Abstract
Cavernous angioma is an uncommon vascular malformation of the central nervous system with a tumoural aspect. Spinal cavernous angioma mainly occurs within vertebral bodies; only 3 - 5% of tumours are located entirely in the vertebral canal. This case report describes a case of cavernous angioma, originating from the nerve roots of the cauda equina at the L1 level, in a 57-year-old woman presenting with acute lower back pain. The lesion was surgically resected 6 months after symptom onset and the structural integrity of the nerve root was maintained. Histopathological examination confirmed the diagnosis of cavernous angioma. The patient experienced no postoperative neurological deficit or recurrence. The diagnosis, histopatho -logical features and surgical treatment of this case are presented, together with a literature review of clinical details and surgical procedures undertaken in cases of cavernous angioma of the cauda equina.
Introduction
Cavernous angioma of the vertebra and spinal cord is a vascular malformation with a reported incidence of 5 – 12% of all spinal vascular abnormalities.1,2 In the majority of cases, the lesion develops from the vertebral body and progresses by local invasion of the extradural tissue. 3 Only 3% of spinal cavernous angiomas are localized intradurally, 4 with 16 cases5–19 reported in the cauda equina. The current report describes a case of cavernous angioma originating from the nerve roots of the cauda equina, which presented with acute symptom onset and was successfully treated with surgery. A review of the clinical and surgical details of published cases5–19 is also provided.
Case report
A 57-year-old woman presented at the Department of Neurosurgery, Xuanwu Hospital, Capital Medical University, Beijing, China, on 7 December 2009, with acute lower back pain radiating bilaterally to the lower extremities, with greater severity on the left side. Neurological examination revealed lower-extremity weakness, and bladder and bowel dysfunction. Laboratory findings were normal. Magnetic resonance imaging (MRI) of the lumbar spine 3 days after pain onset revealed a mass at the L1 level, with heterogeneous nonenhanced T1- and T2-weighted signals, and a haematoma in the caudal portion (Fig. 1). Spinal angiography revealed no vascular abnormalities. The patient received conservative treatment (30 mg edaravone administered via intravenous injection, twice daily; 500 mg mecobalamin administered orally, three times daily; 50 mg diclofenac sodium enteric-coated tablets, administered orally three times daily, when necessary). Her symptoms gradually improved; she spent 5 days in hospital and was discharged on 50 mg diclofenac sodium enteric-coated tablets, administered orally, three times daily, when necessary, with follow-up scheduled for 6 months.
Magnetic resonance images (MRIs) of the lumbar spine of a 57-year-old woman 3 days after the onset of acute lower back pain: (A) T1-weighted image (WI), sagittal view; (B) T2 WI, sagittal view; (C) contrast-enhanced sagittal view; (D) T2 WI, coronary view. MRI revealed a mass (0.7 × 0.9 × 1.4 cm; black arrow) adherent to the nerve roots at the L1 level, with heterogeneous signal intensity in both T1 and T2 WI. A nonenhanced high-signal haematoma (white arrow), with low signal in both T1 and T2 WI, was present on the caudal side of the mass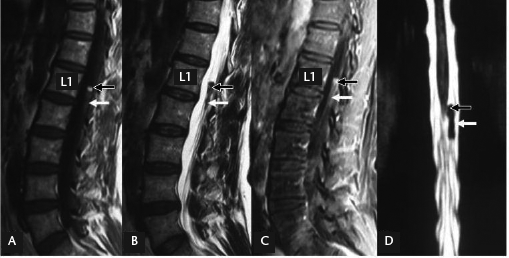
At the 6-month follow-up examination, the patient had slight hypoaesthesia of the left leg, corresponding to the L4 spinal region. A heterogeneous enhancing mass was evident at the L1 level on MRI, with a hyperintense or isointense T1-weighted signal and an isointense T2-weighted signal (Fig. 2). A black haemosiderin ring surrounding the mass was visible on T2-weighted imaging. Surgery was performed at the Department of Neurosurgery, Xuanwu Hospital, Capital Medical University, including L1 laminectomy and opening of the dura. A dark-red, well-defined mass (0.7 × 0.9 × 1.4 cm) was present at the conus medullaris nerve roots, originating on the interior side and densely adherent to adjacent nerve roots (Fig. 3). The adhesion was carefully dissected with the aid of a surgical microscope, allowing complete resection of the mass and the invaded pia mater. Histopathological examination of the mass revealed dilatated vascular channels of variable sizes, with thin or hyalinized walls, lined with flattened endothelial cells and containing blood clots. Haemosiderin-containing macrophages were noted. Scattered multifocal areas of fibrosis were present, including dilatated blood vessels and fragments of peripheral nerve fibres (Fig. 4). A diagnosis of cavernous angioma was observed. An MRI scan undertaken 3 months confirmed on the basis of these findings. No later confirmed complete removal of the mass postoperative neurological deficit was and no evidence of recurrence (Fig. 5).
