Abstract
Background:
Despite evidence demonstrating the utility of using Person-Centred Outcome Measures within palliative care settings, implementing them into routine practice is challenging. Most research has described barriers to, without explaining the causal mechanisms underpinning, implementation. Implementation theories explain how, why, and in which contexts specific relationships between barriers/enablers might improve implementation effectiveness but have rarely been used in palliative care outcomes research.
Aim:
To use Normalisation Process Theory to understand and explain the causal mechanisms that underpin successful implementation of Person-Centred Outcome Measures within palliative care.
Design:
Exploratory qualitative study. Data collected through semi-structured interviews and analysed using a Framework approach.
Setting/participants:
63 healthcare professionals, across 11 specialist palliative care services, were purposefully sampled by role, experience, seniority, and settings (inpatient, outpatient/day therapy, home-based/community).
Results:
Seven main themes were developed, representing the causal mechanisms and relationships underpinning successful implementation of outcome measures into routine practice. Themes were: Subjectivity of measures; Frequency and version of Integrated Palliative care Outcome Scale; Training, education, and peer support; Building and sustaining community engagement; Electronic system readiness; The art of communication; Reinforcing use through demonstrating value.
Conclusions:
Relationships influencing implementation resided at individual and organisational levels. Addressing these factors is key to driving the implementation of outcome measures into routine practice so that those using palliative care services can benefit from the systematic identification, management, and measurement of their symptoms and concerns. We provide key questions that are essential for those implementing and using outcome measures to consider in order to facilitate the integration of outcome measures into routine palliative care practice.
Routine use of Person-Centred Outcome Measures improves health status and well-being in patients through enhancing quality of care and facilitating healthcare professionals in addressing symptoms and concerns that are most important to patients
Outcome measures are used inconsistently (if at all) in routine palliative care practice
Barriers to the implementation of outcome measures into routine practice include lack of knowledge, time, and feedback, and the absence of champions driving change
Understanding of distinct implementation challenges for specific outcome measures and how these may impact quality and safety of care
A theoretically informed explanation of the causal mechanisms behind how individual and team interactions within different palliative care settings impact on the implementation of outcome measures
A key set of implementation questions for leaders and users to consider before and during the implementation of outcome measures into routine palliative care
Accessible I.T. infrastructure for inputting, viewing, sharing, and extracting outcomes data is an essential but not sufficient condition for the implementation of outcome measures
‘Buy-in’ to implementation requires the involvement of all team members in the implementation process and the ‘normalisation’ of outcome measures into routine organisational practices
The use of appropriate theory can provide insight into complex implementation challenges where individuals and teams interact within organisations and wider systems of care
Introduction
Measuring outcomes is an integral part of evidence-based practice because it provides healthcare professionals with the information that they need to make decisions regarding diagnosis, prognosis, and the evaluation of clinical interventions.1,2 Person-centred outcome measures (herein referred to as ‘outcome measures’) are standardised and validated questionnaires that provide healthcare professionals with information of a person’s own perception of their well-being. 3 Because many patients with advanced disease may have impaired cognition, or may be too unwell to complete outcome measures, 4 they also include proxy-reported ratings which are reported by others. 3
There is strong evidence for the utility of outcome measures within palliative care settings in: (a) improving communication between patients and clinicians; (b) identifying unrecognised needs and monitoring symptoms; (c) increasing the amount of clinical action taken; (d) improving outcomes through person-centred care; and (e) demonstrating the value of palliative care.3,5–9 Because they help to improve patient outcomes, their implementation into routine practice has been advocated by the European Association for Palliative Care Task Force on Outcome Measurement. 10 Despite these recommendations, outcome measures are still used inconsistently (if at all) in palliative care settings. Common challenges to routine use include time constraints, lack of training/knowledge, tools being perceived as burdensome, negative attitudes, availability of champions to drive change, and fear of added work.1,8,11–14 This evidence, however, has not been translated into meaningful changes to clinical practice.
