Abstract
Objectives
To evaluate the physical and functional outcomes of the ‘Ending Pyjama Paralysis’ intervention in an inpatient geriatric rehabilitation unit.
Design
Quasi-experimental mixed-methods design nested within the ‘REStORing health of acutely unwell adulTs’ (RESORT) prospective, observational, longitudinal cohort of geriatric rehabilitation inpatients study.
Setting
Geriatric rehabilitation wards in a major metropolitan public hospital between June 2019 and March 2020.
Intervention
The ‘Ending Pyjama Paralysis’ movement originated in the UK. Its aim was to encourage patients to ‘Get up, Get dressed and Get moving’ to reduce hospital-associated functional decline. However, the physical and functional benefits of this campaign have not yet been evaluated. The ‘Ending Pyjama Paralysis’ was adopted as an integrated intervention on two out of four geriatric rehabilitation wards. The two control wards received usual care.
Main Measures
Physical measures included the Short Physical Performance Battery, and functional measures included the Katz Index of Independence in Activities of Daily Living and Lawton and Brody’s Instrumental Activities of Daily Living, which were completed on admission and discharge. A linear mixed-effects model was used to analyse the results.
Results
A total of 833 admissions were included in this study. Of these, 512 patients were in the control group, and 321 were in the intervention group. There were no significant differences in both physical and functional measures between the intervention and control groups.
Conclusion
The ‘Ending Pyjama Paralysis’ campaign did not result in enhanced functional or physical benefits in geriatric rehabilitation inpatients in this setting when applied in addition to usual care.
Keywords
Introduction
Physical inactivity and sedentary behaviour are known to be high during hospitalisation, which contributes to functional decline.1–3 Approximately 30% of older adults do not regain their premorbid level of independence completing activities of daily living (ADL) on discharge from an acute hospital setting.4–6 Patients who lose ADL independence during hospitalisation have a higher mortality rate post-discharge.7,8 An older person's ability to continue premorbid routines, such as showering and dressing themselves, is reduced in the hospital due to the limitations inherent in a hospital environment. 4 This is coupled with patients' perception that ‘bed rest’ can be an important part of their recovery during hospitalisation. These factors contribute to overall functional decline.4,5,9–12
The ‘Ending Pyjama Paralysis’ movement originated in the UK and aimed to reduce functional decline by empowering patients in hospitals to move away from the ‘sick role’ and become more active partners in their own recovery. 13 The guiding principles of this movement are to actively encourage patients to get dressed in their day clothes and spend more time out of bed. Patients were also encouraged to be more physically active during their hospitalisation.13,14 This was achieved through the implementation of various non-standardised local initiatives and driven largely via the social media campaign #endpyjamaparalysis. The movement was premised on enabling a cultural shift in both staff and patients’ perceptions of hospitalisation, and would not require additional staffing or material resources. To date, there have been no studies exploring the impact of this campaign on a patient's physical and functional outcomes in geriatric rehabilitation patients.
The aim of this study was to evaluate whether the ‘Ending Pyjama Paralysis’ intervention improved the physical and functional outcomes in an inpatient geriatric rehabilitation unit, when applied in addition to usual care.
Methods
This study draws from data collected in the REStORing health of acutely unwell adulTs (RESORT) longitudinal observational study which has been reported on previously..3,6 The data from this study was not pooled in analysis of potentially dependent variables in publications using the RESORT database. Conducted at the geriatric inpatient rehabilitation unit of the Royal Melbourne Hospital in Victoria, Australia, participants included all eligible patients who were admitted from 3 June 2019 to 15 March 2020. Inclusion criteria were all inpatients who were medically stable, whilst those with a terminal illness or patients who were bedbound were excluded. No other exclusion criteria were applied. Written informed consent was obtained from all patients or their carers. Each ward has 20–25 beds with similar nursing ratios of 1:4. Patients are admitted according to bed availability at the time at which they were deemed suitable for transfer from the acute care setting to the geriatric rehabilitation wards.
The ‘Ending Pyjama Paralysis’ campaign was adopted as an integrated model of care in a prospective quasi-experimental study design on two out of four geriatric rehabilitation wards. This study was approved by the Melbourne Health Human Research Ethics Committee (HREC/17/MH/103) with all ethical guidelines followed in full accordance with the Declaration of Helsinki. 15
The two control wards received usual care, which consists of a multidisciplinary approach including medical, nursing and allied health interventions to address patient goals and needs. Most patients receive daily allied health input to improve mobility and function, in both individual and group settings. The multidisciplinary team works collectively to support patients in attaining their goals.
