Abstract
Objective:
To analyse clinical outcomes of three types of pelvic surgery for the correction of female mixed or stress urinary incontinence.
Methods:
Women who underwent surgery for urinary incontinence between January 2000 and June 2010 were included in the study (n = 268). Patients were nonrandomly assigned to undergo colporrhaphy, suspension procedure or sling procedure according to their clinical situation. Perioperative parameters were recorded. Short- (< 5 years) and long-term (5 - 10 years) success rates were determined for each group.
Results:
The short- and long-term complete cure rates were significantly lower, and the duration of catheterization significantly longer, in patients who underwent colporrhaphy compared with both other groups, but there were no significant differences between suspension or sling procedures.
Conclusion:
Sling and suspension procedures were equally effective in this study, and both were preferable to colporrhaphy.
Introduction
Urinary incontinence is defined as the objectively demonstrated involuntary passing of urine that becomes a social or a hygiene problem. 1 The prevalence of female urinary incontinence varies between populations, and has been reported to be 25 – 50% in Turkey and 42% in the UK.2–4 It is possible that the actual rate is higher than that reported, due to patients' perceptions of incontinence as a normal part of the ageing process and the failure of physicians to enquire about incontinence when they take a medical history. 5 Continence requires a combination of sufficient bladder capacity for low-pressure urine storage, a healthy urinary bladder neck, an effective distal urethral sphincter and sufficient support from pelvic floor muscles. 6 The main risk factors for urinary incontinence are increasing age, female gender, vaginal delivery, pregnancy, menopause, obesity and smoking.7–10 Stress incontinence is the most common form, and arises from intravesical pressure that exceeds urethral pressure without increased detrusor activity. 11 Mixed incontinence is a combination of stress incontinence and an overactive bladder. 12 Many surgical techniques are available for the treatment of stress incontinence. 13
This observational study examined the clinical outcomes of three different surgical techniques that are used to correct stress or mixed female urinary incontinence.
Patients and methods
Patient Population
Women admitted to the Department of Gynaecology and Obstetrics, Taksim Training and Research Hospital, Istanbul, Turkey, between January 2000 and June 2010, who underwent surgery for mixed or stress urinary incontinence, were included in this study. Incontinence was diagnosed on the basis of urinary stress and urodynamic testing (see below). Exclusion criteria were diabetes mellitus, grade 3 or 4 cystocele or rectocele (pelvic organ prolapse quantification system 14 ), and underlying neurological pathology. Patients with urinary tract infections were treated with antibiotics and were included in the study. Age, menopausal status, duration of urinary incontinence, any systemic disease and any previous operations for incontinence were recorded for each patient.
The Ethics Committee of Taksim Training and Research Hospital approved the study. Written and verbal informed consent was obtained from all patients prior to study enrolment.
Diagnosis of Incontinence
All patients underwent preoperative urinary stress, pad and urodynamic testing for the diagnosis of incontinence. In the pad test, a sanitary napkin was weighed before and after wear during 20 – 60 min of physical activity (including walking, standing up, picking up objects from the floor, coughing and running). In the urinary stress test, the patient was required to stand with a full bladder and then cough with increasing intensity; any urine leakage was recorded. Urodynamic testing was performed to determine the first sensation to void, bladder capacity, maximum detrusor pressure, strong desire to void and detrusor contractions. A flexible urinary catheter was inserted and the bladder was filled with water until the first urge to urinate. The volume of water in the bladder was measured at this point, and more water was added until involuntary urination occurred. Stress or mixed incontinence were diagnosed according to the results of these tests. 15
A pelvic examination was performed while the patient was straining, to investigate the presence of uretrocele, cystocele of the anterior wall, uterine prolapse or enterorectocele of the lateral and posterior walls.
Surgical Procedures
Patients were nonrandomly assigned to a surgical group, according to clinical findings. Patients with pelvic organ prolapse underwent anterior colporrhaphy; those who required additional abdominal surgery underwent a suspension operation (Burch, Raz or Marshall– Marchetti–Krantz retropubic urethropexy procedures 16 ); those with pure stress urinary incontinence underwent either a tension-free sling procedure (after 2005: transobturator tape [TOT], tension-free transvaginal tape [TVT] or TVT SECUR™ [Ethicon, Somerville, NJ, USA]), 17 or colporraphy or suspension procedure (before 2005). Data regarding duration of surgery, catheterization, hospital stay and postoperative residual urine volume were recorded for all patients.