Implementation science – the systematic study of methods to promote the integration of evidence-based practices/interventions into routine practice15,16 – presents a potential solution by providing a menu of theories and determinant frameworks to facilitate the implementation of outcome measures. 16 Determinant frameworks – such as the Consolidated Framework for Implementation Research and Promoting Action on Research Implementation in Health Services – have been used in palliative care research to describe the barriers/enablers to using outcome measures.1,13 However, these frameworks are limited to description and categorisation rather than delivering the ‘explanatory power’ that is crucial in specifying the causal mechanisms that underpin implementation. 15 This makes it difficult to explain how and why implementation is likely to succeed or fail ‘thus restrain[s] opportunities to identify factors that predict the likelihood of implementation success and develop better strategies to achieve more successful implementation’. 15 Consequently, there has been calls for theoretical development in outcome measure implementation within palliative care.8,10,16–18
Implementation theories go beyond description by providing comprehensive and generalisable explanations of individual, organisational, and structural mechanisms underpinning implementation, including
Whilst implementation theories have proved useful in implementing outcome measures in other fields,
16
they have not been used in palliative care outcomes research. In this study, our
A description of the different Normalisation Process Theory constructs that underpin the implementation of person-centred outcome measures into routine practice. Derived from May (2013). 22

Methods
Design
An exploratory design grounded in an interpretive paradigm. 23 Thus, we sought to explore the mechanisms underpinning successful implementation, whilst appreciating that the knowledge developed was subjective and co-constructed between researchers and participants within particular socio-cultural contexts.
Participants and setting
This was a multi-site project conducted with 11 services delivering specialist palliative care in Yorkshire, England. Participants were recruited using a purposive maximum variation sampling technique 24 to reflect variations in age, experience, role, and settings (inpatient, outpatient/day therapy, home-based/community). Participants were approached via email and provided with a participant information sheet. Written informed consent was obtained. Recruitment and data collection took place between May-Dec 2019.
Data collection
Single, face-to-face semi-structured interviews were conducted by one of three researchers with prior interviewing experience [AB (male, research fellow), MS (female, research nurse), MM (female, PhD candidate)] within participants’ workplaces. The interview guide (supplementary file 1) was developed through a literature search seeking the most common challenges regarding the implementation of outcome measures in healthcare settings. This included questions on their collection, transfer, and feedback, and how these issues may be addressed to aid implementation. Data collection continued until the research team were confident that data saturation 25 had been achieved. Interviews were audio recorded, anonymised, and transcribed verbatim.
Analysis
Interview data were analysed deductively using a thematic Framework approach26,27 whereby data was reviewed, and themes were developed, in correspondence to the different components of Normalisation Process Theory. The Framework approach was adopted because it allows for iteration between raw data and developing findings to preserve the context of participants’ experiences 26 but has a greater emphasis than thematic analysis on making the process of data analysis transparent.27,28 Analysis was conducted in NVivo (version 12) and entailed seven, interconnected steps: (1) transcription; (2) familiarisation; (3) coding; (4) developing an analytic framework; (5) indexing; (6) charting; and (7) interpreting the data. Whilst themes are presented under the different constructs of Normalisation Process Theory, the boundaries between these were porous, meaning that some constructs crossed over and interacted with one another.
Quality
A relativist approach to judging quality 29 was adopted. This entailed using lists of criteria on what constitutes high quality qualitative research30,31 as a starting point, and then selecting criteria that was appropriate for the context, purposes, and methodology of this study. A list of selected criteria and how these were fulfilled can be seen in Table 2.
List of quality criteria selected and how it was fulfilled in this study.

Ethical approval
Approved by Hull York Medical School Ethical Committee [19 15, 26/03/2019].