Patients in the intervention wards received the ‘Ending Pyjama Paralysis’ initiatives in addition to standard/usual care. No other interventions were introduced during this time that could bias the results.
Approval was obtained by senior management, and key medical, nursing and allied health stakeholders to ensure support for the intervention would be promoted at all levels of staffing. Following this, an intensive ‘onboarding’ process was completed with nursing and allied health staff on the intervention wards. This included 30-minute education sessions run by the allied health staff who formed the project team. These were held twice per week per ward in the three weeks leading up to project commencement, outlining the purpose and goals of the project in a visual presentation format, providing an opportunity for questions and answers relating to project implementation. Support was obtained from the Nurse Clinical Educators to ensure an additional promotion of the campaign was integrated into their support of nursing staff on wards. Weekly meetings with nurse unit managers in the intervention wards were held to troubleshoot issues such as non-compliance with the campaign by patients or nursing staff. Members of the project team (allied health staff from intervention wards) also attended nursing ‘huddles’ three times per week in the first month of the project rollout to respond to any queries or questions that staff had.
Prior to the intervention commencing, 20 patients were interviewed regarding their perceptions of barriers to physical activity in hospital using surveys on both intervention and control wards. This information was used to develop patient information brochures that outlined the key principles of the ‘End Pyjama Paralysis’ movement, including the expectation that patients wear their own clothing and footwear during the day. These brochures were translated into the three most common languages spoken by patients in the hospital (Greek, Italian, and Arabic) and distributed to patients within 48 h of their admission to the hospital. Various posters were also developed and prominently displayed on the intervention wards, outlining the key message of the campaign. All promotional material used the catchphrase: ‘Get up, Get dressed, Get moving’.
Changes were introduced to the intervention wards in stages to consolidate practice change across the staff. This approach was developed as part of the co-design process with key stakeholders. Given a significant practice change in the wards, weekly meetings were held to evaluate the uptake of each stage of the intervention and to determine readiness to implement the next component. All changes were designed to ensure successful uptake within existing ward processes and staffing resources. The resources for the mobilisation program was adapted from the MOVE Canada ‘Mobilisation of vulnerable older adults’, 16 Johns Hopkins Activity And Mobilization (AMP) promotional tools and resources 17 and based on the recommendations outlined in the American Geriatrics Society (AGS) white paper on hospital mobilisation. 18 The program was designed to engage all relevant stakeholders in the mobilisation strategy, including staff, patients and their families/carers. All patients who met the inclusion criteria were orientated to the program within 48 h of admission.
A mobility chart was introduced and displayed in all patient rooms and communal areas. This was based on a ‘traffic light’ system, which prescribed generic physical activity to the patient in accordance with their functional level, as assessed by a therapist on the ward. Patients who were able to mobilise were encouraged to do so three times per day in addition to standard therapy, with or without assistance, depending on their level of independence, as assessed by the ward physiotherapist. Prior to introduction of the ‘Ending Pyjama Paralysis’ campaign, inpatients were not encouraged to mobilise outside scheduled therapy hours.
A ‘Walk of Fame’ board was designed and displayed in the main thoroughfare of each intervention ward. Only patient initials were used on the board to protect confidentiality. Participation with the ‘Walk of Fame’ was optional. Patients, their families/carers and all staff were encouraged to use the board to record the number of times a patient mobilised outside of allocated therapy times and the total distance mobilised in metres. Individual distances were then summarised daily and weekly and displayed, with friendly competition encouraged among patients. The final mobilisation strategy was the introduction of weekly patient goals sheets, with goals closely aligned with the mobility chart. Staff members and families/carers engaged with patients to complete both the setting and achieving of goals on a weekly basis including walking three times per day, sitting out of bed for all meals, and getting dressed in day clothes every day.
Environmental changes were made in the intervention wards to encourage patients to spend more time away from their bedsides. A communal dining area was established where communal dining was encouraged twice per week, aiming for an average of four to eight attendees. Prior to this intervention, patients routinely ate their meals in their rooms, often in their beds. A clothing bank was established on each ward, so patients who were socially disadvantaged could gain access to day clothes if they did not otherwise have the means to source the clothing. ‘Laundry baskets’ were placed in each room with signage prompting patient's families/carers to ensure there were sufficient clean day clothes for patients during the inpatient stay. A walking track was introduced to each ward to encourage ambulation, with brightly colored posters placed on corridor walls at 10-meter increments to encourage mobilisation and assist patients in calculating the total distance walked.
