Abstract
Ovarian adult-type granulosa cell tumors are often associated with endometrial hyperplasia or even uterine cancer. Herein, we present a case report of a 65-year-old female patient who had undergone curettage of the uterine cavity several times due to abnormal and irregular uterine bleeding. Owing to recurrent episodes of vaginal bleeding as well as ineffective pharmacological treatment of simple endometrial hyperplasia without atypia, the patient underwent a laparoscopically-assisted vaginal hysterectomy. Owing to an enlarged right ovary with bluish color, intra-operative pathological examination was immediately performed. Surprisingly, an ovarian adult-type granulosa cell tumor was diagnosed, and the surgery was extended to pelvic lymphadenectomy and omentectomy. Immunohistochemical staining with selected antibodies (Arginase 2, Nidogen 2, BAF250a/ARID1A, GPR30, SF-1/NR5A, and 1LRH-2E1/NR5A2) was also performed. In conclusion, in cases of recurrent vaginal bleeding concomitant with endometrial hyperplasia, the existence of rare ovarian tumors connected with extensive estrogenic stimulation must be taken into account. Immunostaining with selected antibodies (Arginase 2, Nidogen 2, ARID1A, or GPR30) may help elucidate the possible molecular mechanisms associated with the BAF250a/development of various ovarian/endometrial abnormalities.
Keywords
Introduction
Granulosa cell tumors (GCTs) constitute up to 7% of malignant ovarian tumors and nearly 70% of ovarian gonadal tumors.1,2 GCTs are characterized by low dynamics as well as late relapses, and they are sub-divided into juvenile- or adult-type. 2 In general, GCTs are potentially curable, with only a low percentage of treatment failures.2,3 The main feature of these tumors is their ability to synthesize sex steroid hormones, estrogens in particular.1–3
Approximately 66% of women affected by GCTs develop abnormal and recurrent uterine bleeding as the first clinical symptom of disease.3,4 Moreover, abdominal swelling or even palpable structures may be incidentally detected during gynecologic examination. As a result of hyperestrogenism, there is a high percentage of co-occurrence of endometrial hyperplasia with cellular atypia (ranging from 24% to 80%), and approximately 5% of highly-differentiated endometrial neoplasms are subsequently diagnosed.2,4–6 Additionally, there is a predisposition for the parallel occurrence of endometrial and breast cancers. 3 The determination of estradiol, although not in all patients, is applicable for monitoring treatment results. In approximately 30% of patients, hormone levels are not elevated due to the lack of thecal cells in some tumors. Thecal cells produce the estradiol precursor, which in granulosa cells with aromatase activation, is converted into the active form. 3
The prognosis of women with ovarian GCTs is generally good.4,7 Overall, the long-term survival reaches 75% to 90%. The 5-year survival of patients with stage I disease is 92% to 100%. Unfortunately, while stages III and IV are uncommon, they are associated with unfavorable outcomes, similar to that of ovarian cancer. In these stages, the 5-year survival rate is only 22%.3–5,7
In this report, we describe a patient with recurrent vaginal bleeding, who developed ovarian adult-type GCT concomitant with simple endometrial hyperplasia without atypia. Moreover, immunohistochemistry (IHC) with selected antibodies (Arginase 2, Nidogen 2, BAF250a/ARID1A, GPR30, SF-1/NR5A1, and 1LRH2E1/NR5A2), whose activity have previously been reported in different human malignancies,8–13 was also studied. There are only a limited number of cases assessing the IHC staining of these antibodies in ovarian adult-type GCT (PubMed database).
Case report
Patient data
A 65-year-old woman (P3A0) presented with recurrent episodes of vaginal bleeding. At the age of 57, the patient underwent resection of the pheochromocytoma from the right adrenal gland. She suffered from arterial hypertension for several years.
The first abnormal vaginal bleeding appeared when she was 60, 7 years after the last menstruation. The patient underwent endometrial biopsy, which confirmed the presence of simple endometrial hyperplasia without atypia. After treatment with lynestrenolum (5 mg, three times per day for 21 days with a 7-day break) for 4 months, an end-stage gestagen reaction was detected. After 2 years, she returned to the hospital with abnormal vaginal bleeding. After the first month of hormonal therapy, which the patient tolerated well, another endometrial biopsy was performed. The presence of simple endometrial hyperplasia without nuclear atypia was detected once again, and she was subsequently treated with lynestrenolum. Abnormal vaginal bleeding returned after 1 year, and the presence of a simple hyperplasia with fibrous endometrial polyp was detected. For 1 year, the bleeding repeated. Anatomopathological examination revealed simple endometrial hyperplasia with partially polypoid endometrium. Administration of progesterone (100 mg twice per day) for 6 months was prescribed but, unfortunately, recurrent vaginal bleeding repeated when therapy was finished.