Results
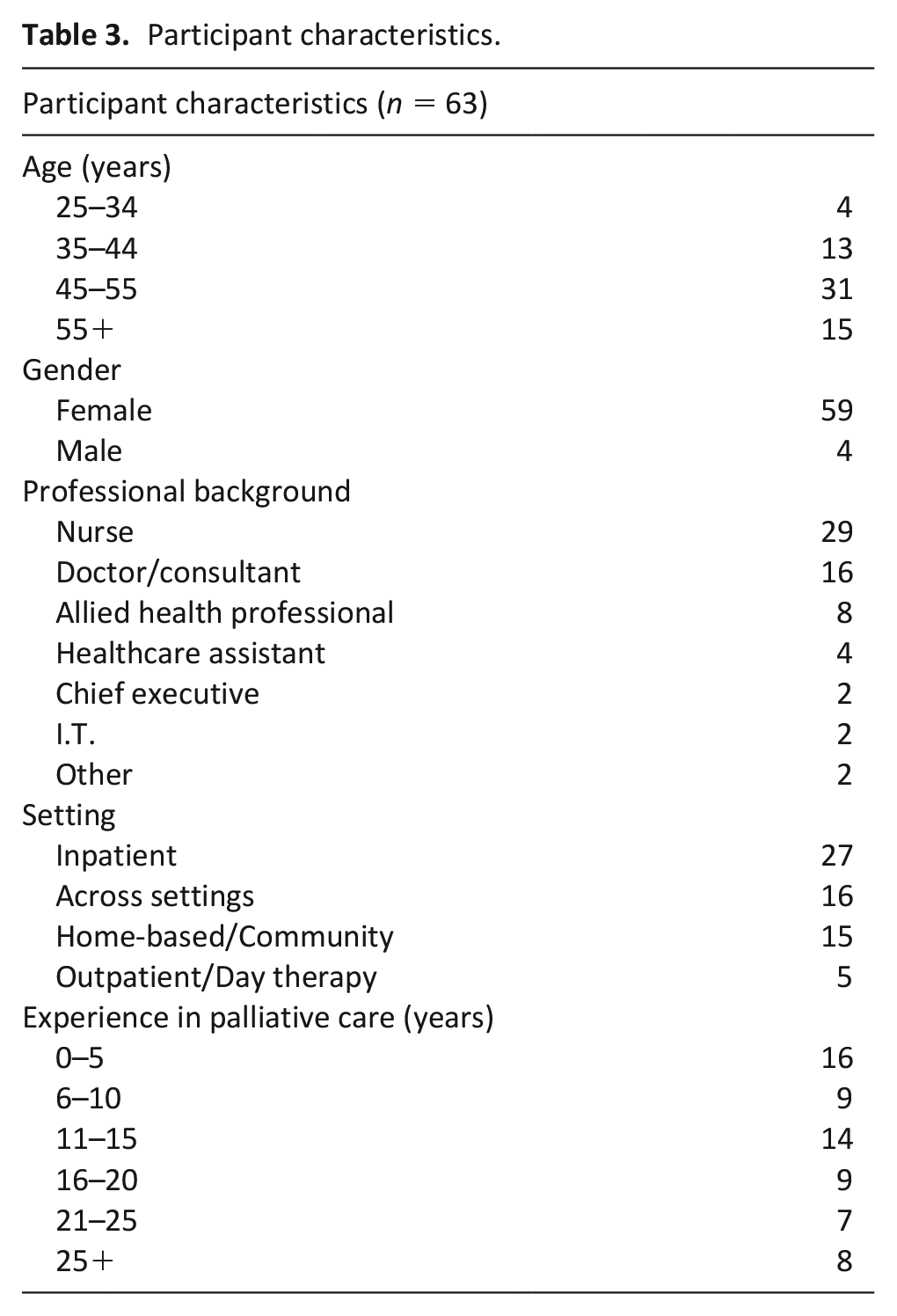
A total of 63 participants were recruited (see Table 3). Interviews lasted on average 37 minutes.
Participant characteristics.
Seven themes (and seven sub-themes) encompassed within different, interconnecting constructs of Normalisa-tion Process Theory were identified as important processes in the implementation of outcome measures (see Figure 1).