Baseline measures
Patient characteristics were assessed within 48 h of admission and at discharge from geriatric rehabilitation by a multidisciplinary team using a comprehensive geriatric assessment (CGA) 19 . Age, sex and length of stay (LOS) in the acute ward and geriatric rehabilitation were extracted from medical records. Patients’ accommodation status prior to hospitalisation (home, retirement village, nursing home or others) and the use of a walking aid were assessed through a survey completed by the patient and/or carer, or data was extracted from medical records. A stadiometer assessed standing height for inpatients able to stand. Otherwise, knee height was assessed, and height was calculated using the Chumlea equation for Caucasians. 20 Weight was assessed by a standing scale, seated scale or a weighted hoist depending on ambulation status. Body mass index (BMI) was calculated by body mass (kg) divided by height squared (m2) and expressed in kg/m2.
The patients’ primary reason for hospital admission was collected via medical records and categorized into the following: musculoskeletal, neurological, cardiovascular, respiratory, infection, gastrointestinal, psychiatric, metabolic and urology. Comorbidity burden was assessed by the ward medical staff using the Charlson Comorbidity Index (CCI) 21 and the Cumulative Illness Rating Scale (CIRS). 22 Frailty was assessed by physicians using the Clinical Frailty Scale (CFS), a 9-point scale (1 being considered fit and 9 extremely frail). 23 All patients are screened for the presence of delirium using the Short Confusion Assessment Method (CAM), 24
Cognitive impairment was defined as (1) dementia or cognitive impairment documented in medical records or the CCI; (2) an abnormal standardized Mini-Mental State Examination (sMMSE) 25 score of <24 points; (3) an abnormal Montreal Cognitive Assessment (MOCA) 26 score of <26 points; or (4) an abnormal Rowland Universal Dementia Assessment Scale (RUDAS) 27 score of <23 points.
Outcome measures
Physical performance was assessed by physiotherapists using the Short Physical Performance Battery (SPPB) on admission and discharge. The SPPB includes three objective tests of lower body function including standing balance, timed mobilisation and a timed chair stand test. The SPPB has been established as valid, reliable and feasible, with a moderate predictive accuracy and validity in hospitalised older adults.28,29 The SPPB score is created by adding scores from the individual tasks with a higher score indicating better physical performance. 30
Functional performance was assessed by occupational therapists on admission and discharge using the Katz Index of Independence in ADL 31 and Lawton and Brody’s Instrumental ADL (IADL). 32 The ADL measure assessed independence in six self-care tasks, including bathing, dressing, toileting, transferring, continence and feeding. It has a dichotomous 0/1 rating scale, or dependent/independent. A score of 6 indicates full function, and a score of 2 or less indicates severe functional impairment. 33 This assessment has been shown to be reliable and valid. 34
IADL measure assesses independence in domestic and community tasks, which are characterised as complex activities a person needs to be able to perform to live independently in the community. It has a total score of 8, and the evaluation of independence again takes on a dichotomous rating scale of 0/1. The tool is valid and reliable. 35
Handgrip strength was assessed three times on each hand alternating using a handheld dynamometer (JAMAR hand dynamometer; Sammons Preston, Inc. Bolingbrook, IL, USA). 36 The maximum score in kilograms was used. 36 Patient mood was assessed using the Hospital Anxiety and Depression Scale (HADS), which is a simple and reliable tool used to screen for the presence of anxiety and/or depression symptoms. 37 The score ranges from 0 to 21 points, and a cut-off score of ≥8 points on each subscale indicating borderline/abnormal symptoms. Quality of life was assessed using the EuroQoL-5D-5L scale, a visual analogue scale that asks patients to rate how good they feel their health is on a scale of 0–100. 38
Fidelity measures
Hospital-reported key performance indicators were collected routinely throughout the intervention period. These included rates of falls across all wards and rates of hospital-acquired pressure injuries. These were monitored on a weekly basis by the project team and the nurse unit manager on the intervention wards to track any variance from baseline and any adverse outcomes were reviewed by the project team.
An audit feedback process was developed to measure rates of success in achieving the outlined goals. These audits were completed weekly on non-consecutive, randomly allocated days during the implementation period and recorded the location of the patient, for example, at the bedside, in the bathroom, in the communal area; the activity in which the person was engaged in at that particular moment in time, if any; and whether or not the patient had another person with them at that time, including staff.
