Abstract
Objective:
This meta-analysis was conducted to summarize the association between the serum concentration of C-reactive protein (CRP) and chronic obstructive pulmonary disease (COPD).
Methods:
MEDLINE®, Cochrane Central Register of Controlled Trials, and EMBASE databases were searched for relevant studies. Data were extracted; pooled weighted mean differences (WMDs) and 95% confidence intervals (CIs) were calculated.
Results:
Twenty studies were selected for final inclusion in this analysis. Patients with COPD had higher serum CRP concentrations than healthy controls (WMD 4.72 mg/l, 95% CI 2.98, 6.47). In addition, patients with severe COPD had higher serum CRP concentrations than those with moderate COPD (WMD 1.26 mg/l, 95% CI 0.78, 1.73). There was no significant difference in serum CRP concentration between patients with mild and moderate COPD (WMD 0.67 mg/l, 95% CI -0.08, 1.42).
Conclusions:
This meta-analysis suggested that patients with stable COPD had higher serum CRP concentrations than healthy controls. CRP might be an indicator of disease severity in patients with COPD, thus highlighting the importance of measuring serum CRP concentrations in patients with stable COPD.
Introduction
Chronic obstructive pulmonary disease (COPD) is a leading and still growing cause of morbidity, mortality and disability. 1 Increasing evidence shows that COPD is a complex chronic inflammatory disease of the lungs, involving a number of different inflammatory cells and mediators. 2 C-reactive protein (CRP) is a marker of systemic inflammation that has been the subject of considerable research for many years. Several studies have shown that patients with COPD have higher systemic concentrations of CRP than healthy controls.3–5 Results from an epidemiological study have also shown an inverse relationship between systemic CRP concentrations and forced expiratory volume in 1 s (FEV1). 6 In addition, data indicate that serum CRP concentrations provide prognostic information beyond that achieved by traditional markers of prognosis in patients with COPD, and may enable more accurate detection of those who are at high risk of mortality.7,8 It remains uncertain whether CRP directly contributes to the accelerating decline in lung function, or whether aspects of COPD cause systemic inflammation. Conflicting information exists regarding the relationship between serum CRP concentrations and lung function over time, and available data are somewhat limited by small sample sizes.4,5 To analyse the evidence relating to these issues comprehensively, a systematic review and meta-analysis was undertaken to examine the association between serum CRP concentrations and COPD.
Materials and methods
Identification and Eligibility of Relevant Studies
A systematic search of publications listed in electronic databases (MEDLINE®, Cochrane Central Register of Controlled Trials [CENTRAL] and EMBASE), covering all papers published up to October 2011, was conducted using the following search terms: ‘C-reactive protein', ‘CRP', ‘chronic obstructive pulmonary disease', and ‘COPD', as well as combinations of these terms. There was no restriction on the language of publication. All eligible studies were retrieved and their bibliographies were checked for other relevant publications. Abstracts of relevant scientific meetings were examined, to ensure complete review of available studies.
Study Selection and Data Extraction
Two investigators (Y.Z., H.B.) identified articles eligible for further review by performing an initial screen of identified titles and abstracts. Broad inclusion criteria were used at this stage and studies could be included by either of the two investigators: papers were included if they reported the results of cross-sectional or longitudinal studies of CRP in patients with COPD. Further screening was based on a review of the full-text article. To be included at this stage, studies had to be prospective cohort or historical cohort studies, with data available for analysis. Patients with COPD had to be in a clinically stable condition. Hospital-based studies were not included because hospital-based controls may have inherent selection biases when controls were associated with the disease-related conditions. The two investigators' results were compared, with disagreements resolved by discussion and consensus.
The first author's surname and the year of publication of the article were used for identification purposes. Data concerning study design, baseline characteristics of study participants (including age, FEV1 and number of participants) were extracted.
Statistical Analyses
Weighted mean differences (WMDs) and 95% confidence intervals (CIs) were calculated for each trial using means and SDs. When only SE was reported, it was converted into SD. The
Results
The initial electronic database searches identified 992 articles. Of these, 829 were excluded after the first screening based on their abstracts or titles, leaving 163 articles for full-text review. A further 115 studies were excluded because they contained no relevant outcomes, no controls or hospital-based controls, insufficient information for analysis or they were trials involving patients in the acute stages of the disease. Following a more detailed review, 28 additional papers were excluded for the following reasons: results were given as median (range); data were not available; participants did not have COPD at baseline; studies involved patients with asthma. A total of 20 studies were selected for final inclusion in the systematic review and meta-analysis (Fig. 1).11–30
Flow diagram of the literature search and trial selection process for identifying studies that investigated the relationship between serum C-reactive protein concentrations and chronic obstructive pulmonary disease (COPD)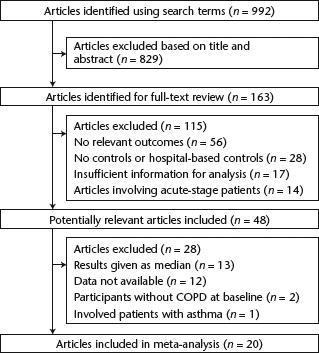
One study reported participants separately in smoking and nonsmoking groups, so each group was considered as a separate study in this meta-analysis. 11 Six studies presented the serum CRP concentration according to COPD severity and the closest to the value of the controls was selected, to avoid an overestimation of the true effect.15–18,22,27 Three studies contained both smoking and nonsmoking controls.15,19,23 In order to take into consideration that most patients with COPD were smokers, controls who were smokers were selected to reduce any bias.