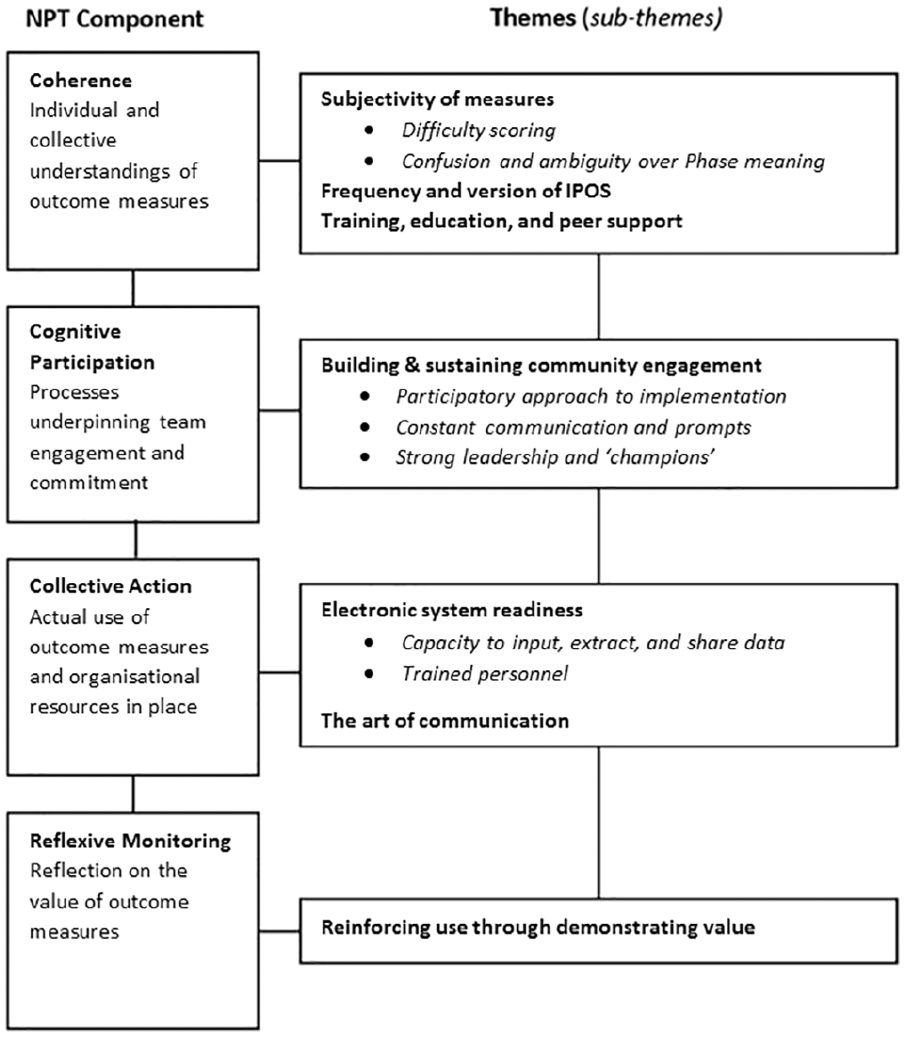
Main themes and sub-themes in relation to Normalisation Process Theory constructs.
Coherence
Three themes represent how
Theme 1: Subjectivity of measures
Sub-theme 1: Difficulty scoring
Many participants commented on how they perceived outcome measures to be inherently subjective which made confidently and consistently scoring patients difficult:
Participants also found scoring psychosocial items on the Integrated Palliative care Outcome Scale difficult. The ‘at peace’ item was perceived as especially difficult to score because participants felt as though staff and patients found it hard to understand what was meant by this question:
Subjectivities over scoring interrupted implementation because instead of measures becoming an ‘invisible’ process completed with little thought, participants spent time deliberating over, as opposed to efficiently using, the measures.
Sub-theme 2: Confusion and ambiguity over Phase of Illness meaning
The meaning of the Palliative Phase of Illness measure caused many participants confusion. This was because the meanings of terms within this measure were different within palliative care compared to other medical settings:
This was problematic to successful implementation because it meant that whilst this measure was being used throughout practice, it was often being used incorrectly.
Theme 2: Frequency and version of Integrated Palliative care Outcome Scale
Some participants reported that their ability to collect full Integrated Palliative care Outcome Scale (IPOS) data was thwarted by poor understandings of the frequency through which to use it. These misunderstandings led to excessive and unnecessary assessment that overburdened already unwell and fatigued patients, causing them to disengage from completing measures:
Misunderstandings of which version of IPOS to use was also problematic. Use of patient reported IPOS when the staff version might have been better meant that some patients were asked to continuously reflect on symptoms and concerns that were not improving, making them feel emotionally distressed:
Whilst this theme highlights challenges to implementing IPOS, it also raises concerns about how poor knowledge of outcome measures may lead to them being used in ways that compromise the quality and safety of care delivered to patients.
