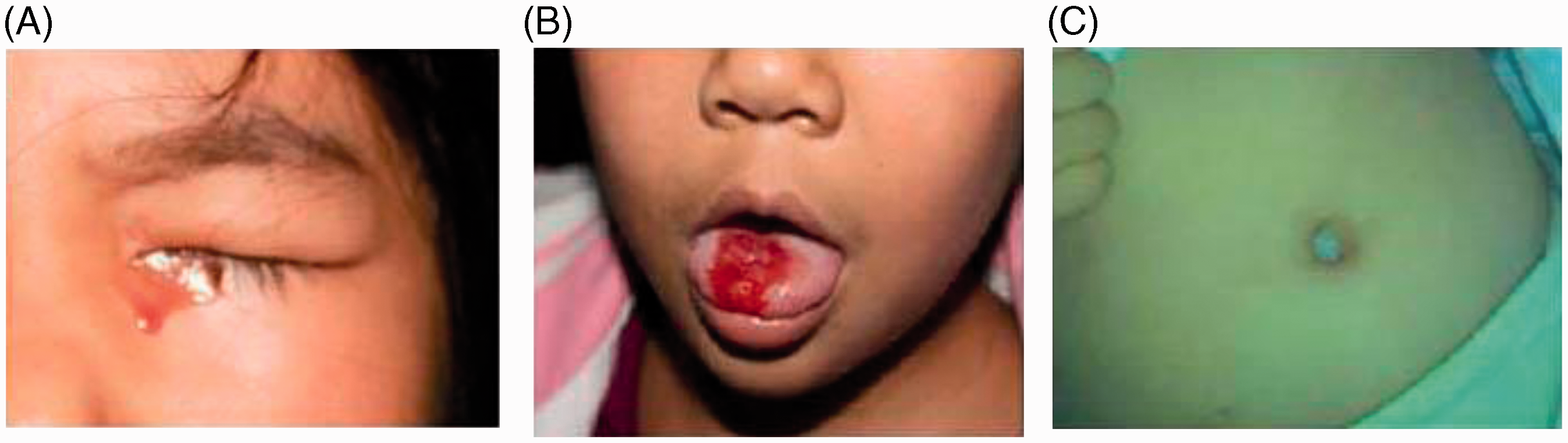
Laboratory investigations showed that her complete blood count, blood biochemistry, platelet aggregation, bleeding time, coagulation screening tests, various coagulation factors and von Willebrand factor results were all within normal ranges (Table 1). The bloody exudate was smeared onto a glass slide, observed using light microscopy and was shown to contain all the components of peripheral blood, including red blood cells, leukocytes and platelets (Figure 2A), while the white frothy secretions taken from the umbilicus only revealed leukocytes (Figure 2B). A skin biopsy taken of the waist bleeding site after a bleeding event was normal, showing no signs of blood extravasation or bleeding sweat glands (Figure 2C). An electroencephalogram (EEG) performed immediately after a seizure indicated cerebral parieto-occipital epilepsy, which was characterized by an intermittent medium-high amplitude θ rhythm (5–7 Hz) with rare spikes over the bilateral parietal and occipital region (Figure 3). During an asymptomatic period, intermittent medium amplitude θ rhythm still existed over the same region. In contrast, brain magnetic resonance imaging showed no significant abnormalities (such as atrophy, sclerosis, tumours or arteriovenous malformations). The diagnosis of epilepsy was made according to epilepsy guidelines.
7
Representative photomicrographs of samples taken from a 9-year-old girl who presented with recurrent episodes of ‘bloody sweat’ suggestive of haematidrosis; (A) smear prepared from a sample of ‘bloody sweat’, which contained red blood cells, leukocytes and platelets (Wright’s stain); (B) smear of the white frothy secretion collected from the navel, which contained only leukocytes (Wright’s stain); (C) tissue section taken from the waist bleeding site after a bleeding event, showing the normal structure of the skin tissue without any indications of blood extravasation (haematoxylin and eosin). Scale bar, 10 µm. Electroencephalogram performed immediately after a seizure in a 9-year-old girl demonstrated cerebral parietooccipital epilepsy, characterized by intermittent medium-high amplitude θ rhythm (5–7 Hz) with rare spikes over bilateral parietal and occipital regions. These abnormalities remained during an asymptomatic period, as demonstrated by intermittent medium amplitude θ rhythm over the same region. Pink regions show abnormal brain waves; green region is not clinically relevant. Results of haemostatic tests undertaken on a 9-year-old girl who presented with recurrent episodes of ‘bloody sweat’ suggestive of haematidrosis.