Three of the 20 studies included did not report data for healthy controls. Thus, a meta-analysis of 17 studies demonstrated that patients with COPD had higher serum concentrations of CRP than control subjects without COPD (WMD = 4.72 mg/l, 95% CI 2.98, 6.47,
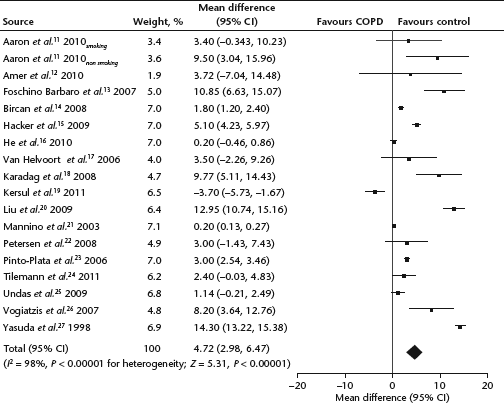
Only five studies evaluated CRP levels by severity of COPD,16,21,28–30 of which only four showed data comparing mild and moderate COPD.16,21,29,30 Compared with moderate COPD, severe COPD was associated with a higher serum CRP concentration (WMD = 1.26 mg/l, 95% CI 0.78, 1.73,
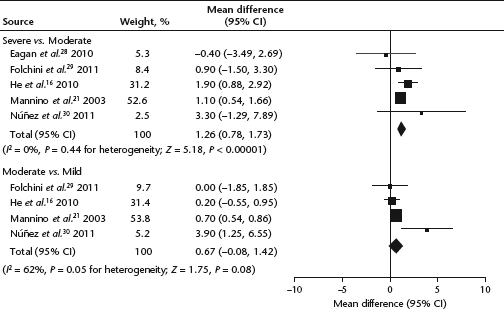
A sensitivity analysis was performed to explore the heterogeneity among studies: this was conducted by sequential omission of individual studies in each group. The pooled result was not significantly affected by any single study in the analysis of the association between serum CRP concentration and COPD. Náñez
Discussion
To our knowledge, the present study is the most comprehensive meta-analysis to assess the relationship between serum CRP concentrations and stable COPD. This meta-analysis showed that patients with COPD had higher serum CRP concentrations than healthy controls, and that the serum CRP concentration might be an indicator of disease severity.
The pooled analysis of 17 studies showed that patients with stable COPD had higher serum CRP concentrations than control subjects. There was, however, evidence of heterogeneity between the studies included in this analysis. A sensitivity analysis was conducted and the pooled result was not significantly affected by any single study. Reasons for the heterogeneity were unclear. It might be due to methodological differences between the studies, particularly with regard to the populations that were included and the severity of the COPD that was studied.
An interesting finding was that severe COPD was associated with a higher serum CRP concentration than moderate COPD. There was, however, no significant difference between patients with moderate and mild COPD, suggesting that the inflammatory process might be self-limiting and reversible in the early disease stages.
18
As the disease progresses, pulmonary inflammation becomes persistent and it produces substantial extrapulmonary manifestations, which might lead to more pronounced increases in serum CRP concentrations in patients with COPD who have severe airflow obstruction. Sensitivity analysis showed the study of Núñez
Currently, the serum CRP concentration is usually only determined if an exacerbation of COPD is suspected. The present meta-analysis has several clinical implications. As high-sensitivity CRP assays are inexpensive and convenient, clinicians and researchers should measure serum CRP concentrations in patients with stable COPD. The present study showed that a high serum CRP concentration may be a marker of disease progression. Such evidence might help physicians to stratify patients with COPD in terms of their risk of disease progression, such that they can implement an early interventional strategy to modify that risk.
There were certain limitations to the present study. First, as a meta-analysis, it was not possible to assess the impact of confounding factors (such as smoking, age, sex and other patient characteristics) and incorporate them into the analysis. Secondly, in some studies, the sample sizes were relatively small, with not enough statistical power to explore the real association. Finally, the trials included in this analysis were conducted in different institutions, therefore methods used to measure serum CRP concentrations may have varied, which could have biased the results.
In conclusion, this current meta-analysis suggested that patients with stable COPD had higher serum CRP concentrations than healthy controls, and that the serum CRP concentration might be an indicator of disease severity. These findings highlight the importance of employing high-sensitivity CRP assays in patients with stable COPD.
Footnotes
Acknowledgements
We are extremely grateful to Dr Fen Lan of the Department of Respiratory Medicine, Second Affiliated Hospital, College of Medicine, Zhejiang University, Hangzhou, China for her review and scientific editing of the manuscript. The Screening and Test Evaluation Programme is supported by the Clinical Academic Key Funds of the Chinese Ministry of Health (No. 2007353) and the Special Funds for Scientific Research on Public Causes of the Chinese Ministry of Health (No. 201002008).
The authors had no conflicts of interest to declare in relation to this article.
