Abstract
Objective
Cysteine-rich, angiogenic inducer, 61 (CYR61) is a key gene in the transforming growth factor-β signalling pathway, which is involved in the development of many tumour types. This study aimed to clarify the status and clinical significance of CYR61 expression in patients with ovarian epithelial carcinoma.
Methods
Tissue from patients with ovarian epithelial carcinoma or benign ovarian tumours were investigated retrospectively for CYR61 expression at mRNA and protein levels, using reverse transcription–polymerase chain reaction and immunohistochemistry, respectively. Correlations between immunohistochemical scores and several clinicopathological parameters were investigated.
Results
In 50 patients with ovarian epithelial carcinoma and 50 patients with benign ovarian tumours, CYR61 expression on mRNA and protein levels was significantly higher in ovarian epithelial carcinoma tissue than in benign ovarian tissue. CYR61 expression was associated with regional lymph node metastases and progression of clinical disease stage. There was no difference in CYR61 expression between patients aged <50 years and ≥50 years.
Conclusions
CYR61 expression was significantly upregulated in ovarian carcinoma tissue compared with benign ovarian tumour tissue samples. Protein CYR61 levels were associated with lymph node metastases and Union for International Cancer Control stage. Protein CYR61 may be useful in targeted diagnosis and therapy, for patients with ovarian epithelial carcinoma.
Keywords
Introduction
Ovarian epithelial carcinoma, which accounts for 90% of ovarian cancer cases, continues to be the leading cause of death among gynaecological malignancies. 1 Over two-thirds of cases are not diagnosed until the disease has spread beyond the ovaries, due to the asymptomatic nature of early stage disease.2,3 The development of novel biomarkers 4 for early detection of ovarian epithelial carcinoma is therefore essential to improve the survival of patients with this disease.
Cysteine-rich, angiogenic inducer, 61 (CYR61) encodes protein CYR61, which belongs to the connective tissue growth factor, CYR61 and nephroblastoma overexpressed (CCN)1–6 family, and has been implicated in diverse biological processes such as cell adhesion, migration, angiogenesis and wound healing.5,6 CYR61 is an important gene in the transforming growth factor-β (TGF-β) signalling pathway and it can be activated by thrombospondin-1 through its interaction with latent TGF-β binding proteins. This interaction results in activation of TGF-β so that it can bind to its receptors, thus stimulating the Smad pathway.7,8 Smad proteins can bind to protein CYR61, which leads to transcription of CYR61, and activation of angiogenesis and tumour growth.9,10 CYR61 expression can, therefore, play a key role in growth and development, and is critically involved in the development of some tumours.11,12 CYR61 expression has been shown to be significantly higher in Barrett’s oesophageal adenocarcinoma tissue than in Barrett’s oesophageal tissue with no sign of cancer.13,14 The significance of CYR61 expression and prognosis in ovarian epithelial cancer, however, remains uncertain.
The present study aimed to explore CYR61 expression and determine whether protein CYR61 could be a prognostic factor in ovarian epithelial carcinoma. Expression of CYR61 in ovarian epithelial carcinoma was investigated by immunohistochemical staining. In addition, the relationship between CYR61 expression and clinicopathological parameters in patients with ovarian epithelial carcinoma was investigated.
Patients and methods
Study population and sample collection
Patients with primary ovarian epithelial carcinoma and patients with benign ovarian tumours, treated at the Department of Obstetrics and Gynaecology, The Second Hospital, Jilin University, Changchun, China between December 2011 and March 2013, were included in this retrospective study. Patients with a previous or secondary malignancy, or who had previously undergone chemotherapy or radiotherapy treatment, were excluded from the study. Clinicopathological information was collected from the data held in records for the patients diagnosed with ovarian epithelial carcinoma. Tumours were staged according to the tumour–node–metastasis staging system of the Union for International Cancer Control (UICC; 5th edition). 15
All patients received standard surgery as appropriate, to provide maximal tumour resection. For each patient, a sample of ovarian tissue had been fixed in 10% formalin, embedded in paraffin wax and cut into 4 -µm thick serial sections for immunohistochemical staining; a second sample had been snap-frozen at –80℃ for subsequent total RNA isolation; methodologies are described fully below.
This study was approved by the Ethics Committee of the Second Hospital, Jilin University. Written informed consent was obtained from all participants.