During follow-up, transvaginal ultrasonography was repeatedly performed, which confirmed the presence of a linear endometrium of 5 to 7 mm thickness and homogenous myometrium. Although recent transvaginal ultrasonography scans showed that both ovaries were normal-sized with no liquid in the recto-uterine pouch, a small ovarian tumor (2 cm in diameter) was surprisingly found on her right ovary. The CA125 marker was within the normal range (<30 U/mL) over several examinations; inhibin-B levels were not determined. After discussing the performed tests and presenting therapeutic possibilities with the patient, the gynecologist-oncologist recommended surgical intervention. Owing to recurrent episodes of vaginal bleeding as well as ineffective pharmacological treatment of simple endometrial hyperplasia, the patient underwent a laparoscopically-assisted vaginal hysterectomy. Owing to finding an enlarged right ovary of bluish color, intra-operative pathological examination was immediately performed. Surprisingly, a ovarian adult-type GCT was diagnosed, and surgery was extended to pelvic lymphadenectomy and omentectomy.
The postoperative course was uneventful, and the patient was discharged on postoperative day five. She subsequently submitted to consultation with the gynecologist-oncologist. Based on her examination and pathologic data, no adjuvant therapy was recommended. She was free of disease at 1-year follow-up, and her inhibin-B level was within the normal range. She is still under careful follow-up.
IHC
IHC was performed using a two-step method. Sections were deparaffinized and rehydrated using routine methods. Antigen retrieval by microwave and blocking of endogenous peroxidase activity were conducted before primary antibody incubations. The primary antibodies [anti-Arginase 2,-Nidogen 2, -BAF250a/ARID1A, and -1LRH-2E1/NR5A2 (Merck Millipore, Burlington, MA, USA); anti-SF-1/NR5A1 (Perseus Proteomics, Tokyo, Japan); anti-GPR30 (Abcam, Cambridge, UK); all diluted 1:200] were applied overnight at 4°C. The primary antibodies were then removed, and the slides were incubated for 30 minutes at room temperature with a biotin-free horseradish peroxidase enzyme-labeled polymer of the EnVision+ detection system (DAKO, Denmark). Following reaction with 3,3-diaminobenzidine, the sections were counterstained with hematoxylin, dehydrated, and cover-slipped. Positive controls (normal placental tissue) was processed according to manufacturer's recommendation. Sections processed without primary antibody were used as negative controls. Immunostained sections were evaluated by two independent investigators as follows: (−) no staining; (+) a majority of cells with weak staining, (++) moderate staining of a majority of cells; (+++) intense staining of a majority of cells.
Results of IHC staining
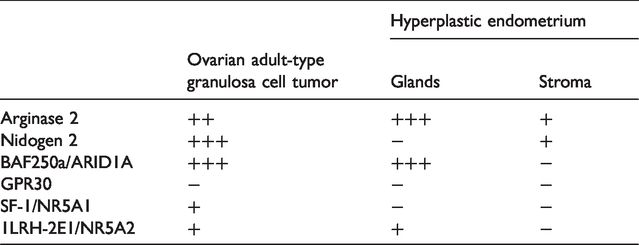
A summary of the IHC results are listed in Table 1. Briefly, there was moderate Arginase 2 expression in the ovarian tumor cells as well as in the glands of the hyperplastic endometrium (Figure 1a–b), whereas ARID1A showed intense staining in a majority of the ovarian adult-type GCT cells as well as in the endometrial hyperplasia/glands (Figure 1c–d). Nidogen 2 was highly positive only in the ovarian adult-type GCT cells (Figure 1e–f). It is worth noting that GRP30 immunoreactivity was reported in neither malignant ovarian cells nor in endometrial glands or stroma (Table 1). SF1/NR5A1 and 1LRH-2E1/NR5A2 showed only weak or no immunoreactivity (Table 1).
Summary of the immunohistochemical staining results in the ovarian adult-type granulosa cell tumor and hyperplastic endometrium.

Expression of Arginase 2 in the ovarian adult-type granulosa cell tumor (a) and simple hyperplastic endometrium (b); Nidogen 2 immunoreactivity in the ovarian adult-type granulosa cell tumor (c) and simple hyperplastic endometrium (d); Immunostaining for ARID1A in the ovarian adult-type granulosa cell tumor (e) and simple hyperplastic endometrium (f) (magnification: 600×).
Discussion
In this study, we report the case of a 65-year-old women who underwent several interventions owing to recurrent vaginal bleeding. After ineffective pharmacological treatment, surgery was applied. During a careful intra-operative pathological examination, adult-type GCT of her right ovary was detected, which was associated with the previously reported endometrial pathologies. We did not find evidence of ovarian malignancy during the several transvaginal ultrasonography scans, although the most recent one displayed a small (2 cm in diameter) ovarian tumor on her right ovary. As an explanation, prolonged endometrial exposure to estrogen stimulation that is produced by a small adult-type GCT may cause endometrial abnormalities, leading to endometrial hyperplasia or even cancer.