The aims of the campaign were to get (1) 80% of patients in their day clothes by 11 a.m., (2) 80% of patients to be wearing appropriate footwear when out of bed, (3) 80% of patients to eat lunch and dinner sitting out of bed and (4) a 50% increase in participation of daily physical activity activities (reported elsewhere). 3
The results of the audits were displayed on specially designated staff notice boards on the wards and used as a promotional tool, to provide visual feedback to staff regarding compliance rates.
The results of the audits provided the parameters through which the successful implementation of the ‘Ending Pyjama Paralysis’ intervention could be measured.
Statistical analysis
Patient characteristics at admission were summarised by intervention arm (intervention vs control). Continuous data were summarised using the median (interquartile range, IQR), and categorical data were summarised as frequencies and percentages. To compare the primary and secondary study outcomes between intervention groups, a linear mixed-effects model with a random intercept for individuals was used, adjusted for baseline values to examine the primary outcomes SPPB, ADL and I-ADL and the secondary outcomes handgrip strength and EuroQoL-5D-5L score at discharge. A mixed-effects multinomial logistic regression model with a random intercept for individuals, adjusted for baseline values was used for HADS depression and HADS anxiety categories at discharge. For all primary and secondary endpoints with a positively skewed (non-symmetrical) distribution (SPPB, ADL, I-ADL, handgrip and EuroQoL-5D-5L score), log-transformed variables were used in the analysis models. Subgroup analysis for the secondary outcome handgrip was performed for the subgroups of sex, by fitting a linear mixed-effects model with a random intercept for individual, adjusted for baseline values, with an interaction term between the treatment arm and the variable for subgroup analysis, which is sex. No adjustments for multiple testing were conducted. Two-sided 95% confidence intervals, and p-values are reported. All descriptive statistics and statistical analyses were based on available data. All statistical analyses were conducted using Stata 16.1. 39
Results
There were 833 admissions throughout the data collection period, of which 669 patients had one admission, 70 had two admissions, and eight had three or more admissions. A total of 512 patients were admitted to control wards, and 321 patients were admitted to intervention wards. Baseline characteristics are reported in Table 1.