RNA preparation and semiquantitative RT–PCR
Total RNA was isolated from the frozen ovarian tissue samples using TRIzol® reagent (Invitrogen™, Life Technologies, Carlsbad, CA, USA) according to the manufacturer’s protocol. In short, the tissue, frozen at –80℃ was ground using a pestle and mortar. 100 mg of ground tissue was then incubated with 1 ml TRIzol® reagent for 5 min at room temperature. Cell debris was removed by centrifugation at 12 000 g for 10 min at 4℃ and 0.4 ml chloroform was added. The mix was then vortexed, followed by incubation for 5 min at room temperature. The phases were separated by centrifugation at 12 000
Immunohistochemistry assay
To detect CYR61 expression and localization of protein CYR61 in ovarian tissue, immunohistochemistry was performed using a streptavidin–peroxidase immunohistochemical staining kit (Tiangen; Beijing, China) according to the manufacturer’s instructions. In short, ovarian tissues were fixed in 10% buffered formalin, dehydrated in ethanol, embedded in paraffin wax and cut into 4 -µm thick sections for use in immunohistochemistry analyses. Sections were deparaffinized in xylene and rehydrated with graded alcohols. For heat-induced epitope retrieval, sections were immersed in 0.01 M citrate buffer solution (pH 6.0) and pressure cooked for 10 min (the pressure of this step was not constant). Sections were then cooled for 1 h at room temperature, then washed in water and 0.01 mM phosphate-buffered saline (PBS; pH 7.2). Hydrogen peroxide (0.3%) was applied to block endogenous peroxidase activity and the sections were incubated with normal goat serum at 37℃ for 2 h to reduce nonspecific binding. Sections were then incubated overnight at 4℃ with primary rabbit antihuman CYR61 (polyclonal; 1 : 25 dilution; Santa Cruz Biotechnology, Santa Cruz, CA, USA), then washed three times in 0.01 mM PBS (pH 7.2) for 5 min. Secondary biotinylated goat antirabbit serum immunoglobulin G 1 : 200; Tiangen Biotech, Beijing, China) was added at 37℃ for 2 h. After washing 3 times in 0.01 mM PBS (pH 7.2), sections were stained using the ImmunoCruz™ ABC staining system (Santa Cruz Biotechnology), and the colour was developed with diaminobenzidine, according to the manufacturer’s instructions. The immunohistochemical staining was evaluated at × 100 and × 400 magnifications using an Olympus BX51 light microscope (Olympus Optical, Tokyo, Japan). PBS was used in place of the primary antibody as a negative control.
The level of immunoreactivity was assessed according to a semiquantitative method 16 and was measured using a scale between − and +++, where − represented no immunostaining; + represented <25% cells reactive; ++ represented 25–50% of cells reactive; +++ represented >50% of cells reactive. Scores of − and + were considered to be negative; scores of ++ and +++ were considered to be positive.
Statistical analyses
Statistical analyses were performed with SPSS® software, version 13.0 (SPSS Inc., Chicago, IL, USA) for Windows®. Student’s t-test was used to compare means between two groups. The relationships between CYR61 expression and clinicopathological variables (including age, UICC stage and presence of lymph node metastasis) in patients with ovarian epithelial carcinoma were examined using Χ2-test. Data were presented as mean ± SD and n (%) incidence. P values <0.05 were considered to be statistically significant.
Results
This study included 50 patients with ovarian epithelial carcinoma (mean age, 51.23 ± 2.1 years) and 50 patients with benign ovarian tumours (mean age 50.4 ± 1.9 years). There were no significant between-group differences in terms of mean age (Student’s t-test).
Semiquantitative RT–PCR analysis showed that levels of CYR61 mRNA were significantly increased in ovarian epithelial carcinoma tissue compared with benign ovarian tumour tissue (P < 0.05; Figure 1).
Cysteine-rich, angiogenic inducer, 61 (CYR61) mRNA levels in ovarian epithelial carcinoma and benign ovarian tumour tissue samples. (A) Representative reverse transcription –polymerase chain reaction agarose gel, showing differences in CYR61 expression: lane 1, ovarian epithelial carcinoma tissue; lane 2, benign ovarian tissue; lane M, DNA ladder. (B) Integrated density value (IDV) of CYR61 mRNA ovarian epithelial carcinoma and benign ovarian tissue. Data presented as mean ± SD. There were significantly different CYR61 mRNA levels between the two tissue groups (P < 0.05, ovarian epithelial carcinoma tissue versus benign ovarian tissue (Χ2-test).
Protein CYR61 immunoreactivity in ovarian tissue appeared as fine, granular to diffuse cytoplasmic and membrane staining (Figure 2). Positive immunohistochemical staining for protein CYR61 (i.e. ++ or +++ staining intensity) was detected in tissue samples from 35/50 (70 %) patients with ovarian epithelial carcinoma; these levels of staining were significantly higher than those seen in the benign tumour group (13/50 [26.0 %] patients; P < 0.05).
Representative immunohistochemical diaminobenzidine staining of cysteine-rich, angiogenic inducer, 61 protein in human ovarian epithelial carcinoma and benign ovarian tumour tissue samples.; (a) benign ovarian tissue. (b) Stage II ovarian epithelial carcinoma tissue; (c) Stage IV ovarian epithelial carcinoma tissue The colour version of this figure is available at: http://imr.sagepub.com.
The relationship between cysteine-rich, angiogenic inducer, 61 (CYR61) expression (measured using immunohistochemical staining of protein CYR61 in ovarian epithelial tissue) and clinicopathological features in patients with ovarian epithelial cancer.