The patient was first treated with a tranquillizer (2.5 mg diazepam, administered orally, three times a day) and a β-blocker (10 mg propranolol, administered orally, three times a day) for 10 days, but the bleeding episodes did not improve. She was then treated with an antiepileptic drug (150 mg oxcarbazepine, administered orally, twice a day). The symptoms of both epilepsy and haematidrosis were decreased after a week of oxcarbazepine treatment and had completely disappeared 1 month later. The patient has been treated with 150 mg oxcarbazepine orally, twice daily, and followed-up for 1 year, and has had no relapse or recurrence of the haematidrosis except for one occasion when she fought with another girl and then experienced a minor ‘bloody sweat’ on the forehead. It was not associated with an epileptic seizure and was not treated. After 1 year of controlling the epilepsy, the dose of oxcarbazepine was gradually tapered and finally withdrawn. The patient has had no further epileptic seizures.
Written informed consent for publication of the patient’s information and images was obtained from the parents. The First Affiliated Hospital of Soochow University Suzhou, Suzhou, Jiangsu Province, China does not require ethical approval for reporting individual cases.
Discussion
The patient described in this current case report was an otherwise-healthy 9-year-old girl without any laboratory evidence of bleeding diathesis or any other illness; her haemostatic tests were normal, indicating no evidence for any possible haemorrhagic disorders. She was not at the age of menarche, which excludes the possibility of vicarious menstruation. However, it was noted by the medical personnel that the repeated bleeding episodes appeared immediately following clinical manifestations of epilepsy, which was confirmed by an abnormal EEG, characterized by intermittent medium-high amplitude θ waves and sudden bursts of electric spikes. These findings suggest that haematidrosis was associated with parieto-occipital epilepsy in this patient.
Few reports describe histopathological examinations in patients with haematidrosis; published findings have shown only minimal and inconsistent changes (including congested or occluded capillaries, or minor blood extravasation from capillaries).5,6,8–10 The histopathology of a skin biopsy taken from the bleeding site at the waist area of this current patient was normal. All of these observations indicated no obvious pathological changes, which suggests that there was a functional abnormality in the local skin vasculature. As already mentioned, fear and extreme levels of stress are the most common triggers of haemotidrosis, 1 and sympathetic nerve activation might be involved. 6 In this current patient, epileptic seizures appear to have triggered the bleeding events. Therefore, it seems likely that haematidrosis can be caused by an increase in local vasopermeability, caused by exceptional stimulus from the various neuropsychological activities associated with an epileptic seizure. However, the reason why it is extremely rare for people to present with ‘bloody sweat’ remains unknown. Further research is required to define the pathological mechanisms involved in the development of haematidrosis.
To date, there are no specific treatments for haematidrosis. Administration of vitamin C and general haemostatic drugs has been proven not to be efficacious. 1 Manonukul et al. 11 administered the anxiolytic, lorazepam, to reduce a patient’s anxiety level, and achieved an excellent result in terms of the haematidrosis. An excellent result was also previously achieved with the β-blocker, propranolol, in a patient with haematidrosis associated with sympathetic nerve activation. 8 Subsequent reports have confirmed the beneficial effect of propranolol,10,12,13 but one other report on haematidrosis did not mention treatment. 14 These findings suggest that propranolol is an effective agent for some patients with haematidrosis. However, the patient described in this current case report was not responsive to propranolol, but made a complete recovery after being treated with oxcarbazepine. These findings suggest that in this patient the episodes of ‘bloody sweat’ were associated with the epileptic seizures. Oxcarbazepine provides adequate control of seizures in >60% of patients with epilepsy. 15 It would be interesting to investigate whether treating a nonepileptic patient with haematidrosis with oxcarbazepine can control the bleeding episodes. In addition, other anticonvulsive drugs could be used to treat this current patient with haematidrosis, to investigate if they also control haematidrosis. This would help to confirm if oxcarbazepine is the only antiepileptic drug that can control haematidrosis.
Haematidrosis is a very rare bleeding disorder; little is known about its aetiology and pathophysiological mechanisms. This current case report describes a female patient with haematidrosis that was associated with concomitant epilepsy, who achieved complete control of her seizures and total resolution of the bleeding episodes when treated with the antiepileptic drug oxcarbazepine. This current case is representative of the heterogeneity of this bleeding disorder with regard to symptoms, aetiology and response to treatment. Each patient with haematidrosis requires an individualized treatment plan that takes into consideration the possible aetiological factors.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This work was supported by the National Science Foundation of China (no. 30770917, no. 81070395), the Priority Academic Programme Development of Jiangsu Higher Education Institutions (PAPD), Jiangsu Province’s Key Medical Centre (no. ZX201102), and Life and Health Special Funds of the Jiangsu Province’s Science and Technology Bureau (no. BL2012005).