The question of whether endometrial biopsy should be routinely performed in symptomatic/asymptomatic patients with adult-type granulose cell tumors of the ovary now must be addressed. Previously, Ottolina et al. 14 suggested that endometrial sampling should be done in symptomatic women above 40 years old. However, in asymptomatic patients below 40 years old, endometrial sampling is of low quality. 14 In the literature, endometrial hyperplasia has been concomitantly detected in nearly 30% of adult-type GCT patients, whereas endometrial cancers occurred in only 7.5% of this population. 14 Interestingly, 16.5% of patients (162 out of 1031) diagnosed with ovarian GCT showed concurrent simple endometrial hyperplasia, while GCT and endometrial cancer were reported together in 251 women (25.5%). 6 In another report, 15 all patients (n = 4) with GCTs revealed simple endometrial hyperplasia without atypia, similar to our case.
We next applied selected human antibodies (Arginase 2, Nidogen 2, BAF250/ARID1A, GPR30, SF-1/NR5A1, and 1LRH-2E1/NR5A2), all of which have been previously investigated in various human malignancies, for IHC. Among this panel, Arginase 2, Nidogen 2, and ARID1A revealed enhanced immunoreactivity in both adult-type GCT and simple endometrial hyperplasia. Conversely, lack of IHC reactivity was found for GPR30.
In a rat model, Arginase 2 expression varied among different organs, suggesting it may play organ-specific roles in the urea cycle. 16 Moreover, Arginase 2 is expressed in human lung cancer cells, but does not affect immune escape or disease progression. 8 Altogether, Arginase 2 expression has been implicated in immune system dysfunction, infection, vascular disease, and the development/progression of many human malignancies. 17 In this case, Arginase 2 expression in the ovarian tumor and simple endometrial hyperplasia may be connected with the development of these abnormalities, but the role of Arginase 2 alterations in disease progression is still unknown.
In this study, Nidogen 2 was highly positive only in the ovarian adult-type GCT cells. In the literature, both IHC and genetic data have suggested that loss of Nidogen 2 expression has a pathogenic role in gastrointestinal, lung, and nasopharyngeal malignancies.9,18–21 Moreover, absence of Nidogen 2 in the endothelial basement membrane of the lung has been implicated in metastasis formation. 19 These data suggest that Nidogen 2 overexpression may have a potentially beneficial influence on ovarian tumors and disease progression.
In a previous review, Takeda et al. 21 reported that ARID1A mutations are involved in a subset (40%–57%) of endometrial and ovarian malignancies. Moreover, the expression of ARID1A protein was associated with the differentiation status of endometrial cancers but not with other clinicopathological features (FIGO stage, depth of myometrial infiltration, or lymph node involvement) or patient survival. 22 Recently, Khalique et al. 10 showed that optimized ARID1A IHC assessment predicted its mutational status in various gynecological malignancies. They suggested that this could be useful for recruiting patients into clinical trials based on ARIDIA mutational status. Therefore, the expression of ARID1A protein may reliably suggest genetic alterations in adult-type GCT, which could be informative because it is involved in neoplastic formation via the PI3K/AKT pathway.
GPR30 is an alternative estrogen-responsive receptor that is overexpressed in neoplasms where ER/PgR are downregulated. GPR30 is also involved in the initiation and progression of various human malignancies.11,23–25 Previously, Smith et al. 23 suggested that patients with GPR30 overexpression had significantly poorer survival than those who lack immunoreactivity(65.2% vs. 100%; p = 0.005). Moreover, the G protein-coupled estrogen receptor GPR30 independently predicts poor relapse-free survival in women treated with tamoxifen. 24 In early-staged (FIGO I) cervical carcinomas, cytoplasmatic overexpression of GPR30 was positively correlated with tumor grade, predicting beneficial complete- and relapse-free survival. 25 Based on this case, lack of GPR30 immunoreactivity may be potentially associated with favorable outcomes for women affected by adult-type GCT; however, this observation needs verification in a larger cohort.
Conclusions
In cases of recurrent vaginal bleeding concomitant with endometrial hyperplasia, the existence of rare ovarian tumors that are connected with extensive estrogenic stimulation must be taken into consideration. Immunostaining with selected antibodies (Arginase 2, Nidogen 2, ARID1A, and GPR30) may help elucidate the possible molecular mechanisms associated with the development of various ovarian/endometrial abnormalities.
Footnotes
Acknowledgements
The authors would like to acknowledge the administration of the Hospital of Princess Anna Mazowiecka in Warsaw, Poland, for access to histological specimens. We would also like to thank Mrs. Karina Zajączkowska for her excellent immunostaining analysis.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics approval and consent to participate
This study was approved by the Independent Ethics Committee at the Warsaw Medical University, Warsaw, Poland/Ethics Committee reference number 43/11/.
The patient provided written informed consent for publication of her clinicopathological data as well as histological images.
Funding
This research was funded by the Military Institute of Medicine, Warsaw, Poland (grant 7/8826 project 302 to W.S.) and by Lublin Medical University, Lublin, Poland (grant number 326/19 to A.S.).