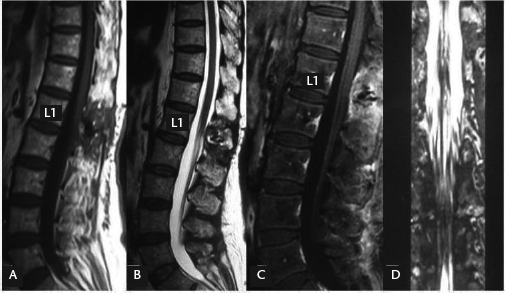
Magnetic resonance images (MRIs) of the lumbar spine of a 57-year-old woman 6 months after the onset of acute lower back pain: (A) T1-weighted image (WI), sagittal view; (B) T2 WI, sagittal view; (C) contrast-enhanced sagittal view; (D) T2 WI, coronary view. MRI revealed a mass (0.7 × 0.9 × 1.4 cm; black arrow) with an isointense/hyperintense signal in T1 WI, isointensity in T2 WI and heterogeneous contrast-enhanced haematoma absorption. A haemosiderin ring surrounded the mass Intraoperative images during L1 laminectomy and opening of the dura in a 57-year-old woman with a mass at the L1 level that was initially revealed by magnetic resonance imaging. (A) Dark-red, well-defined mass (0.7 × 0.9 × 1.4 cm; arrow) at the conus medullaris nerve roots, originating on the interior side and densely adherent to adjacent nerve roots; (B) complete resection of the mass Photomicrograph of haematoxylin and eosin-stained tissue from a 57-year-old woman, revealing variable sized dilatated vascular channels with thin or hyalinized walls, lined with flattened endothelial cells and containing blood clots. Haemosiderin-containing macrophages were noted. These histopathological findings confirmed the diagnosis of cavernous angioma. Original magnification × 100 Magnetic resonance images (MRIs) of the lumbar spine of a 57-year-old woman 3 months after complete surgical resection of a cavernous angioma, indicating absence of recurrence: (A) T1-weighted image (WI), saggital view; (B) T2 WI, sagittal view; (C) contrast enhanced sagittal view; (D) T2 WI, coronary view


Discussion
Cavernous angioma is a mulberry-shaped vascular malformation with abnormal, dilatated and packed sinusoidal vascular channels without interposed neural tissue: it is characterized by haemosiderin deposition. 14 MRI is a useful diagnostic tool for this lesion, and results in a variety of signal intensities due to differences in blood flow, haemosiderin deposition and calcification. 20 A characteristic MRI finding is a hypointense signal ring around the lesion, which occurs as a result of haemosiderin deposition. 21
We performed a systematic review of the literature in January 2011 to identify cases of cavernous angioma located in the cauda equina. The PubMed™ and Ovid databases were searched using the terms “cauda equina”, “cavernous angioma”, “cavernous hemangioma” and “cavernous malformation”. This search strategy identified 16 cases of cavernous angioma in the cauda equina (mean age at diagnosis 46.8 years; Table 1).5–19 In most cases, symptoms were related to acute bleeding and compression of the cauda equina due to haematoma formation. Symptoms included subarachnoid haemorrhage,5,7,10,11 low back pain with or without bilateral radiation to the lower extremities, hypoaesthesia and lower extremity weakness,6,8,11,13 – 15,17 – 19 and hydrocephalus.9,12 In one report, the patient was asymptomatic. 16 Symptoms may gradually improve during the natural pathological evolution of the angioma as the haematoma is absorbed, until the patient experiences another bleeding episode. 22 The patient in the current case presented with acute onset of symptoms including compression of the cauda equina. The acute onset and MRI findings suggested a diagnosis of cavernous angioma, which was confirmed by histopathological examination.