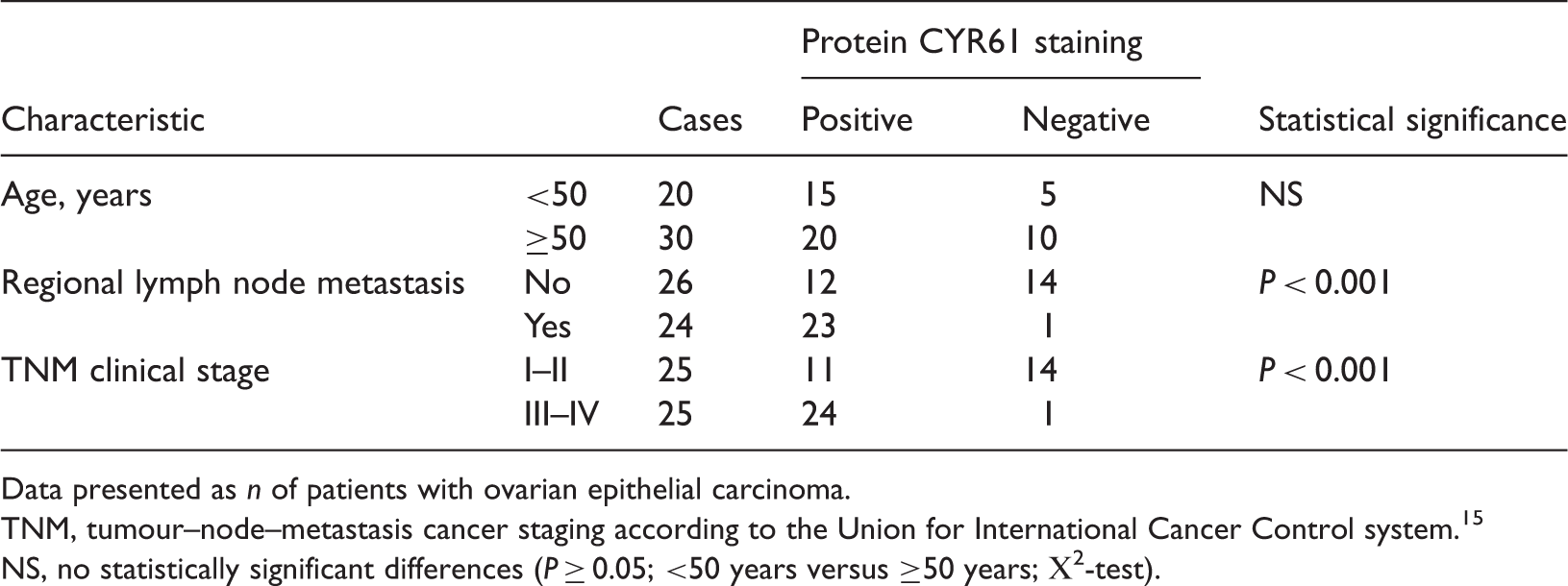
Data presented as n of patients with ovarian epithelial carcinoma.
TNM, tumour–node–metastasis cancer staging according to the Union for International Cancer Control system. 15
NS, no statistically significant differences (P ≥ 0.05; <50 years versus ≥50 years; Χ2-test).
Discussion
The present study investigated expression of the CYR61 gene in ovarian tissues from patients with ovarian epithelial carcinoma or benign ovarian tumours. Levels of CYR61 expression were significantly upregulated in the ovarian epithelial carcinoma group compared with the benign tumour group at both an mRNA and protein level. Furthermore, in the patients with ovarian epithelial carcinoma, significant associations were identified between levels of protein CYR61 and UICC stage and lymph node metastasis, suggesting that CYR61 expression may be involved in disease pathogenesis.
Protein CYR61 is a secreted, heparin-binding and extracellular matrix-associated angiogenic inducer belonging to the CNN1–6 family, which regulates cell adhesion, migration, proliferation and differentiation, and is involved in tumour growth.5,6 Research shows that CYR61 may be regarded as both a suppressor and a promoter of cancer progression and tumour invasion.14,17 Studies have shown that CYR61 can suppress carcinogenesis in nonsmall cell lung cancer or gastric carcinoma.17,18 However, other studies have shown that CYR61 can enhance carcinogenesis.19–21 The findings that CYR61 enhances tumour growth in a gastric adenocarcinoma cell line, RF-1, and in breast cancer cell lines,19–21 are consistent with results of the present study, in which CYR61 expression levels were increased in patients with ovarian epithelial carcinoma compared with those with benign tumours, and upregulation of protein CYR61 was significantly associated with lymph node metastases and UICC stage. These results suggest that the level of CYR61 expression may be associated with the malignant potential of ovarian epithelial carcinomas.
In conclusion, the present retrospective study demonstrated that CYR61 expression was significantly upregulated in ovarian carcinoma tissue compared with benign ovarian tumour tissue, and that upregulation of protein CYR61 was significantly associated with presence of lymph node metastasis and UICC stage III–IV disease, in patients with ovarian epithelial carcinoma. The present study findings suggest that CYR61 may play a key role in the development of malignant tumours.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
The authors gratefully acknowledge the financial support provided by The Health Bureau of Jilin, grant No. 2012Z019.