Theme 3: Training, education, and peer support
In addressing subjectivity of measures, participants spoke about the importance of training and education. This was so that they clearly understood what the measures were, their value, and how to collect data in clinically meaningful ways:
Participants also valued peer support in which more experienced team members shared their skills and knowledge of outcome measures to facilitate their confident and consistent use by others:
Cognitive participation
One theme, comprised of three sub-themes, represented the processes that underpinned
Theme 4: Building and sustaining community engagement
Sub-theme 1: Participatory approach to implementation
If teams were to embrace change, it was crucial that implementation came from the bottom up, allowing those who used outcome measures the agency to shape how they were being implemented:
This linked to participants’ coherence of measures because involvement in implementation helped them to understand how using outcome measures formed a legitimate part of their role. It also allowed them to feel a sense of responsibility and ownership by feeling a valid part of something that was meaningful to patient care:
Sub-theme 2: Constant communication and prompts
Participants spoke about the importance of constantly communicating with outcome measures through using them to drive discussions and decisions regarding patient care. This was so that the measures were continuously in view and people saw how they connected to their roles daily:
Over time, this helped to normalise their consistent collection and use until they became so ingrained that it was something that participants did not need to think about:
Sub-theme 3: Strong leadership and ‘champions’
Participants perceived that leaders were important in introducing and driving the use of outcome measures. These people were passionate and experienced in using these measures, and were integral in ensuring that the measures were understood and used in everyday discussions:
Collective action
Two themes represent the ways in which participants’
Theme 5: Electronic system readiness
Three sub-themes demonstrate how having appropriate electronic systems in place was a linchpin to implementation. Electronic system readiness directly connected to how participants appraised the value of outcome measures (reflexive monitoring) and, in turn, their coherence of why they were using them. This was because efficient electronic systems were key to feeding back outcomes data to staff who collected them. Where this was possible, healthcare professionals were more likely to understand the clinical utility of outcome measures, thus appraise them as useful tools within clinical practice.
Sub-theme 1: Capacity to input, extract, and share data
Having an electronic system with the capability of inputting, viewing, sharing, and extracting data was ‘
In organisations where this was not the case, the implementation of outcome measures was severely disrupted, and in extreme instances, abandoned. This was because many participants questioned the value of, and time that it took to collect, data if this information sat dormant in electronic systems without being used for patient benefit:
Sub-theme 2: Trained personnel