Clinical characteristics of geriatric rehabilitation inpatients in the control and intervention group.
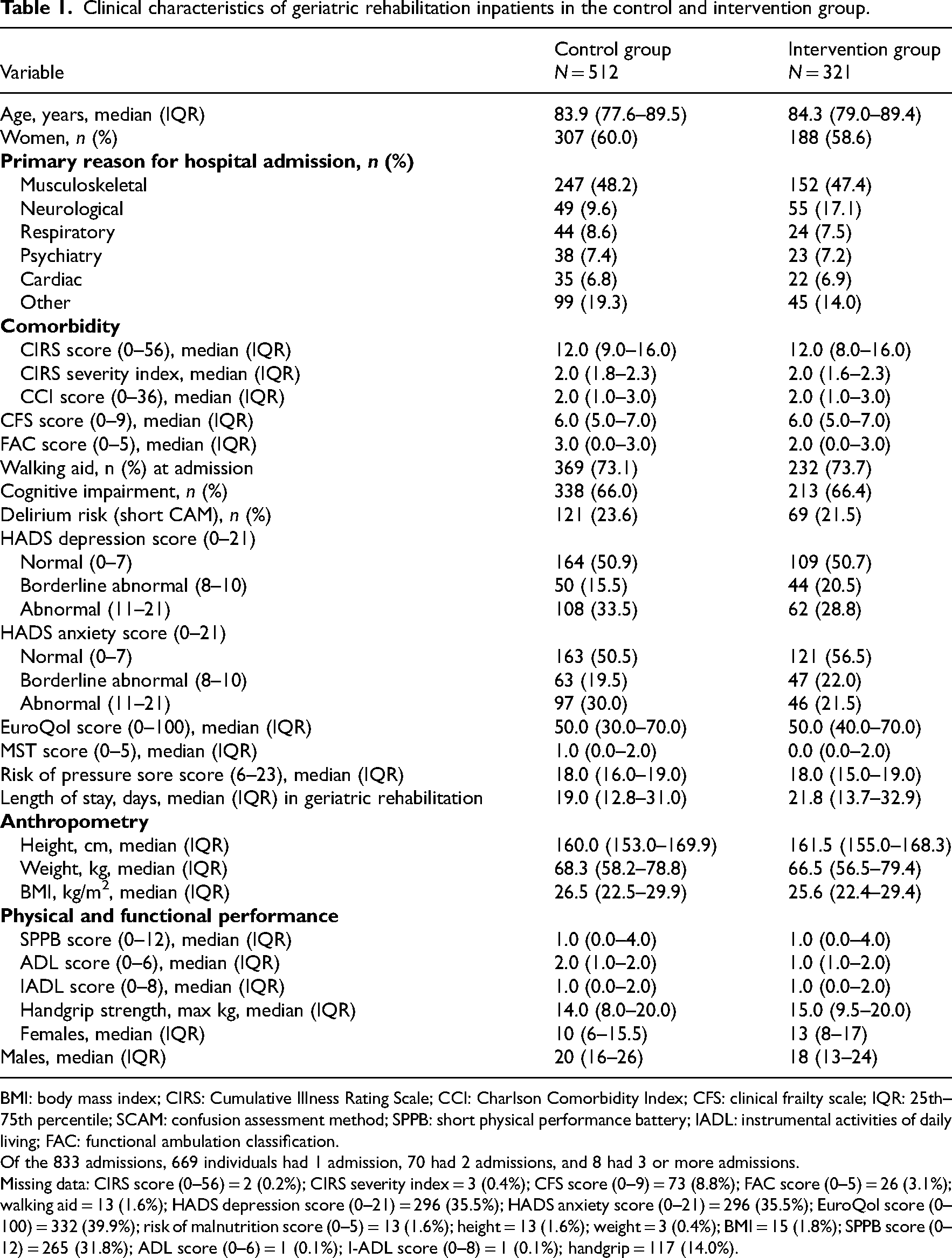
BMI: body mass index; CIRS: Cumulative Illness Rating Scale; CCI: Charlson Comorbidity Index; CFS: clinical frailty scale; IQR: 25th–75th percentile; SCAM: confusion assessment method; SPPB: short physical performance battery; IADL: instrumental activities of daily living; FAC: functional ambulation classification.
Of the 833 admissions, 669 individuals had 1 admission, 70 had 2 admissions, and 8 had 3 or more admissions.
Missing data: CIRS score (0–56) = 2 (0.2%); CIRS severity index = 3 (0.4%); CFS score (0–9) = 73 (8.8%); FAC score (0–5) = 26 (3.1%); walking aid = 13 (1.6%); HADS depression score (0–21) = 296 (35.5%); HADS anxiety score (0–21) = 296 (35.5%); EuroQol score (0–100) = 332 (39.9%); risk of malnutrition score (0–5) = 13 (1.6%); height = 13 (1.6%); weight = 3 (0.4%); BMI = 15 (1.8%); SPPB score (0–12) = 265 (31.8%); ADL score (0–6) = 1 (0.1%); I-ADL score (0–8) = 1 (0.1%); handgrip = 117 (14.0%).
The median age in the control groups was 83.9 years (SD 77.6–89.5) (60% female) and 84.3 years (SD 79–89.4) (58.6% female) in the intervention group. The vast majority of admissions on both control and intervention wards were musculoskeletal. The median LOS was 19 days in control (IQR 12.8–31) and 21 days in intervention wards (IQR 13.7–32.9) (Table 1).
Audits completed on both control and intervention wards from June to December 2019 revealed a significant increase in rates of compliance with the intervention, with the number of patients wearing day clothes during the day increasing to 75%. In contrast, in the control wards, an average of 33% of patients were wearing their day clothes during the day. The average number of patients wearing shoes on the intervention ward across the data collection period was 30%, compared to 13% of patients wearing their own shoes on the control wards. Finally, on the intervention wards, an average of 75% of patients were sitting out of bed for their lunch. This compares to 65% on control wards.
There were no differences in the primary measures of SPPB, ADL and IADL scores from admission to discharge between the intervention and control groups (Table 2).
Analysis of primary endpoints, physical and functional measures, at discharge.