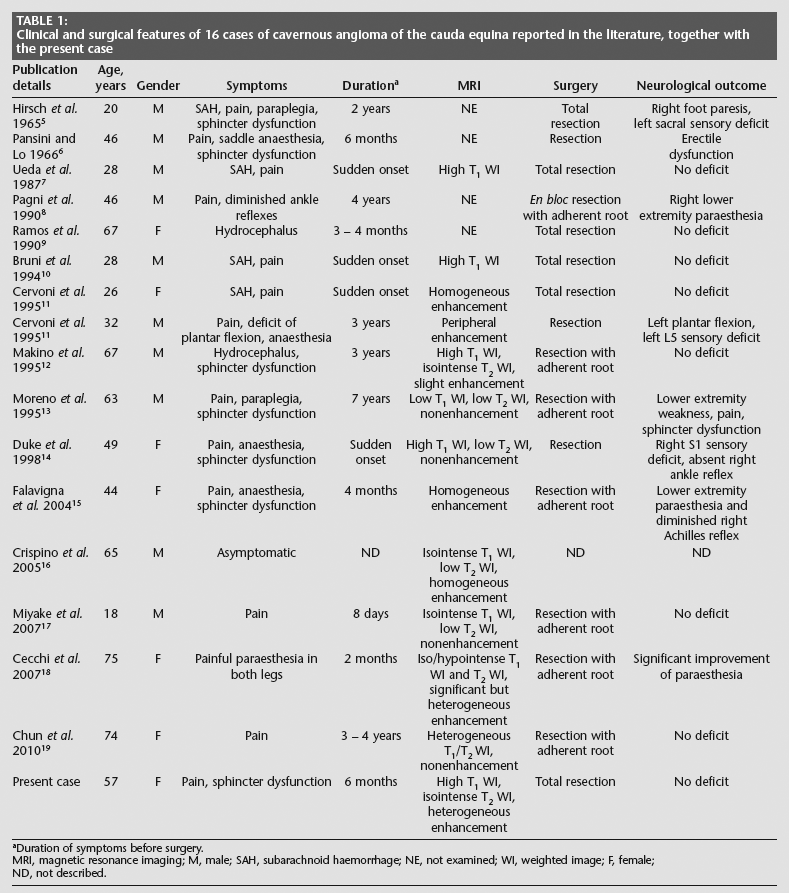
Clinical and surgical features of 16 cases of cavernous angioma of the cauda equina reported in the literature, together with the present case
_
Duration of symptoms before surgery.
MRI, magnetic resonance imaging; M, male; SAH, subarachnoid haemorrhage; NE, not examined; Wl, weighted image; F, female; ND, not described.
The optimal treatment strategy for cavernous angioma is microsurgical resection, with en bloc resection recommended as a therapeutic alternative. 23 Cavernous angioma originates from subpial vascular tissue and does not usually contain any nervous tissue. 23 Surgical procedures are technically difficult to perform, due to the formation of dense adhesions between the cavernous angioma and the nerve roots. In some cases, dissection of the nerve roots that are assumed to be the origin of the mass is unavoidable: nerve roots were resected along with the lesion in seven of the cases reviewed here,8,12,13,15,17–19 and paraesthesia or muscle weakness developed in three of these cases.8,13,15 Protection of nerve roots during surgical excision of cavernous angioma of the cauda equina is critical, in order to avoid postoperative neurological deficit. It may be preferable to perform the surgery after the acute phase, when the haemosiderin ring provides a border around the lesion that helps to avoid further damage to the cauda equina. In the present case, surgical resection of the mass was performed 6 months after symptom onset. The structural integrity of the nerve root was maintained and the patient did not experience any postoperative neurological deficit, recurrence or angioma residue.
Footnotes
The authors had no conflicts of interest to declare in relation to this article.