Having people within organisations that had the skills and knowledge to tailor electronic systems to local needs, resources, and structures, alongside supporting the workforce’s effective use of these systems, was important to implementation:
Theme 6: The art of communication
Participants spoke about how the communication skills required to effectively collect IPOS data were akin to an art form in which patients should be made to feel empowered and listened to:
This art entailed being able to ‘
However, many participants recognised that because of the intimate and unpredictable nature of the psychosocial and spiritual questions included in IPOS, that collecting full data was sometimes thwarted because it led to ‘
Reflexive monitoring
One theme captures the ways in which participants
Theme 7: Reinforcing use through demonstrating value
Crucial to implementation was that the use of outcome measure was reinforced by providing those who collected data with real-life feedback of how they were being used to improve patient care and outcomes:
Without feedback on their clinical utility, measures were viewed as a pointless exercise. This undermined staff buy-in required for successful implementation because it led to ambivalence and loss of motivation in accurately collecting outcomes data:
Discussion
The main findings of this study may be understood through the constructs of Normalisation Process Theory. For coherence, it was important that those using outcome measures understood their value/how to use them appropriately and were provided with up-to-date training within their organisation. For cognitive participation, it was key that organisations built practices around outcome measures through adopting a participatory approach to implementation and having strong leaders/champions driving their integration into practice. Within collective action, it was key that there was efficient electronic infrastructure in place to operationalise outcomes and that healthcare professionals were able to communicate effectively using the measures with patients. Finally, within reflexive monitoring, it was crucial that those using the measures were provided with regular, meaningful feedback of data. These findings corroborate others that have reported similar challenges to implementing outcome measures in routine palliative care practice across Europe.1,8,11–14,17,32,33
What this study adds
This study contributes to theoretical development in this area by going beyond descriptive lists of barriers/challenges/enablers to implementation by drawing on Normalisation Process Theory to explain the causal mechanisms/relationships through which individual and structural challenges impact implementation (see Figure 2) and proposing theoretically-informed questions to address these challenges (see Table 4). Through demonstrating the value of Normalisation Process Theory as a robust theory for explaining the implementation of outcome measures in palliative care, this study also adds knowledge on implementation, acting on recent calls to ‘advance our collective understanding of how, why, and in what circumstances [implementation science] frameworks and implementation strategies [may] produce successful implementation’. 16
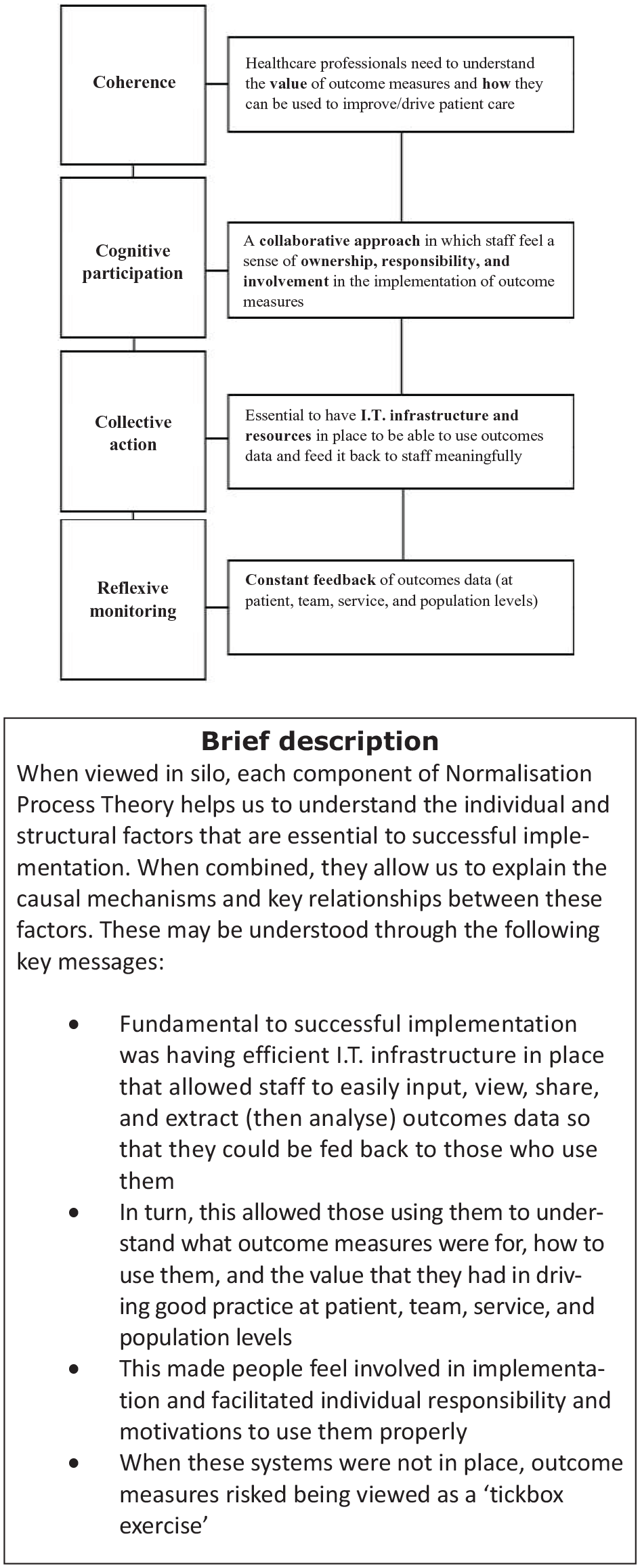
A summary explanation of the key relationships and causal mechanisms between the different Normalisation Process Theory constructs in the successful implementation of outcome measures into routine practice.