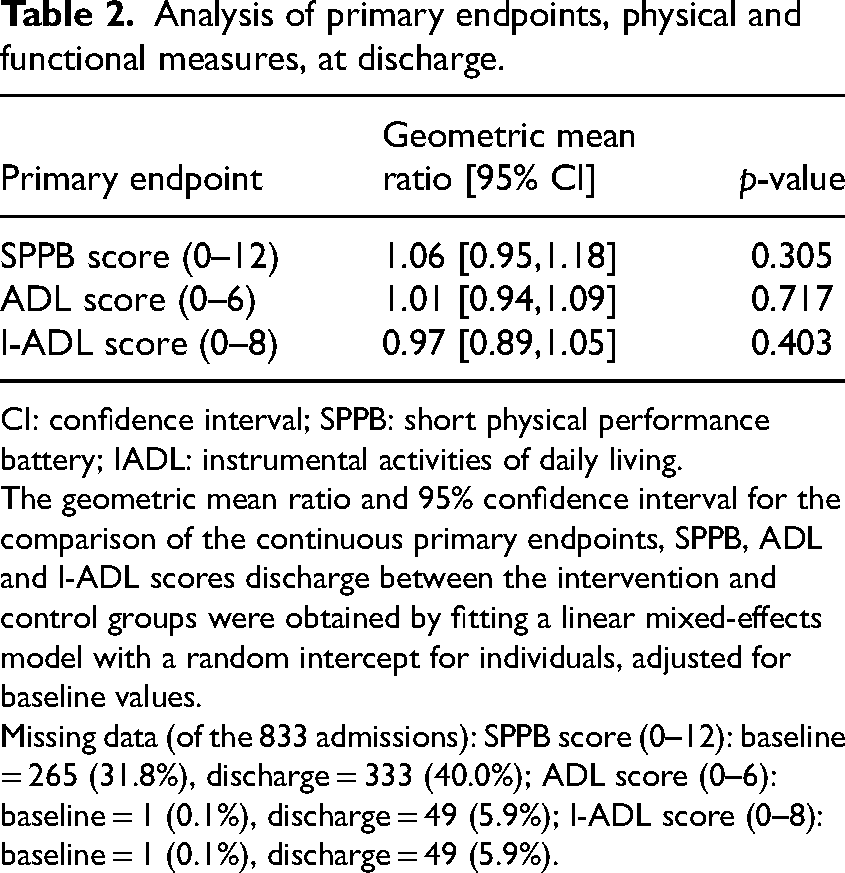
CI: confidence interval; SPPB: short physical performance battery; IADL: instrumental activities of daily living.
The geometric mean ratio and 95% confidence interval for the comparison of the continuous primary endpoints, SPPB, ADL and I-ADL scores discharge between the intervention and control groups were obtained by fitting a linear mixed-effects model with a random intercept for individuals, adjusted for baseline values.
Missing data (of the 833 admissions): SPPB score (0–12): baseline = 265 (31.8%), discharge = 333 (40.0%); ADL score (0–6): baseline = 1 (0.1%), discharge = 49 (5.9%); I-ADL score (0–8): baseline = 1 (0.1%), discharge = 49 (5.9%).
There was no significant difference between the intervention and control groups in handgrip strength and HADS depression and HADS anxiety categories.
For categorical data, the mixed-effects multinomial logistic regression model found no significant difference between the intervention and control groups for HADS depression data. There were no significant differences observed in the handgrip and EuroQoL-5D-5L scores at follow-up between the treatment arms (Table 3).
Analysis of secondary endpoints at baseline and follow-up.
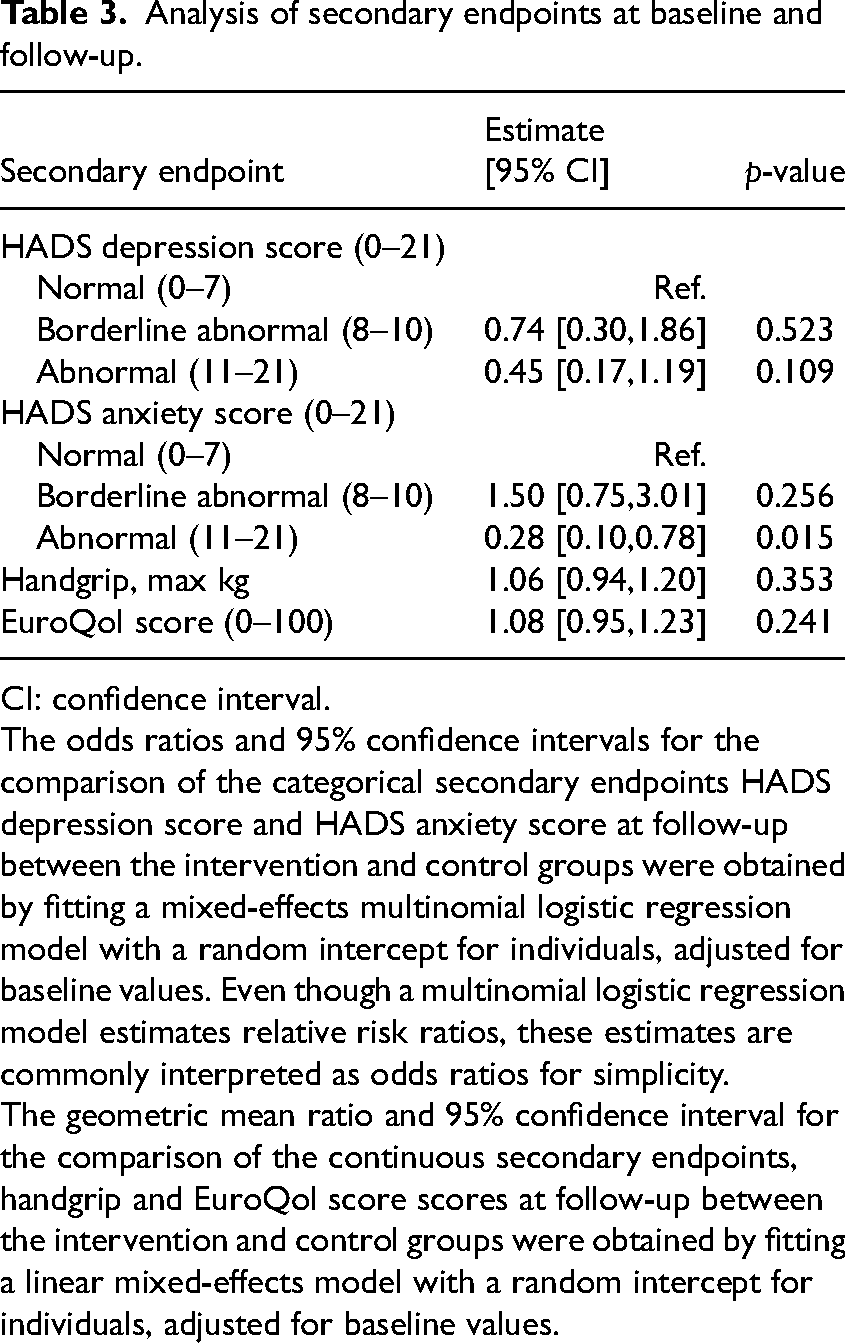
CI: confidence interval.
The odds ratios and 95% confidence intervals for the comparison of the categorical secondary endpoints HADS depression score and HADS anxiety score at follow-up between the intervention and control groups were obtained by fitting a mixed-effects multinomial logistic regression model with a random intercept for individuals, adjusted for baseline values. Even though a multinomial logistic regression model estimates relative risk ratios, these estimates are commonly interpreted as odds ratios for simplicity.
The geometric mean ratio and 95% confidence interval for the comparison of the continuous secondary endpoints, handgrip and EuroQol score scores at follow-up between the intervention and control groups were obtained by fitting a linear mixed-effects model with a random intercept for individuals, adjusted for baseline values.