Follow-Up
Patients were followed-up at 3 and 6 months after surgery, and annually thereafter. Investigations included a gynaecological examination, pelvic ultrasonography, urinary stress testing and a satisfaction questionnaire. 18 Short- (< 5 years) and long-term (5 – 10 years) success rates were estimated in each surgical group. Complete cure was defined as: (i) complete absence of incontinence; (ii) 90% satisfaction; (iii) negative urinary stress test; (iv) absence of urinary leakage during exercise (negative pad test); (v) no postoperative urinary retention. Significant cure was defined as: (i) negative urinary stress test; (ii) 75 – 89% satisfaction; (iii) no postoperative urinary retention. Surgery was considered to have failed to correct incontinence if patients did not meet these postoperative criteria. Recurrence was defined as recurrence of symptoms following significant/complete cure.
Statistical Analyses
Data were presented as mean ± SD. Between-group comparisons were made using Student's t-test, χ2-test, Kruskal–Wallis analysis of variance and descriptive statistics. Statistical analyses were performed using SPSS® version 15.0 (SPSS Inc., Chicago, IL, USA) for Windows®. A P-value < 0.05 was considered statistically significant.
Results
A total of 268 women (mean age 52.1 ± 12.6 years), undergoing scheduled corrective surgery for urinary incontinence, were recruited to the study. In total, 161 patients underwent anterior colporrhaphy, 30 underwent suspension operations (Burch n = 26, Raz n = 2, Marshall–Marchetti–Krantz n = 2), and 77 underwent sling procedures (TOT n = 48, TVT n = 22, TVT SECUR™ n = 7). Baseline demographic and clinical data are presented in Table 1. Mean age was significantly higher in the colporrhaphy group, and the duration of incontinence was significantly longer in the suspension group compared with other groups (P < 0.05 for both comparisons; Table 1).
Baseline demographic and clinical data for women who underwent corrective surgery for urinary incontinence, stratified according to surgical procedure (n = 268)
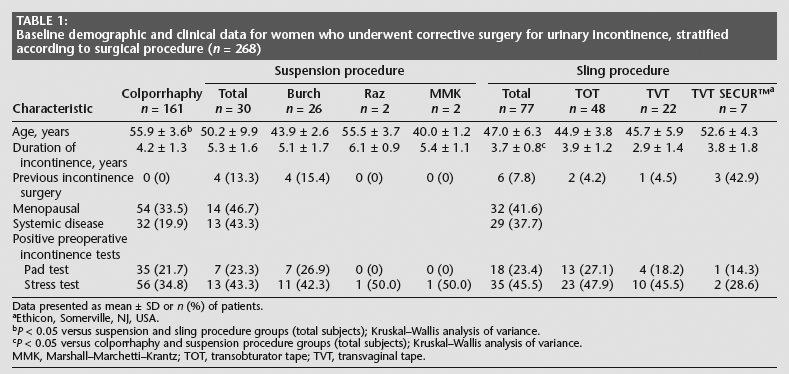
Data presented as mean ± SD or n (%) of patients.
Ethicon, Somerville, NJ, USA.
P < 0.05 versus suspension and sling procedure groups (total subjects); Kruskal-Wallis analysis of variance.
P < 0.05 versus colporrhaphy and suspension procedure groups (total subjects); Kruskal-Wallis analysis of variance.
MMK, Marshall-Marchetti-Krantz; TOT, transobturator tape; TVT, transvaginal tape.
Data regarding perioperative parameters are shown in Table 2. Durations of surgery and hospital stay were significantly longer in the suspension procedure group than in the other groups (P < 0.05). Duration of catheterization and residual urine volume were significantly greater in the colporrhaphy group than in the other groups (P < 0.05).
Perioperative data for women who underwent corrective surgery for urinary incontinence, stratified according to surgical procedure (n = 268)
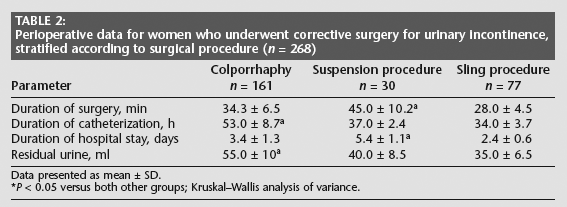

Data presented as mean ± SD.