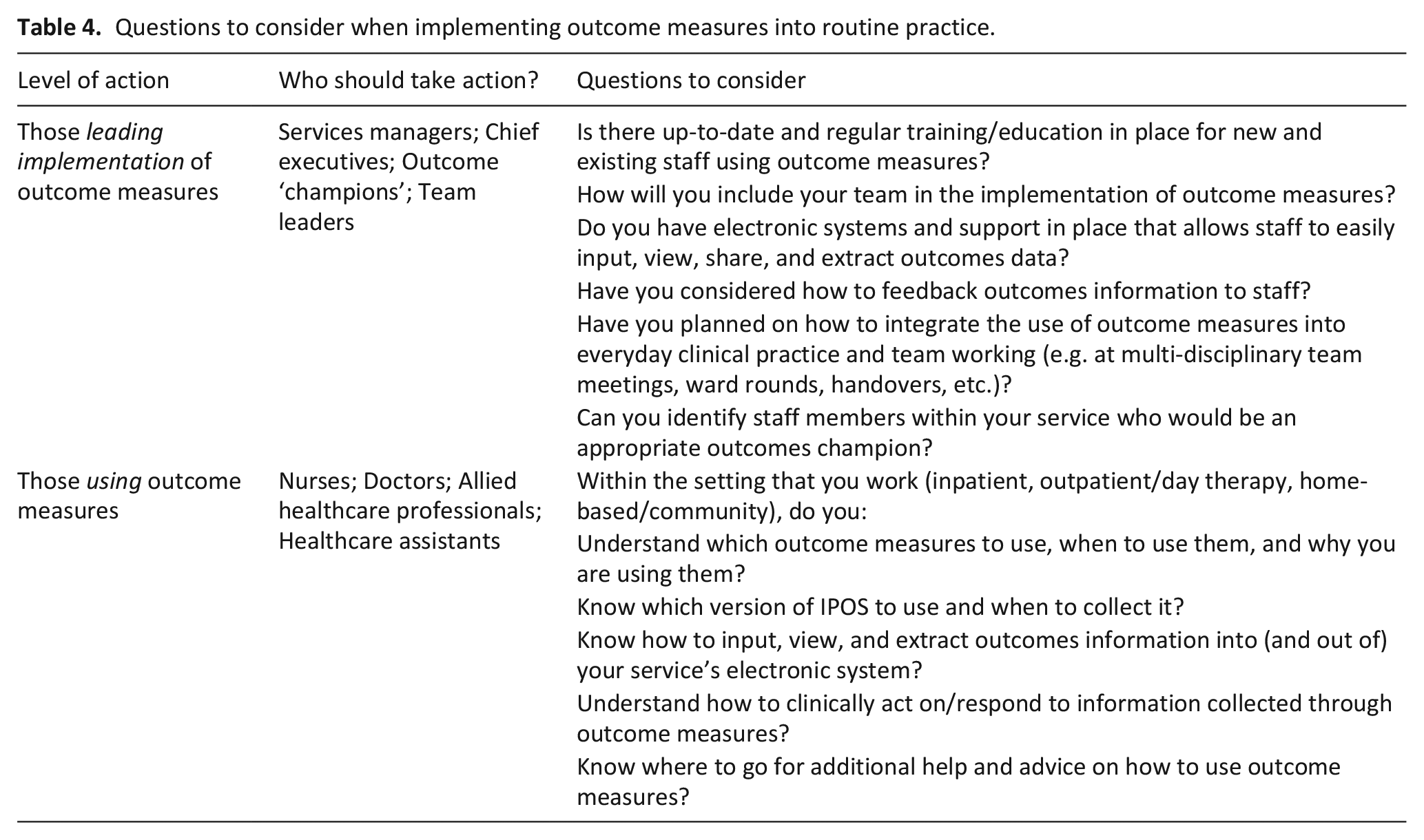
Questions to consider when implementing outcome measures into routine practice.