There were no significant differences in rates of falls on intervention wards when compared to baseline data.
Discussion
This study found that the ‘Ending Pyjama Paralysis’ initiative did not demonstrate physical and functional benefits to geriatric rehabilitation inpatients, as determined using the measures described. Implementation of the ‘Ending Pyjama Paralysis’ campaign saw a higher number of patients on the intervention wards being up and dressed, in comparison to the control wards. However, this did not translate to improved functional outcomes for older people at discharge from the hospital. This campaign has seen worldwide recognition, and the principles have been replicated in hospitals across numerous countries. Routinely collected operational and clinical data including LOS, pressure ulcers, falls, and patient complaints have been the primary measures used to evaluate the success of this campaign. Reporting of these outcomes has been limited to local organizational and government reporting methods. The campaign has been criticised as ‘insufficient to tell us whether the clinical effects of the intervention are replicable, scalable, and sustainable at other sites’. 40 Despite the perceived and widely promoted benefits of the ‘Ending Pyjama Paralysis’ campaign on hospitalized elderly, there has been very limited research to date that has sought to systematically evaluate functional outcomes at the patient level.41,42
The present study demonstrated no functional or physical benefits of the ‘Ending Pyjama Paralysis’ campaign on geriatric rehabilitation patients when applied in addition to usual therapy in this setting. Despite many anecdotal reports from staff, patients and next of kin that the encouragement patients received to wear their own clothes did improve their general sense of well-being, the very act of getting dressed does not in and of itself improve patient outcomes. This also indicates that a one-size-fits-all intervention to reduce hospital-associated disability does not consider the complexity and heterogeneity of the frail older adults.