*P < 0.05 versus both other groups; Kruskal–Wallis analysis of variance.
Short- (< 5 years) and long-term (5 – 10 years) postoperative outcome data are shown in Table 3. Colporrhaphy (group 1) was associated with significantly fewer complete cures and significantly more failures than either sling or suspension procedures, at both short- and long-term follow up (P < 0.05 for all comparisons). There were no significant differences between the sling and suspension procedures in terms of complete cure or failure rates at short- or long-term follow-up. There were no between-group differences in rates of significant cure or recurrence.
Short- (< 5 years) and long-term (5 – 10 years) postoperative outcomes in women who underwent corrective surgery for urinary incontinence, stratified according to surgical procedure
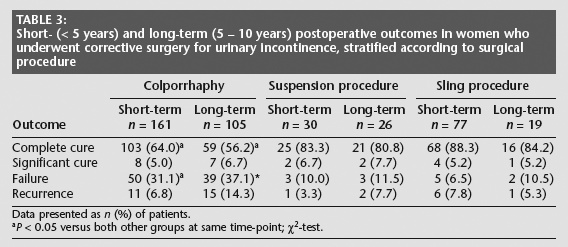
Data presented as n (%) of patients.
P < 0.05 versus both other groups at same time-point; χ2-test.
Discussion
Older age, female gender, vaginal delivery, pregnancy, menopause, obesity and smoking are the main known risk factors for urinary incontinence, which has become a common and severe health problem.7–10 The increase in incontinence with advancing age is thought to be due to impairment of the urethral muscle structure, characterized by reduction in the number of striated muscle fibres in the anterior wall of the urethra. 19 Urinary stress incontinence was reported to be 6.24-fold more common among women aged 65 years than those aged 15 – 24 years, 20 with the highest prevalence reported in women aged 51 – 60 21 or 45 – 54 years. 22 The mean age of the patients in the present study was 52.1 years, which is within the age range with the highest prevalence of incontinence. Urinary incontinence is most common during the postmenopausal period, 23 and 100/268 (37.3%) of the patients in the current study had reached the menopause.
More than 200 types of surgery have been described for the treatment of urinary stress incontinence, with varying success rates. 24 All of these surgeries aim to prevent urethral mobility during increased intra-abdominal pressure, support the suburethral fascia and allow posterior movement of the bladder floor. 25 The mean durations of surgery and hospitalization for each of the three procedures used in the current study were consistent with other reports. 26 In contrast, the duration of catheterization in suspension and sling procedures in the present study exceeded that reported in the literature. 27
The American Society of Urology Female Stress Urinary Incontinence Clinical Recommendations Panel reported success rates of 61% for anterior colporrhaphy, 84% for retropubic suspension and 83% for sling procedures, 28 which is consistent with the finding that none of the surgical techniques used for treating female urinary incontinence in the current study provided a complete cure. Success rates for anterior colporrhaphy have been reported to be 31 – 69% after 1 – 5 years and 55% after 5 – 10 years, 29 which is similar to the complete cure rates in the present study of 64.0% and 56.2% at short- and long-term follow-up, respectively.
Suspension operations (the Burch procedure) have a reported cure rate of 72%. 30 The present study found complete cure rates for suspension procedures (all types) of 83.3% and 80.8% at short- and long-term follow-up, respectively. The long-term success rate of sling procedures has been reported as 80 – 92%.31–36 Sling procedures resulted in a complete cure rate of 88.3% at short-term and 84.2% at long-term follow-up in the current study. A meta-analysis comparing the Burch suspension operation with sling procedures concluded that the long-term success rates of both techniques were similar. 37 Variations in success rates for the same surgical technique arise from modifications in surgical methods, patient selection criteria and an absence of standardized criteria for measuring postoperative success.
In conclusion, sling procedures offer similar long-term outcomes to suspension operations, but have several advantages including shorter durations of surgery and hospital stay, low complication rates and ease of application. In addition, they can be used for treating de novo urge incontinence in patients with a history of previous pelvic surgery. 38
Footnotes
The authors had no conflicts of interest to declare in relation to this article.