Our data also presents novel contributions regarding the measure-specific challenges that healthcare professionals experience when using outcome measures, thus challenging a recent systematic review that argued ‘challenges in implementing [outcome measures] are not exclusive to the characteristic of the chosen measure’. 1 Measure-specific challenges included confusion and ambiguity with regards to using Palliative Phase of Illness, and the art of communication required to effectively collect IPOS information. Furthermore, we also demonstrated how misunderstandings of which IPOS version to use and when disrupted implementation and raised concerns about the ways in which excessive person-centred assessments may compromise the quality and safety of care for patients. These issues need to be considered when planning for safe implementation of outcome measures into routine practice.
Implications for research and clinical practice
Through interpreting the findings of this study, we have proposed a set of questions – based on Normalisation Process Theory – that professionals who are leading rollout and using outcome measures should consider before and during implementation (Table 4). Critical application of these questions may potentially be transferable to healthcare settings outside of palliative care that are seeking to implement outcome measures into routine practice.
Strengths and limitations
A strength of this study is that it was a multi-site project conducted across an entire geographical region. Purposive sampling was used to recruit a diverse range of participants that were broadly representative of the palliative care workforce and settings in which specialist palliative care is delivered. This may allow naturalistic generalisations 34 to be made for healthcare professionals using outcome measures within a palliative care context. That is, the findings of this study are likely to resonate with the personal experiences of staff using outcome measures within palliative care. Potential limitations of this study are that it relied on one-off interviews that may not have been able to capture how the processes of implementing outcome measures identified in this study may have changed over time. We also did not explore patients’ perspectives regarding how the implementation of outcome measures impacted their experiences of palliative care. Finally, we found that some concepts included within Normalisation Process Theory overlapped, making these more difficult to use.
Future directions
This study highlights the mechanisms underpinning the successful implementation of outcome measures into routine palliative care and adds to the development of strategies to overcome implementation challenges. How effective these interventions are at facilitating implementation still needs to be established, and future work using process evaluations will be beneficial in assessing and understanding which implementation strategies are most effective for integrating outcome measures into practice.
Conclusion
The aim of this study was to understand and explain the processes that underpin successful implementation of outcome measures within a palliative care context. Factors influencing implementation resided at individual and organisational levels. For individuals, it was important that staff were confident in their understanding of which measures to use, when, how, and why, and felt included in the implementation process. At an organisational level, important factors to implementation included: ensuring up-to-date and regular training for staff, that effective electronic systems were in place to input, view, and extract outcome measures, everyday practice was built around their use, and that staff using measures were provided with timely feedback. Addressing these factors is key to driving the implementation and sustained use of outcome measures by facilitating behaviour change in staff and creating environments in which their effective and safe use is possible. We provide key questions that are essential to consider in dealing with these issues.
Supplemental Material
sj-pdf-1-pmj-10.1177_0269216320972049 – Supplemental material for Implementing person-centred outcome measures in palliative care: An exploratory qualitative study using Normalisation Process Theory to understand processes and context
Supplemental material, sj-pdf-1-pmj-10.1177_0269216320972049 for Implementing person-centred outcome measures in palliative care: An exploratory qualitative study using Normalisation Process Theory to understand processes and context by Andy Bradshaw, Martina Santarelli, Malene Mulderrig, Assem Khamis, Kathryn Sartain, Jason W. Boland, Michael I. Bennett, Miriam Johnson, Mark Pearson and Fliss E. M. Murtagh in Palliative Medicine
Footnotes
Acknowledgements
The authors would like to thank Rebecca Corridan for proof-reading and formatting.
Author contributions
A.B.: conceptualisation and design, data collection, analysis, interpretation of data, led the writing process and drafted original article and reviewing for critically important content. M.S.: data collection, interpretation of data and reviewing for critically important content. M.M.: data collection. A.K.: interpretation of data and reviewing for critically important content. K.S.: interpretation of data and reviewing for critically important content. J.B.: interpretation of data and reviewing for critically important content. M.B.: interpretation of data and reviewing for critically important content. M.J.: interpretation of data and reviewing for critically important content. M.P.: conceptualisation and design; interpretation of data and reviewing for critically important content. F.E.M.: conceptualisation and design, interpretation of data and reviewing for critically important content. All authors take responsibility for appropriate portions of the content of this article
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by Yorkshire Cancer Research through the RESOLVE Programme [L412].
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