To improve outcomes of this population, a system-level, organization-wide approach is needed to ensure a thorough integration of principles that work to address the harm of immobility that is prevalent in hospital settings. That is, ‘immobility harm’ needs to be recorded and treated with the same diligence as pressure injuries and falls data and should be reported and reviewed to ensure instances of immobility harm are reduced in this setting. 17 It seems possible that in many settings, there is a pervasive fear of perceived harm that can arise from patient mobilisation, for example, falls, and that this might be a primary contributor to low physical activity and poor functional outcomes.43,44
Intervention must be combined with additional strategies to improve patient physical activity and expectations of patient participation in this setting. More resources need to be allocated to prevent functional decline in hospitals, with sustainable staffing structures and ratios to ensure mobilisation and functional independence are prioritized. Interventions provided more than once daily, for 15–30 minutes and 5–7 times per week lead to improved functional independence and physical performance as well as the performance of ADL 3 months after discharge.45,46 This type of intensity cannot typically be performed with current staffing ratios in aged care rehabilitation, and new models of care need to be examined to improve patient outcomes. Unsupervised mobilisation programs have been found to be unsuccessful, with most patients non-compliant with directives to move more. 47 Despite incorporating environmental enrichment strategies into the intervention wards as part of the ‘Ending Pyjama Paralysis’ program, patients remained constrained by the physical and organizational imperatives of a ward environment.
The interventions and initiatives described above were introduced in a staggered way to ensure the engagement of key stakeholders. However, key elements of the program, such as mobilisation strategies, were implemented later in the program and were ceased prematurely due to the COVID-19 pandemic, which saw restrictions on visitation by family members and curtailed staff access to the ward. Furthermore, a mixed methods approach requires the selection of data that may not capture all possible outcomes.
The ‘Ending Pyjama Paralysis’ campaign did not result in enhanced functional or physical benefits in geriatric rehabilitation inpatients in this setting when applied in addition to usual care using the measures described.
More needs to be done to address the barriers to physical activity that are inherent in a hospital environment to prevent functional decline in geriatric rehabilitation patients.
Supplemental Material
sj-docx-1-cre-10.1177_02692155231197510 - Supplemental material for Is there a relationship between ‘getting up and dressed’ and functional and physical outcomes in geriatric rehabilitation inpatients? A quasi-experimental study
Supplemental material, sj-docx-1-cre-10.1177_02692155231197510 for Is there a relationship between ‘getting up and dressed’ and functional and physical outcomes in geriatric rehabilitation inpatients? A quasi-experimental study by Rose Goonan, Edward Mohandoss, Celia Marston, Jaqueline Kay, Anurika Priyanjali De Silva, Andrea B Maier, Esmee Reijnierse and Marlena Klaic in Clinical Rehabilitation
Supplemental Material
sj-png-2-cre-10.1177_02692155231197510 - Supplemental material for Is there a relationship between ‘getting up and dressed’ and functional and physical outcomes in geriatric rehabilitation inpatients? A quasi-experimental study
Supplemental material, sj-png-2-cre-10.1177_02692155231197510 for Is there a relationship between ‘getting up and dressed’ and functional and physical outcomes in geriatric rehabilitation inpatients? A quasi-experimental study by Rose Goonan, Edward Mohandoss, Celia Marston, Jaqueline Kay, Anurika Priyanjali De Silva, Andrea B Maier, Esmee Reijnierse and Marlena Klaic in Clinical Rehabilitation
Supplemental Material
sj-png-3-cre-10.1177_02692155231197510 - Supplemental material for Is there a relationship between ‘getting up and dressed’ and functional and physical outcomes in geriatric rehabilitation inpatients? A quasi-experimental study
Supplemental material, sj-png-3-cre-10.1177_02692155231197510 for Is there a relationship between ‘getting up and dressed’ and functional and physical outcomes in geriatric rehabilitation inpatients? A quasi-experimental study by Rose Goonan, Edward Mohandoss, Celia Marston, Jaqueline Kay, Anurika Priyanjali De Silva, Andrea B Maier, Esmee Reijnierse and Marlena Klaic in Clinical Rehabilitation
Footnotes
Acknowledgements
The authors would like to thank the @Age team from the the Royal Melbourne Hospital (removed for peer review) for their support in data acquisition and management and (2) all medical, nursing and allied health staff at the Royal Melbourne Hospital for their clinical work and data collection.
Author contributions
Authors’ contribution is defined by meeting the International Committee of Medical Journal Editors (ICMJE) criteria. RG, EMo and MK were responsible for the study concept and design and drafting of the manuscript. MK and AD were responsible for the data analysis. All authors contributed to the analysis and interpretation of the data and the critical revision of the manuscript. All authors approved the final version of the manuscript to be published.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
